Fig. 23.1
Right globe in primary gaze, top view. Green dashed line indicates the plane of the iris; blue dashed line indicates the mid-sagittal plane of the eye and the visual axis through the center of the pupil. The optic nerve lies on the nasal side of the mid-sagittal plane of the eye. Note how the temporal orbit rim is set back from the rest of the orbit rim at or about the globe equator, making for easy needle access to the retrobulbar compartment. A 31-mm needle is advanced beyond the equator of the globe and then directed toward an imaginary point behind the macula, being careful not to cross the mid-sagittal plane of the eye. In a globe with normal axial length as illustrated here, when the needle/hub junction has reached the plane of the iris, the tip of the needle lies 5–7 mm beyond the posterior surface of the globe
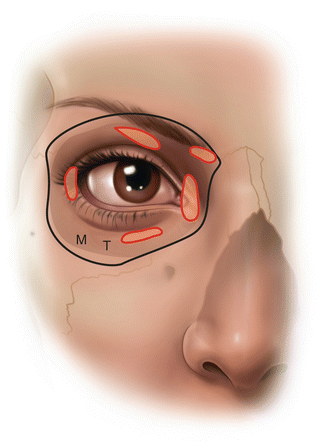
Fig. 23.2
Photo of a patient with a superimposed template of the orbital walls and extraocular muscles at the level of the junction of the optic nerve and the posterior pole of the eye. The traditional inferior block injection site (“T”) is just inside the orbit rim at the junction of the medial two-thirds and lateral third of the inferior orbital rim. A modified injection site (“M”) is just inside the orbit rim at the junction of the inferior and lateral orbital rims. Injection at the modified site is best with a percutaneous approach, the entry point on the skin being 4–5 mm inferior to the lateral canthus
The diagnosis of perforation may be suspected with hypotony, a poor red reflex, a patient complaint of poor vision, or flashes of light; however, more than 50 % of iatrogenic needle penetrations of the globe go unrecognized at the time of their occurrence [22]. The patient may report marked pain and the intraocular pressure will be high if the anesthetic is inadvertently injected intraocularly [29]. Ocular rupture may occur rarely with regional anesthesia as a result of intraocular injection with catastrophic consequences [30].
The initial management of potential/suspected globe perforation requires indirect ophthalmoscopy (fundus examination) by the ophthalmologist [31]. If perforation is identified, immediate referral to a retinal specialist is appropriate. Cases with minimal vitreous hemorrhage enabling a view of the retinal perforation site can be managed with laser photocoagulation or cryotherapy at the time of surgery if the site is outside the macula. If visualization of the fundus is not possible as a result of vitreous hemorrhage, the patient should be referred to a specialist for urgent examination and B-scan ultrasonography to rule out a retinal detachment [29, 31, 32].
Strabismus
Transient diplopia and ptosis is not uncommon for 24–48 h postoperatively when long-acting local anesthetics have been used in large volume for regional anesthesia. However, when this persists for days or weeks, or fails to recover, it may be evidence of toxic reaction within muscle, or damage to the support structures of the ocular motor apparatus. Despite a perfect surgical outcome, the patient will be bitterly disappointed by diplopia if the eyes become permanently misaligned.
Local anesthetics have been used to induce muscle necrosis in skeletal muscle regeneration studies [33–35]. Higher concentrations of local anesthetic agents are more likely to result in myotoxicity [34]. A common cause of prolonged muscle malfunction, whatever concentration has been used, is intramuscular injection [36]. Muscle necrosis, degeneration, and regeneration follow a typical sequence and time course (Table 23.1).
Table 23.1
Time course of muscle degeneration and regeneration induced by aminoacyl local anesthetics
Minutes to hours | Muscle fiber swelling and increased eosinophilia |
|---|---|
Day 1–3 | Phagocytic degeneration of muscle fibers |
Day 4 | Myoblasts appear in remaining basal lamina of degenerated muscle fibers |
Day 5 | Myoblasts fuse to form myotubules (the beginning of sarcomeres) macrophages still present |
Day 7 | Myotubule maturation well underway, organized myofibrillar bundles, macrophage numbers decreasing |
Case 2: A 76-year-old female underwent uncomplicated cataract surgery after a painful infero-temporal retrobulbar block . From the first day after surgery, she complained of vertical diplopia. At day six, her examination was consistent with left inferior rectus under action (inability of the left eye to look down) due to direct intramuscular anesthetic injection. With time there was resolution of the apparent left inferior rectus palsy but then reversal of the vertical diplopia secondary to progressive late fibrosis/contracture of the damaged left inferior rectus muscle (inability of left eye to look up) (Fig. 23.3).
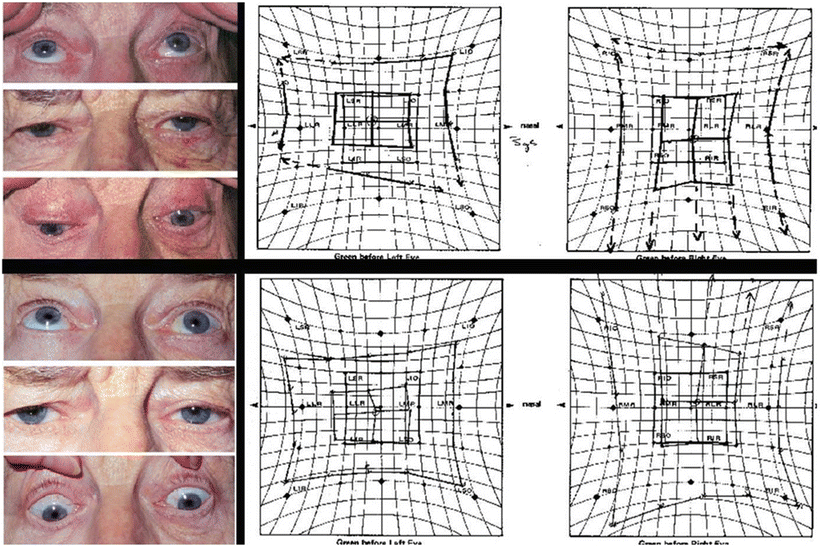

Fig. 23.3
Top: 6 days after surgery, photos and Hess chart show a left hypertropia with limitation of depression of the left eye. Bottom: 2 weeks after surgery, photos and Hess chart show reversal of strabismus to hypotropia of the left eye with restricted elevation
Once the angle of deviation of the eye was stable, she underwent strabismus surgery under general anesthesia with muscle adjustment under topical anesthesia immediately post op and regained a good functional area of single vision.
Etiologies of these muscle malfunctions include direct trauma with anesthetic myotoxicity [36–42], disruption of the LR/SR band which holds the lateral rectus in its anatomical position [43], surgical trauma, inappropriately placed antibiotic injection, and ischemic contracture of the Volkmann’s type after trauma or hemorrhage [39]. It is imperative to have a good three-dimensional knowledge of the anatomy of the orbit and its contents to accurately place injections. A number of articles report damage to the inferior rectus muscle [36, 39, 41, 42], likely associated with the infero-lateral approach of the retrobulbar block and proximity of the muscle. Less frequently affected are the superior oblique [40], the inferior oblique [37], and the superior rectus muscles [38]; however, it should be recognized that any muscle is susceptible depending on needle placement. Extraocular muscles are more easily avoided by using an infero-temporal orbital entry point for the retrobulbar injection .
Effects on Ocular Circulation
After completion of regional anesthetic blocks, mechanical orbital decompression devices [44–47] are frequently used to promote ocular hypotony and reduce the vitreous volume [48], especially when larger volumes of orbital injectate have been used (as in periconal or peribulbar blocks ). Because blood flow to the retina and optic nerve depends on the balance between the intraocular pressure and the mean local arterial blood pressure, it is possible for these devices to induce ischemia [49, 50].
In the presence of significant local arterial disease, orbital hemorrhage, or in patients with glaucoma, vascular occlusion may result [51]. Preexisting small vessel disease, as seen in diabetes mellitus, may increase the likelihood of this complication. The omission of epinephrine from the retrobulbar injectate may be prudent in these cases [25, 52]. The retrobulbar block may also tamponade the vessels within the optic nerve and/or the small vessels supplying the nerve itself either by the volume of drug injected or by causing intrasheath hemorrhage [53–55].
Optic Nerve Damage
The incidence of this complication, while rare, is unknown, as is the exact etiology. Most cases associated with cataract surgery are thought to be due to direct nerve injury or vascular occlusion (central retinal artery or vein) resulting in optic neuropathy. Management would include ocular examination and neuroimaging for confirmation. The administration of systemic steroid has been suggested but its effectiveness remains unknown [56].
Pupillary Anomalies
A permanently dilated pupil may be seen occasionally after intraocular surgery. The pupil fails to constrict with pilocarpine. The mechanism is thought to be related to trauma to the pupillary sphincter from the intraocular surgery itself [57, 58]; however, a case of damage to the ciliary ganglion within the muscle cone has been reported with regional anesthesia for strabismus surgery [59]. In cases of denervation due to ciliary ganglion damage, pupillary constriction in response to topical pilocarpine should be preserved.
Therapeutic Misadventures (Including Systemic Toxicity)
The incidence of systemic toxicity with local anesthetics is related to the total dose given, vascularity of the site of injection, drug used, speed of injection, and whether epinephrine has been used as an additive to delay systemic release. The amount of local anesthetic agent required to be effective in ophthalmic anesthesia is relatively small in comparison with regional anesthesia for most other types of surgery, and so, systemic toxicity is unlikely [15]. That being said, if given rapidly, unintentional intravenous injection of the total volume of local anesthetic required for an eye block may result in systemic toxicity to the CNS and myocardium. Aspirating before injection and injecting slowly reduces the likelihood of this complication. Inadvertent intra-arterial injection of local anesthetics with retrograde flow to the cerebral circulation may result in an acute grand mal seizure [60, 61].
Seventh Nerve Block Complications
An isolated facial nerve block is rarely necessary in modern ophthalmic practice. Complications associated with blocking the main trunk of the facial nerve at the base of the skull have been reported [62, 63]. In these cases, patients experienced difficulty swallowing and respiratory obstruction related to unilateral vagus, glossopharyngeal, and spinal accessory nerve blockade. For facial blockade at this site, experts suggest injecting no deeper than 12 mm and avoiding hyaluronidase in the injectate [63, 64]. Bilateral facial nerve block is not recommended [65].
Allergy
True allergy to local anesthetics is extremely rare [66]. Allergic reactions are almost exclusively confined to the ester-linked drugs (e.g., tetracaine or proparacaine as used in topical anesthesia ). The breakdown product of the esters, para-aminobenzoic acid, is thought to trigger an allergic reaction in certain individuals. Reaction with preservatives, such as methylparabens, in multidose vials is possible; hence, it may be better to use preservative-free vials where a history of the problem exists. Hyaluronidase , an enzyme that enhances the spread of a local anesthetic agent, is sometimes added to the injection and can cause an allergic reaction, as in angioedema [67]. A myasthenia-like response to various agents including local anesthetics has been reported [68]. Well-documented cases of true allergy to amide agents (procaine, mepivacaine, and lidocaine ) have been reported [69, 70].
Anticoagulants and Antiplatelet Therapy
A reduction or discontinuation of anticoagulant therapy for some days is common before nonophthalmic elective surgery. Whereas this action may be appropriate for more major ophthalmic surgical procedures, such as orbital surgery, its advisability in cataract surgery has been questioned. No serious complications were observed in 26 eyes of patients on coumadin who underwent cataract surgery with an extracapsular technique requiring an anterior scleral incision and greater risk of bleeding [71]. Discontinuation of anticoagulant medication may result in thrombotic complications such as cerebral vascular accident, pulmonary embolism, and death. Hemorrhagic complications associated with continuance of anticoagulants, including retrobulbar hemorrhage, had no long-term effects on visual acuity [72]. This implies that the risk of stopping anticoagulants for this type of surgery is probably greater than any risk imposed by their continuance.
As most cataract surgery is performed with a clear corneal incision, the risk in this case is not related as much to surgery as to the choice of anesthesia, where retrobulbar hemorrhage might be possible if regional anesthesia was chosen over topical anesthesia . In a review of almost 20,000 cataract surgeries in nine centers in the USA and Canada, there was no evidence to suggest that patients who continued regular anticoagulation were at more risk of retrobulbar hemorrhage, nor was there evidence that patients who stopped anticoagulation were at increased risk of medical events [73]. At present the medical risks of altering or stopping the regimen of antiplatelet or anticoagulation medication outweigh the risks of regional anesthesia for cataract surgery. Further, there is no strong evidence to support the use of a blunt cannula in a sub-Tenon’s approach over a sharp needle with a peribulbar block [74]. A consensus statement on the perioperative management of patients on antiplatelet therapy for coronary artery disease identified the potential risk of these agents in patients undergoing vitreo-retinal surgery (bleeding within a closed space) [75]. The management of these cases should be individualized and deferred to their medical team. Formal guidelines concur with the last statement as this applies to cases in which the ophthalmic surgery is more complex and the risk of bleeding is higher [76].
