, Corinna Eleni Psomadakis2 and Bobby Buka3
(1)
Department of Family Medicine, Mount Sinai School of Medicine Attending Mount Sinai Doctors/Beth Israel Medical Group-Williamsburg, Brooklyn, NY, USA
(2)
School of Medicine Imperial College London, London, UK
(3)
Department of Dermatology, Mount Sinai School of Medicine, New York, NY, USA
Keywords
Non-melanoma skin cancerNMSCBCCBasal cell carcinomaSkin cancerKeratinocyteSun exposureFair skinExcisionBiopsyMohs micrographic surgery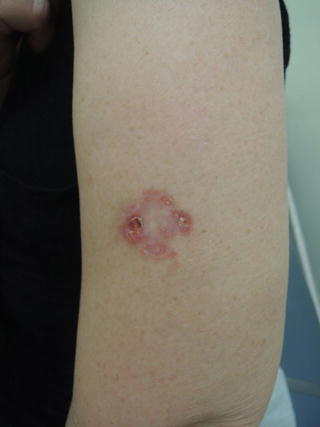
Fig. 7.1
From a distance, note the gross asymmetry of this lesion
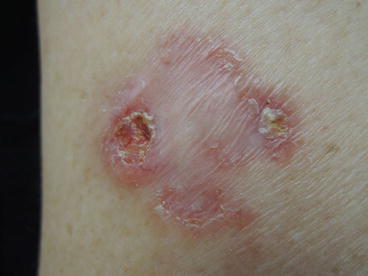
Fig. 7.2
Closer inspection reveals a scaly poorly-demarcated plaque with telangiectasias and an abraded surface
Primary Care Visit Report
A 50-year-old female with no past medical history presented with a rash on her left upper arm that had been there, per the patient, “for at least 10 years.” She said it changed in appearance sometimes but was always dry, scaly, and often itchy. The patient said she tried her best not to scratch it. She also reported that the lesion occasionally bled spontaneously. In the past, she had applied hydrogen peroxide and apple cider vinegar with no effect. She had also tried over-the-counter hydrocortisone cream and moisturizer, both of which made the scab and scale go away, revealing a red base.
Vitals were normal. On exam, on her left upper arm, there was a 2.5 cm × 2.5 cm erythematous, scaly plaque with irregular borders and peripheral scab.
The lesion was suspected to be psoriasis as the patient previously had a rash in her intergluteal cleft, which was diagnosed and treated as inverse psoriasis. However, she was referred to dermatology for further evaluation. At the dermatology clinic, the arm lesion was biopsied and found to be basal cell carcinoma. She subsequently underwent Mohs surgery to remove it.
Discussion from Dermatology Clinic
Differential Dx
Basal cell carcinoma
Amelanotic melanoma
Bowen’s disease
Extramammary Paget’s disease
Squamous cell carcinoma
Lichenoid keratosis
Favored Dx
In this case, biopsy was diagnostic of basal cell carcinoma (BCC). Psoriatic lesions would typically be more thickened. Long-standing pruritic, scaly lesions located in sun-exposed areas and accompanied by spontaneous bleeding, as well as the patient’s fair skin and age, are aspects of the history and physical examination that would raise clinical suspicion of BCC in the absence of biopsy results. This patient’s BCC appears to belong to the superficial subtype (discussed in more detail below), as the lesions are flat and scaly.
Overview
Skin cancers are the most commonly occurring type of cancer, with over one million diagnoses per year in the USA [1, 2]. BCC is a neoplasm of keratinocytes (an epidermal cell that produces keratin) of the lowest, or basal, layer of the epidermis, and accounts for 75–80 % of non-melanoma skin cancers [1, 2]. It affects men more commonly than women, and is considered a cancer of the elderly, although incidence is increasing overall particularly among younger women [1–4]. BCC predominantly affects fair-skinned people [2]. The actual incidence of BCC is difficult to estimate as non-melanoma skin cancers may not be included in cancer registry statistics [1, 5]. Additionally, in some countries only the first instance of BCC is reported, and recurrence as well as multiple lesions are common [3].
The pathogenesis of BCC is complex, and represents an interaction between genetic, phenotypic and environmental factors [5]. The main genetic abnormality in BCC is thought to be upregulation of the Hedgehog (HH) signaling pathway found on the PTCH1 gene, which is responsible for normal tissue maintenance in adult life. UV radiation appears to induce mutations that inactivate PTCH1, p53 and other tumor suppressor genes [2]. PTCH1 mutations are present in 68–90 % of sporadic BCCs [2, 5].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








