87 Infectious Endocarditis
 Pathophysiology
Pathophysiology
Infectious endocarditis is a microbial infection of the endocardial surface of the heart. The process is initiated by bloodborne microorganisms that adhere directly to the endothelium or by nonbacterial thrombotic endocarditis. The most important factors facilitating nonbacterial thrombotic endocarditis are organic valvular lesions, with associated perturbation of blood flow, and prosthetic valves. Circulating microorganisms can adhere to microscopic lesions, which explains why some patients with infectious endocarditis have no previously known valvular abnormality.1
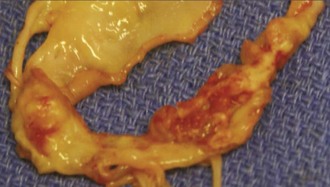
In simple infectious endocarditis, infection is limited to the valve cusps or leaflets and chordae and consists of vegetations (Figure 87-1) which are formed by pathogens, platelets, fibrin, and inflammatory cells. In advanced infectious endocarditis, deep tissue invasion results in the destruction or invasion of valvular and perivalvular structures. The infection may spread as cellulitis, with the formation of an abscess or pseudoaneurysm that can rupture to another heart chamber or even the pericardium.
In prosthetic valve endocarditis (PVE), lesions may differ according to the type of prosthesis. With biological prostheses or homografts, the infection may be limited to cusps, whereas with mechanical prostheses, involvement of the sewing ring and the valve annulus is the rule. Bacterial adherence to the prosthesis results from a complex relationship among the biomaterial, plasma proteins (e.g., fibronectin, laminin, thrombospondin, fibrinogen), and bacterial adhesion proteins. Staphylococci express numerous surface factors: clumping factors A and B, which promote their adhesion to fibrinogen and fibrin, and fibronectin-binding proteins A and B, which permit adhesion to fibronectin.2 In addition, once staphylococci have escaped the microbicidal effects of platelet peptides, they can bind to the platelet surface by a series of pathogenetic steps including direct binding to the platelet surface, up-regulation of platelet surface receptors for fibrinogen, and interaction between specific bacterial proteins and platelet surface receptors. Surface charge modifications are associated with increased in vitro resistance profiles of Staphylococcus aureus to a number of endogenous cationic antimicrobial peptides such as α-defensins.3,4
 Incidence and Classification
Incidence and Classification
The incidence of infective endocarditis ranges from one country to another within 3 to 10 episodes/100,000 person-years. This may reflect methodological differences between surveys rather than true variations.5 The overall annual incidence of infectious endocarditis in Europe and the United States is between 15 and 60 cases per million. In a study conducted in France, the crude annual incidence of infectious endocarditis was 30 (95% confidence interval [CI], 27 to 33) per million inhabitants.1 Infectious endocarditis can be classified into three groups that differ markedly in terms of incidence, clinical presentation, microbiological features, and outcome: left-sided native valve, right-sided native valve, and PVE.
Right-sided native valve infectious endocarditis is usually associated with intravenous (IV) drug use and still accounts for 10% of all infectious endocarditis episodes.6 Nosocomial cases are frequently a consequence of catheter-related infections. In most cases of pacemaker and implantable cardioverter-defibrillator infectious endocarditis, vegetations are located only on leads, but tricuspid valve involvement may also occur.7
Prosthetic valve endocarditis occurs in 1% to 6% of patients with valve prosthesis, with an incidence of 0.3% to 1.2% per patient year.4 It accounted for 21% of 2781 patients with definite infective endocarditis in the ICE Prospective Cohort Study6 (ICE-PCS). Early PVE is classically defined as occurring within 1 year of surgery, and late PVE beyond 1 year, because of significant differences between the microbiological profiles observed before (usually nosocomial origin) and after this time point (predominance of community-acquired pathogens).8 However, a recent large prospective multicenter international registry found that 37% of all PVE was associated with nosocomial infection or non-nosocomial healthcare-associated infections in outpatients with extensive healthcare contact.9
 Demographics and Etiologic Profiles
Demographics and Etiologic Profiles
Classic and Changing Patient Characteristics
The demographic characteristics of patients who develop infectious endocarditis have changed over the last few decades. Today, patients tend to be older, and their underlying diseases have changed.10,11 In ICE-PCS, 38% of all definite infectious endocarditis occurred in patients older than 65 years.11 In developing countries, rheumatic heart disease remains the most frequent underlying cardiac condition predisposing patients to infectious endocarditis. In contrast, in the United States and Western Europe, nonrheumatic heart abnormalities, including mitral valve prolapse, aortic valve calcification, aortic bicuspid valve, and hypertrophic obstructive cardiomyopathy, are the main risk factors. For patients with mitral valve prolapse, risk factors include mitral regurgitation and thickened mitral leaflet. However, results of a 1-year survey of infectious endocarditis in France showed a significantly lower incidence of known underlying heart disease between 1991 and 1999. Nowadays, congenital heart diseases are rarely involved, except bicuspid aortic valve. Other conditions including diabetes mellitus, long-term hemodialysis, and immunosuppression are associated with a higher incidence of infectious endocarditis. At Duke University Medical Center, rates of hemodialysis dependence and immunosuppression among 329 patients with infectious endocarditis rose significantly between 1993 and 1999.12 Moreover, a recent study showed that more than one third of cases of native valve endocarditis in non–injection drug users involve contact with health care. Such episodes of endocarditis maybe nosocomial if they occur in a patient hospitalized for more than 48 hours before the onset of signs or symptoms consistent with infective endocarditis. A higher proportion of non-nosocomial healthcare-associated endocarditis is now observed in patients with extensive out-of-hospital contact with healthcare interventions or systems (wound care, receipt of hemodialysis or IV chemotherapy, residence in a nursing home or long-term care facility).13
Causative Organisms
Overall Distribution
Most Frequently Isolated Pathogens
Streptococci are traditionally the most common causative agent of infectious endocarditis, but the results of the ICE-PCS show that streptococci had fallen into second place to staphylococci as the leading cause.6 However, this apparent temporal shift from predominantly streptococcal to predominantly staphylococcal infective endocarditis may be partly due to recruitment/referral bias in specialized centers, since this trend is not evident in population-based epidemiologic surveys of infective endocarditis.14 Streptococcus species (mainly Streptococcus mitis, Streptococcus sanguis, Streptococcus mutans), which abound in the mouth and nasopharynx, are associated with dental procedures and diseases. Poor dental hygiene and minor or unrecognized periodontal disease may be the source of Streptococcus viridans infectious endocarditis. Streptococcus gallolyticus (previously S. bovis) may be involved in valve infection of dental or buccal origin. In addition, the association of S. gallolyticus with carcinoma or other lesions of the colon (e.g., diverticulitis, polyps) is well known. Beta-hemolytic streptococci (groups A, B, C, and G) and Streptococcus milleri are isolated from 6% of patients with infectious endocarditis,1 with the predominant species being group B. The majority of nonpregnant patients with group B streptococcal infectious endocarditis have an underlying condition such as diabetes mellitus, breast cancer, decubitus ulcer, or cirrhosis.15
Enterococci, mainly Enterococcus faecalis and Enterococcus faecium, account for only 10% of cases of infectious endocarditis.6 These pathogens affect older patients, as demonstrated by a description of 93 episodes of enterococcal infectious endocarditis occurring in patients with a mean age of 74 years.16 The portals of entry are the gastrointestinal and urogenital tracts through a lesion or a procedure (e.g., injection sclerosis of esophageal varices, transurethral prostate resection, urethral dilatation) resulting in transient bacteremia, in which case the infection is healthcare associated.
Staphylococcus aureus is now implicated in approximately 30% of all cases of left-sided native valve infectious endocarditis,6 in 23% of PVE,9 and is the most common cause of healthcare-associated infections.15 S. aureus is also the causative agent in most acute infections, with about half of patients having no previously known heart disease. A clinically identifiable focus of infection (e.g., carbuncle, cellulitis, bursitis, ulcer, burn, osteomyelitis) may be present. However, in 50% to 60% of cases, no obvious portal of entry is detected, although the skin is probably the source in many of them. The relationship between S. aureus nasal carriage and infection has been established in specific subsets of patients, especially in IV drug users and patients with diabetes mellitus or on hemodialysis.12 Methicillin-resistant strains are isolated in healthcare-associated endocarditis, although rare cases of community-acquired methicillin-resistant endocarditis have been reported.
Coagulase-negative staphylococci (CoNS), in a recent international study, were found to cause 16% of 537 cases of definite noninjecting drug use–associated PVE. Nearly 50% of patients with CoNS PVE presented between 60 days and 365 days of valve implantation. Methicillin resistance was present in 68% of CoNS strains.17 CoNS are also a well-documented, albeit rather rare, cause of native valve infectious endocarditis. Most patients have documented valvular abnormalities, especially mitral valve prolapse. A substantial subset of CoNS infective endocarditis has been identified as being due to Staphylococcus lugdunensis, which causes destructive cardiac lesions; its differentiation from other CoNS species in the laboratory may be difficult.
Infrequent Pathogens
Enterobacteriaceae and HACEK Group. Despite the high frequency of Enterobacteriaceae bacteremia leading to severe sepsis or septic shock, infectious endocarditis caused by these pathogens is extremely uncommon, probably because gram-negative bacilli adhere less avidly to the endothelium than gram-positive cocci do. Most cases of native valve infectious endocarditis develop in patients with severe comorbidities, including cirrhosis or immunosuppression.18 Gram-negative bacilli are usually encountered in early and late PVE, but they account only for 2% of the cases. Bacteria of the HACEK group (fastidious organisms) originate from the oropharyngeal or urogenital flora and include Haemophilus aphrophilus or paraphrophilus (H), Actinobacillus actinomycetemcomitans (A), Cardiobacterium hominis (C), Eikenella corrodens (E), and Kingella species (K). These HACEK pathogens are implicated in 2% of cases of infectious endocarditis on either native or prosthetic valves.6
Streptococcus pneumoniae infectious endocarditis occurs more commonly in alcoholics, but other patients, such as those with diabetes, malignancy, or chronic obstructive pulmonary disease, may be affected. Approximately 65% to 80% of patients have no known predisposing cardiopathy. The primary infection focus is the lungs, and meningitis is present in 40% to 60% of cases.19
Fungi are a rare cause of infective endocarditis, being isolated in 2% of cases but in 4% of those patients with prosthetic valve infection. Although injection drug use was traditionally an important risk factor, a recent study showed that patients with Candida infective endocarditis were more likely to have a prosthetic valve, short-term indwelling catheters, and healthcare-associated infections.20 Other fungi such as Aspergillus spp. are even less frequently encountered. Fungi are frequently responsible for mural endocarditis.
Patients with Negative Blood Cultures
Five main points should be emphasized: (1) Abiotrophia spp. (previously classified as nutritionally variant streptococci) are the main cause of culture-negative infectious endocarditis in patients who have recently received antibiotics. (2) Only 5% to 7% of patients who have not recently taken antibiotics have negative blood cultures. Polymerase chain reaction (in blood, excised vegetation, or systemic emboli) can be used to identify the causative organism, such as Bartonella spp., Tropheryma whippelii, or Coxiella burnetii, but also streptococci or other pathogens not isolated from blood cultures.21 (3) Serologic tests are useful to diagnose infectious endocarditis caused by those organisms or by Brucella and Legionella species. (4) HACEK organisms may require prolonged incubation and subculturing. (5) Candida (but not Aspergillus) spp. are usually isolated from routine blood cultures, but in some cases, fungi are recovered only from excised vegetations or peripheral emboli.
Specific Microbiologic Characteristics of Infectious Endocarditis in ICU Patients
The microbiological characteristics of infectious endocarditis in patients who require ICU admission differ from those in the overall population. Analysis of a large series of infectious endocarditis patients hospitalized in two medical ICUs in a Parisian teaching hospital between 1994 and 2001 showed that S. aureus was the leading pathogen responsible for left-sided native valve and PVE22 (Tables 87-1 and 87-2). Those figures were confirmed by an Austrian study of 33 ICU patients with infectious endocarditis: S. aureus was isolated from 36% of them, versus 15% S. viridans and 12% enterococci.23 In a French multicenter study, S. aureus accounted for 46% of 198 critically ill patients with definite endocarditis according to Duke criteria (see later discussion).24 Clearly these findings are largely explained by S. aureus causing valve destruction, septic shock, and emboli to vital organs such as brain.
TABLE87-1 Causative Agents of Left-Sided Native Valve Infectious Endocarditis
| Microorganisms | ICE-PCE (2781 patients)6 Number (%) | Bichat-Claude Bernard ICUs (120 patients): Number* (%)22 |
|---|---|---|
| Streptococci | 810 (29) | 42 (35) |
| Staphylococcus aureus | 869 (31) | 48 (40) |
| Enterococci | 283 (10) | 4 (3) |
| CoNS | 304 (11) | 2 (1) |
| Streptococcus pneumoniae | NR | 5 (4) |
| HACEK | 44 (2) | NR |
| Fungi | 45 (2) | 4 (3) |
| Other | 121 (4) | 9 (7) |
| Negative blood cultures | 277 (10) | 10 (8) |
CoNS, coagulase-negative staphylococci; HACEK, Haemophilus aphrophilus or paraphrophilus, Actinobacillus actinomycetemcomitans, Cardiobacterium hominis, Eikenella corrodens, and Kingella species; NR, not reported.
* The number of microorganisms exceeds the number of patients because some cases were polymicrobial.
TABLE87-2 Causative Agents of Prosthetic Valve Endocarditis (PVE)
| Microorganisms | Early PVE (n = 51) Number (%) | Late PVE (n = 331) Number (%) |
|---|---|---|
| Staphylococcus aureus | 19 (37) | 61 (18) |
| Coagulase-negative staphylococci | 9 (17.5) | 66 (20) |
| Streptococcus viridans | 1 (2) | 34 (10) |
| Streptococcus bovis | 1 (2) | 22 (7) |
| Other streptococci | 0 | 11 (3) |
| Enterococci | 4 (8) | 42 (13) |
| Streptococcus pneumoniae | 0 | 3 (1) |
| Propionibacterium | 0 | 5 (1.5) |
| HACEK | 0 | 7 (2) |
| Enterobacteriaceae | 2 (4) | 3 (1) |
| Pseudomonas aeruginosa | 1 (2) | 1 (0.3) |
| Fungi | 5 (10) | 11 (3) |
| Other | 0 | 5 (1.5)* |
| Culture negative | 9 (17.5) | 41 (12) |
HACEK, Haemophilus aphrophilus or H. paraphrophilus, Actinobacillus actinomycetemcomitans, Cardiobacterium hominis, Eikenella corrodens, and Kingella species.
* Other: Listeria monocytogenes, 2; Micromonas, 2; Mycobacterium spp., 1.
Adapted from Wang A, Athan E, Pappas PA, et al. Contemporary clinical profile and outcome of prosthetic valve endocarditis. JAMA 2007;297:1354-61.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree