General
Dental
Ophthalmologic
Orthopedic
Plastic
Urologic
Number (Percent)
35 (8.9%)
43 (10.9%)
24 (6.1%)
118 (30.0%)
133 (33.8%)
40 (10.2%)
Amazingly, 98% of Snow’s patients survived. Of the five who died, only one underwent surgery, and that death resulted from uncorrected hemorrhage and occurred several days after the surgery (Table 65.2). The other patients had anesthesia for reasons that we would smile upon today.
Patient age | Reason for anesthesia | Comment |
|---|---|---|
3 yrs | Pertussis | Anesthetized for treatment of pertussis’died 1 day post anesthesia |
2 yrs | Status epilepticus | Weak, rapid pulse during anesthesia. Died 1 hr after awakening from anesthesia, still in status |
1 yr | Meningitis | Seizures and increased intracranial pressure pre-anesthesia. Died with fixed and dilated pupils |
16 yrs | Above knee leg amputation | Hemorrhage during and after surgery. Died 4 days after surgery |
17 yrs | Typhoid fever | Died post anesthesia’possibly from dehydration |
As Table 65.2 indicates, anesthetic failures joined successes. Shortly after the introduction of chloroform, 15-year-old Hannah Greener died during removal of a toenail under chloroform, the first reported anesthetic death in a child [7]. She had survived a previous anesthetic with ether.
John Snow’s remarkable safety record overshadowed that of his peers, both because of his genius and because, in contrast to the occasional anesthetist, he practiced anesthesia nearly full time. Today, 6.5 children die per 100,000 anesthetics (excluding cardiac surgery) [8]. Under Snow’s care, 20 per 100,000 died’in a less than friendly environment’mostly homes or surgeon’s offices, and without monitoring, intravenous fluids, antibiotics, or postoperative pain relief [6]!
Like adults, children benefited from the introduction of anesthesia. Surgeons were not rushed by patient screams, and previously impossible surgical procedures were now possible: repair of congenital anomalies, gastrostomies, excision of tumors, and increasingly intricate orthopedic procedures. However, for a half-century, surgeons rarely entered the thoracic or abdominal cavities (e.g., see Table 65.1) because of unacceptable post-operative infection rates and pulmonary failure.
For more than a century after the discovery of anesthesia, ether or chloroform given by “rag and bottle” were the primary anesthetics administered to children. Ethyl chloride was a minor addition. It was introduced into Europe as a general anesthetic in 1894, and spread to Britain, the British Commonwealth, and the US in the beginning of the twentieth Century. It was commonly used for dental anesthesia, especially in children (Fig. 65.1). Although Snow recognized the great advantage of control over the concentration of anesthetic delivered, the general use of reliable versions of anesthetic delivery was delayed for a century. Precision vaporizers (e.g., the Copper Kettle) appeared in the 1950s, and radically increased the control over and safety of anesthetic delivery.

Fig. 65.1
Rupert Hornabrook (Australia’s firt full-time anesthesiologist) produces anesthesia with a spray of ethyl chloride to a cloth held to a child’s face. (Courtesy of Rod N. Westhorpe and the Geoffrey Kaye Museum of Anaesthetic History)
Ether stimulated ventilation, an advantage that Snow recognized [9] and Gregory et al. quantified 113 years later [10]. The adult ether masks commonly applied to children, imposed dead space and thus increased rebreathing and carbon dioxide (hypercarbia), and decreased oxygen (hypoxemia). Better to use ether than chloroform since the latter depressed breathing leaving the child more vulnerable to oxygen lack and rebreathing of carbon dioxide. In the 1890s, the concurrent administration of oxygen with ether allowed anesthetists to minimize hypercarbia and hypoxia. Frederick Hewitt (1857–1916) thought this especially helpful for children.
By the early nineteenth century, physicians recognized that children differed from adults in more than size. This recognition led to the development of Children’s hospitals (Table 65.3) and associated specialties. Just as it took time for anesthesia to be recognized as a medical specialty in its own right, pediatric anesthesia did not develop as a subspecialty until the first half of the twentieth century. Until 1900, it was likely that the hospital physician, the surgeon’s assistant, the family doctor or a nurse would administer the anesthetic given to a child.
Table 65.3
Founders and founding years for early pediatric hospitals
Founded | Hospital | Founder(s) |
|---|---|---|
1778 | Hôpital Necker’Enfants Malades (Paris) | Madame Necker |
1802 | Hospital des Enfant Maladies (Paris) | Conseil général des Hospices |
1821 | National Children’s Hospital (Dublin) | Henry Marsh, Philip Crampton Charles Johnson |
1852 | Hospital for Sick Children, Great Ormond St (London) | Charles West |
1855 | Children’s Hospital of Philadelphia (Philadelphia) | Francis W Lewis, T Henson Bache, Charles Bingham Penrose |
1869 | The Boston Children’s Hospital (Boston) | Francis Brown and associates |
1870 | National Hospital, National Medical Center (Washington, DC) | Board of Lady Visitors, DC Busey, F.A. Ashford, William B. Drinkard, & William W. Johnston |
Most pediatric surgery in the nineteenth century was for minor ailments. Intrathoracic and intra-abdominal surgery awaited the invention of antisepsis and asepsis, developments of the late 1800s. Asepsis and antibiotics were as important to the surgical care of children as they were to adults. Without control and treatment of infections, pediatric surgery (and hence anesthesia) could not advance, especially since the immune system of neonates and infants is less developed than that of older patients [11]. Before asepsis, infection-induced mortality of children following surgery sometimes exceeded 90%.
With the development of the subspecialty of pediatric anesthesia, it became clear that patients cared for by pediatric anesthetists had fewer complications and fewer anesthesia-related deaths than patients cared for by adult anesthetists [12,13]. Those caring for many patients with similar problems provided better results than those caring only occasionally for such patients. Today, children’s hospitals in the United States, and elsewhere, are the backbone of pediatric care and research.
Adventurous Surgery
Two congenital anomalies awaiting anesthesia and asepsis for their successful repair were omphalocele (a large midline abdominal hernia) and gastroschisis (an intrauterine vascular accident that produces a large lateral abdominal hernia). For both anomalies the abdominal contents protrude through the abdominal wall at birth. These lesions are easily repaired and today more than 95% of such infants survive. In the early 1800s, William Hey (1749–1819) and James Hamilton (1749–1835) accomplished the first successful repair, doing so without anesthesia or antibiotics.
In 1889, Joseph O’Dwyer of New York City failed in his attempt to repair an infant’s congenital diaphragmatic hernia (CDH). In 1905, Lothar Heidenhain (1860–1940) in Germany successfully repaired the CDH of a 9-year-old. Repair of CDH then and now exacted an invariant heavy price. Mortality exceeded 50% in 1925 and hasn’t changed much since, despite Intensive Care Nurseries (ICNs), mechanical ventilation, and extracorporeal membrane oxygenation (ECMO) [14].
In 1939, William Ladd (1880–1967), in Boston, was the first to repair a tracheo-esophageal fistula (TEF; a connection between the trachea and esophagus), another usually lethal congenital lesion [15]. Ladd favored a two-stage approach (he first closed the fistula and fed the child through a gastrostomy until the child had grown. He later repaired the esophageal atresia). In 1941, Cameron Haight (1901–1970) of the University of Michigan ligated the fistula and did a primary repair of the esophagus as a single procedure [16], inventing the treatment used today. Ether or chloroform given via mask to spontaneously breathing patients supplied the anesthesia for early TEF repairs. Mortality exceeded 70%. Today nearly all these patients survive if they have no other congenital anomalies.
In 1946, Alfred Blalock (1899–1964), a surgeon, and Helen Taussig (1898–1986), a pediatrician at John Hopkins Medical Center, devised an operation to treat infants with Tetrology of Fallot. Tetrology of Fallot is a congenital defect that diverts blood flow from the lungs, limiting oxygenation of the arterial blood and resulting in a “blue baby” [17]. Merel Harmel (1917–) and Austin Lamont (1905–1969) anesthetized the first 100 of these patients [18], doing so with minimal monitoring (they felt the pulse, counted respiration and occasionally measured blood pressure in most cases). Some patients breathed spontaneously via a facemask, even when the chest was open! Patients recovered in the operating room and were cared for on the ward after surgery. Mortality was remarkably only 25%, a testimony to the skills of the anesthetists and surgeons’and the resilience of young children!
For decades, surgeons sought to repair congenital abnormalities in utero [19], thinking it would improve outcomes. Target lesions included diaphragmatic hernias, teratomas, anomalies of the lung (e.g., cysts), and possibly cleft lips. In utero repair of cleft lips might have the great advantage of leaving no scars. But can we anesthetize the mother without excessive depression of the fetus? Biehl et al. showed that the maternal MAC was considerably greater than the fetal MAC (e.g., see Fig. 65.2) [20]. And fetal surgery may precipitate premature labor’a disaster at 20 weeks gestation because birth at this age is not compatible with extra-uterine life. Fetal surgery remains a tantalizing possibility for several lesions, and a success for others (e.g., twin-twin transfusion).
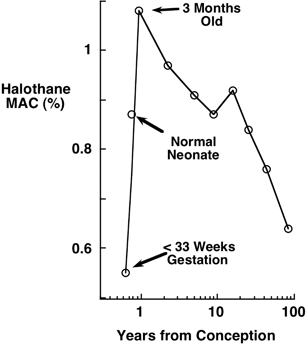
Fig. 65.2
Anesthetic requirement (MAC) for halothane changes with ageing. MAC is the minimum alveolar concentration of anesthetic needed to suppress movement in response to surgery
Giants Appear
With the end of World War I, came the appearance of the first giants in pediatric anesthesia, anesthetists who prompted the development of the discipline. These included Charles Robson (1884–1969), Betty Lank (1904–2002), Robert Smith (1913–2009), M Digby Leigh (1904–1975), M Kathleen Belton (1916–1980), C Ronald Stephen (1916–2006), Philip Ayre (1902–1980), and Gordon Jackson–Rees (1918–2001; Fig. 65.3). Beyond a focus on children, all of these clinically skilled anesthetists shared a love of teaching, and several advanced the science of pediatric anesthesia.

Fig. 65.3
Gordon Jackson-Rees (Courtesy of Rod N. Westhorpe)
Robson, considered the father of pediatric anesthesia, returned from World War I to become Anaesthetist-in-Chief at the Hospital for Sick Children in Toronto. He defined the major problems extant in pediatric anesthesia’and their solutions [21]: children differed from adults in their physiology and their response to drugs (e.g., children “take more anesthetic … than do adults” a fact later quantified) [22–24]. Children, he said, require anesthesia equipment designed for their needs (what a concept!), and in conflict with beliefs of some surgeons, he argued that operating on a child without adequate anesthesia was “vivisection”.
Robson advocated simple vital aspects of pediatric care, including recognition that induction of anesthesia with an inhaled anesthetic required maintenance of a patent airway. He claimed that “starvation” prior to surgery led to acidosis, and he fed children “strained gruel” up to four hours beforehand, withholding food after that to minimize vomiting, aspiration, and possible lung injury or death. He warned that “accident cases” and patients in pain took longer to empty their stomachs and were at greater risk of vomiting and aspiration. He suggested the insertion of a gastric catheter to relieve the gastric distention of patients who had pyloric stenosis (a constriction at the exit from the stomach). He administered ether as his anesthetic of choice, by open drop or by insufflation via an “ether hook.” (i.e., he “blew” ether into the mouth). He did not hesitate however, to use tracheal intubation, especially when using cyclopropane, a respiratory depressant, for complicated cases.
A little south of Robson, William Ladd (1880–1967) was busy in Boston Children’s Hospital developing Pediatric Surgery (he was its ”father”). Betty Lank, the Chief Nurse Anesthetist at Children’s from 1936 to 1957, enabled Ladd’s success [25]. She adapted Riva Roca’s measurement of arterial blood pressure to children, initially making the blood pressure cuffs herself. She designed and had built, size-appropriate facemasks and breathing bags for children’later produced by Foregger [26]. She had anesthetic firsts to brag about: Ladd’s first patient for tracheo-esophageal fistula repair in 1939; Gross’ (1905–1988) first patient for ligation of a patent ducts arteriosus in 1938 [27], and his first patient for repair of a coarctation (narrowing) of the aorta in 1945 [28]. She was the first to administer cyclopropane to children in the United States. She usually gave ether or cyclopropane via mask, even to prone patients (something that would terrify today’s anesthetist).
Smith learned anesthesia in a three-month US Army course during World-War II. In 1945, he arrived at the Boston Children’s Hospital “knowing very little” about pediatric anesthesia (Personal communication), his previous patients having been soldiers. Smith said Lank “made me a pediatric anesthesiologist”. His first rate training program in Pediatric Anesthesia influenced the development of pediatric anesthesia worldwide.
Leigh, another early force in pediatric anesthesia, asked difficult, intriguing questions. He contributed a one-way valve that reduced the amount of carbon dioxide re-inspired by children during surgery. His textbook “Pediatric Anesthesiology,” written with Belton in 1948 [29] preceded Smith’s book (above) and contained much of what we “know” today, albeit based on an enormous amount of informed speculation.
A fourth early North American (another Canadian) pioneer of pediatric anesthesia’also a product of World War II’was Stephen. An outstanding teacher, he published a small textbook “Essentials of Pediatric Anesthesia” in 1954 [30]. He was among the first to (appropriately) raise concerns regarding the effects of operating room temperatures on patient well being. Like Leigh, he developed a valve to prevent carbon dioxide rebreathing.
The first textbook of Pediatric Anesthesia “Anesthesia in Children” was published in Great Britain in 1923 [31]. The next such book, “Précis Clinique et Opératoire de Chirurgie Infantile” was published in France 1925 [32]. Following the publication of Leigh and Belton’s book, in 1950, Smith wrote the first comprehensive textbook on “Anesthesia for Infants and Children” and therein, concisely described how to provide anesthesia for infants and children undergoing various surgical procedures [33]. Gregory’s textbook “Pediatric Anesthesia” was the first physiology-based pediatric anesthesia textbook [34].
The increasing interest in pediatric anesthesia was not confined to North America. The Englishman, Philip Ayre, invented a simple system for delivery of anesthesia to children undergoing craniofacial surgery [35], His “T”-piece (Fig. 65.4) avoided the imposition of increased resistance to breathing, particularly important for infants having cleft lip and palate surgery, and allowed him to get his hands out of the surgical field.
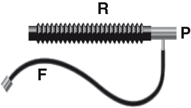
Fig. 65.4
Ayre’s “T”-piece consisted of a T connected to the tracheal tube at P and to a reservoir tube, R. Gas containing anesthetic entered the system through F. Intermittently occluding the otherwise open end of R caused ventilation of the patient’s lungs. (www.frca.co.uk/ images/ayre1.gi. Accessed 31/03/2010)
Ayre was a master pediatric anesthetist. Like many of his patients, he had a cleft lip and palate, badly repaired, and he spoke with a “honking” sound that adults found difficult to understand. But his voice apparently mesmerized children, especially during induction of anesthesia, distracting them from the vapors they breathed.
Electronic versions of Ayre’s simple device underlie many modern pediatric ventilators. Gordon Jackson–Rees (1918–2001) added an open-ended bag to Ayre’s “T”-piece; the bag could be used to control or assist ventilation [36]. We used this modification to provide Continuous Positive Airway Pressure (CPAP) and improve the outcome of premature infants who had hyaline membrane disease (HMD) (See below) [37].
Control of Breathing
Anesthetists recognized early on, that airway obstruction commonly occurred with induction of anesthesia, particularly due to the tongue falling to the back of the oropharynx, and collapse of the upper airway. In 1847, Francis Sibson (1814–1876) applied a jaw thrust (lifting the jaw at its angles) to treat this problem [38], and Snow also suggested maintaining light anesthesia and jaw thrust. In 1908, Frederick Hewitt made an oropharyngeal airway roughly similar to those used today to treat this problem [39].
The increasing demands of surgery, particularly surgery of the chest, abdomen, and cranium, required better control of the airway and a need to protect the airway from contamination with blood, pus, and gastric contents. It required that the anesthetist ensure adequate ventilation and oxygenation. The solution lay in passage of a tube into the trachea, and in this, both surgeons and anesthetists led the charge. In 1882, Joseph O’Dwyer (1841–1898), a New York surgeon, used one of the first “tracheal tubes” (really a tube into the larynx) when he inserted a metal tube into the glottis of children to bypass the pseudo membranes of diphtheria that caused glottic obstruction and death [40]. He adapted the positive pressure artificial respiration apparatus developed by his colleague George Fell, by replacing Fell’s mask with O’Dwyer’s glottic tube. He was thus able, when necessary, to ventilate the patient’s lungs with air supplied by a foot-operated bellows (Fig. 65.5).
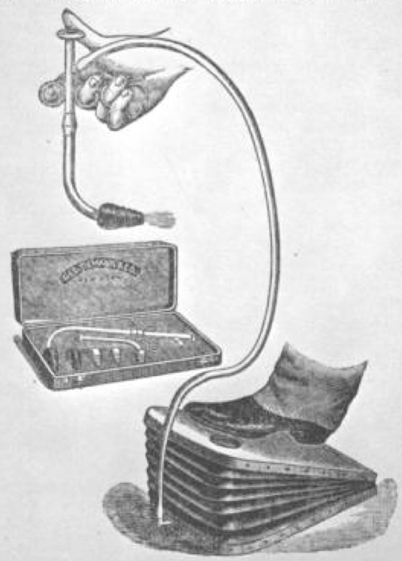
Fig. 65.5
The Fell-O’Dwyer apparatus. The O’Dwyer tube was held in the operator’s hand and passed into the glottis. To ventilate the patient’s lungs, a bellows was compressed with the foot and the opening on top of the tube occluded with the thumb. During exhalation, the thumb was removed and gas exited the lungs through the opening in the top of the tube. (Courtesy of AATS: Founders)
After initial failure with a spring-loaded device intended to insert his tube into the glottis of children, O’Dwyer placed the tube blindly by lifting the epiglottis with a finger, sliding the tube along that finger and into the glottis, a technique still occasionally used today (Fig. 65.6).
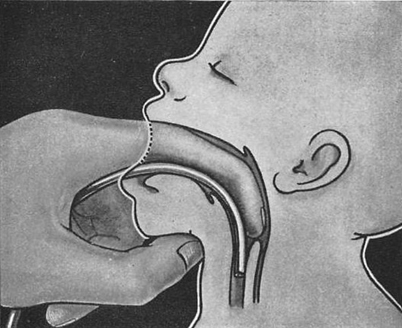
Fig. 65.6
In the “digital” method of tracheal intubation, the index finger was passed into the mouth and the epiglottis is lifted (note identity to the approach used with the MacIntosh blade). A tracheal catheter was passed along the finger and into the trachea. The author was taught this method of tracheal intubation as a medical student before a full time anesthetist (Sol Shnider’1929–1994) directed anesthesia in the delivery room at UCSF and taught us to use a laryngoscope to visualize the glottis for tracheal intubation. (http://www.hmc.org.qa/mejem/mar2002/comm/comm1.htm. Accessed 31/03/2010)
The Scottish surgeon William Macewen (1848–1924) was the first to use tracheal intubation to deliver anesthesia. He inserted a tube into the trachea of a patient with tongue cancer in 1878, to facilitate excision of the mass [41]. In the early twentieth century, surgeons Charles Elsberg (1872–1948) of New York and Rudolph Matas (1850–1967) of New Orleans, used blind tracheal intubation and manual ventilation of the lungs to facilitate thoracic surgery. At approximately 1920, Ivan Magill (1888–1996) and Stanley Rowbotham (1878–1979) developed laryngoscopes that allowed anesthetists to visualize the glottis of children [42]. Despite the availability of laryngoscopes and tracheal tubes, neonates and infants seldom underwent tracheal intubation until the advent of pediatric thoracic and cardiac surgery, and even then many were anesthetized with open drop ether! Early tracheal tubes were stiff, often made of hard rubber or latex covered spiraled wire, thick-walled devices that increased resistance to gas flow and caused airway damage.
Cole seemingly solved the resistance problem by making tracheal tubes with a short, narrow distal end that inserted into the trachea. This short end connected to a wide bore, low resistance tube [43] (Fig. 65.7). The shoulder at the junction of the larger and smaller tubes sat on the vocal cords and reduced the incidence of bronchial intubation. However, in 1969, Bernard Brandstater (1929–) reported that downward pressure could force the upper wide portion of the tube between the vocal cords and damage the larynx [44].
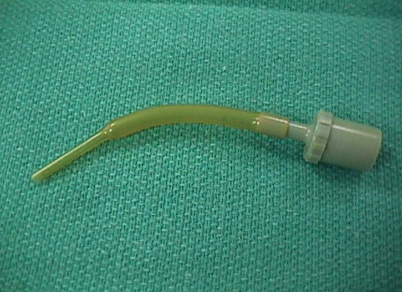
Fig. 65.7
The Cole tube had a wide (low resistance) upper part and a short narrower (higher resistance) lower portion; the short portion was placed into the trachea. The beveled portion rested on (and could distend) the vocal cords. (old.cvm.msu.edu/services/aneth/docs/cat-intu/. Accessed 31/03/2010)
Brandstater was one of the pioneers of prolonged intubation in infants. While working at the American University in Beirut in the late 1950s, he achieved encouraging results in 40 infants with tetanus, intubating the trachea with soft polyvinyl chloride tubes, and ventilating their lungs with room air. He used a Harvard sine wave pump from the research laboratory, carefully covering the plaque, which read “For use in laboratory animals only”. In 1963, Tom Allen (1923–2011) at the Children’s Hospital in Adelaide, Australia, introduced prolonged nasal intubation as an alternative to tracheotomy for croup, and his paper with Ian Steven (1926–2006), published in 1965, paved the way for prolonged airway management in children [45,46].
