Type of procedures
Ileostomy
Colostomy
Urostomy
Abdominoperineal resection (APR)
√
Hartmann’s
√
Low anterior resection
√
Ultra-low anterior resection
√
Proctocolectomy
√
Cystectomy
√
Table 15.2
Type of stoma and description of output consistency
Type of stoma | Ileostomy | Colostomy | Urostomy |
|---|---|---|---|
Description of output | Watery to loose faecal matter | Formed faecal matter | Urine |
End | 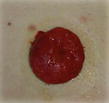 | 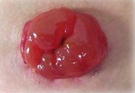 | 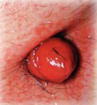 |
Loop | 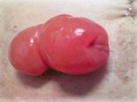 | 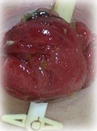 | |
Double-barrel | 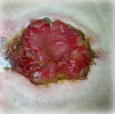 |
The need for a stoma is often regarded as a drastic changing event which can be traumatising for patients both psychologically and physically (Gesaro 2012). An ostomist’s journey is apprehensive with many difficulties to face, requiring significant adaptation. Challenges encountered have an impact on all aspects of an ostomist’s life, including psychosocial, spiritual, physical and sexual health and cultural and religious beliefs. Thus, a transdisciplinary approach in the delivery of stoma care would provide much benefit in dealing with these challenges.
Transdisciplinary stoma care encompasses the collaborative input from various healthcare professionals’ different specialties for holistic care. This team comprises a colorectal nurse specialist, surgeon, oncologist, social worker, dietician, pharmacist, caregiver and the patient (Fig. 15.1). Each member of the team plays an important role with the common goals of improving an ostomist’s outcome, rehabilitation to the premorbid status and achieving self-care. Effective communication between the healthcare team and the patient or caregiver is crucial to ensure continual and holistic stoma care, enhancing each dedicated role in the team for holistic stoma care. In this chapter, the delivery of stoma care in a transdisciplinary approach will be discussed.
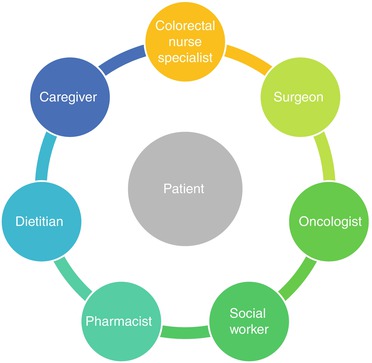

Fig. 15.1
Transdisciplinary stoma team
15.2 Roles of Healthcare Professionals
Many aspects of healthcare involve a collaboration between doctors and allied healthcare professionals. In transdisciplinary stoma care, each member of the team plays a vital role in the provision of comprehensive stoma care.
15.2.1 Medical Professionals
The surgeon is traditionally seen as the team leader and primary decision maker for the surgical patient. In a transdisciplinary team, the surgeon continues to manage the surgical aspects of patient care but takes a step back and actively listens and incorporates the input from the other members of the team.
The decision for a stoma is ultimately a surgical decision. The need for a stoma may be required given the nature of the surgery but may also be an intraoperative decision. If there is a possible or definite need for a stoma, the surgeon would counsel the patient appropriately but should also highlight this to the transdisciplinary team, allowing for various members of the team to initiate contact with the patient preoperatively. This will aid in the patient’s subsequent acceptance of the stoma and accelerate their ability to provide self-care.
15.2.2 Medical Social Worker (MSW)
The medical social worker plays an important role in patients who have financial, caregiver or social issues and if psychosocial support is required. Elderly patients may require step-down facilities for rehabilitation postoperatively, and the MSW is required for the consideration of step-down options, for instance, community hospital or day rehabilitation services. For patients who stay alone, the MSW could arrange an interim caretaker for a few weeks to help boost the patient’s confidence in self-care.
The MSW can provide counselling and psychosocial support for patients and family, for both stoma care and especially in patients with terminal disease. The MSW can provide a listening ear while spending time with the patient and may link the patient up with an appropriate support group. Financial assistance for stoma care can also be arranged. In our local setting, an application can be made for the provision of stoma supplies from a charitable organisation – Singapore Cancer Society. Thus, the MSW works together with the colorectal nurse specialist, ensuring that appropriate appliances can be provided to patients with support from respective institution as required.
15.2.3 Dietician
The dietician serves the role of providing dietary advice and dietary guide for stoma patients. In our institution, the dietician counsels for small frequent meals with low fibre during the initial postoperative period for colonic resections. In patients with high ileostomy output, the dietician and pharmacist work together to provide education on usage of oral rehydration salt (ORS) as salt replacement and on appropriate fluid intake. Specific dietary plans may be required in patients with premorbid medical issues such as end-stage renal failure or heart failure. Supplements may be introduced to patients who are malnourished with the aim to increase caloric intake.
15.2.4 Pharmacists
In patients with high ileostomy output, education to the patient and caregiver by the pharmacist on the use of ORS (6 sachets in 1 l of water) is required. The surgeon may also initiate antidiarrhoeal medications such as loperamide. The pharmacist is required to provide counselling on the titration of loperamide to the patient and caregiver to prevent overdosing. Alternatively, the pharmacist should educate the patient to drink isotonic water to replace the electrolytes lost from the ileostomy output. Involvement from stoma care nurses includes educating patients to measure their output and titrate their medication accordingly after discharge.
Elderly patients with multiple medical issues may have numerous medications and supplements. Medication reconstitution is done by pharmacists to help them identify medications which are stopped and in the introduction of new medications. Furthermore, a medication pillbox is a useful aid for elderly patients to ensure compliance to their long-term medications. Advices on the effect of specific medications on the colour of stools should be provided to the patient and caregiver to allay anxiety and prevent unnecessary readmissions.
15.2.5 Colorectal Nurse Specialist
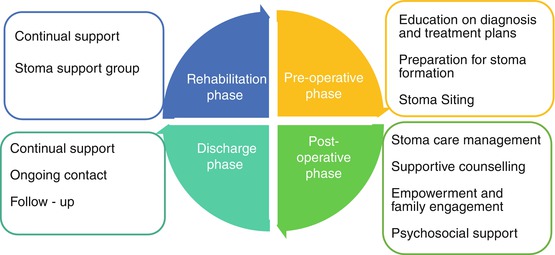
The colorectal nurse specialist plays the role of the facilitator and ensures smooth collaboration between team members for the care of the ostomist from preoperative to postoperative phases. Moreover, the provision of care does not end upon discharge from the hospital. The continuation of stoma care with follow-up after discharge by the nurse is fundamental in ensuring all needs are taken care of (Borwell 2009). Figure 15.2 illustrates the role of the colorectal nurse specialist in different phases of an ostomist’s preparation to a life with stoma. The nurse serves as a coordinator ensuring that the team provides the delivery of holistic care for ostomists.
Case Study
We present the journey of Mr. J., a 28-year-old gentleman with familial adenomatous polyposis (FAP) and anal cancer, to illustrate the role of transdisciplinary team. Mr. J. underwent neoadjuvant chemotherapy prior to surgery, with the aim of curative resection through a total proctocolectomy with an end ileostomy. Through the different phases of preparation, he completed the journey to become an ostomist with the transdisciplinary team.
15.3 Preoperative Phase
The preoperative phase marks the commencement of an ostomist’s journey towards living with a stoma. The goal for preoperative care is to prepare patients to cope with stoma physically and psychologically, allowing them to anticipate the subsequent phases. This also increases acceptance of a stoma and reduces the impact on body image (Slater 2010).
15.3.1 Preoperative Counselling Session
Prior to an elective surgery, a planned session between the patient and the colorectal nurse specialist serves as a valuable platform to build rapport and establish the foundation for a smooth-sailing transition to living with a stoma (Slater 2010). Not only does it provides an opportunity for the patient to raise concerns or difficulties, but also aids in maintaining ownership of health (Borwell 2009). Furthermore, it allows the nurse to perform an initial assessment which encompasses biological, physical and psychosocial aspects and to gain an understanding of the patient’s expectation.
The initial assessment is important as every individual differs in their concerns, needs and expectations. During preoperative counselling and consultation, the colorectal nurse specialist will bring the patient through the diagnosis and proposed treatment plan such as surgery, chemotherapy and need for the creation of stoma. Details on the management of stoma and expectation of postoperative changes will also be further discussed with the patient. Table 15.3 states the components of preoperative counselling. The use of multimedia such as brochures, flip charts and video or the showcasing of stoma pouches is used to engage the patient. Provision of detailed information will allow the patient to have a better understanding of the effects of surgery and stoma. Moreover, it offers better awareness and allays anxiety.
Table 15.3
Components of preoperative counselling
Diagnosis and prognosis |
Preparation for life with stoma |
Type and effects of surgery |
Communication |
Psychological/sexual awareness |
Future care (chemotherapy) |
Stoma siting |
A preoperative counselling session was arranged with the surgeon, colorectal nurse specialist and Mr. J. present. The surgeon discussed the operation including the creation of a stoma and its potential complications with the aid of illustrations for better understanding. The colorectal nurse specialist explored his understanding of the operation and stoma creation and clarified doubts. Moreover, the colorectal nurse specialist provided him an alternative date for a second preoperative counselling session to prevent information overload and allow him time to think through and process the information.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree