, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Erythema migransLymeLyme diseaseBorreliosis Borrelia burgdorferi Borrelia SpirocheteReactive arthritis Ixodes TicksDeer tick Ixodes scapularis BabesiosisVector-borneTick-borneArthralgiaChronic Lyme diseasePost-treatment Lyme disease syndromeAntibioticsDoxycyclineBell’s palsyTrigeminal neuralgia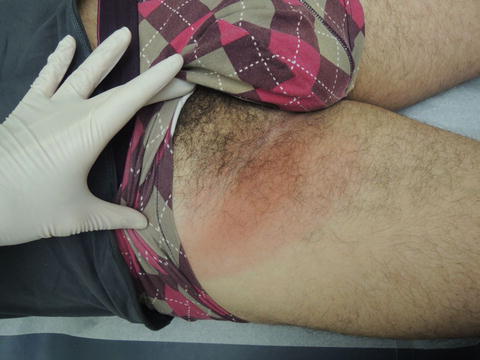
Fig. 43.1
Do not get hung up looking for a perfect target; sometimes this two toned patch is all you will get
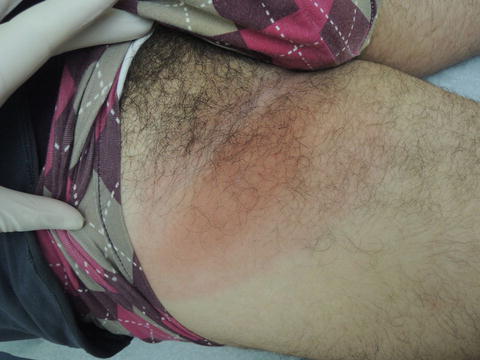
Fig. 43.2
Two-toned inguinal ovoid patch without scale
Primary Care Visit Report
A 38-year-old male with no past medical history presented with a rash in his right inguinal area that had been growing in size. About 10 days prior to his visit, the patient had some mouth sores, a fever, neck stiffness, and a severe headache. The fever and mouth sores resolved; however, the patient’s neck remained stiff and he continued to have intermittent headaches. Then about 6 days prior to his visit, the rash in his right inguinal area developed. It started with one sore spot, which the patient thought might have been an infected hair follicle. He tried putting a warm compress on the rash; however, the rash continued to get bigger. The patient had no known exposure to Lyme disease.
Vitals were normal. On examination, in his right inguinal area there was an 18 cm × 10 cm mildly erythematous blanchable macular lesion. Within that lesion was a 10 cm × 3 cm macule with darker erythema, which was also blanchable. Within the smaller macule, there was a central 2 mm × 2 mm tender, peeling area (3/10 pain). There was no induration, and no abscess noted. The skin texture was irregular.
The rash was treated as cellulitis and the patient was given Bactrim DS twice daily for 10 days. The appearance of the rash was suspicious for Lyme; however, attempts to draw blood in order to test for Lyme titers were unsuccessful, and the patient was advised to return when he was better hydrated. The borders of the rash were marked with permanent marker and the patient was instructed to return if the rash extended beyond its marked borders.
The patient returned 2 days later because the rash continued to spread beyond its original borders. The patient reported no fever or headache, and said the rash was very itchy.
Vitals remained normal. On examination, his right inguinal area had a 22 cm × 13 cm erythematous macular rash with a 17 cm × 8 cm central darker erythematous area. The center of the rash was tender on deep palpation.
The rash was still suspicious for Lyme, so the patient was given a 21-day course of doxycycline 100 mg three times daily, while continuing the Bactrim. Blood was drawn for Lyme titers , complete blood count, liver function tests, and erythrocyte sedimentation rate.
The patient returned 1 day later (now status post three doses of doxycycline and seven doses of Bactrim) because the rash continued to extend beyond its prior borders and the patient was feeling “loopy.” The rash continued to be highly pruritic. The patient also reported fatigue, increased sleep, and waking up groggy, but noted the onset of his fatigue had been gradual over the preceding 2 months.
Vitals remained normal. On examination, the rash in his right inguinal area had extended beyond its previous borders, and was warm and edematous. Three right inguinal lymph nodes were enlarged and tender. Two left inguinal lymph nodes were enlarged and tender. There was no other lymphadenopathy.
The labs were reviewed. The initial Lyme screening was positive but remaining Lyme tests were still pending. His CBC and LFTs were normal. The ESR was elevated.
The patient was referred to the Emergency Room to address ongoing concern about cellulitis and the potential need for IV antibiotics.
The patient went to the ER later that day after he developed a severe headache, neck pain, and back pain in addition to the rash. In the ER, they gave him a 900 mg dose of clindamycin for possible cellulitis. They stopped the Bactrim and sent him home on clindamycin 300 mg twice daily for 7 days for cellulitis, and instructed him to continue the doxycycline (for Lyme). They also gave him a referral to follow up with an Infectious Disease specialist.
The following day, all Lyme titers were received, with Lyme IgM positive and Lyme IgG negative. The rash was improving, and the headache and neck pain were starting to resolve. The clindamycin was discontinued, and the doxycycline 100 mg twice a day was continued for Lyme disease treatment. The patient had a follow-up appointment with an infectious disease doctor scheduled.
One week later, the infectious disease specialist saw the patient and thought perhaps the patient had Lyme and coxsackie, as Lyme disease could not explain the presence of mouth sores. He advised that 10–14 days of doxycycline were adequate to treat Lyme and that the patient did not need to finish the 21-day course. The patient continued to improve, the rash gradually became lighter in color, and the neck pain and headache were resolving.
Discussion from Dermatology Clinic
Differential Dx
Lyme disease
Babesiosis
Human granulocytic anaplasmosis (HGA)
Erysipelas
Cellulitis
Arthropod bite
Southern tick-associated rash illness (STARI, caused by Amblyomma americanum tick)
Favored Dx
The characteristic erythema migrans rash and confirmed titers indicate Lyme disease in this patient.
Overview
Lyme disease is an infectious disease caused by Borrelia spirochete bacteria, lending the disease the alternate name Lyme borreliosis . It was first diagnosed in Lyme, Connecticut in 1977 following a cluster of unusual cases of recurrent arthritis [1].
In the USA, Lyme disease is caused primarily by Borrelia burgdorferi , bacteria which are transmitted by Ixodes ticks of the species Ixodes scapularis and Ixodes pacificus [2]. In Europe and Asia, the disease is also caused by B. afzelii, B. garinii, and other related species [3]. I. scapularis ticks also carry Anaplasma phagocytophilum and Babesia microti, making them vectors for human granulocytic anaplasmosis and babesiosis , infections that sometimes occur with Lyme disease. Ticks must be attached for at least 36 h in order to transmit Lyme disease, with peak infection in the 48–72 h range [2, 4]. The overall risk of developing Lyme disease following a bite with an infected tick is 1–3 %, although this may be higher in endemic areas [4].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








