, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
OnychomycosisDermatophytosisDermatophyteFungusFungal infectionToenail Trichophyton rubrum Candida albicans Tinea pedisYellow nailPAS stainOnycholysisNail cultureJubliaCiclopiroxPenlacTerbinafineAntifungal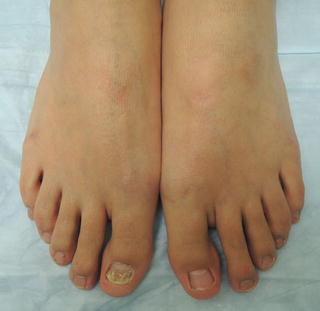
Fig. 18.1
Note not all toenails are typically affected
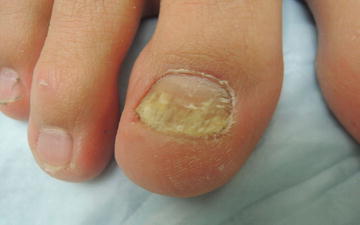
Fig. 18.2
Thickened nails with subungual debris, discoloration, and dystrophic nail plate
Primary Care Visit Report
A 27-year-old female with no past medical history presented with a yellow, layered, scaly big toe toenail . Her toenail had been like that for almost 10 years; however, she had never treated it.
Vitals were normal. On exam, the right foot hallux toenail presented with thickening, scaling, peeling and yellow discoloration. The second toe of her left foot featured peeling of the distal skin of the toe.
This was treated as onychomycosis. A blood test for baseline liver function was ordered, and the patient was started on a 12-week course of oral terbinafine .
Discussion from Dermatology Clinic
Differential Dx
Onychomycosis
Psoriasis
Lichen planus
Trauma
Onychogryphosis
Subungual wart
Favored Dx
Physical examination is consistent with onychomycosis, distal subungual type. The peeling skin indicates underlying tinea pedis , which should also be treated.
Overview
Onychomycosis is a fungal infection of the nail by dermatophytes , yeasts, and non-dermatophyte molds. It is a common condition that affects 10–12 % of the population in the USA [1]. Incidence can be up to 25 % in some countries [2]. Prevalence increases with age, to affect up to 50 % of people above the age of 70, and it is increasing overall across all age groups [2–4]. Onychomycosis is often preceded by untreated tinea pedis which then spreads to the nail bed . Onychomycosis affects toenails more than fingernails, and tinea pedis accompanies onychomycosis in 30 % of cases [3]. Other risk factors are diabetes, immunocompromised state such as HIV, trauma, and poor peripheral circulation [3, 5].
The majority of onychomycosis cases are caused by the dermatophytes Trichophyton rubrum , T. interdigitale , and T. mentagrophytes [3–5]. The yeast Candida albicans is present in some fingernail onychomycosis, especially in cases of chronic paronychia. Immunocompromised status is a risk factor for developing candidal onychomycosis [6]. Candida is not thought to play a role in toenail onychomycosis. Acremonium, Aspergillus, Fusarium, and Scopulariopsis are nondermatophyte mold species that have been associated with fungal infection of the nail in rare instances.
Presentation
There are three clinically distinct subtypes of onychomycosis : distal subungual onychomycosis (DSO) , proximal subungual onychomycosis (PSO) , and white superficial onychomycosis (WSO) . These have a clinically similar appearance, and are distinguished by the anatomical location of colonization. DSO affects the distal edge of the nail, PSO affects the proximal nail fold, and WSO results from direct invasion of the dorsal surface of the nail plate. DSO is the most common subtype overall, and PSO is more common in immunocompromised persons. PSO mostly involves T. rubrum and may be considered a sign of HIV [4].
Onychomycosis presents as thickened, opaque nail(s) with white, yellow, brown, or black discoloration. The nail(s) can feature shedding, onycholysis (separation of the nail from the nail bed), and subungual hyperkeratosis , marked by a chalk-like material that builds up under the nail [5]. All feature nail thickening, although WSO may not initially as the area beneath the surface of the nail may not yet be colonized [3]. WSO presents with superficial white spots on the nail plate. Fifty percent of cases of nail dystrophy have an underlying fungal etiology [3].
Workup
The diagnosis of onychomycosis should be confirmed by laboratory test prior to initiating oral treatment. Periodic-acid-Schiff (PAS) staining of a nail clipping is preferred as it is the most sensitive test for onychomycosis [7–9]. For this test, the affected nail is clipped just distal to its attachment to the nail bed, and the clipped nail along with its attached subungual debris are sent in 10 % formalin to the lab. A culture of the nail plate and subungual debris may be taken; however, it takes 3–6 weeks to obtain results [7]. If a culture is negative but the clinical suspicion is high, it should be repeated as culture results are associated with a high proportion of false negatives [8, 9].
A KOH test may be performed; however, it cannot identify the fungal species nor differentiate between dermatophyte , yeast, and mold infections. The subungual debris from the affected area is scraped onto a slide, KOH is added, and it is then viewed under the microscope. In cases of onychomycosis, KOH examination of subungual debris would reveal hyphae, pseudohyphae, or spores. KOH examinations and cultures are associated with more false negatives than PAS staining [6, 7]; however, KOH test has the advantage that it can be done rapidly in-office, at a low cost. A liver function test can be performed in advance of confirmed diagnosis in order to be able to potentially initiate oral antifungal treatment without having the patient return for this blood test.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