Alternative Methods of Ophthalmic Anesthesia
Ongoing reports of rare but serious complications of intraconal anesthesia stimulated editorials and reintroduced the concept of alternative nonakinetic methods of regional anesthesia for ophthalmic surgery [77, 78]. These fall into three groups: subconjunctival (perilimbal) [78–82], injection of local anesthetic by needle or cannula beneath Tenon’s capsule [83–86], and solely topical corneo-conjunctival anesthesia [87–89]. With these methods, the surgeon encounters a varying limitation of ocular movement and lid closure, and sensitivity of intraocular contents, particularly the iris and ciliary muscle with solely topical anesthesia [78, 90]. A systematic search of the literature concluded that retrobulbar block provided better pain control than topical anesthesia [90]. Topical anesthesia is increasingly used for cataract surgeries and intravitreal injection of anti-VEGF agents for the treatment of age-related macular degeneration. Pain control did not appear to be superior with subconjunctival lidocaine injection or a lidocaine-soaked pledget [91].
Intravitreal and subconjunctival injections and sub-Tenon’s infusions are best performed by an ophthalmologist due to the skill and familiarity required for safe ocular manipulation. The patient’s ocular history is important to consider. Previous retinal surgery with scleral buckle may make sub-Tenon’s injection impossible. Similarly, patients with cicatrizing conjunctival diseases (such as Stevens–Johnson syndrome) may not be good candidates for sub-Tenon’s or subconjunctival injections . Extreme caution must be exercised if a patient has had a filtering procedure for glaucoma with a subconjunctival bleb to avoid bleb failure and preserve the conjunctiva for future procedures.
Summary and Current Practice of Anesthesia for Cataract Surgery
Topical anesthesia alone for standard cataract surgery has now been widely accepted as safe, efficacious, and cost effective. The advantages of topical anesthetic over injectable forms of anesthesia include the relative ease of application, elimination of patient pain and anxiety related to injection, avoidance of injection-related complications, and quicker postoperative visual recovery without diplopia or ptosis [92, 93].
Anesthetics which are commonly used include 2 % lidocaine gel, 0.5 % proparacaine, or 0.5 % tetracaine drops. Topical anesthesia is performed by placing local anesthetic directly on the patient’s cornea and conjunctiva. Usually, lidocaine gel is placed within the inferior fornix, and the eyelid is taped closed by the anesthetist 10–15 min prior to draping. An additional sterile anesthetic drop can be given just prior to the actual start of surgery.
Topical anesthesia should not be considered in those with communication problems (deafness, language, comprehension), in younger patients more susceptible to pain, or those with more difficult or complicated cases anticipated to last more than 20–30 min. Drawbacks to topical anesthesia include the risk of corneal toxicity, the short-acting nature of the anesthesia and possible need for intraoperative supplementation, and the lack of globe and lid akinesia which can make even short routine surgery challenging [92].
Topical anesthesia may not provide the same level of pain control compared to retro- or peribulbar anesthesia, as anterior segment structures are not directly anesthetized [94, 95]. Patients may sense pressure changes or discomfort when the iris is touched. As such, intracameral injection of nonpreserved 1 % lidocaine is an effective and safe adjunct to reduce patient pain intraoperatively [96, 97].
Intravenous or oral sedation can be helpful in those patients who exhibit higher than normal levels of anxiety or unease . Although it may not be routinely beneficial [98, 99], in select patients, adjuvant sedation during topical anesthesia can decrease patient pain and anxiety, while improving patient operative satisfaction. It is imperative that blood pressure, heart and respiration rate, and pulse oximetry be properly monitored by trained personnel during sedation. A minimal dose of intravenous midazolam (0.5–1.0 mg) or oral diazepam (2.5–5.0 mg) is often adequate to avoid oversedation, allowing for both full patient cooperation during surgery and a smooth, uneventful postoperative recovery [100].
