Fig. 37.1
Simulation course timeline . Timeline showing simulation course components. Physical resources are color-coded. Pre-class material is viewed on the website which occurs before the day that the simulation takes place, as indicated by the interrupted timeline. The simulator course requires the use of a conference room and a simulated operating room
Interviewing End-Stage Liver Disease Patient
It is important for the anesthesiologist to be a part of the team assessing ESLD patients for liver transplantation. Therefore, a mock preoperative interview of a potential candidate for liver transplantation, impersonated by one of the instructors gives the opportunity to focus on the history and physical condition of the patient and how to optimize the condition of the patient prior to surgery [7]. In addition it also permits the learners to deal with delicate social issues such as Hepatitis C, HIV, and the special requirements of Jehovah’s Witness patients. This session takes about 20–45 min. The learner is given the stem patient, for example: 52 year old male with ESLD due to Alcoholism for OLTX. Debriefing after the preoperative interview is helpful in emphasizing unique points pertinent to this patient population [5, 8].
Setting Up the Environment of the Operating Room
At this point the participants should be able to test their abilities with the high-fidelity simulated clinical scenarios [9]. It is very important to create an environment that is as close as possible to the operating room (Fig. 37.2, Table 37.1.) Props provide a sense of place and tools to perform the expected action. The goal is to provide enough stimuli and generate enough data to engage the learner and thus promote the interactions needed to achieve the learning objectives. The checklist for the room set-up should be provided in the pre-course material, this way the participant can anticipate how the simulated operating room will look. Creating a sense of familiarity decreases the level of anxiety during the clinical scenarios while encouraging engagement. It might not be feasible to provide a working trans-esophageal echocardiography machine (TEE), thromboelastography (TEG), or rapid infusion system due to cost, but having similar looking equipment and projecting the virtual data on a screen is cost effective and a reasonable facsimile to the OR experience of LTx (Fig. 37.3). Blood products can be made available in the form of bags filled with red colored liquid for packed red cells and yellow colored liquid for fresh frozen plasma. The bags should be labeled with identification numbers and blood group, placed in a cooler and made available upon request. Details, such as presence of a phone to make simulated phone calls to the blood bank, laboratory and attending for advice should not be overlooked. One of the instructors plays the role of the surgeon and use this opportunity to interact with the participants during the clinical scenario, helping to provide clues to the differential diagnosis: “I have drained six liter of ascites” or “this liver is old, long cold ischemia time” or creating some tension: “liver is congested I cannot manipulate it, do something about it.” All these statements are meant to help participants integrate the input from the surgical team and assess how well they can communicate. The presence of an anesthesia technician will help to assess how well the participants can use the resources at hand.
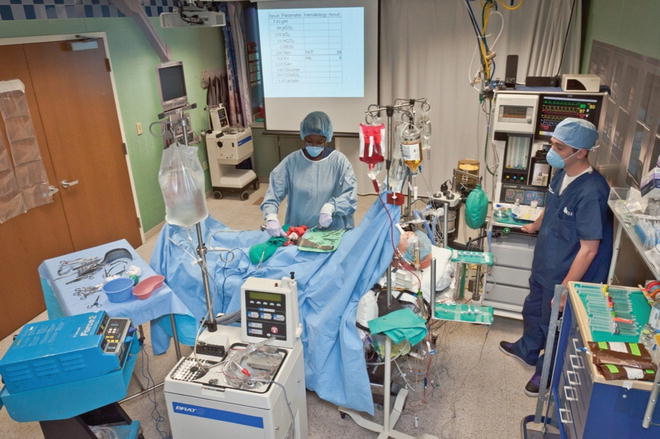
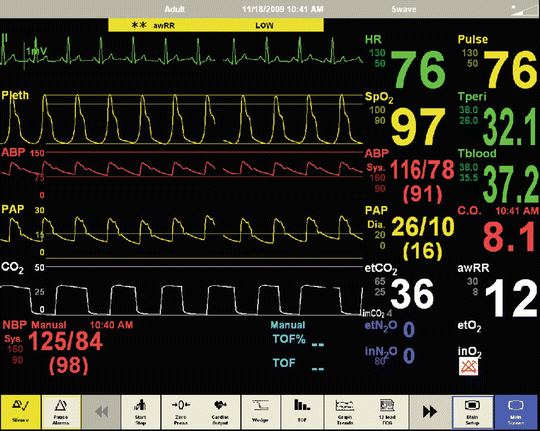

Fig. 37.2
Simulated operating room for liver transplantation
Table 37.1
Props present in the simulated operating room
Simulated environment | |
|---|---|
Equipment | High-fidelity simulation mannequin |
Anesthesia cart with common OR set-up and medication | |
Anesthesia machine | |
High-fidelity monitor (EKG, blood pressure, CVP, pulmonary pressure, SpO2, ETCO2, temperature) Fig. 37.2 | |
Rapid Infusion System | |
Transesophageal echocardiography probe/machine | |
Projector screen for additional data | SvO2 and cardiac output |
Arterial blood gas results | |
TEE video-loops | |
TEG images | |
Additional material | Telephone |
Blood products | |
Personnel | Surgeon |
Anesthesia technician | |

Fig. 37.3
Anesthesia machine monitor display for the high-fidelity simulation of a liver transplant patient
The environment created should be such that learners are challenged in their thinking and action but never intimidated. The teacher should raise relevant topics and the learners should reflect on those topics. In the beginning of the course the learners can be reassured that perfection is not the expectation of this course but that this is an environment for learning by interaction.
Central Venous Line Placement
By the time most participants are assigned for a liver transplant anesthesia rotation they are in the 3rd or 4th year of anesthesia residency and should be experienced in placing central venous lines. The goal of central venous line placement simulation is to understand the necessary vascular access, the options and risks associated with each line and special risks in ESLD patients who are often coagulopathic. The placement of a veno-venous bypass cannula (# 18 Fr) is unique to liver transplant anesthesia and malposition is disastrous [10, 11]. Emphasis is placed on how to set up the procedure tray, patient preparation, identification of landmarks, insertion and confirmation of the guide wire location, dilation of the tissue path and finally confirmation of placement. Other topics include: how to avoid air embolism, detection of inadvertent malplacement, and the procedures to initiate and terminate veno-venous bypass.
Simulation Session
The clinical scenarios are held with high-fidelity mannequin-based simulation. The goal of the clinical scenario is to engage the learner in the scenario so that they will have the experience of recognizing problems, identifying available resources, and making decisions. Advanced learners become bored if presented with overly simple problems that fail to challenge their skill sets. The scenario must reflect clinical events that would move the learner toward the final goals of understanding the events of liver transplantation and being able to anticipate responses to their actions. For example, during the pre-anhepatic stage of liver transplantation hypotension is common and the etiology invariably is hypovolemia or hypocalcemia. Creating a scenario of simple hypovolemia will be easily recognized and corrected, however it may lead to a discussion of atypical causes of hypotension. Ultimately, through the simulated clinical scenarios the participants should have the opportunity to make a differential diagnosis and take action based on data presented or that they should have known to request. They should also be able to judge the effectiveness of their intervention and change the intervention accordingly. If the initial problem is properly managed, the scenario moves to a second problem; however, if the participant fails to identify and address the initial problem the patient will spiral down and not survive. Thus the scenario could be terminated after covering one or two challenging medical issues, depending on the participants’ performance. Either way, the learning objective would be accomplished and reinforced during the debriefing session following the scenario.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






