Fig. 18.1
Electromicroscopic slide of Staphylococcus epidermidis: Biofilm. Upper figure: Staphylococcus aureus from fluid culture; lower figure: Staphylococcus aureus in Biofilm (REM-slide from S. Sailer and I. Chatterjee, Homburg/Saar)
18.1.4 Prevention of Infections in Trauma and Orthopaedic Surgery
The treatment and healing process can be divided into three phases: preoperative, intraoperative, and postoperative.
In all three phases, the reduction of soft-tissue damage, the prevention of contamination, and the improvement of blood perfusion are necessary [6–8]. Therefore, the fracture should be reduced as early as possible, sufficient blood pressure should be reached, a examination of open fractures should be performed under sterile conditions in the operating room, and antibiotic drugs must be administered in the emergency room. The radical removal of dead tissue is required on open fractures. Additionally, the type of osteosynthesis and operative procedure chosen should prevent a decrease of local and systemic conditions for wound healing. In critical soft-tissue conditions, the method of choice is a temporary covering of the wound with a vacuum closure. Time plays a vital role in the third phase. By the time the surgeon reflects whether a revision procedure is necessary, the revision should be done.
The majority of severe infections and development of osteitis can be prevented with early and consequent management of complications in the third postoperative phase.
18.1.5 Principles of Clinical Examination
The usual principles for diagnosis of osteitis are valid.
In the clinical presentation of open fractures, operative fracture treatment, complications during wound healing, diabetes mellitus, and signs of general inflammation-like fever, swelling, and redness are indicative of osteitis.
Local signs of infection on clinical examination depend on the level of infection. The spectrum of local symptoms ranges from pain under stress to redness and swelling, up through the existence of fistula with purulent secretion, and in severe cases, systemic sepsis.
18.1.6 Laboratory Diagnostics
A specific laboratory parameter for detecting osteitis does still not exist.
18.1.7 Imaging Methods
There are different imaging methods for diagnosing acute postoperative and the chronic osteitis. For the diagnosis of acute osteitis, the imaging methods are less helpful [9, 11].
For chronic osteitis, plain radiographs, computed tomography (CT), and magnetic resonance imaging (MRI) are methods of diagnosis. Thus, enclosed gas in a bone formation seen on CT scans is a strong argument for chronic osteitis. The uptake of contrast medium in the adjacency of a bone sequester is deemed to be strong evidence of chronic osteitis.
Ultrasound imaging is not appropriate for the diagnosis of osteitis because it is not highly specific. In recent years, results using fluorodeoxyglucose positron emission tomography (FDG-PET) have shown to be a valid method for the diagnosis of osteitis. Available studies report sensitivity with an of average 96 % and specificity of 91 % compared with bone scintigraphy (82 %/25 %), leukocyte scintigraphy (61 %/77 %), and MRI (84 %/60 %) [12]. Using FDG-PET CT should show an improvement of expressiveness (Fig. 18.2).
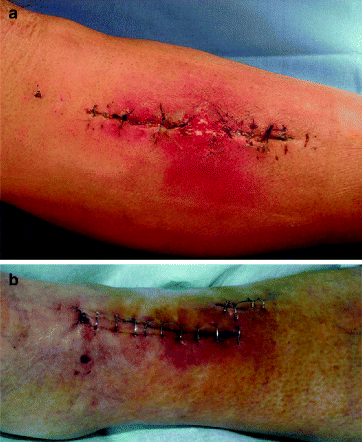

Fig. 18.2
(a, b) Acute osteitis: clinical aspect
18.1.8 Bacteriology
A positive microbiological culture shows the highest evidence for the diagnosis of osteitis. The bacterial probes must be taken from the intraoperative situs. The tests must be representative for aerobe and anaerobe bacteria. The time between extraction of the material and the beginning of processing the microbiological investigation is important for the significance of the probes. If incubation of the probes begins too late, a false negative result can present for noninfected tissue. The same is essential for the extraction of the probes from the wound. Using gloves and instruments for avoiding contamination from the skin and other tissue areas is indispensable. In clinical cases with a high suspicion of infection without a positive microbiological result, specific infections must be excluded (e.g., tuberculosis, Lues).
18.2 Acute Osteitis
18.2.1 Synonyms
Acute posttraumatic osteitis
18.2.2 Definition
The definition of acute posttraumatic osteitis (APO) is the bacterial infection of bone and soft tissue adjacent to a fracture, and implants within 6 weeks after fracture treatment or joint replacement.
18.2.3 Epidemiology/Etiology
Depending on the type of fracture and the operative procedure the incidence of APO ranges between 0.5 % in elective orthopaedic surgery up to 40 % in acute trauma surgery of open factures [13, 14].
The level of soft-tissue damage, type and amount of bacterial contamination, presence of implants, and the general conditions of the patient are the most important parameters.
In addition to these factors, postoperative wound management plays an important role. The wound hematoma presents the bacteria with ideal conditions for growth. With the early removal of postoperative hematoma, effective prevention of the development of APO is possible.
The occurrence of APO is connected to an increase of number of days in hospital to an average of 13–24. As a result, additional costs for one case of APO are estimated to rise up to 14,000 € [6].
18.2.4 Symptoms
Clinical symptoms of APO are redness, swelling, fever, increasing CRP level, pain, and treatment of fracture within the previous 6 weeks (Fig. 18.2a, b).
18.2.5 Complications
The most important complication is absent and failed treatment of APO and has the potential consequence of turning into chronic osteitis. During the treatment of APO, dependant on localization, general conditions, type of bacteria, and type of previous treatment, surgical complications may occur. Because treatment of APO immobilization of the affected region requires, the risk of thromboembolism is high. The use of a cast imcontains the risk of pressure ulcer to prevent pes equinus. The risk for thromboembilism and pressure ulcer rise in the presence of bad general conditions and other factors (e.g., diabetes mellitus, arteriosclerosis).
18.2.6 Diagnostics
18.2.6.1 Recommended European Standard for Diagnostic Investigation
The diagnostic of APO is based on:
Medical history
Operative treatment, open fracture, complications after primary surgery,
Bad general conditions
Clinical investigation
Pain, redness, swelling, fever, decreased function
Laboratory findings
Increasing CRP, positive microbiological blood culture
Imaging
Radiographs for detecting loosening of the implant, CT for detecting gas in necrotic bone
Microbiological culture
Positive microbiological culture from the affected tissue (aerobe and anaerobe testing).
18.2.6.2 Useful Additional Examinations
In preparation for surgical revision of a joint replacement, the puncture is helpful in detecting bacteria. The indication for the puncture must be handled carefully because contamination of the joint by the puncture is also possible.
18.2.7 Conservative Treatment
18.2.7.1 Recommended European Treatment Procedures
In consideration of the pathophysiological features a conservative treatment of APO is not reasonable.
18.2.7.2 Useful Additional Therapeutic Strategies
Additional systemic administration of antibiotics
18.2.8 Surgical Treatment
18.2.8.1 Recommended Surgical European Standard
Early revision of the affected wound, if necessary under emergency conditions
Revision of all parts of the wound
Removal of tissue probes for urgent bacteriological investigation
Change of the sterile covering, gloves and instruments after wound irrigation and before vacuum closure
Local antibiotics
Closure of the wound after revision surgery with vacuum technique
Immobilization (cast, external fixator)
Systemic antibiotic drugs (cephalosporin of the third generation or analogue)
Repetition of the revision procedure after 2–3 days
Administration of the antibiotic drugs according to the result of the first microbiological probes
Removal of the implant, if after repeated revision procedures a negative bacteriological result can not be achieved
18.2.8.2 Useful Additional Surgical Treatment
The low pressure jet lavage of long bone marrow hole is helpful, but not mandatory. For the lavage of soft tissue jet lavage is not favorable, because mechanical alteration occurs with decrease of tissue nutrition and possible impaction of residual bacteria into tissue.
18.2.9 Differential Diagnosis
The abacterial postoperative wound haematoma is the most important differential diagnosis, clarified always as the result of a surgical revision procedure.
18.2.10 Prognosis
Healing of APO is accomplished in the majority of cases if a consequent surgical revision concept is applied. In 40 % of cases, the removal of the implant cannot be avoided [15–17].
Nevertheless, therapy for APO is not successful in all cases, with 10–30 % progressing to chronic osteitis.
18.2.11 Surgical Procedure
18.2.11.1 Septic Operative Management
There is no question about the consequent realisation of the principles of aseptics and antiseptics during septic surgery in the operating room to prevent further contamination and osteitis [15, 16, 18, 19].
The goal of surgical therapy is the complete removal of necrotic tissue and therefore the decrease of the number of bacteria in the wound.
In addition to parameters such as general conditions, blood perfusion, soft-tissue covering, and antibiotic drug therapy, the amount of bacteria in the wound is a deciding factor for the emergence of osteitis (s. Sect. 18.1.3). Decreasing of quantity of bacteria in septic surgical procedures can be achieved by changing gloves, instruments, and sterile coverings after débridement of the necrotic tissue and lavage of the wound [20–22]. During the process of changing these items, an antiseptic solution can be used. The same handling is essential in cases of exchanging implants. A decrease of positive bacterial culture of 70 % was observed in laboratory investigations.
The first revision procedure is aimed at identifying the surgical problem, taking microbiological samples, and performing a sufficient vacuum closure. Whereas the first look must be done as an emergency procedure, the planned second and following procedures are elective. In preparation of revision procedures in long bones and joint replacements a major blood loss must be calculated. Usage of a cell saver or a self blood donation is not feasible.
At the beginning of revision procedure the closure of the wound must be taken into consideration because the soft-tissue covering is the basis for all further surgery. Under the revision concept, the edge of the wound has a tendency of retracting. With the vacuum closure of the wound the approximation of the edges of the wound with a continuous intracutane suture should be used (Fig. 18.3). Immobilization of the affected region is required during the revision procedure.
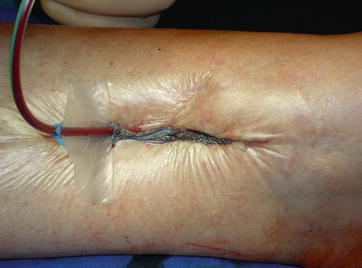

Fig. 18.3
Vacuum closure of the wound
Proceeding with additional revision procedures is determined by the results of the microbiological samples.
18.2.11.2 Wound Revision
Technique
Removal of skin sutures, revision of all parts of the wound and necrotic tissue, excision of the affected wound edge, and taking tissue samples for microbiological testing must be done under sterile conditions.
Possible Complications
Possible complications include bleeding, wound closure inability, additional damage to bone and functional structures.
18.2.11.3 Removal of Implants
Technique
Removal of implants should be approached through existing scars if possible and with positioning of the patient on the table with possibility for intraoperative imaging. Removal of all implants should be achieved without additional soft-tissue damage. Planning should be undertaken the wound closure and bone stabilization after revision procedure, as well as preparation of casts for lower leg immobilization during the salvage procedure.
Possible Complications
Possible complications during removal of implants include injury of functional structures, implant breakage, incomplete removal, or instability after removal of implant.
18.2.11.4 Nail Exchange
Technique
Planning for availability of instruments and implants.
Reaming of the medullary canal after removal of the nail.
Positioning of the patient on the table with a possibility for reosteosynthesis.
Prevention of additional bone destruction.
Possible Complications
Possible complications include loosening of the locking bolts, shortening, torsional displacement, and additional fracture of the affected bone.
18.2.11.5 External Fixator
Technique
Placement of the pins should be in the center of the cortical bone with drilling before positioning the pins. Bicortical fixation. Adequate soft-tissue incision regarding to joint movement.
Possible Complications
Displacement of the pins, injury of functional structures, soft-tissue impairment, pin track infection.
18.3 Chronic Osteitis
18.3.1 Synonyms
Osteomyelitis
18.3.2 Definition
Bacterial infection of bone and implants over a period of 6 weeks or longer after treatment of fracture or joint replacement.
18.3.3 Epidemiology/Etiology
In trauma and orthopaedic surgery, the presentation of chronic osteitis is a major complication following primary surgery [16, 23]. Chronic osteitis is characterized as bacterially infected bone after a period of longer than 6 weeks following primary surgery. Chronic osteitis is a challenge for the patient, the patient’s family, as well as the surgeon.
In Germany, a change in condition from acute osteitis to chronic osteitis is estimated to occur in 10–30 % of all cases [24–26] (s. Sect. 18.2). The change to chronic osteitis as a result of inconsequent surgical management of acute osteitis, open fractures, and extensive soft-tissue damage.
Most detected bacteria are Staphylococcus aureus, Pseudomonas, Proteus, Streptococcus, and other types that include mixed flora bacteria [1, 27]. The causes for chronic osteitis are necrotic and avital tissue parts and implants colonized by bacteria.
Depending on the virulence of the bacteria, the local soft-tissue situation, and the immunological competence of the patient, different levels of infection can evolve. The clinical appearance can change from pseudarthrosis without signs of infection, to local infection with fistula, to septic shock.
The lower limbs, particularly the shank, are most affected with chronic osteitis because the soft-tissue covering in this region is inadequate.
18.3.4 Symptoms
Local and general signs of infection differ depending on the level of infection and localization (s. Sect. 18.3.3)
In low-grade infections, symptoms present with a clinical impression of pseudarthrosis with pain, marginal swelling, and redness. Existing fistula near the fracture region will sometimes demonstrate chronic osteitis (Fig. 18.4).
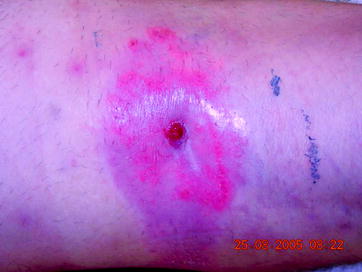

Fig. 18.4
Chronic osteitis: fistula in the hollow of the knee
Classic signs of inflammation are seen in acute recrudescing chronic osteitis and with infection of joint replacements in the aforementioned interval. In cases of unknown fever, inflammation, and a positive medical history, an infection of the bone and joint replacement must be excluded.
18.3.5 Complications
Chronic osteitis that is left untreated can lead to septic shock and additional problems. If treatment is unsuccessful, amputation or exarticulation can result. Addicted to the type of method for salvage (eradikation) the chronic osteitis deformities of affected limbs and decreased function are feasible.
18.3.6 Diagnosis
A positive medical history of open fracture, additional infection, and indices for immunodeficiency are indices for chronic osteitis. Laboratory findings are not specific, but depending on the grade of infection, the signs of inflammation are typically positive. Progression of CRP indicates chronic osteitis.
Plain radiographs are mandatory, but not argumentative. An irregular periosteum will sometimes demonstrate a chronic inflammatory reaction and in advanced cases, sequestering of bone can be found. CT is required for detecting necrotic bone (Fig. 18.5a, b). Uptake of contrast medium adjacent to sequestering as well as gas formation in the bone are deemed as evidence for chronic osteitis (s. Sect. 18.1.7)
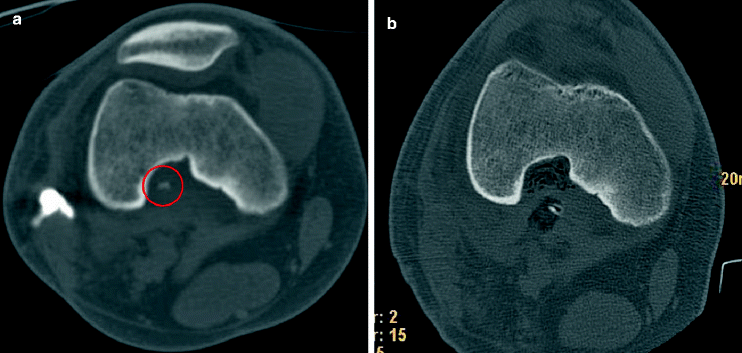

Fig. 18.5




(a, b) Chronic osteitis: bone sequester in the popliteal fossa before and after removal. In the center of the red circle a small piece of bone was detected as a sequester which was the cause for chronic infection (a). After removal of this piece of necrotic bone the infection was healed
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








