, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
ParonychiaNailPeriungualIncision and drainageChronicAcuteBacterial Candida albicans Occupational dermatitisWork related dermatitisWarm water compressAntibioticsAntifungalTopical steroid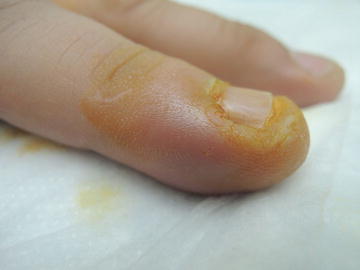
Fig. 10.1
Tender, boggy, erythematous tissue at right perionychium (Patient has applied iodine to account for yellow color)
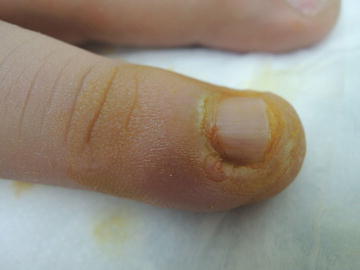
Fig. 10.2
Possible inoculation point noted at site of disrupted cuticle
Primary Care Visit Report
A 32-year-old male with no past medical history presented with swelling of his right hand fourth finger, near his fingernail. It started the day prior to this visit, and he said he felt a lot of pressure in the fingertip. He tried icing it overnight with no improvement.
Vitals were normal. On exam, the skin lateral to the fingernail on his right hand fourth finger was erythematous , edematous, warm, and very tender to palpation. There was minimal fluctuance.
This was treated as paronychia. His finger was first soaked in warm water for 30 min, then an incision and drainage procedure was performed with a digital nerve block. However, no pus was expressed. The patient was sent home with instructions to soak his finger in warm water twice daily and to apply bacitracin to the area. He was asked to return to the office if the redness and swelling persisted or worsened.
Discussion from Dermatology Clinic
Differential Dx
Bacterial paronychia
Candidal paronychia
Drug-induced paronychia
Nail fold dermatitis
Herpetic whitlow
Ingrown nail
Favored Dx
Clinical examination and history are consistent with acute bacterial paronychia. It is apparent from physical examination that the patient is a nail biter, which is one of the predisposing factors for paronychia.
Overview
Paronychia is a common inflammation of the proximal nail fold and periungual soft tissues , which is classified as acute when it lasts fewer than 6 weeks, and chronic when it lasts greater than 6 weeks. The majority of cases are acute paronychia, which is most commonly associated with bacterial infection following mild local trauma, while chronic paronychia is associated with candidiasis. Predisposing factors for paronychia are exposure to chemical irritants, mechanical factors such as nail biting, picking, or finger sucking, and systemic conditions, such as diabetes and HIV [1, 2]. Less frequently, paronychia has been associated with use of certain medications, such as protease inhibitors, antiretrovirals, and chemotherapeutic agents.
The most common bacterial pathogen involved in acute paronychia is Staphylococcus aureus . Streptococcus pyogenes , Pseudomonas aeruginosa , and Proteus species are involved with less frequency [1–3]. Most cases of bacterial paronychia are caused by mixed flora, and paronychia that comes in contact with oral flora, as in nail biting and finger sucking, typically involves anaerobic bacteria [2, 4]. Candida albicans is often found in chronic paronychia. The pathogenesis of chronic paronychia is usually complex and multifactorial, and is currently thought to be an inflammatory process which may feature an overlying acute (i.e., bacterial) paronychia. Chronic paronychia is associated with excessive moisture, which may be the result of frequent immersion of the hands in water, as happens with occupational wet work. Paronychial herpes simplex virus lesions are referred to as herpetic whitlow.
Presentation
Acute paronychia presents as rapid-onset periungual erythema, swelling, and tenderness. Acute paronychia may develop within hours, and there may be ulceration and purulence. It usually presents on a solitary digit [2].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








