Fig. 9.1
Factors involved when staying upright
Risk factors can therefore affect all the mechanisms that help us stay upright.
Having taken a detailed and comprehensive history, one will now be able to think about which factors are likely to be affecting the various systems illustrated above. Consider someone with a non-syncopal fall with a background of diabetes, hypertension and cerebrovascular disease:
Is there any evidence of disrupted cerebral perfusion pressure?Are there significant fluctuations in blood pressure or evidence of symptomatic and clinically correlated orthostatic hypotension?
Has the cerebrovascular disease affected balance—either directly through motor or sensory impairment or more indirectly through disrupting cortical processing pathways?
Is vision affected—stroke, diabetes, hypertension could all perturb vision alongside other common pathologies such as cataracts?
Is joint position sense affected because of diabetic neuropathy or conditions such as arthritis that disrupt large joint proprioception?
Is there a history of middle ear disease or cerebellar problems that could affect vestibular function?
What’s their strength like? It might be MRC grade 5 on formal testing, but can they “get up and go”?
One could divide risk factors into intrinsic or extrinsic as done in Fig. 9.2. Falls are often multifactorial, and the priorities in the ED are to understand the cause and circumstances of the fall, any precipitating factors and the consequences of the fall such as injuries or a prolonged period on the floor. It is important to be thorough with obtaining the history so as not to miss conditions such as Parkinson’s disease, chronic musculoskeletal pain, knee osteoarthritis, cognitive impairment, stroke and diabetes as all increase the risk of falls.
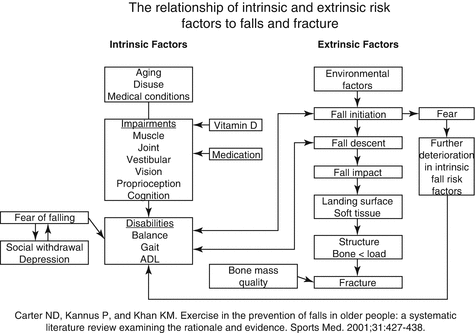

Fig. 9.2
Intrinsic and extrinsic risk factors
Medications are an important risk factor. A meta-analysis from Woolcott et al. showed a correlation with nine unique drug classes; see Table 9.1. Situations where one should be especially careful include new prescriptions and polypharmacy, that is, more than four drugs with at least one in the “at-risk classes”.
Drug class | Odds ratio | 95% CI |
|---|---|---|
Antihypertensive | 1.24 | 1.01–1.50 |
Diuretics | 1.07 | 1.01–1.14 |
Beta blockers | 1.01 | 0.86–1.17 |
Sedatives and hypnotics | 1.47 | 1.35–1.62 |
Neuroleptics and antipsychotics | 1.59 | 1.37–1.83 |
Antidepressants | 1.68 | 1.47–1.91 |
Benzodiazepines | 1.57 | 1.43–1.72 |
Narcotics | 0.96 | 0.78–1.18 |
Non-steroidal anti-inflammatory | 1.21 | 1.01–1.44 |
The patient’s home circumstances are especially relevant as it may provide further clues to falling, trigger the need for a home assessment and influence disposition and rehabilitation. People with dementia are at particularly higher risk of falls and can be very difficult to manage as many have a habit of wandering at night. More than this is when the risk is compounded by inappropriate use of sedatives to reduce these wanderings which translates to increased daytime falls.
The American Geriatrics Society and the British Geriatrics Society (AGS and BGS) guideline recommends everyone aged 65 and over be screened for falls in the ED [12]; this can be carried out with minimal impact on efficiency. A positive answer to any of these puts the patient at high risk of falls.
- 1.
Have you had two or more falls in the last 12 months?
- 2.
Have you presented acutely with a fall?
- 3.
Do you have problems with walking or balance (not necessarily restricting activity)?
These provide context to an unexplained fall as secondary to syncope: abnormal ECGs, heart failure, exertional syncope, family history, sudden cardiac death <40 years, new or unexplained breathlessness, heart murmur, age > 65 and no prodrome and falls irrespective of posture including while sitting.
Postprandial hypotension as a cause of fall or collapse is also increasingly described and appreciated (http://biomedgerontology.oxfordjournals.org/content/60/10/1268.full) as are postprandial reactive hypoglycaemia from ingestion of refined sugar.
9.4 Management
There are two situations when older people present to emergency departments that provide opportunities for improving management of falls and prevention of future ones.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





