, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
CellulitisBacteriaErysipelasInfectionSoft tissueMRSAWoundUlcerStaphStrep Staphylococcus Streptococcus ExudateAntibioticCompression socks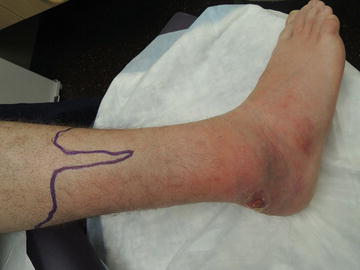
Fig. 17.1
Edges marked to gauge tracking of erythema and edema
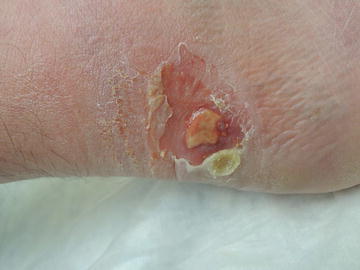
Fig. 17.2
Ulceration secondary to heavy third-spacing of fluid in tissue
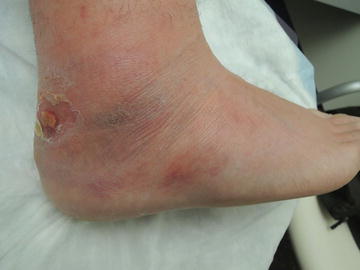
Fig. 17.3
Significant edema accompanies the erythematous rash
Primary Care Visit Report
A 24-year-old male with past medical history of staphylococcal and streptococcal skin infections and abscesses presented with an open lesion on his right posterior ankle accompanied by right leg erythema and edema. The patient reported that he had formed a blister in this same right heel 7 months prior. That blister healed, however the overlying skin did not fully return to normal. The patient said, “there was always a dark spot there after that.”
Five days prior to this visit, his right foot and leg started swelling and becoming red, and the site of the prior blister opened up. The day prior to this visit, a “black spot” appeared adjacent to the open lesion, which then also “broke open,” forming a large wound. He denied fever or chills, and felt otherwise well. The patient reported that the area had been much more painful 2–3 days prior to this visit, at which time he could not put on a shoe due to the pain and swelling. The pain had improved by the time of visit.
Vitals were normal. On exam, there was a 3.5 cm × 2 cm weeping ulcer on the lateral Achilles area of his right heel, with surrounding blanchable erythema on his foot and ankle that extended to the mid lower leg. There was 1+ edema on the right lower leg.
This was treated as cellulitis progressing from an open abscess on the patient’s posterior ankle. Since the patient had a history of staph and skin infections, he was treated for possible MRSA . The patient was prescribed oral sulfamethoxazole/trimethoprim 800–160 mg twice daily for 10 days, and topical bactroban 2 % three times daily to the open wound. The proximal border of the erythema was outlined with a permanent marker. The patient was advised to go to the Emergency Department if the erythema extended beyond the marked line or if any systemic symptoms developed as that could be an indication for intravenous antibiotic treatment.
Discussion from Dermatology Clinic
Differential Dx
Cellulitis
Abscess
Erysipelas
Impetigo
Necrotizing fasciitis
Stasis dermatitis
Favored Dx
Physical examination indicates cellulitis.
Overview
Cellulitis is a soft tissue bacterial infection caused mainly by gram-positive pathogens such as Staphylococcus aureus , MRSA , and β-hemolytic Streptococci . The infection occurs following breaks in the skin, commonly from surgical wounds, ulcers, or eczematous conditions.
Cellulitis is a common infection that complicates wounds, ulcers , and skin abrasions. It affects the dermis and subcutaneous tissue. The depth of involvement can be used to differentiate cellulitis from erysipelas , which is clinically very similar but affects superficial layers of the skin, and has well defined margins. The incidence of soft-tissue infections is high, accounting for as many as 10 % of hospital admissions, and cellulitis is estimated to occur in 200 per 100,000 people but is variable depending on populations [1, 2]. Incidence of cellulitis is on the rise, mirroring the increase of MRSA infections.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








