Fig. 50.1
(a, b) AP and lateral view chest X-ray : Termination of electrodes at T8 and T10 confirms the absence of obvious lead migration. Images from personal library
At the conclusion of placement, the patient’s electrodes were programmed and the patient was educated on adjusting pulse width and amplitude. After the adjustment session, the patient increased the amplitude to higher values. He was unable to walk because of a wide, fixed, spastic gait with instability. Lying down did not improve the symptoms. A CT brain scan was ordered to rule out a cerebrovascular disorder. Amplitude setting was widely deviated from the initial PACU settings on interrogation (Fig. 50.2).
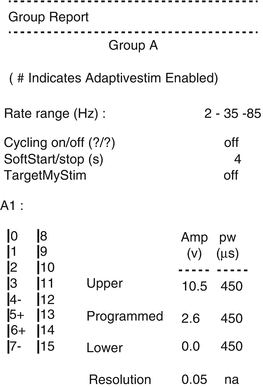

Fig. 50.2
Print out from the implanted stimulator with the set programmed amplitude of 2.6 V that the patient increased during the event to 7.5 V. As seen the adaptive stim has not been yet activated for this patient. This created the need for increase of the amplitude with the side effects described in the text when position was changed from sitting to standing. Symptoms resolved with resetting of the system to lower amplitudes and activation of the position change device. Image from personal library
The amplitude was 7.5 mA (maximum 10.5), adjusted by the patient who did not sense the stimulation while prone. When the stimulator was turned off, sensation and motor control returned almost immediately. Physical examination demonstrated normal gait and no focal neurologic deficits. Thoracic radiography showed no migration of the leads (Fig. 50.1). After adjustment of the settings, the patient’s symptoms improved dramatically and he was discharged home. His pain remained low 2–3/10 on a numeric rating scale.
50.2 Case Discussion
Spinal cord stimulators were first used to treat pain in 1967. The gate theory mechanism of pain hypothesized that the substantia gelatinosa in the dorsal horn of the spinal cord modulates transmission of sensory stimuli. Large fibers inhibit and small fibers activate the gate [1]. At first, neuromodulator devices were placed directly on the dorsal column to stimulate large fibers to inhibit pain transmission. As technology advanced over the next few decades, devices became smaller, safer and more efficacious.
Indications for spinal cord stimulation therapy are failed back surgery syndrome, complex regional pain syndrome, peripheral neuropathy, ischemic limb pain, phantom limb pain, and chronic angina pectoris. Before placement, patients undergo rigorous screening criteria including a minimal response to conservative therapy for at least 6 months and a psychiatric evaluation to exclude somatoform disorders. Prescription or illicit drugs must be discontinued. Finally, there must be no secondary gain or litigation involved with the case.
The larger needle (14G) used to reach the epidural space in SCS tends to increase the risk of unintended intravascular cannulation or damage of vascular structures in the epidural space. Patients older than 65 years who take antiplatelet or anticoagulant medications are at highest risk for spinal hematoma. Symptoms include sharp, transient back and leg pain that can lead to flaccid paralysis. Symptoms tend to develop over hours after implantation, which is consistent with this patient’s presentation.
Epidural abscess is another complication of stimulator placement. In such cases, symptoms of fever, malaise, and back pain develop 1–3 days after placement. Flaccid (early) or spastic (late) paralysis can be experienced, depending on the effect on the spinal cord. Strict aseptic surgical techniques may limit this complication. Imaging studies help to clarify the diagnosis. Our patient did not experience these complications.
About one of three spinal cord stimulator insertions will produce a complication [2]. Surgical revision is required for 23% of patients. The most common reasons are lead migration, lead connection failure, and lead breakage [3]. Lead migration occurs within the first few days after implantation and more often with percutaneous leads than with surgically placed paddle leads. The most common reasons for stimulator removal are infection, equipment malfunction, and unsatisfactory pain relief. Infection was found in 4.6%, and it may be deep or superficial. True hardware malfunction was found in 10% of implantations. Malfunctions can be discovered in the pulse generator, leads, or wires. In the event of a dural puncture on electrode placement, the lead malfunctions temporarily, and the patient may experience a post-dural puncture headache [4]. Patients most likely to respond to stimulators have allodynia [5]. After a 1-week trial that decreases pain by 50%, a permanent system is implanted.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






