, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Tinea crurisJock itchGroinFungusFungalInfectionDermatophyteAntifungalTrichophyton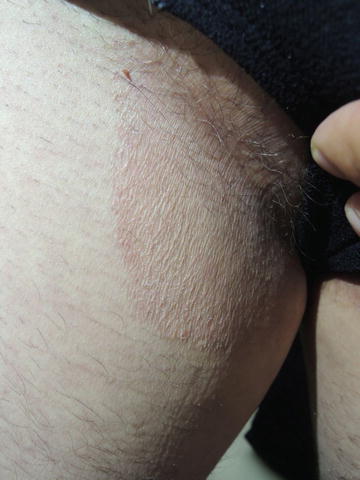
Fig. 29.1
Heavy itch and most commonly seen in more sedentary individuals with a higher body mass index (BMI)
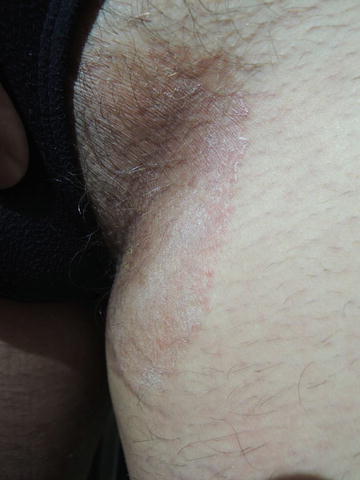
Fig. 29.2
May be bilateral as in this patient or unilateral. Maceration may be present if perspiration is heavy
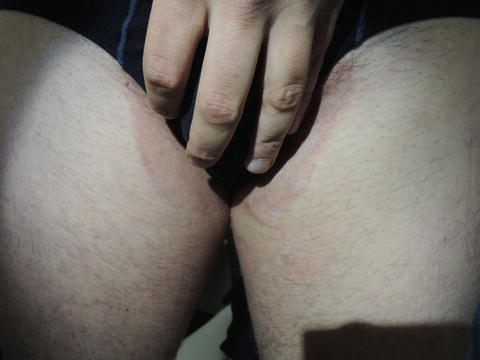
Fig. 29.3
The wavy border seen in this condition helps differentiate it from inverse psoriasis
Primary Care Visit Report
A 33-year-old male with no prior medical history presented with a rash in his inguinal creases. The patient described the rash as itchy, and said it felt irritated and had a rough texture. He had a similar rash 3 years prior for 3 weeks but it resolved on its own. Over the prior 1½ years, the rash had recurred and abated, sometimes lasting for 6 months at a time. During that time, the patient used over-the-counter hydrocortisone cream , which helped with the itchiness and irritation, but the discoloration and texture-change remained. The present rash recurred 3 months prior to this visit. The patient reported exacerbation with exercise or warm weather. The patient tried changing to a different detergent, which had no effect.
Vitals were normal. On exam, in the bilateral inguinal creases, there were erythematous scaly patches with well-delineated borders extending inferiorly to the medial thighs and extending medially about 1 cm medial to the inguinal crease. Woods lamp exam revealed orange fluorescence in a 2 cm × 1 cm area in the left inguinal crease. The remainder of the rash did not fluoresce.
The differential diagnosis considered was erythrasma vs. tinea cruris vs. contact dermatitis. Since the rash did not fluoresce red overall (as would be expected with erythrasma), it was treated as tinea cruris with 2 % ketoconazole cream twice daily for 21 days. The patient was advised to change out of sweaty gym clothes immediately after exercising.
Discussion from Dermatology Clinic
Differential Dx
Tinea cruris
Erythrasma
Contact dermatitis
Intertrigo
Inverse psoriasis
Langerhans’ cell histiocytosis (rare)
Favored Dx
Tinea cruris thrives in warm, humid conditions. The patient history of symptoms getting worse with exercise and warm weather is suggestive of tinea cruris. Pruritus is a requisite in making this diagnosis.
Overview
Tinea cruris is a fungal infection of the thighs, groin , and pubic region commonly referred to as “jock itch .” It is a superficial cutaneous subacute or chronic dermatophytosis most often caused by the Trichophyton rubrum fungus . The infection typically occurs in adulthood and is more common in males [1]. Infection can be passed from person to person via skin-on-skin contact; however, it is not a common cause of contagion. It may also be passed through shared unwashed clothing [2] or other objects that carry the infected scales [3]. Contact sports may be associated with tinea because of frequent or prolonged skin-on-skin contact, or other factors such as contact with wrestling mats, time spent in sweaty clothes, and use of shared shower facilities.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








