CHAPTER 17
Foreign Body, Conjunctival
Presentation
Low-velocity projectiles, such as windblown dust particles, can be stuck under the upper tarsal plate, loose in the tear film, or lodged in a conjunctival sac. The patient will feel a foreign-body sensation but may not be very accurate in locating the foreign body by sensation alone. On examination, normally occurring white papules inside the lids can be mistaken for foreign bodies, and transparent foreign bodies can be invisible in the tear film (until outlined by fluorescein dye). Most particles are easily identified as dark specks, which are most often found under the upper eyelid.
What To Do:
 Make sure that the mechanism of injury did not include high-velocity debris (e.g., hammering metal on metal, drilling, grinding, or exposure to explosive forces).
Make sure that the mechanism of injury did not include high-velocity debris (e.g., hammering metal on metal, drilling, grinding, or exposure to explosive forces).
 Instill topical anesthetic drops (proparacaine [Ophthaine, Alcaine, Ophthetic] or tetracaine [Pontocaine]). This should relieve discomfort and any uncontrollable blepharospasm.
Instill topical anesthetic drops (proparacaine [Ophthaine, Alcaine, Ophthetic] or tetracaine [Pontocaine]). This should relieve discomfort and any uncontrollable blepharospasm.
 Perform a best-corrected visual acuity examination and funduscopy; examine the cornea, anterior chamber, and tear film with a bright light (best done with a slit lamp), and then examine the conjunctival sacs.
Perform a best-corrected visual acuity examination and funduscopy; examine the cornea, anterior chamber, and tear film with a bright light (best done with a slit lamp), and then examine the conjunctival sacs.
 To examine the lower sac, pull the lower lid down with your finger while the patient looks up (Figure 17-1).
To examine the lower sac, pull the lower lid down with your finger while the patient looks up (Figure 17-1).
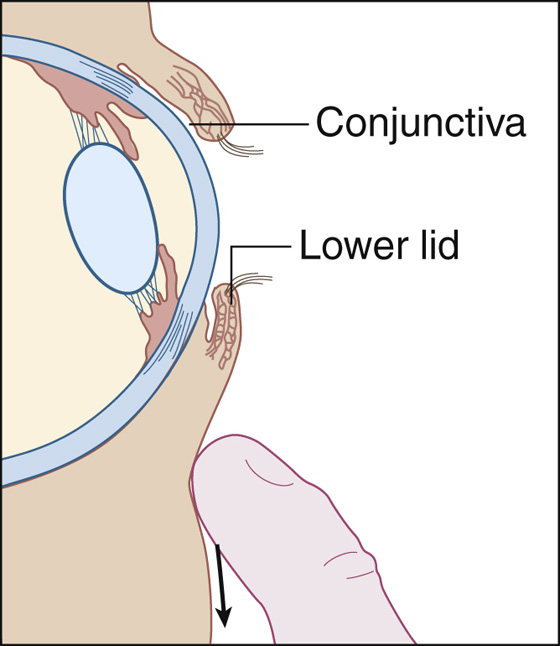
Figure 17-1 The patient looks up while the lid is pulled down.

 To examine the upper sac; hold the proximal portion of the upper lid down with a cotton-tipped swab while pulling the lid out and up by its lashes, everting most of the lid, as the patient looks down. Push the cotton swab downward to help turn the upper conjunctival sac “inside out” (Figure 17-2, A to C). The stiff tarsal plate usually keeps the upper lid everted after the swab is removed, as long as the patient continues looking downward. Looking up will reduce the lid to its usual position.
To examine the upper sac; hold the proximal portion of the upper lid down with a cotton-tipped swab while pulling the lid out and up by its lashes, everting most of the lid, as the patient looks down. Push the cotton swab downward to help turn the upper conjunctival sac “inside out” (Figure 17-2, A to C). The stiff tarsal plate usually keeps the upper lid everted after the swab is removed, as long as the patient continues looking downward. Looking up will reduce the lid to its usual position.
