Chronic or acute kidney failure
Heart failure—acute or chronic
Hypertensive crisis
Tachy- or bradyarrhythmias
Lung arterial embolism, pulmonary hypertension
Critical ill patients with respiratory insufficiency and septic condition
Acute neurological disease, i.e. stroke or subarachnoid bleeding
Aortic dissection, aortic valve diseases or hypertrophic cardiomyopathy
Contusion of the heart, ablation therapy, pacemaker stimulation, cardioversion or endomyocardial biopsy
Hypothyroidism
Takotsubo cardiomyopathy
Rhabdomyolysis
Myocarditis
Infiltrative myocardial disease like amyloidosis, hemochromatosis, sarcoidosis and sclerodermia
Drugs toxicity, i.e. adriamycine, 5-fluorouracile, herceptine, snake venoms
17.3.6 Treatment
In general, older patients have a high risk of complications during antithrombotic therapy and revascularization. The ACC/AHA guidelines thus recommend for older patients [22, 23]:
- (a)
Decisions on management should reflect considerations of general health, comorbidities, cognitive status, and life expectancy (Ic)
- (b)
Attention should be paid to altered pharmacokinetics and sensitivity to hypotensive drugs (Ib)
- (c)
Intensive medical and interventional management of ACS may be undertaken but with close observation for adverse effects of these therapies (Ib)
Furthermore, the 2015 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation emphasize that despite the lower rate of revascularization in older patients, its benefit appears to be maintained at older age. According to paying attention to altered pharmacokinetics and possible adverse effects of therapies, 10–15% of patients were deemed to have contraindications for aspirin, beta-blockers, and statins. Nevertheless, it has to be suggested—based on registry data—that even in the very old patient, adherence to recommended therapies within 24 h of admission reduces in-hospital mortality [23]. This benefit was observed despite the increased risk of side effects from pharmacological treatment and, specifically, the increased risk of bleeding events associated with antithrombotic therapy in older patients [23]. However, the management strategy must take into account possible end-stage diseases like cancer or dementia and the hereby-accompanied quality of life into account and weigh up costs and benefits of diagnostic and therapeutic interventions.
17.3.6.1 Cardiac Catheterization
More than half of all ACS trials in the last decade did not enroll patients >75 years. This subgroup only accounted for 9% of all patients enrolled in trials [20]. Among patients >75 years of age, the likelihood of catheterization decreased by 15% each year of advancing age [24]. Due to the exclusion of patients based on age, there is only limited evidence for the use of cardiac catheterization in older patients with ACS. For the same reason, there still is uncertainty about the benefits and risks in the use of newer medication in ACS. Comorbidities do not simplify the decision-making either, and older populations are heterogeneous in ways not captured by standard assessments.
Older patients >75 years undergo less cardiac catheterization than younger ones. In the USA, about 77% of older patients undergo cardiac catheterization, compared to 91% in younger patients [24].
The 2015 ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation recommend an early invasive strategy with PCI within 48 h after initial presentation for all high-risk NSTE-ACS patients, whereas high risk implies indicators such as recurrent angina, elevated cardiac markers, ST-segment depression, heart failure, arrhythmias, prior coronary bypass or PCI. It was shown that the older population has a greater benefit in terms of absolute and relative risk reduction in reducing death with early invasive strategy, but these benefits coexist with an increase in major bleeding events [23].
17.3.6.2 Pharmacological Treatment
It has been shown that in-hospital administration of antiplatelet therapy decreases by age, while this is more pronounced for clopidogrel than for aspirin.
According to the ESC guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation guidelines, dual antiplatelet therapy and therefore the use of aspirin and one of the two more potent P2Y12 inhibitors ticagrelor or prasugrel in suspected ACS are highly recommended. The benefit of aspirin does not seem to be affected by age, and its benefit is greatest in highest-risk populations such as older patients [20]. As adjunct to the use of aspirin, the guidelines give a class Ia recommendation for a dual antiplatelet therapy without modification based on age, but there is still a lack of age subgroup data on efficacy and safety of this therapy from randomized trials. In contrast, the 2014 ACC/AHA guidelines for the management of patients with non-ST elevation acute coronary syndromes recommend that either clopidogrel or ticagrelor should be administered in addition to aspirin for up to 12 months to all patients with NSTE-ACS without contraindications who are treated with either an early invasive or ischemia-guided strategy [23].
17.3.6.3 Ticagrelor
A substudy of the Platelet Inhibition and Patient Outcomes (PLATO) trial published in 2012 could show that the clinical benefit of ticagrelor over clopidogrel in patients with acute coronary syndrome with respect to the composite of cardiovascular death, myocardial infarction, and stroke or all-cause mortality, was not significantly different between patients aged ≥75 and those aged <75 years [25]. The authors observed no increased risk of major bleeding complications with ticagrelor versus clopidogrel in patients aged ≥75 years or patients aged <75 years. Side effects like dyspnea and ventricular pauses were more common during treatment with ticagrelor than clopidogrel, with no evidence of an age-by-treatment interaction and no effect on mortality [25].
17.3.6.4 Prasugrel
Prasugrel has several limitations especially in older patients. It should not be given in those with a history of stroke or TIA or patients older 75 years as well as patients with a body weight less than 60 kg.
However, because it still remains unclear whether ticagrelor or prasugrel has a better net clinical benefit in older patients with NSTE-ACS when compared with clopidogrel, the 2015 enrolled “POPular AGE trial (Ticagrelor or Prasugrel Versus Clopidogrel in older Patients With an Acute Coronary Syndrome and a High Bleeding Risk: Optimization of Antiplatelet Treatment in High-risk Older)” is designed to address the optimal antiplatelet strategy in older patients NSTE-ACS patients [26].
In this randomized, controlled, open label, multicenter trial with an estimated enrollment of 1000 patients aged 70 years and older, presenting with non-ST elevation acute coronary syndrome, patients will be randomized to either clopidogrel or one of the P2Y12 inhibitors ticagrelor or prasugrel. Patients will be followed for 1 year for outcomes such as bleeding episodes requiring medical intervention and net clinical benefit, defined as all-cause mortality, nonfatal myocardial infarction, nonfatal stroke, and PLATO major and minor bleeding [27].
17.3.7 Prognosis and Outcomes
In-hospital death rate in patients <65 and NSTE-ACS is 1 in 100, whereas this risk increases dramatically to one in ten in patients >85 years. The 1-year mortality rate for NSTE-ACS patients >75 years is one in five increasing to one in four in patients >85 years [20].
The trends to higher mortality among those not undergoing catheterization were no longer significant after adjustment for predictors of mortality and propensity for cardiac catheterization in the overall population [24]. This supports the need for further studies in higher age populations, as it is suspected that effective therapies are withhold from old people due to the lack of data and higher absolute complication rates.
17.4 General Management of Chest Pain in Older Patients
The general management of acute chest pain should be basically the same as in the general population [28], but frailty needs to be recognized early, and a holistic assessment is mandatory. The management is summarized in Fig. 17.1.
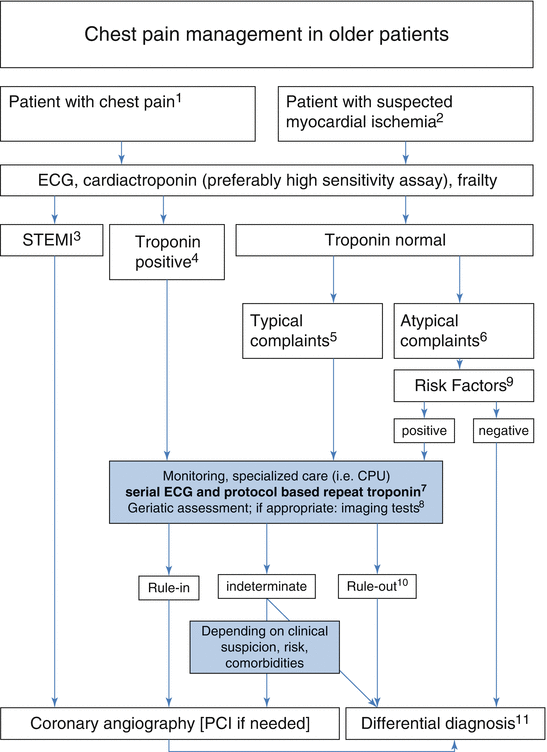

Fig. 17.1




Management of chest pain in older patients. (1) Nontraumatic chest pain without evident extracardiac source; (2) other symptoms include dyspnea and vegetative symptoms like sweating, nausea, vomiting, and shock; (3) STEMI patients are directly ruled in for acute coronary angiography and PCI; (4) troponin positive means above the 99%tile in high-sensitive (HS) assays and above assay-dependent cutoffs in conventional sensitive assays (only if the CV does not allow to use the 99%tile cutoff); (5) typical complaints denote chest pain with radiation in the jaw, back, and both arms, which is not released by the use of nitroglycerin; (6) atypical complaints are punctual, “stabbing” chest pain or episodes which have released already spontaneously or during exertion; specific rule-out strategies are discussed elsewhere; (7) HS troponin every 3 h or in shorter intervals if implemented as protocol, conventional troponin every 6 h; repeat ECG at every clinical event (arrhythmias, significant change of symptoms) and when troponin is repeated; (8) geriatric assessment and comorbidities influencing cardiac troponin levels are crucial; early echocardiography is used in unclear cases to diagnose important differential diagnoses like pulmonary embolism, aortic dissection, or severe heart failure but also to detect regional wall motion abnormalities which support the suspicion of AMI; (9) for risk stratification established scores like TIMI, GRACE, or the HEART score should be used; (10) in case of a negative initial evaluation, an early stress test should be applied within 3 days; (11) differential diagnoses include the important entities mentioned under (8) but also benign disorders like musculoskeletal caused pain, which can be diagnosed on an outpatient basis. Abbreviation: CPU, chest pain unit
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





