CHAPTER 71
Foreign Body, Rectal
Presentation
Rectal foreign bodies may present with abdominal pain, anorectal pain, obstipation, acute urinary retention, or blood or mucus discharge from the rectum. Such foreign bodies are often difficult to diagnose, because the history may not be offered by the patient unless he or she is directly asked. Sometimes the patient will not volunteer that any object has been inserted or will give outlandish explanations, such as having sat or fallen onto the object. When interviewed privately in a non-judgmental manner, however, the patient will usually give an accurate account of the foreign body.
Rectal foreign bodies most commonly are found when an object, such as a dildo or vibrator, is inserted into the rectum by the patient or a partner for sexual stimulation; it then causes pain or bleeding or becomes irretrievable. Presentation is frequently delayed by embarrassment, or prior attempts on the part of the patient to remove the object.
Rectal foreign bodies also are found with practices such as “body packing,” wherein illicit drugs are packed in latex condoms or plastic bags for illegal transport. Rupture of these packets may lead to profound toxicity and death.
Less often, medical instruments, such as enema tips or thermometers, become lodged in the rectum.
What To Do:
 Try to determine how long the foreign body has been lodged and if any attempts at removal have been made. Ask specifically about any assault or rape and respond accordingly. Give special consideration to the psychiatric patient.
Try to determine how long the foreign body has been lodged and if any attempts at removal have been made. Ask specifically about any assault or rape and respond accordingly. Give special consideration to the psychiatric patient.
 The diagnosis of a rectal foreign body can usually be made from the history alone. Perform an abdominal and rectal examination, but defer the rectal examination if the foreign body is suspected to be dangerously sharp.
The diagnosis of a rectal foreign body can usually be made from the history alone. Perform an abdominal and rectal examination, but defer the rectal examination if the foreign body is suspected to be dangerously sharp.
 If there are signs of peritoneal inflammation (i.e., rebound tenderness or pain with movement) or blood on rectal examination, suspect a perforation of the bowel, start appropriate IV lines, draw blood for laboratory analysis, obtain flat and upright abdominal radiographs to look for free air, notify surgical consultants, and administer IV antibiotics. Surgical consultation should also be obtained in all cases of nonpalpable rectal foreign bodies.
If there are signs of peritoneal inflammation (i.e., rebound tenderness or pain with movement) or blood on rectal examination, suspect a perforation of the bowel, start appropriate IV lines, draw blood for laboratory analysis, obtain flat and upright abdominal radiographs to look for free air, notify surgical consultants, and administer IV antibiotics. Surgical consultation should also be obtained in all cases of nonpalpable rectal foreign bodies.
 If there are no signs of perforation, flat and upright abdominal films may still be obtained to help define the location nature, size, and number of foreign objects (as well as to reveal unsuspected free air).
If there are no signs of perforation, flat and upright abdominal films may still be obtained to help define the location nature, size, and number of foreign objects (as well as to reveal unsuspected free air).
 Those objects that lie in the low or midrectum, up to a level of 10 cm, most often can be removed transanally.
Those objects that lie in the low or midrectum, up to a level of 10 cm, most often can be removed transanally.
 When there is no suspicion of a bowel perforation, provide procedural sedation to help in the removal of the foreign body (see Appendix E). Perianal nerve blocks with local anesthesia may be helpful for use by those skilled in this procedure.
When there is no suspicion of a bowel perforation, provide procedural sedation to help in the removal of the foreign body (see Appendix E). Perianal nerve blocks with local anesthesia may be helpful for use by those skilled in this procedure.
 Place the patient on his side in the Sims position, or he can lie prone in the knee-chest position. If anal discomfort persists, instill lidocaine jelly for mucosal anesthesia or locally infiltrate 1% lidocaine with epinephrine into the anal sphincter. In general, a perianal nerve block similar to that used for anorectal surgery works quite well. Some authors favor using lidocaine (Xylocaine) 1% with epinephrine and bupivacaine 0.5% with epinephrine in a 50:50 mix. A superficial block and then an intersphincteric block circumferentially around the anal verge can be performed. Finally, to ensure the greatest degree of anesthesia, a pudendal nerve block can be performed. The branches of the pudendal nerve that innervate the anal sphincter complex approach the sphincter complex from a posterolateral location. A pudendal nerve block is done by infiltrating the tissues deeply in a fanlike technique approximately 1 cm medial to the ischial tuberosities in the posterolateral location bilaterally. Approximately 2 to 5 mL of the local anesthetic mix is used on each side.
Place the patient on his side in the Sims position, or he can lie prone in the knee-chest position. If anal discomfort persists, instill lidocaine jelly for mucosal anesthesia or locally infiltrate 1% lidocaine with epinephrine into the anal sphincter. In general, a perianal nerve block similar to that used for anorectal surgery works quite well. Some authors favor using lidocaine (Xylocaine) 1% with epinephrine and bupivacaine 0.5% with epinephrine in a 50:50 mix. A superficial block and then an intersphincteric block circumferentially around the anal verge can be performed. Finally, to ensure the greatest degree of anesthesia, a pudendal nerve block can be performed. The branches of the pudendal nerve that innervate the anal sphincter complex approach the sphincter complex from a posterolateral location. A pudendal nerve block is done by infiltrating the tissues deeply in a fanlike technique approximately 1 cm medial to the ischial tuberosities in the posterolateral location bilaterally. Approximately 2 to 5 mL of the local anesthetic mix is used on each side.
 The method of removal must be individualized, depending on the size, shape, consistency, and fragility of the object. Individual situations demand creative use of standard medical instruments and supplies. Set a time limit for yourself, and let the patient know that if the foreign body cannot be removed within a reasonable length of time (usually 10 to 20 minutes), it will have to be removed in a setting that allows for more potent anesthetics.
The method of removal must be individualized, depending on the size, shape, consistency, and fragility of the object. Individual situations demand creative use of standard medical instruments and supplies. Set a time limit for yourself, and let the patient know that if the foreign body cannot be removed within a reasonable length of time (usually 10 to 20 minutes), it will have to be removed in a setting that allows for more potent anesthetics.
 When the object can be reached by the examining finger and is of a nature that will allow it to be grasped, a lax anal sphincter may allow slow insertion of as much of a gloved hand as possible to grab the object and gradually extricate it. For instance, perforate fruit with the fingertips to obtain a more effective grasp. Having the patient bear down while performing a Valsalva maneuver may help to “deliver” the object. You can also apply suprapubic pressure from above with your free hand.
When the object can be reached by the examining finger and is of a nature that will allow it to be grasped, a lax anal sphincter may allow slow insertion of as much of a gloved hand as possible to grab the object and gradually extricate it. For instance, perforate fruit with the fingertips to obtain a more effective grasp. Having the patient bear down while performing a Valsalva maneuver may help to “deliver” the object. You can also apply suprapubic pressure from above with your free hand.
 If you are unable to pull out the foreign body by hand, the following are techniques that can be used to get a purchase on the object and break the vacuum behind it:
If you are unable to pull out the foreign body by hand, the following are techniques that can be used to get a purchase on the object and break the vacuum behind it:
 Slide a large Foley catheter with a 30-mL balloon past the object, inflate the balloon, and apply traction to the catheter. (This can be used in conjunction with any of the other techniques.) Two catheters may occasionally be needed, and air should be instilled through the lumen of the catheter to break the vacuum (Figure 71-1). Alternatively, an endotracheal tube can be passed beyond the foreign body, the cuff inflated, and air gently insufflated down the tube.
Slide a large Foley catheter with a 30-mL balloon past the object, inflate the balloon, and apply traction to the catheter. (This can be used in conjunction with any of the other techniques.) Two catheters may occasionally be needed, and air should be instilled through the lumen of the catheter to break the vacuum (Figure 71-1). Alternatively, an endotracheal tube can be passed beyond the foreign body, the cuff inflated, and air gently insufflated down the tube.
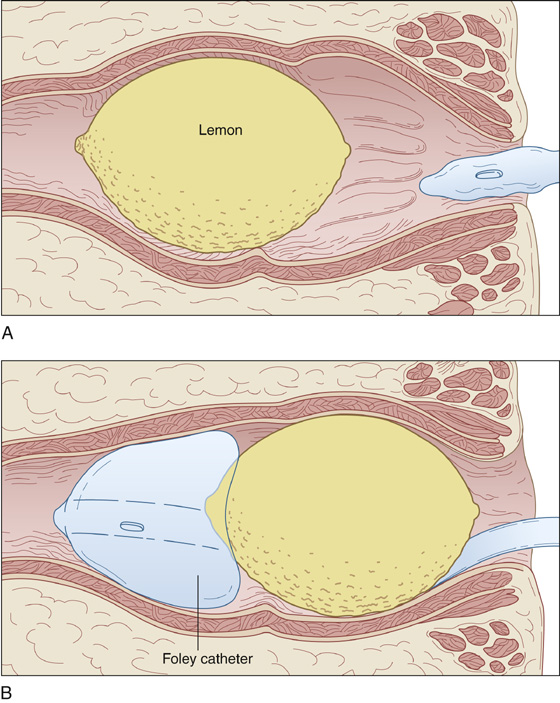
Figure 71-1 The Foley catheter technique is used to break a vacuum behind an object.
 Under direct visualization with an anoscope or a vaginal speculum, attempt to grasp the object with a tenaculum, sponge forceps, Kelly clamp, or tonsil snare (Figure 71-2). Brittle objects, especially glass, should be grasped gently, with rubber tubing or gauze covering the metal surfaces of any clamp or forceps.
Under direct visualization with an anoscope or a vaginal speculum, attempt to grasp the object with a tenaculum, sponge forceps, Kelly clamp, or tonsil snare (Figure 71-2). Brittle objects, especially glass, should be grasped gently, with rubber tubing or gauze covering the metal surfaces of any clamp or forceps.
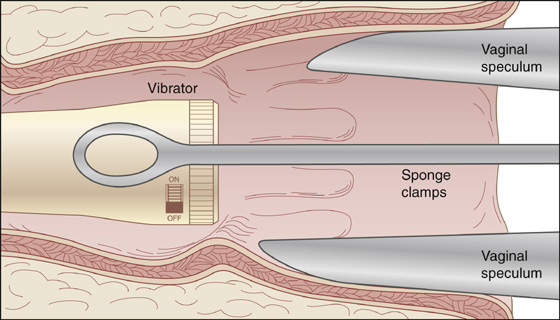
Figure 71-2 Grasp the object with a tenaculum, sponge forceps, Kelly clamp, or tonsil snare.
 An open object, like a jar or a bottle, can be filled with wet plaster, into which a tongue blade can be inserted like a Popsicle stick. When the plaster hardens, traction can be applied to the tongue blade (Figure 71-3). Alternatively, inflation of a Sengstaken-Blakemore tube balloon inside a jar may provide the traction needed to extract the object.
An open object, like a jar or a bottle, can be filled with wet plaster, into which a tongue blade can be inserted like a Popsicle stick. When the plaster hardens, traction can be applied to the tongue blade (Figure 71-3). Alternatively, inflation of a Sengstaken-Blakemore tube balloon inside a jar may provide the traction needed to extract the object.
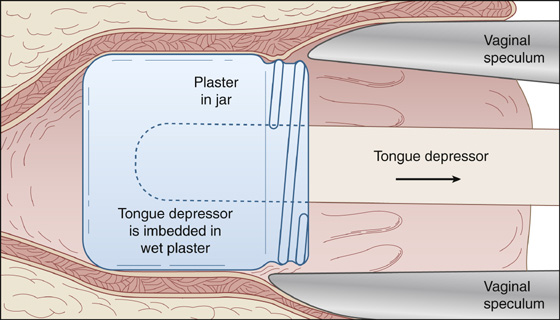
Figure 71-3 Fill jars or bottles with plaster, and insert tongue blade like a Popsicle stick. When plaster hardens, traction can be applied.
 You may be able to place a screw in some objects, which may allow you to grab them and apply traction. Other objects may have to be cut in sections to be removed.
You may be able to place a screw in some objects, which may allow you to grab them and apply traction. Other objects may have to be cut in sections to be removed.
 Forceps or soup spoons can be used to deliver a round object (Figure 71-4). When available, an obstetric vacuum extractor may be even more effective for removing round foreign bodies of compatible size and texture (Figure 71-5). Magnets are sometimes useful to help extract metal objects.
Forceps or soup spoons can be used to deliver a round object (Figure 71-4). When available, an obstetric vacuum extractor may be even more effective for removing round foreign bodies of compatible size and texture (Figure 71-5). Magnets are sometimes useful to help extract metal objects.
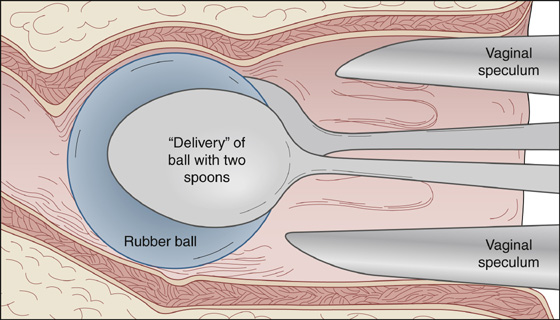
Figure 71-4 Round objects can be removed with forceps or soup spoons.
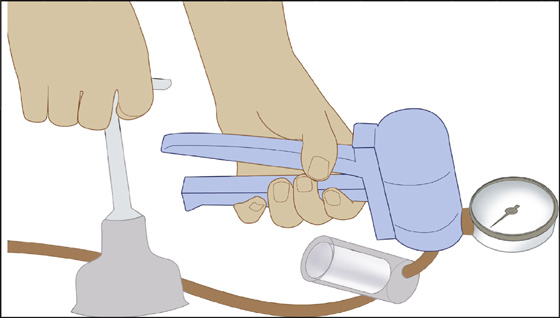
Figure 71-5 Equipment for soft-cup vacuum extraction: cup with traction handle, fluid trap, vacuum gauge, and manual vacuum pump. (Adapted from Putta LV, Spencer JP: Assisted vaginal delivery using the vacuum extractor. Am Fam Physician 62:1316-1320, 2000.)
 As the object is being removed, the speculum or anoscope should be removed along with it so that the foreign body does not have to fit through these instruments.
As the object is being removed, the speculum or anoscope should be removed along with it so that the foreign body does not have to fit through these instruments.
 With an object that is too high to reach, the patient can be admitted and sedated for removal over the next 6 to 12 hours.
With an object that is too high to reach, the patient can be admitted and sedated for removal over the next 6 to 12 hours.
 When the object cannot be removed because of patient discomfort or sphincter tightness, removal must be accomplished in the operating room under spinal or general anesthesia.
When the object cannot be removed because of patient discomfort or sphincter tightness, removal must be accomplished in the operating room under spinal or general anesthesia.
 When blood is present in the rectum, when pain is severe or persistent, when there is fever or rectal discharge, or when the object is capable of doing harm to the bowel, proctoscopic evaluation should be performed after removal of the foreign body to rule out rectal injury. Superficial nonbleeding rectal injuries may be left alone. Those that are bleeding or that involve the muscular wall require repair.
When blood is present in the rectum, when pain is severe or persistent, when there is fever or rectal discharge, or when the object is capable of doing harm to the bowel, proctoscopic evaluation should be performed after removal of the foreign body to rule out rectal injury. Superficial nonbleeding rectal injuries may be left alone. Those that are bleeding or that involve the muscular wall require repair.
 When pain persists or there is any lingering suspicion of a bowel perforation, keep the patient for 24 hours of observation and consider performing a water-soluble contrast enema study. If there are any postprocedural problems, surgical consultation is recommended.
When pain persists or there is any lingering suspicion of a bowel perforation, keep the patient for 24 hours of observation and consider performing a water-soluble contrast enema study. If there are any postprocedural problems, surgical consultation is recommended.
 When the foreign body is extracted without difficulty and the potential for bowel injury is minimal, proctoscopic evaluation is probably unnecessary, and the patient can be discharged after a reasonable period of observation.
When the foreign body is extracted without difficulty and the potential for bowel injury is minimal, proctoscopic evaluation is probably unnecessary, and the patient can be discharged after a reasonable period of observation.
 Consider recommending sexual or psychological counseling.
Consider recommending sexual or psychological counseling.
What Not To Do:
 Do not pressure the patient into giving you an accurate story. He may be embarrassed, and intimidation will not help. Do not use enemas or cathartics to help speed the removal of these objects. These treatments are not likely to be effective and may actually cause harm.
Do not pressure the patient into giving you an accurate story. He may be embarrassed, and intimidation will not help. Do not use enemas or cathartics to help speed the removal of these objects. These treatments are not likely to be effective and may actually cause harm.
 Do not attempt to remove a rectal foreign body in a patient who is having severe abdominal pain or who has signs of a bowel perforation.
Do not attempt to remove a rectal foreign body in a patient who is having severe abdominal pain or who has signs of a bowel perforation.
 Do not attempt to remove a rectal foreign body from a patient whose rectal pain and spasm are severe and cannot be overcome with the infiltration of local anesthetic. These patients will require regional or general anesthesia.
Do not attempt to remove a rectal foreign body from a patient whose rectal pain and spasm are severe and cannot be overcome with the infiltration of local anesthetic. These patients will require regional or general anesthesia.
 Do not push the object higher into the colon while attempting to remove it.
Do not push the object higher into the colon while attempting to remove it.
 Do not blindly grab for an object with a tenaculum or other such device. This can itself lead to a perforation.
Do not blindly grab for an object with a tenaculum or other such device. This can itself lead to a perforation.
 Do not attempt to remove fragile or sharp, jagged objects, such as broken glass, through the rectum. These should only be removed under anesthesia in surgery.
Do not attempt to remove fragile or sharp, jagged objects, such as broken glass, through the rectum. These should only be removed under anesthesia in surgery.
 Do not attempt to remove packets of illicit drugs with clamps or sharp medical instruments, because spillage can lead to toxicity and death.
Do not attempt to remove packets of illicit drugs with clamps or sharp medical instruments, because spillage can lead to toxicity and death.
 Do not send home a patient who is having continued pain. Admit him and observe for peritoneal signs, increased pain, fever, and a rising white blood cell count.
Do not send home a patient who is having continued pain. Admit him and observe for peritoneal signs, increased pain, fever, and a rising white blood cell count.
Discussion
Anorectal foreign bodies can be either ingested orally or inserted anally. Although the vast majority are inserted for autoerotic purposes, they may have been placed iatrogenically or as a result of assault or trauma. Ingested objects are rarely a cause of entrapped rectal foreign bodies. Most often, these are bones that become impaled in the anal canal. Iatrogenic foreign bodies include thermometers, enema tips, and catheters. Objects placed as a result of assault, trauma, or eroticism represent a diverse collection, including sex toys; tools; wire hangers and instruments; bottles, cans, and jars; poles, pipes, and tubing; fruits and vegetables; stones; balls; balloons; light bulbs; and flashlights.
Most of these rectal foreign bodies can be removed safely in the emergency department or acute care clinic. Relaxation is essential, and sedation is usually necessary if retrieval is to be successful. Some practitioners quite reasonably forgo radiographs before manipulation if the patient is free of pain and fever and if the object is benign.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


