, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
FungusFungalYeastInfectionBenignTinea versicolorHyperpigmentationHypopigmentationAntifungal Malassezia 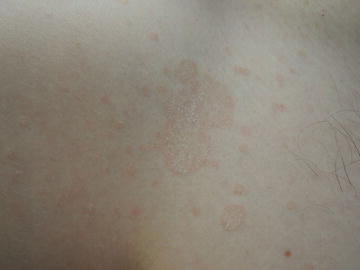
Fig. 21.1
Thin pink or brown plaques with fine scale may be coalescent or occasionally guttate (drop-shaped)
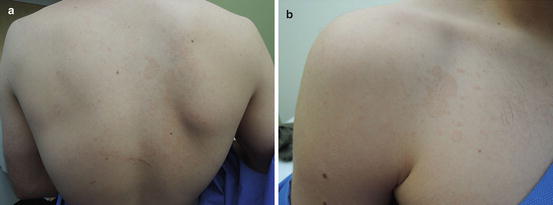
Fig. 21.2
(a and b) Chest and back are most commonly affected
Primary Care Visit Report
A 24-year-old male with no prior medical history presented with a rash on his chest, shoulders and back. The rash started in two spots on his left shoulder about 8 months prior. About 1 week prior to the visit, it spread to his chest. He did not report pruritus. He had not applied anything to the rash yet.
Vitals were normal. On exam, on the patient’s chest, back, and flank, there were multiple scattered erythematous macular and papular lesions with irregular shapes and varied sizes. These lesions had well-delineated borders with mild central scale.
This was treated as tinea corporis based on the well-circumscribed lesions with central scale. The patient was prescribed 2 % ketoconazole cream once daily for 14 days.
Discussion from Dermatology Clinic
Differential Dx
Tinea versicolor
Tinea corporis
Pityriasis rosea
Confluent and reticulated papillomatosis
Early stages of mycosis fungoides, a type of T-cell lymphoma
Favored Dx
Considering the patient’s age, persistence of the rash, location of macules, and minimal pruritus, the favored diagnosis, as reclassified by dermatology, is tinea versicolor. Tinea versicolor is distinct from tinea corporis, and differs from all other tinea diseases (e.g., tinea pedis, tinea capitis) in that it is not a dermatophyte infection. However, they are treated in similar manners, with topical and oral antifungals , so in this case the 2 % ketoconazole would have been the appropriate treatment anyhow.
Overview
Tinea versicolor, also called pityriasis versicolor , is a benign superficial fungal infection characterized by scaly, hyperpigmented or hypopigmented lesions commonly found on the back, chest, and neck. Tinea versicolor is caused by an overgrowth of the lipophilic Malassezia yeast , which is a component of the natural skin flora.
Tinea versicolor is a common condition, most prevalent in tropical and sub-tropical climates, although seen in temperate climates as well. It can be recurrent, and may be seen waning in winter months and returning during the summertime.
Tinea versicolor is more commonly seen in males [1] and tends to occur during young adulthood [2]. It is not contagious, rather the yeast overgrows when favorable conditions are met. Exogenous factors contributing to its development include high heat and high humidity. Internal factors that favor this fungal overgrowth are greasy skin, excessive sweating, hereditary factors, corticosteroid treatment, and immunodeficiency [3]. To that end, people who exercise frequently or work physical jobs may be at higher risk of developing tinea versicolor.
Presentation
Tinea versicolor is typically found on the trunk, neck, and upper arms. Although it may not always be the case, tinea versicolor presents mainly as a hypopigmented rash on darker skin [1], and a hyperpigmented brown or red rash on lighter Caucasian skin. The lesions generally feature a fine scale and begin as round or oval macules or papules (if scaly), and may grow and coalesce to form larger patches or plaques. Some patients may present complaining of mild pruritus, but for most the condition is asymptomatic [2].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








