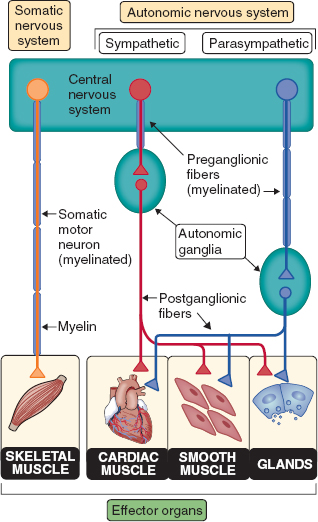
Figure 4-1 Components of central nervous system. (From Preston RR, Wilson TE. Sensory and motor systems. In: Harvey RA, ed. Physiology. Baltimore: Lippincott Williams & Wilkins; 2013:53–90, with permission.)
The Triencephalon (Cerebrum)
The human intellect is considered to be at the level of the cerebrum. It is organized into two cerebral hemispheres and includes the basal ganglia and cerebral cortex. Basal ganglia are a group of nuclei that include the caudate nucleus, putamen, and globus pallidus and, together with the thalamus and cerebral cortex, coordinate motor function. The cerebral cortex is the main terminal for independent thought, consciousness, language, memory, and learning. The function of the cerebral cortex is divided into sensory, motor, and associative areas. The basic sensory and motor functions are responsible for receiving and processing information. The associative function is responsible for the highest level of mental activity, which includes abstract thinking, speech, musical and mathematical skills, as well as intercommunication.

The olfactory nerve is the only cranial nerve whose input reaches the cerebral cortex without going through the thalamus.
The Diencephalon
 VIDEO 4-1
VIDEO 4-1
Pituitary Gland Hormones
The diencephalon contains two structures: thalamus and hypothalamus. The thalamus is involved in motor control as well as with sleep–wake cycles and, if injured, can develop profound coma. The hypothalamus is a major autonomic control center with essential survival functions such as food intake, thirst, water balance, and control of body temperature, blood pressure, and rage. It is the gatekeeper that connects with both the autonomic nerve centers in the brain as well as with the endocrine system. It synthesizes and releases two hormones—oxytocin and antidiuretic hormone—and indirectly controls the release of the pituitary gland hormones.
The Brainstem
The brainstem has several components, namely, the medulla, pons, and midbrain. All the information that passes between the brain and spinal cord traverses the midbrain. Most of the cranial nerves, except cranial nerves I and II, have their origin in the midbrain as well. The cranial nerves provide sensory and motor innervation to the head and neck as well as ensure the primordial senses such as vision, hearing, smell, and taste.
The Cerebellum
The cerebellum is relatively small, but it contains more neurons than the remainder of the brain. This is because it is responsible for coordination of movements such as posture, balance, coordination and speech, overall motor function, as well as learning motor behaviors.
B. The Spinal Cord
The spinal cord is located in the spinal canal and is divided into several regions: cervical, thoracic (dorsal), lumbar, sacral, and coccygeal (Fig. 4-1). The spinal cord is divided into 31 segments that correspond to 31 pairs of spinal nerves, one on each side of the body. Although the spinal cord terminates at L2 vertebral body, the spinal nerves continue caudally until they reach the appropriate dermatome level (cauda equina). The filum terminale marks the tract of regression of the spinal cord. Sensory and motor fibers cross the midline, so in reality the left side of the brain controls the right side of the body and vice versa.
The spinal nerves have components of both sensory afferent and motor efferent fibers and emerge from C2 to S2-3 to control all body functions as well as movement. The sensory component travels toward the spinal cord via a posterior root and enters the spinal canal via the intervertebral foramen (Fig. 4-2). The cell body is located in a spinal ganglion, and the fibers travel upward to synapse with nuclei to the brain or synapse directly with a motor neuron, allowing the cord-mediated reflexes to reflex arc.

FIGURE 4-2 Typical sensory and motor pathways. (From Preston RR, Wilson TE. Sensory and motor systems. In: Harvey RA, ed. Physiology. Baltimore: Lippincott Williams & Wilkins; 2013:53–90, with permission.)
The motor component travels caudally from the brain and synapses with peripheral motor neurons within the spinal cord, exits the spinal column via the anterior root, and travels toward the periphery along the sensory fibers of the spinal nerves.
The spinal cord is organized like a butterfly (Fig. 4-3) with gray matter that contains neuronal cell bodies, dendrites, and unmyelinated axons in the center and white matter that contains myelinated axons surrounding it. The white matter contains bundles of nerve fibers organized into tracts, ascending and descending, which transfer information between the brain and peripheral nervous system. The tracts are named based on their origin and destination (e.g., spinothalamic tract, corticospinal tract, etc.) (see Figs. 37.1 and 37.2). The gray matter is organized into anterior and posterior horns that allow the traveling neurons to synapse. It has commissures that allow information to travel between the two sides.
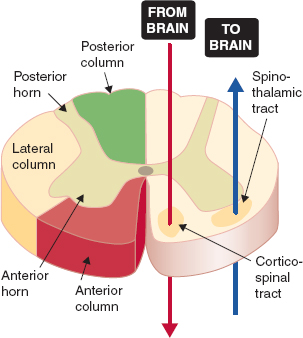
FIGURE 4-3 Organization of the spinal cord. (From Preston RR, Wilson TE. Sensory and motor systems. In: Harvey RA, ed. Physiology. Baltimore: Lippincott Williams & Wilkins; 2013:53–90, with permission.)
Cerebrospinal Fluid
The protection of the CNS is ensured by bone, both at the level of the spinal cord as well as at the level of the brain, three membranes called meninges, as well as a layer of cerebrospinal fluid (CSF). The meninges are comprised of three layers: pia mater (the thinnest), the arachnoid mater (a fibrous membrane), and the thick membrane is dura mater.

The total volume of cerebral spinal fluid is 150 mL, of which 50 mL is in the subarachnoid space of the spinal cord.
The CSF is a sterile colorless fluid produced in the choroid plexus that surrounds the CNS and has a significant function in absorption of shock, providing buoyancy (floatability), allowing some volume changes, and providing homeostasis to ensure a perfect functionality of the CNS.
II. The Autonomic Nervous System
The autonomic nervous system (ANS) is the core of the human organism. It regulates the functions of the visceral organs, including the heart, lungs, gastrointestinal system, hormonal release, as well as body temperature, all of which are not under conscious control.
The ANS is separated into two divisions: sympathetic (adrenergic, SNS), and parasympathetic (cholinergic, PNS) nervous system. These two divisions fine tune organ function and have opposing effects (Table 4-1 and Fig. 4-4) (2,3). The SNS aids the body with fight-or-flight responses and is catabolic (energy expending) system. The role of PNS is quite the opposite; it contributes mainly to body conservation and restoration and is considered a homeostatic or anabolic (energy-conserving) system. The central components of the ANS include the cerebral cortex, hypothalamus, amygdala, stria terminalis, brainstem, and intermediate reticular zone of the medulla.
Table 4-1 Functions of the Autonomic Nervous System
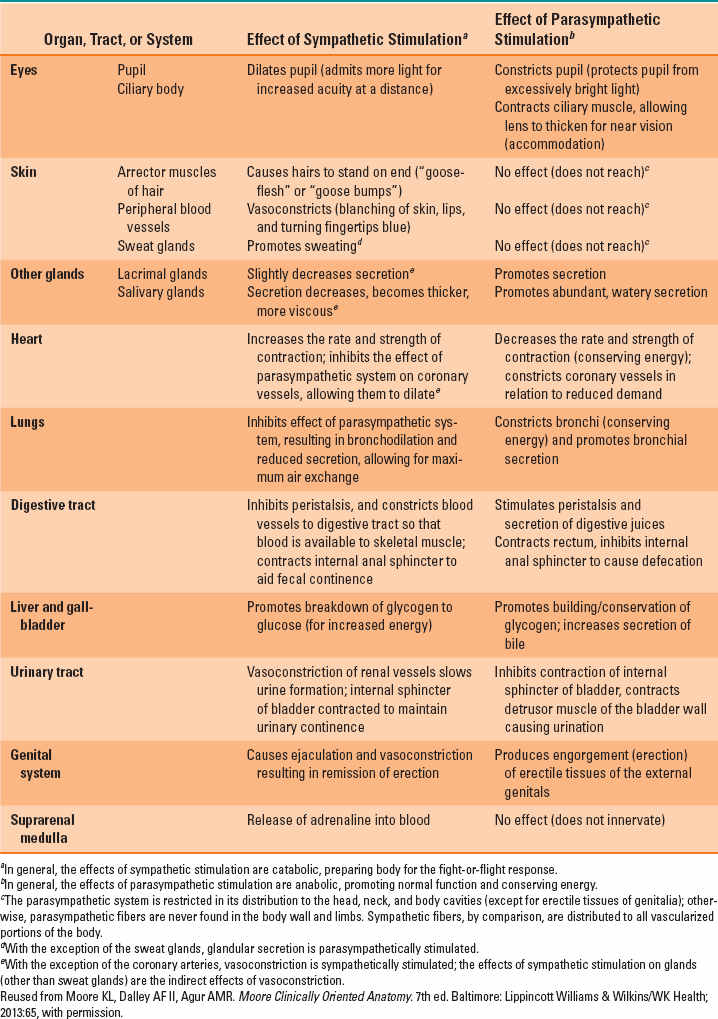
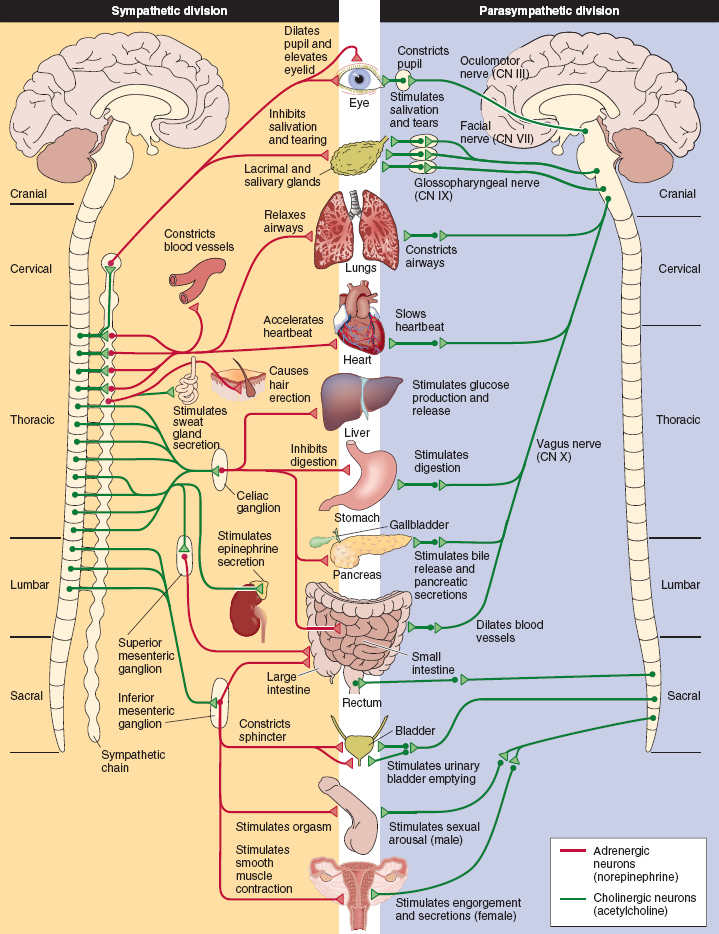
FIGURE 4-4 Organization of the autonomic nervous system. (From Preston RR, Wilson TE. Sensory and motor systems. In: Harvey RA, ed. Physiology. Baltimore: Lippincott Williams & Wilkins; 2013:53–90, with permission.)
Both SNS and PNS have afferent and efferent fibers that close a loop between the spinal cord and visceral organs and determine reflexes that aim toward an equilibrium state of the body.
The afferent pathways have receptors in the visceral organs that are sensitive to mechanical and chemical stimuli as well as temperature variations. The impulses are transmitted along the somatic or autonomic nerves through the dorsal roots toward the spinal cord or the cranial nerves toward the brainstem.
The afferent fibers play an important role in both conducting visceral pain impulses and regulating visceral function. The difference between the ANS and somatic innervation is that the transmission of the impulses from the CNS toward the effector organs is conducted by connecting two multipolar neurons for both divisions of the ANS. Although the somatic motor innervation contains only one neuron (Fig. 4-5). The ANS contains efferent fibers and ganglia that are clustered into two separate groups, the thoracolumbar (for SNS) from T1-L2 and craniosacral for PNS (Fig. 4-4). The preganglionic axons are short, myelinated, and cholinergic and exit the spinal cord and enter the white rami communicans that connect with prevertebral or paravertebral ganglia. The postganglionic axons continue through the gray rami communicans and continue together with blood vessels and nerves toward the end organs. These axons are long, unmyelinated, and primarily adrenergic with the exception of sweat glands, which are cholinergic. The PNS exits the CNS via the cranial nerves III, VII, IX, and X as well as through the sacral roots. The preganglionic fibers are myelinated, cholinergic, and fairly long, because the ganglia are located close to the end organ. The postganglionic fibers are short and cholinergic.