Fig. 13.1
Emilia-Romagna, Italy
Fig. 13.2
Emilia-Romagna integrated trauma care system (SIAT)
The SIAT works according to hub and spoke model: severe and resource-consuming patients are centralized in first-level hubs to guarantee high-quality and efficient care. Every SIAT has a trauma center (hub) connected with a net of peripheral hospitals (spokes).
The main goal of a SIAT is to organize and manage trauma care pathways, to enable quick and adequate treatments in the same way everywhere.
Bufalini Hospital in Cesena is the hub for the Area Vasta SIAT and serves a catchment area of about 1 million people doubling during summertime because of its geographical position on the Adriatic coast.
Moreover, at the Bufalini Hospital a hemophilia center and a thrombosis and hemostasis center inside the transfusion medicine ward are present in order to guarantee consultation on congenital and acquired bleeding disorders.
In 2001 the regional healthcare plan was published, and for the accreditation of the emergency department, a specific protocol and standard operative procedure for the management of major blood loss were required.
A multidisciplinary team for the implementation of the transfusion policy was created involving traumatologists, emergency physicians, and transfusion medicine specialists with expertise in hemostasis.
A first formula-driven protocol for the management of trauma-induced coagulopathy was adopted for the prompt release of the blood component therapy.
In 2012 the protocol was implemented with the introduction of the thromboelastometry (ROTEM) device. The instrument was located in the intensive care unit (ICU), and an intensive training course was started. All the anesthetists and transfusion medicine specialists were trained by classroom lessons with a ratio of one tutor to three students. Every lesson lasted 4 h: two hours of theory and two practical hours of hands-on ROTEM using blood samples from patients in the ICU. Every year a refresh course is organized.
Before introducing the device in the clinical practice, a verification of ROTEM reference ranges was conducted performing assays on blood samples from 20 healthy blood donors with normal coagulation, and results were compared with the reference ranges provided by the manufacturer.
A specific algorithm was defined for the coagulation support to the trauma bleeding patients, and a laminated poster with the algorithm is present in the ICU and in the blood bank.
In the emergency department are available 6 units of zero negative red blood cells, 3,000 units of prothrombin complex concentrates, and 2 g of fibrinogen.
During the management of a major trauma patient with coagulopathy, in order to reduce the turnaround time and the time to treatment, a nurse or a porter is dedicated to the transportation of the blood sample to the ICU where the testing is immediately started. The ROTEM device is electronically connected to the blood bank monitor, where a transfusion medicine specialist oversees the trace and orders the administration of coagulation factor concentrates stored in the emergency department near the patient and immediately releases blood component therapy (platelets or fresh frozen plasma if needed) (Fig. 13.3).
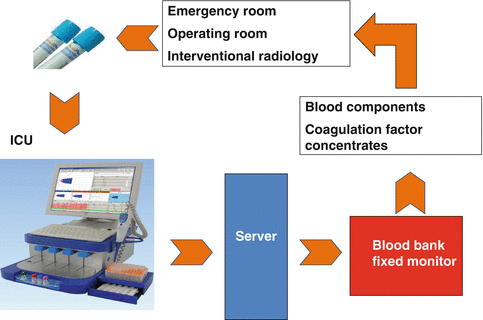

Fig. 13.3
Cesena organization
In 2013 the Cesena Trauma Center adopted the ECS protocol [7, 8] from the Italian Trauma Update research group obtaining a statistically significant reduction of the transfusion of blood products in the first 24 h and during hospital stay (see Chap. 7).
After the positive experience in the setting of trauma, a second ROTEM instrument was introduced for the management of postpartum hemorrhage and perioperative bleeding with the same organization showed in Fig. 13.3.
The implementation of the goal-directed therapy by using ROTEM device has been useful not only for the reduction of transfusion therapy during critical bleeding but also to improve the multidisciplinary approach among different specialists.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






