Nonoperating Room Anesthesia (NORA)
Karen J. Souter
Andrew J. Pittaway
Key Points
Related Matter
Anesthesia in Remote Locations
General Principles
The Three-Step Approach to Nora
The Patient
Table 32-1. Patient Factors Requiring Sedation or Anesthesia for Nonoperating Room Procedures | |
|---|---|
|
The Procedure
The Environment
Anesthesia Equipment and Monitors
In some NOR locations, anesthesia machines and monitors are provided; in others, it may be necessary to bring anesthesia equipment to the location. Small, portable anesthesia machines and monitors are available and recommended in these situations. Anesthesia machines and monitors that remain in a NOR location need to undergo routine maintenance. Infrequent use may result in degradation of equipment and the use of preprocedural checks, preferably with a standardized checklist, cannot be overemphasized before embarking on NORA. If more advanced monitors (e.g., an arterial line, central venous pressure, or intracranial pressure [ICP] monitoring) are required, these devices should be readily available. A preprepared cart containing essential equipment that is checked and restocked after each case is recommended.
Patient Safety in Nonoperating Room Anesthesia
Patient safety is of utmost importance in all types of anesthesia, not least NORA.
Table 32-2. Common Nonoperating Room Anesthesia Procedures | ||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Table 32-3. Asa Standards for Nonoperating Room Anesthetizing Locations1 | |
|---|---|
|
Adverse Events
Significant adverse events occur infrequently in NOR locations, although the large multicenter studies needed to determine their true incidence are lacking.2 The comparative safety of sedation administered by anesthesiology versus nonanesthesiology trained providers is not known.2 Adverse events occurring during NORA have been investigated using the ASA closed claims database.3 In this analysis, NORA was associated with a higher number of deaths compared to anesthesia conducted in the operating room and 50% of these were associated with monitored anesthesia care (MAC). Respiratory depression secondary to over-sedation was the most common type of adverse event in the closed claims study.3 This is consistent with the findings from other studies where the majority of adverse events related to sedation in NORA are due to the airway and respiratory insufficiencies.2 Capnography provides an earlier monitor of impending respiratory depression during sedation and is suggested as an important addition to pulse oximetry.4,5,6
Preprocedural Checklists
The use of checklists and pre- and postprocedural team briefings has been broadly embraced in operating room practice and emerging evidence points toward improved patient outcomes when checklists are employed.7 Similar systems should be adopted in NOR sites and recently a checklist has been proposed for use in interventional radiology suites.8
Patient Transfer
Sick, unstable patients may be transferred back and forth between the intensive care unit, the operating rooms and NOR locations for imaging or diagnostic procedures. During transport the patient should be accompanied by a member of the anesthesia team to evaluate, monitor, and support the patient’s medical condition. These patients are often mechanically ventilated and receiving a number of drug infusions for both sedation and hemodynamic support. Portable ventilators are useful for transport; these are often oxygen powered, and adequate supplies of oxygen must be available for the transfer. A manual self-inflating bag is essential in the event of ventilator failure. Infusion pumps and portable monitors should have adequate battery power for transit. The anesthesiologist should carry spare anesthetic and emergency drugs, equipment for intubation or reintubation, portable suction, and if the patient’s condition requires, a portable defibrillator. It is vital to notify the destination area that the patient is in transit; so appropriate preparations to receive the patient can be made in advance. It is also useful to send personnel ahead to secure the elevators to prevent delays during transfer.
Sedation and Anesthesia
Definition of Sedation and Anesthesia
Many NOR procedures are performed under “sedation” or “MAC”. A consistent definition of these terms is essential for clear communications between the various stakeholders involved in provision of NORA. On January 14, 2011, the Centers for Medicare and Medicaid Services (CMS) issued a revision to Interpretive Guideline (IG) for Hospitals No. 482.52 concerning anesthesia services.12 This revised guideline places the responsibility and oversight for all anesthesia services under the direction of one suitably qualified individual, the “director of anesthesia services.” IG 482.52 defines anesthesia as “the administration of a medication to produce a blunting or loss of, pain perception (analgesia); voluntary and involuntary movements; autonomic function; and memory and/or consciousness.”
The Continuum of Anesthesia
Anesthesia exists along a continuum and the transition from minimal sedation to general anesthesia is not clear-cut6,11 (Table 32-4). As sedation deepens, it is important to recognize the progressive blunting and loss of airway reflexes and patency, together with depression of spontaneous ventilation and cardiovascular function. The individual responsiveness of patients to different sedative agents varies, as do the levels of stimulation during the course of a procedure. Consequently, during the course of a NOR procedure under sedation, the patient may drift to a deeper level than the one intended, including transitioning into general anesthesia with
loss of the airway. In any circumstances where a particular level of sedation is being provided, services must be immediately available to rescue a patient from a deeper than intended level of sedation or general anesthesia.6,11,12
loss of the airway. In any circumstances where a particular level of sedation is being provided, services must be immediately available to rescue a patient from a deeper than intended level of sedation or general anesthesia.6,11,12
Table 32-4. Definition of General Anesthesia and Levels of Sedation/Analgesia6 | |||||||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
Environmental Considerations for Nonoperating Room Anesthesia
X-rays and Fluoroscopy
Hazards of Ionizing Radiation
The use of fluoroscopy for both diagnostic and interventional procedures continues to increase and with it the risks exposure of patients and staff to the effects of ionizing radiation. Radiation exposure for patients varies depending on the type of procedure as well as patient and operator-related factors.13,14 Occupational exposure for staff including anesthesiologists working in radiology suites is an important consideration. The Cardiovascular and Interventional Society of Europe (CIRSE) Standards of Practice Committee and the Society of Interventional Radiology (SIR) Safety and Health Committee have recently published guidelines on occupational protection from radiation.15 A number of terms are used to define exposure to radiation; these are summarized in Table 32-5. Exposure from fluoroscopy is between 100 and 1,000 greater than from simple X-rays. For example, exposure from a simple chest X-ray is 0.02 mSv while pulmonary angiography produces 20 to 40 mSv.16
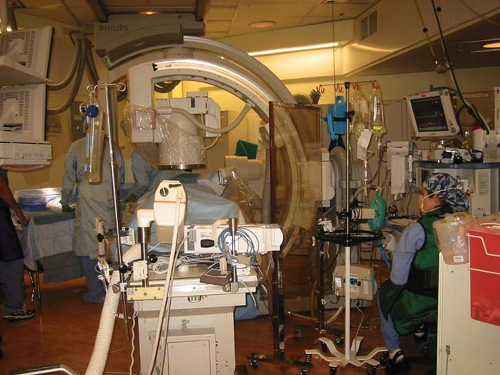 Figure 32.2. A radiology suite showing a C-arm and the high density of equipment that may separate the anesthesiologist from the patient. |
The effects of ionizing radiation on biologic tissues are classified as deterministic (dose related causing cell death and tissue damage) and stochastic (development of cancer from direct DNA ionization or the creation of hydroxyl radicals from X-ray
interactions with water molecules). Protective measures to reduce patient exposure to radiation should always be taken. Staff, including the anesthesiologists must be aware of the hazards of occupational exposure to ionizing radiation.15 Exposure to ionizing radiation may come from direct exposure and scatter. Patients are subjected to direct exposure where the beam enters the skin. Staff working in fluoroscopy suites are more at risk from scattered radiation, and as a general rule the exposure to staff is 1/1,000th the entrance skin exposure at 1 m from the fluoroscopy tube. Staff exposure to radiation can be minimized by14:
interactions with water molecules). Protective measures to reduce patient exposure to radiation should always be taken. Staff, including the anesthesiologists must be aware of the hazards of occupational exposure to ionizing radiation.15 Exposure to ionizing radiation may come from direct exposure and scatter. Patients are subjected to direct exposure where the beam enters the skin. Staff working in fluoroscopy suites are more at risk from scattered radiation, and as a general rule the exposure to staff is 1/1,000th the entrance skin exposure at 1 m from the fluoroscopy tube. Staff exposure to radiation can be minimized by14:
Table 32-5. Common Terms Used in Radiation Exposure14 | ||||||||||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
 Limiting the time of exposure to radiation.
Limiting the time of exposure to radiation.
Increasing the distance from the source of radiation. (Dose rates increase or decrease according to the inverse square of the distance from the source.)
Using protective shielding (lead-lined garments or fixed and movable shields).
Lead aprons, thyroid shields, and leaded eyeglasses are bulky and significantly increase staff fatigue. Recent studies have demonstrated that anesthesiologists are at equal risk of developing cataracts as neuroradiologists, and that the radiation may even be directed away from the neuroradiologists and toward the anesthesiologist.17 Anesthesiologists must use appropriate leaded eye protection to minimize this risk. Anesthesiology staff should use movable or fixed lead-lined glass shields so that they can gain easy access to their patients while at the same time protect themselves from radiation.
Using dosimeters.
National organizations set standards that limit the exposure of personnel to radiation doses, all personnel working in sites where there may be exposure to radiation should wear dosimeters to monitor their exposure. The International Commission on Radiological Protection (ICRP) recommends that staff must wear two dosimeters, one under the apron and one at collar level above the lead apron.18 In the United States, the National Council on Radiation Protection and Measurements (NCRP) recommends an occupational limit of 50 mSv in any 1 year and a lifetime limit of 10 mSv multiplied by the individual’s age in years.19 Anesthesiologists who are involved in NOR cases that involve exposure to ionizing radiation must wear dosimeters and be included in the institution’s radiation safety section or medical physics service regular monitoring to ensure that dose limits are not exceeded.15
Intravenous Contrast Agents
Intravenous contrast agents are commonly used in radiologic and MRI to enhance vascular imaging.20 Radiologic contrast media are iodinated compounds classified according to their osmolarity (high, low, or iso-osmolar) and their ionicity (ionic or nonionic). Nonionic contrast agents cause less discomfort on injection and have a lower incidence of adverse reactions. MRI contrast agents are also divided into ionic and nonionic compounds. They are chelated metal complexes containing gadolinium, iron, or manganese.
Adverse reactions to contrast agents may be divided into renal adverse reactions and hypersensitivity reactions.
Renal Adverse Reactions
Contrast agents are eliminated via the kidneys, and contrast-induced nephropathy (CIN) occurs with an incidence of 7% to 15%21; intra-arterial injection is associated with a higher incidence of CIN than intravenous route.20 CIN is defined as an increase in serum creatinine of 0.5 mg/dL or a 25% increase from the baseline within the first 24 hours, peaking at 5 days. It is the third leading cause of hospital-acquired acute renal failure.22 Risk factors for CIN include history of renal disease, prior renal surgery, proteinuria, diabetes mellitus, hypertension, gout, and use of nephrotoxic drugs.20 In the setting of CIN, metformin can cause lactic acidosis and should be discontinued prior to the patient receiving intravenous contrast agents. Iso-osmolar agents have the lowest risk of CIN and iodixanol has the lowest incidence of CIN in patients with renal impairment.23 Preventative measures to avoid CIN include adequate hydration, maintaining a good urine output, and using sodium bicarbonate infusions to improve elimination of the contrast agent. The efficacy of N-acetylcysteine and other agents such as fenoldopam, dopamine, calcium-channel blockers, atrial natriuretic peptide, and L-arginine in mitigating CIN has not been proven.21
Hypersensitivity Reactions
Hypersensitivity reactions to contrast media are divided into immediate (<1 hour) and nonimmediate (>1 hour) reactions.24 Mild immediate reactions occur in about 0.5% to 3% and severe reactions occur in 0.01% to 0.04%. Fatal hypersensitivity reactions may occur in about 1 per 100,000 contrast administrations.24 The frequency of nonimmediate reactions is much more variable (0.5% to 23%) related partly to difficulty in determining whether symptoms relate to contrast agents or not.24 The clinical manifestations of various hypersensitivity reactions to contrast media are outlined in Table 32-6.25 Although widely used, the effectiveness of corticosteroids and antihistamines in preventing hypersensitivity reactions to contrast agents in unselected patients is doubtful.26 Treatment of severe hypersensitivity reactions includes discontinuing the causative agent and supportive therapy; oxygen, airway securement, cardiovascular support with fluids, vasopressors, and inotropes, and if required, bronchodilators. Reactions to gadolinium-based contrast agents used for MRI are less
frequent than to iodinated contrast agents with hypersensitivity to gadolinium-containing agents occurring in 5.9 per 10,000 injections. The rate is higher (13 per 10,000) in patients undergoing abdominal MRI examinations. Severe reactions occur 1:10,000 to 1:40,000 and the mortality rate is 1 in a million injections.27 Gadolinium-containing compounds have been associated with nephrogenic systemic fibrosis (NSF) in patients with renal insufficiency.28
frequent than to iodinated contrast agents with hypersensitivity to gadolinium-containing agents occurring in 5.9 per 10,000 injections. The rate is higher (13 per 10,000) in patients undergoing abdominal MRI examinations. Severe reactions occur 1:10,000 to 1:40,000 and the mortality rate is 1 in a million injections.27 Gadolinium-containing compounds have been associated with nephrogenic systemic fibrosis (NSF) in patients with renal insufficiency.28
Table 32-6. Clinical Manifestations of Immediate and Nonimmediate Hypersensitivity Reactions to Radiocontrast Agents (Most Frequent are Underlined)25 | ||||
|---|---|---|---|---|
|
Specific Nonoperating Room Procedures
Diagnostic and Interventional Radiology
Angiography
Angiography causes minimal discomfort and may be performed under local anesthesia with or without light sedation. Patients are required to remain completely motionless during these procedures, which may be lengthy, particularly spinal angiography. Neurologic disorders such as recent subarachnoid hemorrhage, stroke, and depressed level of consciousness or raised ICP may necessitate anesthesia with formal airway protection. Angiography is usually performed via the femoral artery; the femoral vein may also be accessed when imaging arteriovenous malformations (AVMs) or dural venous abnormalities. Liberal use of local anesthetic at the puncture site precludes the need for intravenous analgesia. The injection of contrast media into the cerebral arteries may cause discomfort, burning, or pruritus around the face and eyes. Hypotension and bradycardia may also occur. During angiography and other interventional radiologic procedures, the patient is placed on a moving gantry and the radiologist positions the patient to track catheters as they pass from the groin into the vessels of interest. It is vital to have extensions on all anesthesia breathing circuits, infusion lines, and monitors to prevent these from being accidentally dislodged as the radiologist swings the X-ray table back and forth. Care should be taken with positioning of radiopaque pieces of equipment. The electrocardiogram electrodes and metallic coils in the cuffs of endotracheal tubes may cause interesting and annoying artifacts if they lie over the area being imaged.
Interventional Neuroradiology
Interventional neuroradiology is an emerging specialty viewed as a hybrid of traditional neurosurgery and neuroradiology and recently defined as the “treatment by endovascular access for the purpose of delivering therapeutic drugs and devices”.29 A variety of neurosurgical conditions especially neurovascular diseases are effectively managed by interventional neuroradiology (Table 32-2).
Cerebral aneurysms and AVMs are particularly amenable to occlusive endovascular treatments. A commonly employed technique is to insert detachable platinum coils into the abnormal vessel(s). Other occlusive agents include cyanoacrylates, “Onyx liquid embolic system” (Microtherapeutics Inc., USA) a biocompatible liquid embolic agent, and polyvinyl alcohol particles. These particles may also be used to produce temporary occlusion of blood vessels for preoperative embolization of vascular tumors such as meningiomas. A large multicenter study, the International Subarachnoid Aneurysm Trial (ISAT), recently reported a better outcome in patients with World Federation of Neurosurgical Societies (WFNS) grades 1 and 2 (good grades) presenting with anterior circulation aneurysms undergoing interventional neuroradiology compared to surgical clipping30,31,32 In poor WFNS grade cerebral aneurysms and elderly patients, the superiority of one treatment or the other has not been clearly established for these patients.33,34 Interventional neuroradiology is the standard treatment for posterior circulation aneurysms especially basilar artery tip aneurysms.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree