, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
AllergyOccupational dermatitisAllergic contact dermatitisSkin allergyAllergenIrritantEdemaType 4 hypersensitivityType IV hypersensitivityT CellT Cell-mediatedAllergic reactionNickelFormaldehydeThimerosalCosmeticsPatch testingPatch testCorticosteroidPrednisone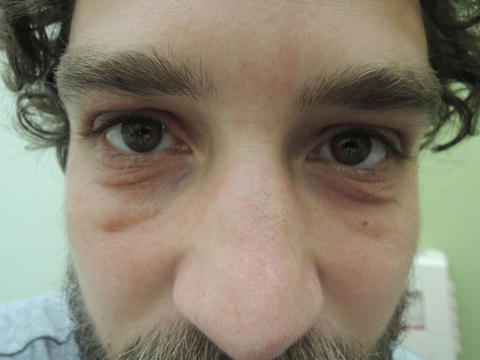
Fig. 46.1
Periocular distribution is one of the more common presentations for this condition
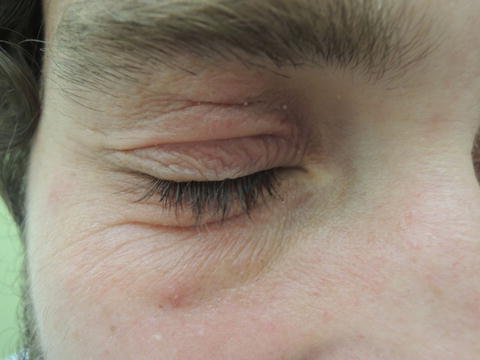
Fig. 46.2
Accentuated skin markings, edema, and redness along with notable itch are hallmarks for this dermatitis
Primary Care Visit Report
A 33-year-old male with past medical history of thrombophilia, on warfarin, presented with a rash around his eyes starting 1 week prior. He tried using some moisturizer, as well as some over-the-counter eye drops. He also had some erythromycin ophthalmic ointment 0.5 % that he applied to the skin beneath his eyes. None of these things helped.
The patient reported no new skin products and had no known allergens .
Vitals were normal. On exam, on his bilateral infra- and supra-orbital areas there was an erythematous and edematous macular rash. The right inferior infra-orbital area had a 1 mm yellow papule.
The differential considered was contact dermatitis vs. mild blepharitis. To cover for a possible bacterial component of blepharitis as well as to treat a possible contact dermatitis, TobraDex (tobramycin and dexamethasone) 0.3–0.1 % ointment was prescribed twice daily for 7 days.
Discussion from Dermatology Clinic
Differential Dx
Allergic contact dermatitis
Irritant dermatitis
Atopic dermatitis
Favored Dx
Allergic contact dermatitis (ACD) can be difficult to definitively diagnose when there is no identified allergen . However, eyelids are a common area for ACD, and edema is a strong diagnostic clue. In this case, ACD is the favored diagnosis.
Overview
Allergic contact dermatitis is a T cell -mediated type IV (delayed hypersensitivity) reaction that occurs after the skin comes in contact with an allergen. As with other type IV hypersensitivity reactions, the skin must have had prior exposure to the offending substance in order to become sensitized. Subsequent exposure leads to a hypersensitivity reaction that develops over the course of 2–3 days.
ACD accounts for 20 % of new cases of contact dermatitides, with the remaining 80 % being cases of irritant contact dermatitis [1]. A large retrospective study estimated the prevalence of contact allergies in the general population to be 21.2 % [2]. The prevalence varies by geographic region, due to differences in exposure, cultural customs, and environmental differences. Workers in certain occupations, especially hairdressers, barbers, metal workers, and health care professionals, are at higher risk for developing contact allergies [3, 4]. Of over 3700 chemicals implicated as causative agents of contact allergy, among the most common are nickel , thimerosal (antiseptic and antifungal agent), fragrance mix, neomycin, and formaldehyde (used as a preservative in many cosmetics ) [1, 2, 4, 5]. The estimated prevalence of contact allergy to cosmetics is 6 % in the general population [5]. Nickel allergies are more prevalent in women, and have been associated with a history of atopic dermatitis in women [2]. Women with pierced ears tend to present with nickel allergies more often than women without pierced ears [2].
Presentation
Allergic contact dermatitis presents as an eczematous rash that can be severely pruritic. The rash tends to have sharply demarcated borders and is localized to the area exposed to the offending allergen . Any geometric or linear distribution of lesions may reveal a plant allergy, as the shapes are consistent with the area of skin that would come in contact with the plant. It is possible for the rash to develop beyond the site of exposure if the allergen is transferred by hands or clothing. Eyelids are susceptible to this kind of transfer, possibly because the thinner skin of the eyelids is more susceptible to reaction [1]. Eyelid ACD typically presents with edema. More severe cases of ACD may be vesicular or bullous.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








