, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Drug eruptionAnaphylaxisAdverse reactionAllergicAllergyMorbilliformRashAcute reactionAntibioticsPenicillinAmoxicillinHivesUrticarialPrednisoneAntihistamine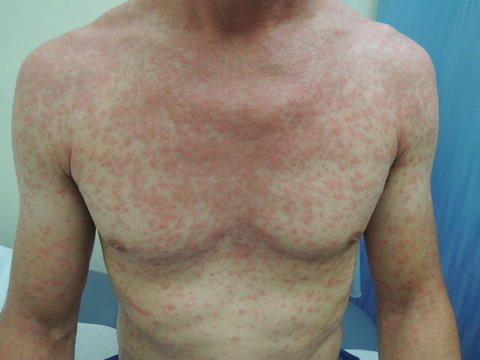
Fig. 38.1
The true “maculopapular” rash involving trunk diffusely
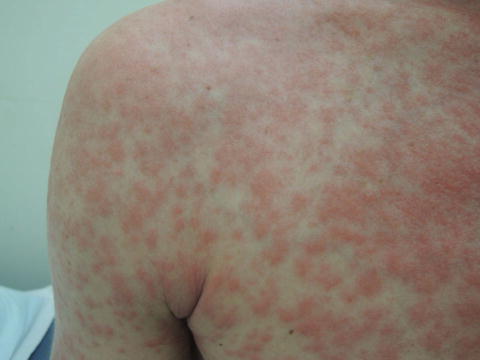
Fig. 38.2
Slight edema and bright red color are characteristic of this condition
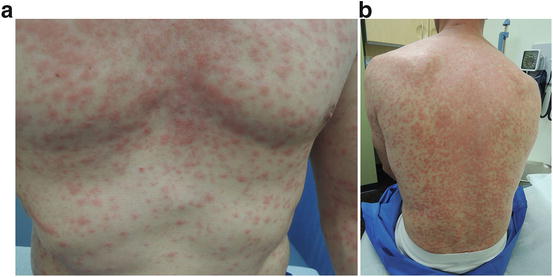
Fig. 38.3
(a and b) Truncal plaque areas of sparing
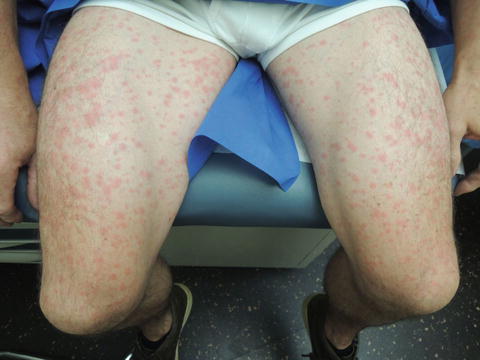
Fig. 38.4
This rash tends to start on the trunk and then spread to extremities
Primary Care Visit Report
A 44-year-old male with no past medical history presented with a rash on his face, chest, back, arms, and legs. One day prior, he had noticed the rash upon waking. It had started on his face and progressively spread down his trunk, and then to his arms and legs. It was not itchy. The day prior was the final day of a 7-day course of amoxicillin (prescribed by a different doctor), which the patient had taken for a tick bite. The patient had no known drug allergies.
Vitals were normal. On exam, there was a diffuse, erythematous morbilliform rash on bilateral arms, bilateral legs, chest, abdomen and back. The rash spared the palms and soles. His face was erythematous but did not have the rash.
The patient was treated for a drug reaction, assuming it was caused by amoxicillin even though the patient had no prior reaction to that medication. Since he had finished the course of amoxicillin already, we did not have to discontinue it or switch to a different antibiotic. We started the patient on a 15-day prednisone taper starting with 80 mg for 3 days, then 60 mg for 3 days, then 40 mg for 3 days, then 20 mg for 3 days, then 10 mg for 3 days. We advised the patient that going forward he should consider himself allergic to penicillins .
Discussion from Dermatology Clinic
Differential Dx
Drug eruption
Erythema multiforme
Viral exanthem
Urticaria
Collagen vascular disease
Favored Dx
Drug-induced eruption is favored given the extent of cutaneous involvement, and onset of rash while taking an antibiotic commonly associated with adverse reactions .
Overview
Acute cutaneous drug reaction is an umbrella term, inclusive of any abnormal skin findings that manifest as a result of an adverse response to a systemic or topical drug. Drug eruptions can occur as a result of immunologic or non-immunologic responses, which include allergies, overdose, dose accumulation, or drug interactions. Consequently, drug eruptions do not necessarily indicate an allergy to a particular medication. Drug-induced eruption describes a sudden-onset rash that coincides with starting a new drug, or occurs in patients who take multiple medications.
Hives and rashes are among the most common adverse reactions to drugs. Cutaneous drug reactions occur in up to 8 % of the population, and 12 % of children treated with antibiotics [1]. According to the American College of Allergy, Asthma , and Immunology, up to 10 % of the population is allergic to β-lactam (penicillin family) antibiotics [2].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