Thin-walled plastic tracheal tubes replaced Cole tubes in the 1970s. These low resistance tubes tempted practitioners to leave tubes in the trachea for protracted periods to facilitate mechanical ventilation and avoid tracheotomy. Early on, however, practitioners discovered yet another problem: plasticizers in the tubes damaged the trachea and caused subglottic stenosis (narrowing of the trachea) [47]. Removing the plasticizers allowed safer prolonged tracheal intubation.
In 1939, Noel Gillespie (1904–1955) developed a pediatric laryngoscope. Robert Miller (1906–1976) improved on this design in 1946 [48], and “Miller” laryngoscopes became fixtures in delivery rooms, neonatal intensive care units, and operating rooms throughout the world. Other designs specifically tailored to pediatric practice were subsequently introduced. In the past 15 years, newly developed fiber optic intubation equipment has proven useful for guiding tracheal intubation of infants and children with upper airway anomalies.
The T-Piece
Before 1937 it was difficult to ventilate the lungs of neonates undergoing head and mouth surgery because the anesthetist competed with the surgeon for airway space. As noted earlier, Ayre solved this problem with his T-piece (Fig. 65.8). He achieved induction of anesthesia via a mask and then intubated the trachea and attached his device to the tracheal tube, thereby removing his hands from the surgical field and out of the “cranky surgeon’s” way [49]. Ayre believed this approach decreased pallor, tachypnea (rapid breathing), and respiratory distress during and immediately after surgery. His elegantly simple device imposed little resistance to spontaneous breathing. The T-piece had another virtue’it could be used to ventilate the lungs of patients by intermittently obstructing the gas outflow from the T-piece. In 1963, Keuskamp (1915–1992) of Amsterdam, devised the first pediatric ventilator, the LOOSCO, using a solenoid to intermittently “thumb” the gas outlet from what effectively was an Ayre’s T-piece [50]. People called this machine the “electronic thumb”. Some modern infant ventilators use this T-piece principle.
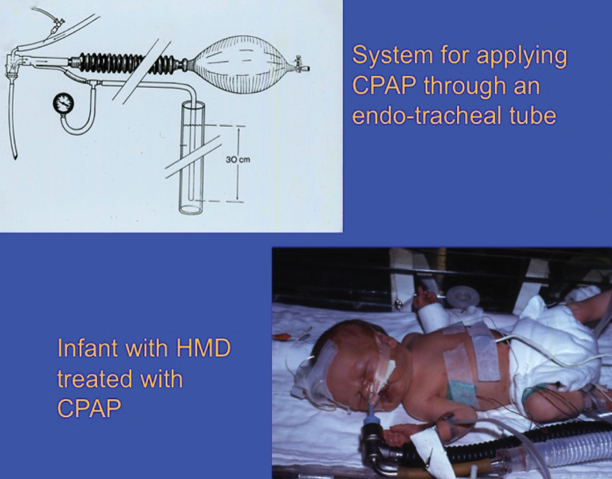
Fig. 65.8
The upper picture is a drawing of the Jackson–Rees modification of the Ayre’s “T”-piece. We added an under water “pop off valve” which set an upper limit to the pressure that could be applied and thus minimized the incidence of pneumothorax. The lower picture shows this device applying CPAP to a preterm baby
Jackson–Rees (1918–2001) modified Ayre’s T-piece by adding a bag to the expiratory tube so that he could ventilate the children’s lungs by squeezing the bag. This modification of the Ayre’s T-piece facilitated hyperventilation, which was part of Jackson-Rees “Liverpool Technique” (see below). We used Jackson-Rees modification of the Ayre’s T-piece to create positive end-expiratory pressure while applying CPAP to the lungs of premature infants (Fig. 65.8) [37].
Like all of the Mapleson rebreathing non-absorption circuits (A to E), versions of the Ayre’s T-piece (Mapleson E, and the Jackson-Rees modification, often referred to as Mapleson F) are generally used with high gas inflows, often at least twice the patient’s minute ventilation, in order to prevent accumulation of CO2. This wastes potent inhaled anesthetic and carrier gases (air, oxygen, N2O). And, unless the gases are scavenged, they contaminate the operating room with anesthetic. The relatively recent application of end-tidal gas monitoring allows anesthetists to administer the minimum fresh gas flow needed to maintain the desired end-tidal CO2, thereby reducing some of the gas wastage.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree







