, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Dyshidrotic eczemaEczemaPompholyxHand eczemaVesiclesVesicular dermatitisChronicTopical steroidCorticosteroidPrednisonePhototherapy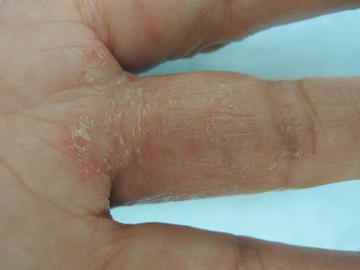
Fig. 13.1
Digits are preferentially affected with roughened plaques and prominent itch
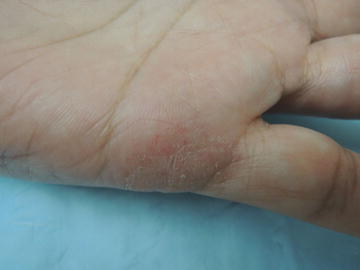
Fig. 13.2
Scale is found throughout this eczematous thin plaque
Primary Care Visit Report
A 60-year-old female with past medical history of hypertension presented with a rash on her hand that she described as intermittently present since the birth of her son 36 years earlier. The rash was on the base of her right hand third finger, and on the lateral aspects of both of her hands. The patient had been using clobetasol on the rash for flares. She reported cycles of clearance for 2–3 weeks followed by recurrence.
Vitals were normal. On exam, on the palmar aspect of the patient’s right hand, at the base of her third finger there was a 3 cm × 2 cm dry, scaly plaque and at the lateral base of her pinky finger there was a 2 cm × 2 cm dry, scaly plaque. On the patient’s left hand, at the lateral base of the pinky finger on the palmar aspect, there was a 2 cm × 2 cm dry, scaly plaque.
This was treated as eczema . The patient had been using clobetasol proprionate (Class I steroid) fairly liberally for many years, but given the frequency with which she used it, she was prescribed desonide 0.05 % (Class VI steroid) cream twice daily for 14 days. A lower potency steroid was chosen to see if it would resolve the rash. The patient was also referred to dermatology.
Discussion from Dermatology Clinic
Differential Dx
Pompholyx (AKA dyshidrotic eczema )
Contact dermatitis
Pustular psoriasis
Scabies
Favored Dx
The desquamation noted on the patient’s palms is consistent with the final stages of the vesicular eruption seen in pompholyx—eczema of the hands or feet.
Overview
Pompholyx is a type of chronic, vesicular dermatitis affecting the hands and sometimes the feet. It is also called dyshidrotic eczema , and it is characterized by small pruritic vesicles. Increased presence of eccrine sweat glands in the palms and soles of feet, as well as its link with hyperhidrosis, has led to the association of the vesicles in pompholyx with sweat glands [1]. These factors also make the condition more prevalent in warm weather.
The etiology of pompholyx is not known, although it has been linked with general eczema, contact allergies, hyperhidrosis, smoking, emotional stress, and immunological responses [2–4]. Immunocompromised populations, such as those with HIV infection, show a greater predisposition to pompholyx [1]. The condition can occur at any age but it shows peak prevalence between the ages of 30 and 40 years [2]. There is no gender preference.
Presentation
Pompholyx typically presents as a vesicular eruption on the palms, particularly the lateral aspects of fingers, and/or soles of feet. Palmar lesions alone occur in seven out of ten cases, palmoplantar lesions (on both hands and feet simultaneously) in two out of ten cases, and plantar lesions alone in one out of ten cases [2]. The tense, deep-seated, fluid-filled vesicles tend to be highly pruritic and may be accompanied by a burning sensation. Patients may report exacerbation of the burning sensation when they come in contact with water. The onset of small vesicles tends to be sudden. They may eventually coalesce and form a larger blister, and the lesions may spontaneously resolve. After the acute phase, patients experience desquamation on the affected skin. Recurrence is common.
Workup
Clinical diagnosis is usually sufficient. If there is a suspicion of contact dermatitis based on patient history, allergy patch testing may be done. Cases that are suspicious for bullous pemphigoid or epidermolysis bullosa, or where vesicles are hemorrhagic, should be referred to dermatology, where an immunofluorescence biopsy testing for the presence of antibodies may be performed. This biopsy requires a special transport medium (Michel’s). Pompholyx of the feet should be evaluated for any dermatophytes as the compromised skin barrier becomes vulnerable to opportunistic infection. Dermatophytes may be detected by performing a KOH test on skin scrapings to look for hyphae.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








