CHAPTER 29 Lateral cutaneous nerve of thigh block
Clinical anatomy
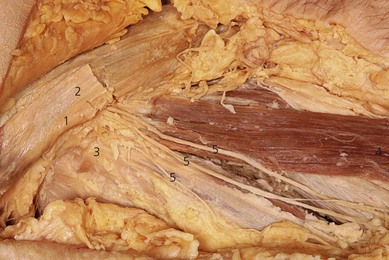
The lateral cutaneous nerve of the thigh (L2, 3) (LCNT) is a purely sensory nerve. It emerges from the psoas muscle along its lateral border. It runs deep to the iliac fascia on the iliacus muscle, emerging immediately inferior and medial to the anterior superior iliac spine. After crossing under the inguinal ligament, it passes through the origin of the sartorius muscle and travels beneath the fascia lata, before dividing into a large descending branch and a smaller posterior branch, a variable distance below the inguinal ligament (Fig. 29.1). The branches pierce the fascia lata separately. The descending branch innervates the anterolateral thigh as far as the knee; the posterior branch innervates the lateral aspect of the thigh to mid-thigh level.
Surface anatomy
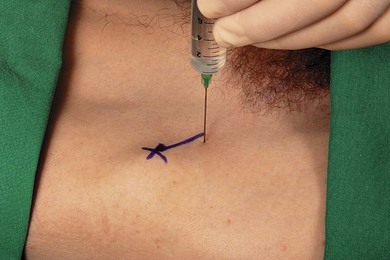
Important anatomic landmarks for block of the lateral cutaneous nerve of thigh include the anterior superior iliac spine and the inguinal ligament. The needle insertion site is located 2 cm medial and 2 cm inferior to the anterior superior iliac spine (Fig. 29.2). This should be below the inguinal ligament, unlike the needle insertion site for the ilioinguinal nerve block.
Sonoanatomy
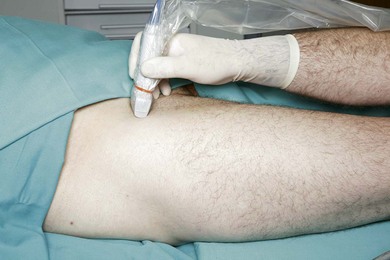
The LCNT nerve is found below the ASIS between the fascia lata and iliaca. These fascial layers are seen as hyperechoic lines. The appearance of the LCNT on ultrasound is as a round or oval hypoechoic (dark) area. Both branches of the LCNT cross the sartorius superficially. Due to the small size of the nerve and anatomical variability, a scanning routine is paramount. Scan initially with a transverse orientation in the medial thigh to identify the femoral vessels and nerve. With continued transverse scanning, move the transducer lateral and cephalad to identify the sartorius (triangular shape on transverse scan) insertion to the ASIS. Move the transducer caudally from here to the proximal third of the thigh (Fig. 29.3). The LCNT can be seen crossing the sartorius superficially or, alternatively, locate both fascial layers (fascia lata and iliaca) medial or lateral to the sartorius (Fig. 29.4). Injection of 5% dextrose between both fascial layers will help nerve visualization (Fig. 29.5). If the nerve is difficult to identify initially, a good focus point is the space between the sartorius and the more lateral tensor fascia lata. A sagittal oblique transducer orientation obtained by moving the medial aspect of the transducer to a slightly caudal position, parallel to the course of the nerve, can help identify the deep circumflex iliac artery (Fig. 29.6). This can be further identified with Doppler. This artery is crossed by the nerve, and can facilitate its identification (Fig. 29.6).
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree