, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Diaper dermatitisDiaper rashNapkin dermatitisCandidiasisIrritant dermatitisMacerationSatellite pustuleTopical antifungalBarrier creamOintment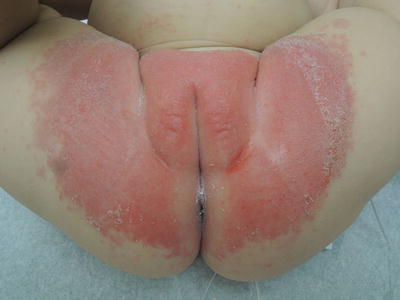
Fig. 31.1
Note relative sparing of inguinal and intergluteal areas protected from exposure
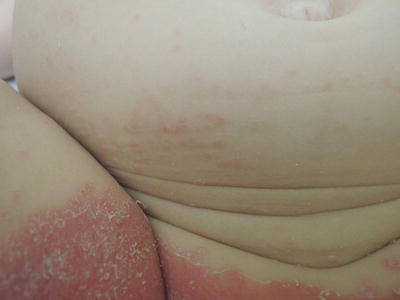
Fig. 31.2
Satellite lesions on abdomen indicate a different process than the confluent beefy red rash
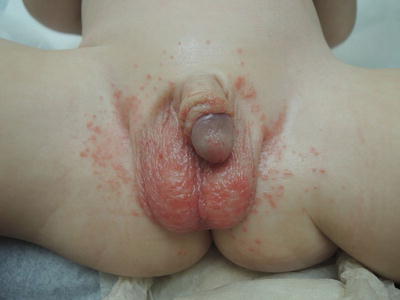
Fig. 31.3
Erythematous beefy-red satellite papules in bilateral groin
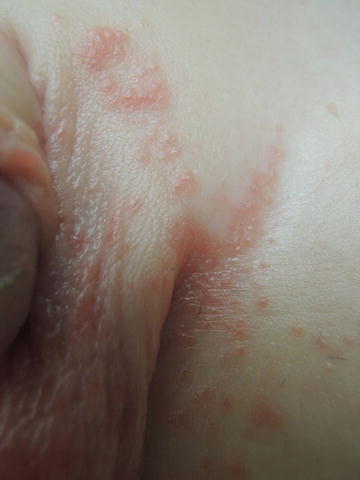
Fig. 31.4
Grouped erythematous papules in the inguinal crease
Primary Care Visit Report
The first patient was an 11-month-old female with no past medical history who presented with a diaper rash . The rash had started 6 days prior, and her parents had applied Desitin diaper rash treatment and gave her plenty of diaper-free time. They said the rash had started to spread outside the diaper area and that the patient had started scratching it. She also had a small rash in her neck fold and on her face.
Her vitals were normal. On exam, in her genital area there was a confluent 10 cm × 15 cm erythematous macular patch with scaling at the edges, with some individual erythematous satellite papular lesions on the periphery of the confluent area. Her inguinal folds had some excoriated areas. Her lower abdomen and chest had scattered 2–3 mm erythematous papular lesions.
This was treated as both irritant contact dermatitis as well as a fungal infection. The patient was prescribed over-the-counter hydrocortisone 1 % cream (Class VII) twice daily for 7 days and nystatin cream 100,000 unit/g three times daily or with every diaper change. The parents were advised to use a barrier cream such as Desitin, A&D, Vaseline, or zinc on top of the steroid cream and the nystatin. They were advised to apply the creams in this order: hydrocortisone cream first, then nystatin, and finally barrier cream.
The second patient was a 1 year-old male with no past medical history who presented with a cough, fever, and diaper rash . The patient had been seen 1 week prior for his 1-year well visit and had the diaper rash then. At that point, he was instructed to use bacitracin ointment on the rash, and to let the area air-dry after each bath. He returned 1 week later for a cough and fever that had developed 2 days after his well visit, and for a persistent diaper rash. He was urinating normally but was having loose stool.
The patient was febrile at 102.4, and his vitals were otherwise normal. On exam, there were erythematous papules and plaques on his penis, scrotum, suprapubic area, and inguinal folds. The rash was confluent on his scrotum with scattered individual papules elsewhere.
He tested positive for influenza A and was treated with Tamiflu for his cough and fever. The rash appeared to be unrelated to the flu as it preceded the flu by 2–3 days. It was treated as a fungal diaper rash with clotrimazole 1 % twice daily and as much diaper-free time as the parents could give him.
Discussion from Dermatology Clinic
Differential Dx
Candidiasis
Irritant dermatitis
Atopic dermatitis
Seborrheic dermatitis
Allergic contact dermatitis
Psoriasis
Granuloma gluteale infantum
Langerhans cell histiocytosis
Acrodermatitis enteropathica (zinc deficiency)
Favored Dx
The female patient has a confluent, erythematous rash typical of irritant diaper dermatitis, as well as satellite papules suggestive of superimposed candidiasis . The male patient’s rash is prominent in the inguinal skin folds and features papules consistent with candidal diaper rash .
Overview
Diaper dermatitis (also called napkin dermatitis or diaper rash) is a nonspecific term used to describe any inflammatory eruption of the skin in the diaper area. Although there are several causes of diaper dermatitis, the general term of diaper dermatitis is most often considered a form of irritant contact dermatitis that presents as a result of prolonged contact with urine and feces. Excessive hydration leads to maceration of the skin, which compromises its barrier function. Additionally, feces and urine increase the pH of the skin, leading to increased fecal enzyme activity and reduced protection from natural skin flora [1]. The area then becomes more susceptible to damage from friction against the diaper and cleansing wipes, as well as damage from increased contact with irritants, such as fecal proteases and lipases, ammonia, and pathogens such as bacteria and yeasts [2]. If irritant diaper dermatitis is not treated, after 3 days, it can then become secondarily infected. Candida albicans is the most common pathogen complicating diaper rash , which leads to candidal diaper dermatitis.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








