Healing by secondary intention
Primary closure
Skin grafting
Local flaps
Distant pedicled flaps
Tissue expansion
Free tissue transfer
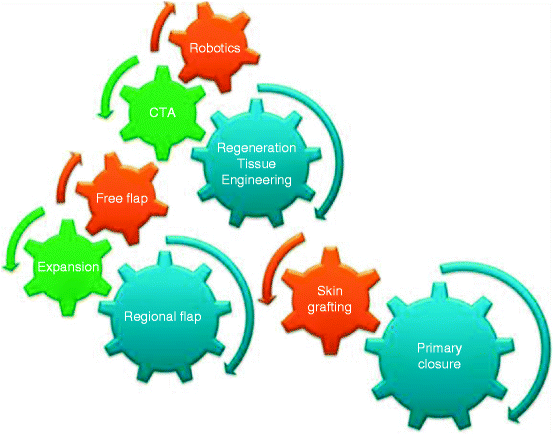
Fig. 12.1
Reconstructive clockwork as a refinement of the reconstructive ladder. CTA composite tissue allotransplantation (From Knobloch and Vogt [3])
12.3 Zone of Injury and Reconstructive Units
Mangled limbs resulting from high-velocity injuries develop a zone of soft-tissue injury that is greater than the visible wound or might increase dramatically within the first hours after trauma [4, 5]. The direct trauma contact area is characterized by a zone of necrosis with an adjacent zone of stasis surrounded by a hyperemic region. Marginally viable soft tissue during the initial trauma might die or will be replaced by fibrous scar tissue, particularly within large soft-tissue defects. The initial management, therefore, requires a fast and effective examination of the patient and should be supported by imaging techniques such as ultrasound, radiography, angiography, magnetic resonance imaging, or other specific imaging procedures. In addition, the early treatment of soft-tissue and osseous defects should prevent an increase of the soft-tissue damage, dead space, infection, nonunion, osteomyelitis, pain, malfunction, or complete tissue or limb loss.
To apply the best treatment method for the patient, the reconstructive surgeon should be familiar with the regional specific physiological vascularization. Furthermore, the type of skin incision that should be parallel to the Langer or resting tension lines, should be considered. Transverse running scars might functionally and aesthetically bother the patient. For reconstruction of soft-tissue defects it has been established that there is a difference between reconstructive and functional (skin) units with respect to local factors such as function, mechanical demands and aesthetics as well as the different possibilities of defect coverage. Additionally, the localization of the defect must be considered with regard to the loco-regional demands as well as the respective treatment options. Palmar skin, for example, differs greatly in its mechanical capacity and sensibility from that of the back of the hand. Attention should also be paid to zones of low resistance where the bone is better located directly beneath the skin without any muscle padding.
12.3.1 Defect Description
Determining the severity of injury to the soft tissues is a central component of patient assessment and affects the management of surgical intervention. The reconstructive surgeon can choose from among a variety of techniques for optimal treatment; however, the surgeon needs to know the exact description of the defect as well as distinct patient- and therapy-imminent criteria (Table 12.2). The defect can be differentiated as acute and chronic soft-tissue defects according to its etiology. Special forms are the combined soft and osseous tissue defect and the soft-tissue defect resulting from a multiple trauma injury. Furthermore, the surgeon must verify whether a tissue dehiscence is the result of tissue elasticity or edema, or whether it is true soft-tissue loss. To rapidly define the extent of the tissue damage, the defect can be classified as type a (defect reaching the fascia), type b (mixed skin-muscle and other soft tissue defects), and type c (combination of soft-tissue and bony defect). A more detailed determination of the soft-tissue injury in combination with closed or open fractures can be obtained using the classification of Tscherne and Oestern, grouped into four categories according to severity (Table 12.3; [6]).
Table 12.2
Decision criteria for the coverage of tissue defects using plastic reconstructive techniques
Defect-associated factors | Patient-associated factors | Therapy-associated factors |
|---|---|---|
Etiology | Acute patient condition | Goal of reconstruction |
Localization | Age | Timing |
Skin defect | Sex | Reconstruction method (Table 12.1) |
Soft-tissue defect | Intelligence/compliance | Sequence of reconstruction |
Soft-tissue and osseous defect | Job | |
Character of the wound | Social background | |
Other diseases | ||
Patient wishes |
Table 12.3
The Oestern and Tscherne classification for soft tissue in closed and open fractures
Grade | Closed fractures | Open fractures |
|---|---|---|
0 | Minimal soft-tissue damage | |
Indirect injury to limb (torsion) | ||
Simple fracture pattern | ||
I | Superficial abrasion or contusion | Small puncture wound without skin contusion |
Mild fracture pattern | Negligible bacterial contamination | |
Low-energy fracture pattern | ||
II | Deep abrasion | Minor skin and soft-tissue contusions |
Skin or muscle contusion | Moderate contamination | |
Severe fracture pattern | Variable fracture patterns | |
Direct trauma to limb | ||
III | Extensive skin contusion or crush injury | Heavy contamination |
Severe damage to underlying muscle | Extensive soft-tissue damage | |
Compartment syndrome | Associated arterial or neural injuries | |
Subcutaneous avulsion | ||
IV | Incomplete or complete amputations |
12.3.2 Timing
The proper timing and adequate planning of wound closure in soft-tissue traumas helps to limit further soft-tissue injury and facilitates its rapid recovery. Therefore, the surgeon should also have clear-sighted vision and not pass up a chance for other treatment possibilities if complications arise. The response of soft tissue to injury involves microvascular and inflammatory processes that produce localized tissue hypoxia and acidosis. Incisions placed through such compromised tissue, particularly in blunt soft-tissue injuries, can lead to wound breakdown and deep infection. Therefore, recognizing the signs of soft-tissue injury is the basis for successful management [7].
In any soft-tissue injury, especially of the limbs, an initial radical débridement of damaged and necrotic tissues is necessary within the first 6 h after trauma. The débridement can also be performed in scheduled second- or third look surgeries after 48–72 h. On the one hand, surgical débridement supports the phagocytic activity of the macrophages and reduces the risk of hypoxia and infection within the inflammatory phase of wound healing [8]. On the other hand, it helps to clearly evaluate the extent of injury for the subsequent treatment regimen. The width of the débridement might sometimes be hard to accept by the operating surgeon because of additional tissue loss, but it is necessary to prevent the above-mentioned complications (i.e., zone of injury).
Appropriate timing for soft-tissue reconstruction and wound closure is a matter of controversy. The recommendation of Godina clearly reveals the advantage of aggressive débridement and closure of the wound with vascularized tissue within 72 h. Through adherence to this timeframe, severe complications can be decreased significantly [9]. A special form of a conservative treatment regimen in local wound support can also be obtained from vacuum assisted closure. Because of the optimization of the wound milieu via continuous wound cleaning, spontaneous regeneration processes will be accelerated and definitive wound closure can be reached significantly faster. Furthermore, the flap reconstruction can also be performed beyond the quoted critical time interval of 72 h with results similar to those of immediate reconstruction [10].
12.3.3 Special Co-injuries
12.3.3.1 Bone Injury
A stable osseous condition is an indispensable prerequisite for successful soft-tissue coverage [11]. For that reason, fractures and bone dislocations must be stabilized, even if only provisionally to restore the essential mechanical stability, to prevent further soft-tissue injury and to limit perfusion problems (Figs. 12.2, 12.3, 12.4, and 12.10). In unclear or severe cases of soft-tissue injury combined with fractures, it has proved valuable to proceed stepwise for definite osteosynthesis. First, on the day of injury, the fracture is adjusted by external fixation with regard to the applied reconstruction techniques, which may cover the defect. Internal fixation should be avoided; however, when there is need for large soft-tissue reconstruction, recent studies have not shown differences in internal versus external fixation [12]. Time and technique of the definite fracture treatment depend on the extent of the soft-tissue injury after demarcation, the extent of the bone defect, the infection, and the defect localization.
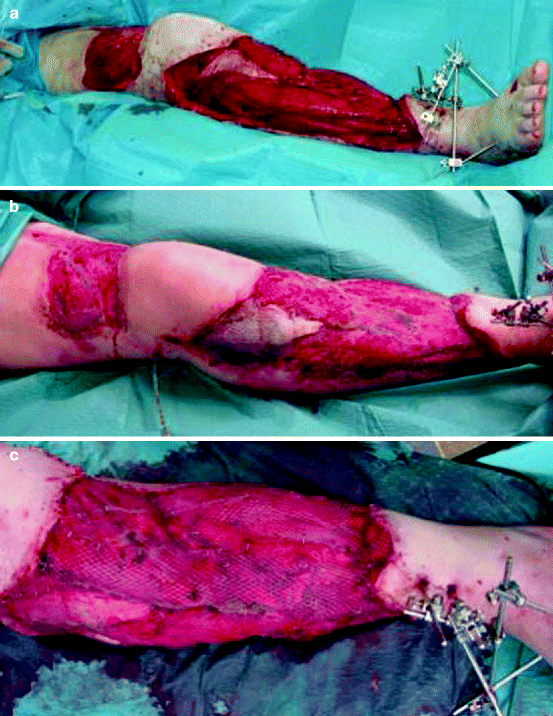
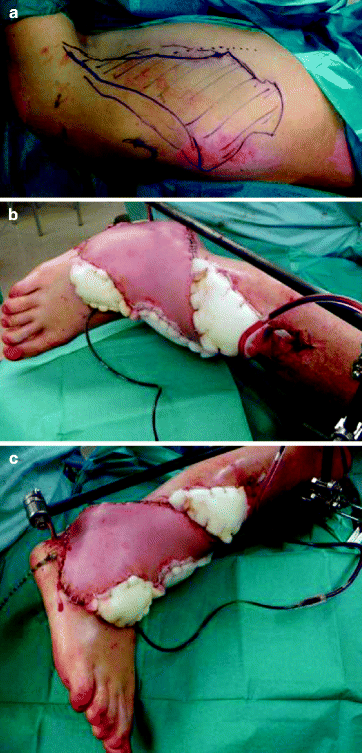

Fig. 12.2
Ankle tibial fracture with a combined severe soft-tissue trauma with a complete loss of skin in the ventral lower leg and proximal knee region (a). The entire defect can be covered by meshed split thickness skin grafts because of the vital muscular wound bed (b, c)

Fig. 12.3




A 35-year-old man suffered from a pilon tibiale and ankle fracture with a severe soft-tissue defect after a motorbike accident. The defect could only be covered with a free microvascular latissimus dorsi flap. (a) The flap design on the back is marked. (b, c) The postoperative result is demonstrated
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