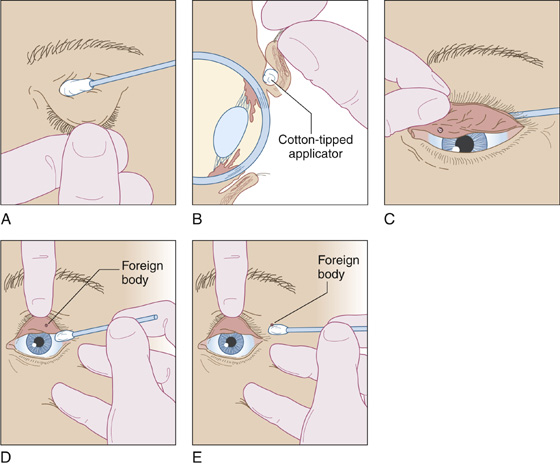
Figure 17-2 A, A cotton-tipped applicator is placed above the upper lid. B, Lid eversion with the patient looking downward. C, Push down on the applicator to reveal a foreign body hidden under the tarsal plate. D and E, The moistened applicator touches the foreign body, lifting it away.
 A loose foreign body usually will adhere to a moistened swab lightly touched to the surface of the conjunctiva and is thereby removed (Figure 17-2, D and E), or it can be washed out by copious irrigation with saline.
A loose foreign body usually will adhere to a moistened swab lightly touched to the surface of the conjunctiva and is thereby removed (Figure 17-2, D and E), or it can be washed out by copious irrigation with saline.
 Perform a fluorescein examination to disclose any corneal abrasions caused by the foreign body. These vertical scratches occur when the lid closes over a coarse object and should be treated as described in Chapter 16.
Perform a fluorescein examination to disclose any corneal abrasions caused by the foreign body. These vertical scratches occur when the lid closes over a coarse object and should be treated as described in Chapter 16.
 Follow with a brief saline irrigation to remove possible remaining fragments.
Follow with a brief saline irrigation to remove possible remaining fragments.
What Not To Do:
 Do not overlook a foreign body lodged in the deep recesses of the upper conjunctival sac.
Do not overlook a foreign body lodged in the deep recesses of the upper conjunctival sac.
 Do not overlook an eyelash that has turned in and is rubbing on the surface of the eye. Sometimes a lash may be sticking out of the inferior lacrimal punctum. Extract any such lashes.
Do not overlook an eyelash that has turned in and is rubbing on the surface of the eye. Sometimes a lash may be sticking out of the inferior lacrimal punctum. Extract any such lashes.
 Do not overlook an embedded or penetrating foreign body. Maintain a high index of suspicion with high-velocity injuries or when there is periorbital tissue damage. Radiography or CT examination should be performed for suspected metallic intraocular foreign bodies, whereas MRI should be obtained to rule out a nonmetallic object.
Do not overlook an embedded or penetrating foreign body. Maintain a high index of suspicion with high-velocity injuries or when there is periorbital tissue damage. Radiography or CT examination should be performed for suspected metallic intraocular foreign bodies, whereas MRI should be obtained to rule out a nonmetallic object.
 Do not overlook a corneal abrasion. Fluorescein staining will uncover these superficial lesions.
Do not overlook a corneal abrasion. Fluorescein staining will uncover these superficial lesions.
Discussion
Good first aid (providing copious irrigation, pulling the upper lid down over the lower lid, and avoiding rubbing of the eyes) will take care of most ocular foreign bodies. The history of injury with a high-velocity fragment, such as a metal shard chipped off from a hammer or chisel, should raise suspicion of a penetrating foreign body, and radiographs or CT scans should be obtained.
The signs associated with an intraocular foreign body can be extremely subtle, causing only slight erythema and local discomfort. Visual acuity often is markedly decreased, but normal visual acuity is possible. There may be conjunctival chemosis, hyphema, localized cataract, or an iris injury with resultant pupil deformity. MRI should be used to locate radiolucent objects but should never be used to image magnetic foreign bodies.
Techniques for conjunctival foreign body removal can also be applied to locating a displaced contact lens (see Chapter 23), but be aware that fluorescein dye absorbed by soft contact lenses fades slowly.
When eyelids become glued shut with cyanoacrylate (Crazy Glue or Super Glue), it is usually impossible to perform a complete eye examination or even gently separate the eyelids. Simply apply an antibacterial ointment and, if more comfortable for the patient, patch the eye. Spontaneous opening will occur in 1 to 2 days, and a more thorough examination can be performed at that time if any discomfort persists.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