Sub-Tenon’s Anesthesia
Sub-Tenon’s anesthesia was introduced in the late 1990s as a safer alternative to the rare but sight-threatening complications of peribulbar and retrobulbar blocks [101]. An incision is made in the inferonasal conjunctiva, 7–10 mm from the limbus. This location is preferred as it avoids the typical sites of retina and anterior segment surgery. Using scissors, Tenon’s capsule is carefully dissected posteriorly toward the inferonasal quadrant. A blunt curved cannula is then inserted through the opening in the conjunctiva and directed posteriorly. The local anesthetic mixture is directed toward the posterior globe.
This block has been rapidly adopted because of its simplicity and presumed safety. In the United Kingdom, a recent survey of anesthesiologists indicated that 87.8 % of respondents used this technique regularly in their practice [102]. Previously, sub-Tenon’s block was either used to augment peribulbar and retrobulbar blocks or used primarily in patients at risk of bleeding. However, recent studies have proven sub-Tenon’s blocks to provide excellent akinesia and anesthesia during surgery . In a recent case series of 6000 consecutive sub-Tenon’s injections reported by Guise [103], 96 % of all blocks were rated by the surgeon as suitable for surgery.
Studies documenting patient pain with sub-Tenon’s anesthesia rated this symptom as mild in 25 % of cases with moderate and severe pain only occurring in 5.4 % and 1.5 %, respectively [103]. This was subjectively described as a “stinging or burning” sensation or a “pressure” sensation when the sub-Tenon’s space was being expanded [104]. Some guidelines have suggested that the most effective way to reduce pain is adequate local anesthetic and careful insertion of the cannula with slow infiltration of anesthetic solution [105].
Ophthalmologists and anesthesiologists consider sub-Tenon’s blocks to be safe. Complications occur frequently, but are of limited clinical significance including pain, chemosis, and subconjunctival hemorrhage. Subconjunctival hemorrhage occurs through the dissection of the conjunctiva or through disruption of the small blood vessels when the cannula is introduced and the anesthetic infiltrated. Typically, the hemorrhage involves only one quadrant, but can potentially spread more circumferentially [106]. Previous studies have reported hemorrhage in 7.4 % to 100 % of cases [103, 105].
Chemosis typically indicates anterior spread of the anesthetic during injection or incorrect injection into the subconjunctival space [105]. This can be confined to the injection site or can move to other quadrants. The incidence of chemosis can be reduced with the use of a longer cannula and gentle side-to-side movement along with infiltration of lower volumes of anesthetic [107]. Typically, this is not an issue with retina and cataract surgery but may adversely affect glaucoma filtering surgery.
Although rare, major life- and sight-threatening complications include: brainstem anesthesia, globe perforation, retrobulbar hemorrhage, retinal ischemia, optic nerve damage, rectus muscle dysfunction, and orbital cellulitis. Signs of brainstem anesthesia are quite variable from drowsiness, confusion, loss of verbal ability, to more serious complications of cranial nerve palsy, convulsions, respiratory depression, and cardiac arrest. Two cases of brainstem anesthesia have been reported in the literature following sub-Tenon’s anesthesia. The first case, reported by Ruschen, resulted in prolonged unresponsiveness to verbal commands and a reduced Glasgow Coma Scale for 3 h following uneventful sub-Tenon’s block [108]. Cardiorespiratory depression did not occur and there were no focal neurological signs. Eventually, the patient made a full recovery without any persistent neurological sequelae. Quantock and Goswami reported another case in an 82-year-old woman who was blocked for cataract surgery [109]. One minute after performing the block the woman had a generalized tonic–clonic seizure and went into ventricular fibrillation. Cardiopulmonary resuscitation was not successful and the patient died; autopsy showed severe coronary artery disease.
Globe perforation has been reported in 3 cases; one was identified 5 weeks after surgery and the remaining two were known at the time of surgery. Of these two, the first case reported by Frieman and Friedberg occurred in a 40-year-old male with a previous scleral buckle who was undergoing a second rhegmatogenous retinal detachment repair [110]. Upon opening the conjunctiva, resistance was present, so sharp scissors were used to cut the tissue and release adhesions [110]. Upon advancing the scissors, the resistance dramatically decreased and the globe suddenly became soft. Indirect ophthalmoscopy identified a vitreous hemorrhage with a small perforation. The second case, reported by Faure and colleagues, occurred in a patient with previous scleritis who was undergoing cataract surgery [111]. During surgery, a vitreous air bubble was noted after the placement of the intraocular lens. Vitrectomy confirmed the location of two retinal breaks with a localized retinal detachment in the infra-nasal quadrant.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree





