, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
PsoriasisPlaqueGuttateInversePustularErythrodermicChronicRelapsingImmuneScalePolygenicNail changesNail pittingOnycholysisPsoriatic arthritisHLAPASICorticosteroidRetinoidCalcineurin inhibitorTacrolimusTarPhototherapyPUVAMethotrexateBiologicsAdalimumabEtanerceptAnti-TNF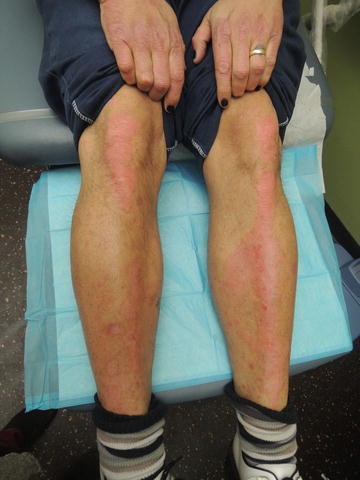
Fig. 36.1
Red hyperkeratotic plaques over knees and pretibia
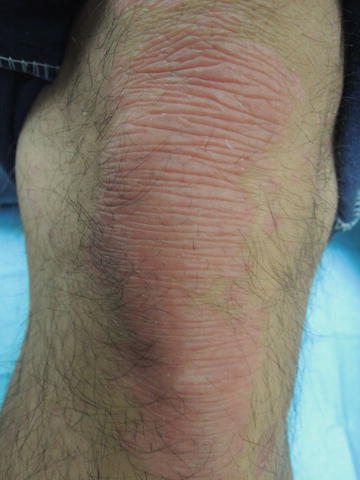
Fig. 36.2
Accentuated skin markings overlying erythematous, well-marginated plaque
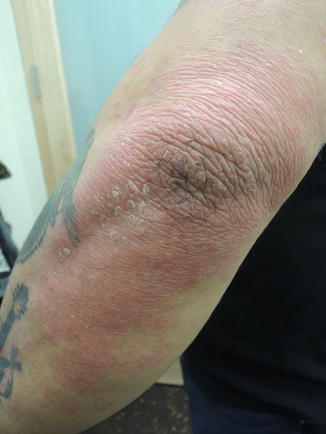
Fig. 36.3
Extensor surfaces predominate in this inheritable condition
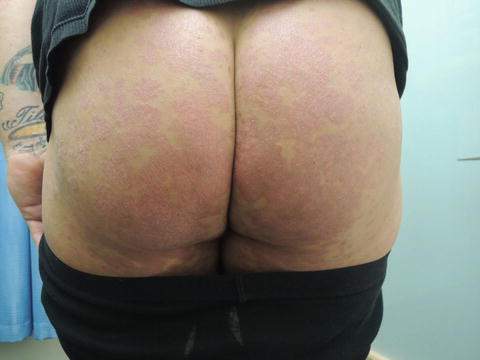
Fig. 36.4
Buttocks with polycyclic scaly erythematous plaques
Primary Care Visit Report
A 47-year-old male with past medical history of asthma and psoriasis presented with a psoriatic flare . The patient had been without health insurance until recently and this visit was his first time seeing a doctor in years. He had been able to control his flares by soaking in water and Epsom salts, and occasionally using a cream.
Vitals were normal. On exam, there were large erythematous scaly plaques on extensor surfaces of the bilateral forearms, bilateral lower legs, and bilateral dorsal hands, as well as on his buttocks and bilateral medial thighs.
Given the patient’s extensive history of psoriasis and the extent of the areas affected, he was referred to dermatology to explore further treatment options.
Discussion from Dermatology Clinic
Differential Dx
Psoriasis
Atopic dermatitis
Nummular eczema
Lichen planus
Lichen simplex chronicus
Tinea corporis
Pityriasis rosea
Subacute cutaneous lupus erythematosus
Favored Dx
The lesion distribution and erythematous , thickened, plaque-like appearance are indicative of psoriasis.
Overview
Psoriasis is a chronic , relapsing , immune-mediated disease estimated to affect 0.5–4.6 % of the population [1, 2]. It affects men and women equally, and is about twice as likely to occur in Caucasians [1, 2]. Onset of psoriatic symptoms is most likely between the ages of 15 and 30 [3]. One large study reported a median age of 28 years [1]. Global epidemiology of psoriasis is varied, with highest incidence in Western Europe, North America, southern Latin America, Australasia, and Asia Pacific [4]. Higher incidence is also associated with higher geographic latitudes (i.e., closer to the North or South Pole) [1, 2].
The exact cause of psoriasis is not known [3]. There is a strong genetic basis for the disease, and its expression is thought to result from contribution by multiple genes. Monozygotic twin studies show a concordance rate of 35–73 %, suggesting there are environmental factors contributing to the pathogenesis of psoriasis [3, 5]. HLA genes on chromosome 6 have been implicated, but the disease is thought to be caused by an interaction of several genes and environmental factors [1–3, 5]. UV exposure may be one environmental factor, supported by the efficacy of UV therapy in treating psoriasis [3].
Onset of psoriasis occurs after predisposed individuals experience a triggering event, such as trauma, infection, allergic drug reaction, or emotional stress [3, 5]. T cell mediated immune responses are activated and proinflammatory cytokines are released. Natural killer cells, TNF-α, and interleukins IL-12, 17, 22, and 23 are frequently involved [3, 5, 6]. These mediators lead to a range of changes on the skin, and nails, and dilation of capillaries causing erythema.
Presentation
There are several phenotypic variants of psoriasis. They include plaque, inverse, guttate , erythrodermic , and pustular psoriasis . The most common is plaque psoriasis, also called psoriasis vulgaris , and accounts for over 80–90 % of cases [1, 3, 7]. It is characterized by erythematous plaques with well-defined borders, occurring on the extensor surfaces of arms and legs, the lower back, scalp, and neck. Plaques may feature a silvery-white scale. The lesions usually occur symmetrically, and range from coin-sized to large plaques [3]. They are often asymptomatic but can be accompanied by pruritus. Nail changes , pitting and onycholysis (separation of the nail from the nail bed) are eventually seen in about half of patients with chronic psoriasis [1, 3]. Psoriatic arthritis occurs in up to 25 % of patients with psoriasis [3]. This usually manifests as joint swelling, particularly at the distal interphalangeal joints, inflammation of an entire finger or toe (dactylitis), and inflammation of the vertebra (spondylitis). It can precede psoriasis in 20 % of patients [1].
Inverse psoriasis occurs in intertriginous areas where skin touches or rubs together, such as the axilla, inguinal folds, and retroauricular folds. This variant accounts for 2–6 % of psoriatic patients, and is more likely to present in obese people [7]. Lesions usually do not feature the scaling typical of psoriasis, and may be confused for tinea infections.
Guttate psoriasis is usually self-limiting (resolution within 6–12 weeks) and occurs following streptococcal throat infection [1, 3, 7]. It is characterized by an eruption of small erythematous papules, most often on the trunk and extremities. Guttate psoriasis is more common in young adults, and is associated with an increased risk of developing plaque psoriasis [7].
Erythrodermic psoriasis is a variant whose most prominent feature is erythema. It can affect all parts of the body and have up to 100 % cutaneous surface area involvement. It can develop slowly in patients with plaque psoriasis, with lesions coalescing over time, or suddenly and unexpectedly [3]. Patients with this variant are at risk of developing hypothermia and hyperthermia in cold and warm climates respectively, due to body temperature loss through extensive vasodilation.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








