The altering of the body as a result of the ageing process also leads to unexpected observations. For instance, whereas in middle age high blood pressure is associated with an increased risk of cardiovascular disease, in a population of 85-year-olds, those with the highest blood pressure have a higher life expectancy compared to those with lower blood pressure. One explanation may be that to maintain adequate perfusion through stiffened arteries by atherosclerosis, a higher blood pressure is needed and that those older patients able to successfully raise their blood pressure apparently are more resilient also to other stressors. For the acute setting, this is also very relevant as it may lead to atypical presentations: an 89-year-old with a systolic blood pressure of 120 mmHg may have a severe sepsis.
In the older patient with a somatic disease, there is an intricate relationship between physical, mental and social function. For instance, an older patient presenting to the emergency department with a severe somatic disease, such as infection or fracture, is at higher risk of getting a delirium. A decrease in physical function may lead to social isolation if mobility of the patient is lost, causing the patient inability to go home after hospitalisation or the other way around: a patient with a depression is at higher risk of social isolation functional decline. As with ageing in general, the same applies to each of these domains: one older patient may be very vulnerable in the physical domain while being mentally very vital, and another patient may be socially isolated and forgetful while being physically vital. These differences are very individual, and therefore, the older patient population is very heterogeneous and the typical older patients do not exist.
Older patients are also different with respect to their treatment preferences. Much more than in younger patients, older patients value the quality of life versus length of life [8]. Whereas a young adult with cancer will typically want the most aggressive treatment to increase the chance of a long life, an older adult may prefer not receiving intensive treatment that reduces the quality of life in what is maybe the last months of their life. Not infrequently older patients choose to not have chemotherapy or an operation but prefer to spend time with their families and make other arrangements regarding the end of their life. However, this also is very individual and may vary between older patients. In similar situations, they may make different choices; decisions should be informed and part of a shared decision-making process.
20.5 Scientific Evidence
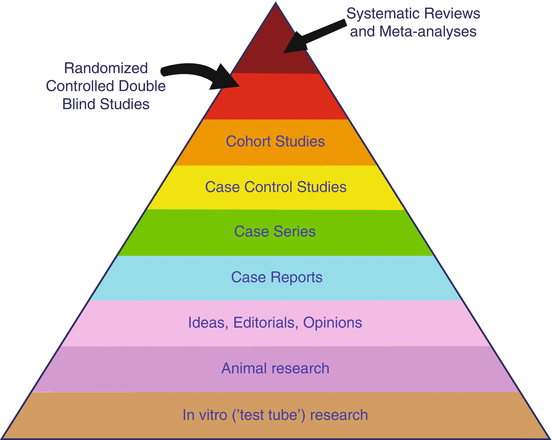
Scientific evidence is generated in different types of studies of which the relevance for clinical patient care varies. The ‘pyramid’ of ‘evidence’ has been widely accepted and shows that at the APEX randomised controlled trials (RCTs) and meta-analyses of RCTs are regarded to have the highest level of evidence. In clinical guidelines, such studies (if conducted properly) would lead to clinical recommendations with a ‘high level of evidence’. Because of this wording, the term ‘evidence-based medicine’ has sometimes been confused with ‘medicine based on RCTs’, disregarding the other two elements of EBM: patient situation and preference and the physicians’ knowledge and clinical expertise.
The fundamental problem with scientific evidence is that older patients are systematically excluded from RCTs, and the older patients that do participate in such trial are not representative of the older patient in clinical practice. In a meta-analysis of all RCTs in 2012, only 7% specifically included older patients [9], much less than the typical proportion of older patients in practice. Another study showed that only 14% of participants in trials on acute coronary syndrome are over 75 years of age [10], whereas their proportion is much larger in the emergency department. Generally, older patients who participate in clinical studies are healthier than patients who visit the doctor. Exclusion criteria often include the use of concomitant medication, renal failure of cognitive impairment. Inclusion criteria often include the willingness and capability to (repeatedly) visit a study centre, obviously selecting for fit and mobile older patients.
Furthermore, RCTs do not study end points so relevant for older patients, such as physical function, cognitive function and quality of life. Typical end points studied in RCTs usually include incidence of cardiovascular disease (in cardiovascular research) or 5- or 10-year survival (in oncology research).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





