CHAPTER 173
Partial-Thickness (Second-Degree) Burns and Tar Burns
Presentation
Partial-thickness burns can occur in a variety of ways. Spilled or splattered hot water and grease are among the most common causes, along with hot objects, explosive fumes, and burning (volatile) liquids. The patient will complain of excruciating pain, and the burn will appear erythematous with vesicle formation. Some of these vesicles or bullae may have ruptured before the patient’s arrival, whereas others may not develop for 24 hours. Tar burns are special in that the tar adheres aggressively to the burned skin and therefore makes the burns look very unsightly.
What To Do:
 To stop the pain, immediately cover the burned area with sterile towels that have first been soaked in iced normal saline, or just use cold tap water. Continue irrigating the burn with the iced or cold solution for the next 20 to 30 minutes or until the patient can remain comfortable without the cold compresses.
To stop the pain, immediately cover the burned area with sterile towels that have first been soaked in iced normal saline, or just use cold tap water. Continue irrigating the burn with the iced or cold solution for the next 20 to 30 minutes or until the patient can remain comfortable without the cold compresses.
 Determine the mechanism of injury and the extent and severity of the burn. The patient’s palm represents approximately 1% of his total body surface and can be used to estimate the total area of the body surface burned. Examine the patient for any associated injuries. Transfer to a burn center and/or initiate generous fluid resuscitation if there are third-degree (full-thickness) burns over 5% of the total body surface, second-degree (partial-thickness) burns (alone or in combination with the third-degree burns) of over 10% to 15% of the total body surface (5% to 10% in children under 10 years of age), or extensive burns involving the face, hands, feet, joints, or genitalia. Special consideration should be given to the elderly or patients with significant comorbidity.
Determine the mechanism of injury and the extent and severity of the burn. The patient’s palm represents approximately 1% of his total body surface and can be used to estimate the total area of the body surface burned. Examine the patient for any associated injuries. Transfer to a burn center and/or initiate generous fluid resuscitation if there are third-degree (full-thickness) burns over 5% of the total body surface, second-degree (partial-thickness) burns (alone or in combination with the third-degree burns) of over 10% to 15% of the total body surface (5% to 10% in children under 10 years of age), or extensive burns involving the face, hands, feet, joints, or genitalia. Special consideration should be given to the elderly or patients with significant comorbidity.
 Consider and report any burn injuries suggestive of child abuse. A supposed mechanism of injury that does not fit the injury or is not consistent with the child’s level of development warrants investigation. Specific injuries that usually should be reported as suspected abuse include burns to the face, dorsum of the feet, and genitalia; cigarette burns; imprint burns, such as those from a hot iron or grill; stocking burns with a sharp line of demarcation from immersion in hot water; or glove burns to the hand as well as any circumferential burns or symmetric extremity burns.
Consider and report any burn injuries suggestive of child abuse. A supposed mechanism of injury that does not fit the injury or is not consistent with the child’s level of development warrants investigation. Specific injuries that usually should be reported as suspected abuse include burns to the face, dorsum of the feet, and genitalia; cigarette burns; imprint burns, such as those from a hot iron or grill; stocking burns with a sharp line of demarcation from immersion in hot water; or glove burns to the hand as well as any circumferential burns or symmetric extremity burns.
 Provide the patient with any necessary tetanus prophylaxis (see Appendix H).
Provide the patient with any necessary tetanus prophylaxis (see Appendix H).
 Administer potent pain medication (e.g., hydromorphone [Dilaudid], morphine, fentanyl [Sublimaze]) as required.
Administer potent pain medication (e.g., hydromorphone [Dilaudid], morphine, fentanyl [Sublimaze]) as required.
 The providers participating in débridement and wound dressing should wear sterile gowns, gloves and masks, generally following “universal precautions” for wound care. This protects the wounds from potential infection and protects the providers as well.
The providers participating in débridement and wound dressing should wear sterile gowns, gloves and masks, generally following “universal precautions” for wound care. This protects the wounds from potential infection and protects the providers as well.
 If the bullae or vesicles are not perforated, they should be left intact. With small burns, patients can be sent home to continue cold compresses for comfort. Otherwise, these vesicles should be protected from future rupture and contamination with a bulky sterile dressing.
If the bullae or vesicles are not perforated, they should be left intact. With small burns, patients can be sent home to continue cold compresses for comfort. Otherwise, these vesicles should be protected from future rupture and contamination with a bulky sterile dressing.
 Open bullae or vesicles that are fresh and uncontaminated can be easily pulled back into their original position to cover the burn surface (Figure 173-1) and then may be left in place as a physiologic burn dressing. This should be covered with nonadherent oil emulsion gauze, such as Adaptic, and then protected with a bulky sterile dressing (e.g., fluffed 4 × 4 gauze pads wrapped with Kerlex). This will hold the thin layer of epithelium in place and absorb any leaking plasma while protecting the burn from contamination and providing comfort.
Open bullae or vesicles that are fresh and uncontaminated can be easily pulled back into their original position to cover the burn surface (Figure 173-1) and then may be left in place as a physiologic burn dressing. This should be covered with nonadherent oil emulsion gauze, such as Adaptic, and then protected with a bulky sterile dressing (e.g., fluffed 4 × 4 gauze pads wrapped with Kerlex). This will hold the thin layer of epithelium in place and absorb any leaking plasma while protecting the burn from contamination and providing comfort.
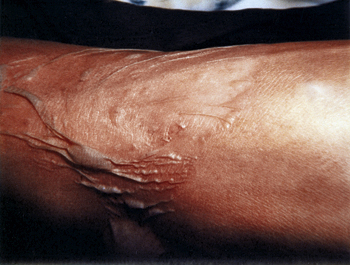
Figure 173-1 Open second-degree burn bullae may be left in place as a physiologic burn dressing.
 Bullae or vesicles that are open and contaminated, old, or whose walls are so friable and damaged that they cannot be used as a biologic burn dressing should be completely débrided. Then the burn surface should be flushed with saline. Using fine scissors and forceps, strip away any of this loose epithelium from the burn.
Bullae or vesicles that are open and contaminated, old, or whose walls are so friable and damaged that they cannot be used as a biologic burn dressing should be completely débrided. Then the burn surface should be flushed with saline. Using fine scissors and forceps, strip away any of this loose epithelium from the burn.
 For small clean burns that have been débrided, covering them with a transparent film of polyurethane with an adhesive coating (OpSite, Bioclusive, Tegaderm) provides a moist environment that enhances reepithelization and is comfortable. There needs to be intact skin surrounding the area being dressed so that the dressing will adhere. Exudate collects under these film dressings and frequently leaks out. An outer absorbent dressing with dressing changes is required when this occurs. The synthetic film is left in place.
For small clean burns that have been débrided, covering them with a transparent film of polyurethane with an adhesive coating (OpSite, Bioclusive, Tegaderm) provides a moist environment that enhances reepithelization and is comfortable. There needs to be intact skin surrounding the area being dressed so that the dressing will adhere. Exudate collects under these film dressings and frequently leaks out. An outer absorbent dressing with dressing changes is required when this occurs. The synthetic film is left in place.
 For larger débrided areas, a simple dressing with oil emulsion gauze (Adaptic) covered with sterile fluffed gauze is an effective acceptable burn dressing. A new soft silicone dressing (Mepitel, Mölnlycke Healthcare, Norcross, Ga.) can also be applied directly to the burn, with an overlying sterile dressing that will provide adequate padding to exclude voids beneath this polyamide net. Mepitel may be left in place for up to 7 to 10 days, but the outer absorbent layer should be changed more frequently as required. One study showed that burn wounds covered with Mepitel healed significantly faster with less eschar formation and less pain than with the standard control dressings.
For larger débrided areas, a simple dressing with oil emulsion gauze (Adaptic) covered with sterile fluffed gauze is an effective acceptable burn dressing. A new soft silicone dressing (Mepitel, Mölnlycke Healthcare, Norcross, Ga.) can also be applied directly to the burn, with an overlying sterile dressing that will provide adequate padding to exclude voids beneath this polyamide net. Mepitel may be left in place for up to 7 to 10 days, but the outer absorbent layer should be changed more frequently as required. One study showed that burn wounds covered with Mepitel healed significantly faster with less eschar formation and less pain than with the standard control dressings.
 Although unnecessary for most superficial partial-thickness burns in outpatients, silver sulfadiazine (Silvadene) cream is most commonly used to cover these open burn wounds. When this cream is used, it is only necessary to provide an absorbent protective gauze dressing over the burn area (without Adaptic); alternatively, the area can be left open and gently washed twice daily, followed by reapplication of the cream.
Although unnecessary for most superficial partial-thickness burns in outpatients, silver sulfadiazine (Silvadene) cream is most commonly used to cover these open burn wounds. When this cream is used, it is only necessary to provide an absorbent protective gauze dressing over the burn area (without Adaptic); alternatively, the area can be left open and gently washed twice daily, followed by reapplication of the cream.
 For greater patient convenience, an alternative is to use a silver-impregnated dressing (Acticoat), which is occlusive, promotes a moist healing environment, and eliminates the need for frequent dressing changes. The Acticoat dressing is placed on the wound and is kept moist by applying sterile water, which activates the release of the silver ions into the wound. An outer layer of gauze bandage, such as Kerlix or Kling, can be used to protect the wound and keep the Acticoat in place. The Acticoat dressing does not have to be changed more frequently than every 3 days.
For greater patient convenience, an alternative is to use a silver-impregnated dressing (Acticoat), which is occlusive, promotes a moist healing environment, and eliminates the need for frequent dressing changes. The Acticoat dressing is placed on the wound and is kept moist by applying sterile water, which activates the release of the silver ions into the wound. An outer layer of gauze bandage, such as Kerlix or Kling, can be used to protect the wound and keep the Acticoat in place. The Acticoat dressing does not have to be changed more frequently than every 3 days.
 Biobrane collagen Silastic is an alternative synthetic dressing that is designed to be placed tightly against the wound with a compressive gauze dressing wrapped over it. Within 2 days, as long as the wound is clean and has no seroma formation, the collagen side of the dressing adheres to the surface of the burn and effectively seals it. The dressing acts as a skin substitute and allows the underlying skin to heal and reepithelialize more comfortably. Biobrane may be left in place for 1 month.
Biobrane collagen Silastic is an alternative synthetic dressing that is designed to be placed tightly against the wound with a compressive gauze dressing wrapped over it. Within 2 days, as long as the wound is clean and has no seroma formation, the collagen side of the dressing adheres to the surface of the burn and effectively seals it. The dressing acts as a skin substitute and allows the underlying skin to heal and reepithelialize more comfortably. Biobrane may be left in place for 1 month.
 Dressings in general are used to absorb secretions, protect the burn from bacterial contamination, and prevent the wound from rubbing against clothing or other objects. When simple sterile dressings are used with Adaptic gauze or Mepitel, the frequency of dressing changes will vary depending on the amount of secretions. When Silvadene cream is used, washing and reapplication require that the dressing be changed once daily. The first dressing change should be done at a return visit to provide teaching instructions and additional dressing material. If available, continued burn management can be provided at a local burn clinic.
Dressings in general are used to absorb secretions, protect the burn from bacterial contamination, and prevent the wound from rubbing against clothing or other objects. When simple sterile dressings are used with Adaptic gauze or Mepitel, the frequency of dressing changes will vary depending on the amount of secretions. When Silvadene cream is used, washing and reapplication require that the dressing be changed once daily. The first dressing change should be done at a return visit to provide teaching instructions and additional dressing material. If available, continued burn management can be provided at a local burn clinic.
 Facial and neck burns cannot be easily dressed and generally require only the soothing topical application of bacitracin ointment. These burns will do well without any topical agents and require only gentle washing with a mild soap twice a day.
Facial and neck burns cannot be easily dressed and generally require only the soothing topical application of bacitracin ointment. These burns will do well without any topical agents and require only gentle washing with a mild soap twice a day.
 Tar burns do not require removal of solidified residual tar. The tar is not toxic to the skin and often forms a sterile wound dressing. By covering the burn and tar with bacitracin ointment and performing daily washing and repeated dressing changes with more ointment, the tar will gradually dissolve away. Neomycin sulfate/polymyxin cream (Neosporin) has been recommended as a preferred tar emulsifier, but it carries the potential of causing allergic contact dermatitis. When tar burns on the face are unsightly, the hardened tar can usually be mechanically débrided or cleaned off with repeated applications of creams or ointments. Petrolatum jelly (Vaseline) and mineral oil can also be used to slowly wipe away the tar. The facial burns are then treated like any other facial burn.
Tar burns do not require removal of solidified residual tar. The tar is not toxic to the skin and often forms a sterile wound dressing. By covering the burn and tar with bacitracin ointment and performing daily washing and repeated dressing changes with more ointment, the tar will gradually dissolve away. Neomycin sulfate/polymyxin cream (Neosporin) has been recommended as a preferred tar emulsifier, but it carries the potential of causing allergic contact dermatitis. When tar burns on the face are unsightly, the hardened tar can usually be mechanically débrided or cleaned off with repeated applications of creams or ointments. Petrolatum jelly (Vaseline) and mineral oil can also be used to slowly wipe away the tar. The facial burns are then treated like any other facial burn.
 Radiator and brief flash burns (when patients attempt to light a gas stove) of the face are not associated with inhalation injuries (even with singed facial hair) and are also treated in the standard manner.
Radiator and brief flash burns (when patients attempt to light a gas stove) of the face are not associated with inhalation injuries (even with singed facial hair) and are also treated in the standard manner.
 Patients should be instructed to keep extremity and facial burns elevated to reduce swelling.
Patients should be instructed to keep extremity and facial burns elevated to reduce swelling.
 Prescribe adequate narcotic analgesics to provide adequate pain relief over the next 24 hours.
Prescribe adequate narcotic analgesics to provide adequate pain relief over the next 24 hours.
 Patients can be reassured that superficial partial-thickness burns will generally heal in 7 to 21 days with full function, and, unless there are complications (such as infection), patients do not have to worry about scarring. Most superficial burns heal within 2 weeks, and long-term follow-up is unnecessary.
Patients can be reassured that superficial partial-thickness burns will generally heal in 7 to 21 days with full function, and, unless there are complications (such as infection), patients do not have to worry about scarring. Most superficial burns heal within 2 weeks, and long-term follow-up is unnecessary.
What Not To Do:
 Do not use large ice-containing packs or compresses that might increase tissue damage. Iced compresses should also be avoided on large burns (greater than 15% of total body surface), because they may lead to problems with hypothermia. When pain cannot be controlled with compresses, use strong parenteral analgesics, such as morphine sulfate.
Do not use large ice-containing packs or compresses that might increase tissue damage. Iced compresses should also be avoided on large burns (greater than 15% of total body surface), because they may lead to problems with hypothermia. When pain cannot be controlled with compresses, use strong parenteral analgesics, such as morphine sulfate.
 Do not provide prophylactic systemic antibiotics. They have not been shown to reduce the incidence of wound infection and are generally not indicated.
Do not provide prophylactic systemic antibiotics. They have not been shown to reduce the incidence of wound infection and are generally not indicated.
 Do not use neomycin-containing creams or ointments. They have the potential to cause a very unpleasant allergic contact dermatitis.
Do not use neomycin-containing creams or ointments. They have the potential to cause a very unpleasant allergic contact dermatitis.
 Do not confuse partial-thickness burns with full-thickness burns. With full-thickness burns, there is no sensory function or skin appendages, such as hair follicles, remaining. They do not form vesicles and may have evidence of thrombosed vessels. If areas of full-thickness burn are present or suspected, seek surgical consultation, because these areas will later require skin grafting.
Do not confuse partial-thickness burns with full-thickness burns. With full-thickness burns, there is no sensory function or skin appendages, such as hair follicles, remaining. They do not form vesicles and may have evidence of thrombosed vessels. If areas of full-thickness burn are present or suspected, seek surgical consultation, because these areas will later require skin grafting.
 Do not discharge patients with suspected respiratory burns or extensive burns of the hands, feet, or genitalia. These patients require special inpatient observation and management.
Do not discharge patients with suspected respiratory burns or extensive burns of the hands, feet, or genitalia. These patients require special inpatient observation and management.
 Do not use caustic solvents in an attempt to remove tar from burns. It is unnecessary and painful and will cause further tissue destruction.
Do not use caustic solvents in an attempt to remove tar from burns. It is unnecessary and painful and will cause further tissue destruction.
 Do not use synthetic dressings on old or contaminated burns, which have a high risk for infection.
Do not use synthetic dressings on old or contaminated burns, which have a high risk for infection.
Discussion
First-degree or superficial burns involve only the epidermis. These burns are usually painful and erythematous and do not blister. The pain usually resolves in 1 to 2 days and generally does not require anything more than cool compresses. These burns usually occur with brief contact with hot liquids.
Second-degree or partial-thickness burns involve the epidermis and portions of the dermis. Damaged dermal vessels leak serum into the stratum spinosum layer of the epidermis, forming the identifiable blisters or bullae. These burns are particularly painful. They heal spontaneously by reepithelization within 10 days to 2 weeks, providing that no infection occurs.
Third-degree or full-thickness burns involve all layers of the epidermis and dermis. These burns take on a “waxy white” appearance, and, with prolonged heat exposure, the skin takes on a yellow-brown “leathery” appearance. These burns are painless because of the damaged nerve endings, but the penumbra of partial-thickness burns may still cause the patient to have significant pain.
Simple partial-thickness burns will do well with nothing more than cleansing, débridement, and a sterile dressing. All other therapy, therefore, should be directed at making the patient more comfortable. Silvadene cream is not always necessary, but it is soothing and may reduce the risk for infection. Bacitracin ointment may also be used on small burns. When it is possible to leave vesicles intact, the patient will have a shorter period of disability and will require fewer dressing changes and follow-up visits. Studies suggest that leaving the burn blisters intact results in more rapid reepithelization than when the blisters are débrided. If the wound must be débrided, the closed-dressing technique may be more convenient and less of a mess than the open technique of washings and cream applications.
Some physicians believe that it is important to remove all traces of tar from a burn. Removal can be accomplished relatively easily by using a petroleum-based antibiotic ointment such as bacitracin, which will dissolve the tar. This can be mixed with an equal amount of Unibase (ingredients: water, cetyl alcohol, stearyl alcohol, white petrolatum, glycerin, sodium citrate, sodium laurel sulfate, propylparaben). Others have found the citrus-and–petroleum distillate industrial cleanser Medi-Sol (Orange-Sol, Chandler, Ariz.) effective, as well as nontoxic and nonirritating. Other effective solvents include polysorbate and Tween 80.
It is interesting to note that raw honey has been used as a successful burn dressing for centuries. One study demonstrated that honey was actually better than Silvadene for superficial burns.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


 When the pain has subsided, gently cleanse the burn, with intact vesicles, with povidone-iodine scrub and rinse this off with normal saline. If bullae or vesicles are open, gently cleanse with plain normal saline.
When the pain has subsided, gently cleanse the burn, with intact vesicles, with povidone-iodine scrub and rinse this off with normal saline. If bullae or vesicles are open, gently cleanse with plain normal saline.