, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
EczemaAtopic dermatitisAtopyAtopic eczemaInflammationInflammatoryAsthmaSeasonal allergiesAllergic rhinitisAtopic marchHygiene hypothesisPruritusPruriticPapuleVesiclePapulovesicularChildhood eczemaFilaggrinXerosisLichenificationDry skinEmollientCorticosteroidTopical steroidChronicRelapsingSkin barrierMoisturizer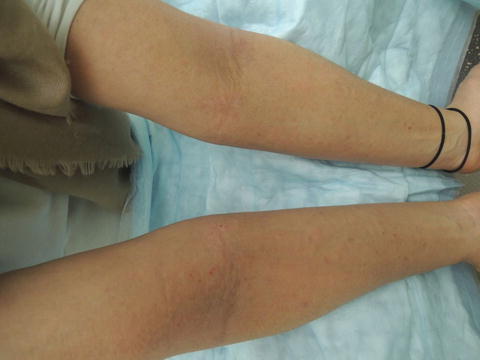
Fig. 35.1
Antecubital poorly marginated erythematous, excoriated plaques
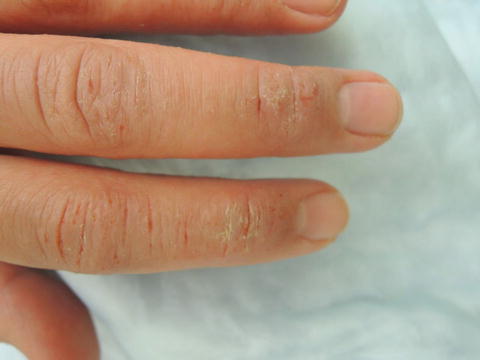
Fig. 35.2
Lichenified, scaly, erythematous plaques dorsal fingers
Primary Care Visit Report
A 29-year-old female with past medical history of asthma , atopic eczema, and sesame/peanut allergies presented with an atopic eczema flare. The patient had atopic eczema and asthma since childhood and experienced frequent flares. She had recently started taking high dose probiotics—75 billion cfu/day—for 3 weeks and while taking them she experienced no atopic eczema flares. One week after stopping the probiotics, she had an acute flare on her fingers, elbows, face, and neck. She initially started getting the rash on her fingers and hands about 15 years ago. The eczema on her face started about 5 years prior when she first started to wear makeup. The eczema on her neck started about 2 years prior. She had run out of higher potency steroid cream so she tried applying polysporin antibiotic ointment as she found the lower potency steroid cream she had made the rash itchier.
The patient’s last severe eczema flare was about 3 months prior and at that time, she was treated with Hydrocortisone Butyrate Ointment (Class V) 0.1 % as well as an oral prednisone 10-day taper.
The patient reported that her asthma had flared as well and she needed to use her albuterol inhaler at least twice daily during this time.
The patient had tried to cut gluten out of her diet but only succeeded in doing this for 1 week and did not notice any improvement.
Vitals were normal. On examination, the dorsum of her hands and fingers featured an erythematous, textured papular rash with some open shallow ulcers on her fingers bilaterally; her antecubital fossae had erythematous plaques bilaterally; her anterior neck had erythematous macules; and her face had erythematous macules on the left cheek, left infraorbital area and across the bridge of her nose extending to her right cheek.
This was treated as an atopic eczema flare and she was prescribed topical hydrocortisone butyrate ointment 0.1 % (Class V) twice daily for 14 days as well as oral prednisone, given the severity. The prednisone was prescribed as a 10-day taper starting with 80 mg daily × 3 days, 60 mg/day × 3 days, 40 mg/day × 3 days, and 20 mg/day × 1 day.
Discussion from Dermatology Clinic
Differential Dx
Atopic eczema
Allergic contact dermatitis
Irritant dermatitis
Scabies
Tinea corporis
Seborrheic dermatitis
Psoriasis
Favored Dx
The xerotic (abnormally dry) and fissured presentation of the patient’s hands is consistent with atopic eczema.
Overview
Atopic eczema (AE) is a non-contagious, chronic, and relapsing highly pruritic inflammatory skin disease. It is very common, with an estimated 15–30 % lifetime prevalence in children and 8–10 % lifetime prevalence in adults [1]. It is often considered a disease of childhood, as up to 85 % of cases are diagnosed before the age of 5; however, it is not uncommon in adults. AE is slightly more prevalent in females.
The overall incidence of AE has increased significantly over the last several decades, especially in developed countries and urban areas [1, 2]. Some have explained this phenomenon in relation to the hygiene hypothesis , which is the idea that decreased exposure to infections and allergens has prompted a rise in allergic diseases; however, this association only appears to be true in affluent countries [1, 3]. In fact, the pathogenesis of AE is complex and influenced by multiple genetic, social, and environmental factors.
Mutations in the filaggrin gene FLG, which encodes a structural protein that contributes to water retention in the skin and maintaining the skin’s barrier function, and dysregulated type 2 T helper cells (Th2) are known to have a strong association with AE [1, 4, 5]. The role of genetic factors is further demonstrated by increased risk of developing AE when there is positive parental history of eczema, asthma , or allergic rhinitis (hayfever), and higher concordance rates in monozygotic compared to dizygotic twins [1, 6–9]. Having AE in childhood predisposes individuals to developing asthma and allergic rhinitis later in life, which is sometimes referred to as the allergic or atopic march [5, 10].
In addition to genetics, social and environmental factors play a role in the pathogenesis of AE. The prevalence of AE is higher among people of black or mixed race, and in metropolitan areas [2]. Emotional stress and infections are associated with acute flares [1]. Having multiple siblings, childhood pet dogs, parents who were born outside the USA, and living in a rural area demonstrate a protective effect against developing AE [2, 11, 12].
Presentation
The presentation of AE varies depending on the age of the patient, and the duration and severity of the disease. In infants, the condition tends to appear on the scalp and face, particularly in the cheek area, and on extensor surfaces of the arms and legs. The rash looks highly erythematous and may be weeping. Childhood AE most commonly appears on flexor surfaces of the extremities, specifically the antecubital and popliteal fossa, and the neck, wrists, and ankles. Adults also tend to experience AE in the antecubital and popliteal fossa, as well as the neck and face, especially in the periorbital area.
AE presents as a xerotic, erythematous rash. For all age groups, it is a highly pruritic condition that can be severe enough to interrupt sleep. Some patients experience pruritus intermittently, corresponding with acute flares, while others experience the sensation at all times. As such, AE lesions may feature excoriations caused by scratching, as well as papules, scaling, and fissures. Symptoms may get worse in the winter months, when air tends to be more dry. Patients who have experienced atopic eczema for years may present with dyspigmented, lichenified (thickened) skin. The dry, cracked skin typical of AE allows pathogens to penetrate and makes individuals more susceptible to infections.
Workup
AE is typically a clinical diagnosis, with appearance of lesions, report of pruritus, history of recurrence, family history of AE, and associated atopic conditions all providing evidence to support the diagnosis. Allergy patch testing can be performed if patient history suggests a specific allergen which triggers a flare, or if contact dermatitis needs to be ruled out. IgE levels are elevated in a large proportion of individuals with AE; however, this parameter is non-specific as IgE can be elevated in other atopic conditions.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








