Cheng Ong This chapter will describe: • why all patients require a preoperative assessment of the airway • how assessment determines the airway management strategy of the anaesthetist • the importance of predicting difficulty with intubation or ventilation • important predictive factors: a history of problems in previous anaesthetics, a disease process affecting the head, neck or mediastinum, signs or symptoms of difficulty with breathing, limitation in mouth opening or in head and neck mobility • a structured approach involving taking a history, looking at the patient and doing a few tests • how linking findings at preoperative evaluation to clinical practice in an individual patient requires professional judgement. Failure to adequately protect and maintain the airway throughout anaesthesia leads rapidly to impaired oxygenation and ventilation or complications of aspiration. The airway is managed during anaesthesia by either the facemask, supraglottic airway such as the laryngeal mask or tracheal intubation and these ‘devices’ offer differing levels of protection and maintenance of the airway. Tracheal intubation offers the highest level of airway protection and maintenance and plays a central role in both planned and emergency airway management. An assessment of the airway should be made in all patients. Figure 7.1 Anatomy of the airway The airway consists of the passage air takes as it is conducted between the external atmosphere and alveolus (Figure 7.1). Air is drawn in initially through the nose or mouth with the nose being used at rest or with light activity. The nasal cavity is lined with highly vascular mucous membrane and leads to the nasopharynx. The oral cavity is bounded anteriorly by the jaw and teeth, inferiorly by the tongue and superiorly by the hard or soft palate. The pharynx is bounded posteriorly by the pharyngeal wall overlying the cervical vertebrae and leads to the laryngeal inlet and upper oesophagus. The epiglottis is a ‘flap’ which protects the laryngeal inlet from ingress of food into the respiratory tract. The larynx is a highly complex structure involving the hyoid bone, thyroid and cricoid cartilages, numerous small muscles, ligaments and the vocal cords. The vocal cords are the instruments of speech and also guard access to the trachea. The trachea begins at the lower border of the cricoid cartilage and comprises 12–20 C-shaped cartilages. Half the length of the trachea is superficial within the neck, before it passes behind the sternum to divide into the main bronchi. The bronchial tree continues to divide into increasingly narrower passages to the alveolus, which is the functional unit where gas exchange takes place. The anaesthetist is able to place devices (Figure 7.2) into the airway to maintain patency, but only to the level of the main bronchus. Oral or nasal airways will bypass the oral or nasal cavities, the laryngeal mask will guide external air directly to the larynx and tracheal intubation provides a secure tube to the mid or lower trachea. From the brief anatomical description it can be seen that abnormalities (particularly swelling) of the lips, jaw, tongue, palate, epiglottis or vocal cords will lead to airway narrowing. The course and diameter of the trachea will be affected by masses in the neck (particularly thyroid enlargement) or in the mediastinum. Figure 7.2 Airway devices for use during surgery Humans are unfortunate that their pharynx is a floppy-walled, common meeting place for anything taken in through the mouth or nose. Highly sophisticated reflexes are required to make certain that patency of the pharynx is maintained and that the contents are forwarded correctly with air to the larynx and fluid or food to the oesophagus. Anaesthesia abolishes many of these protective reflexes. In particular, in the anaesthetised supine adult, patency of the airway is abolished through the tongue and soft palate falling back to meet the posterior pharyngeal wall. Anaesthesia abolishes the protective laryngeal reflexes which guard against passage of fluid or food particles into the trachea. A particularly dangerous situation is reflux of gastro-oesophageal contents from the stomach into the pharynx and then into the lungs. Bi-directional flow of air through the airway is normally under the control of the respiratory centre which senses blood levels of oxygen and carbon dioxide and controls the muscles of respiration. Inspiration is caused by contraction of the diaphragm and intercostal muscles, which act to increase the volume of the thoracic cage generating a negative pressure in the pleural space and alveoli. Air is drawn down the airway until the end of inspiration when relaxation of the diaphragm and intercostals reverses the gas flow in the expiratory phase. Normal negative pressures produced during inspiration are no more than -5 cm H2O but if the airway is narrowed much greater negative pressures are required. In acute airway obstruction, respiratory muscles generate much higher negative inspiratory pressures but tire quickly. If airway obstruction develops over several weeks, the inspiratory muscles become trained and the air passage may be no more than 4–5mm wide at its narrowest point before the patient is short of breath at rest. In normal respiration, the volume of each breath (tidal volume) in the average adult is about 500ml and the respiratory rate is normally 10–12 per minute. This gives a minute ventilation of 5–6 litres. The inspiratory gas may be air (21% oxygen) or may be controlled by the breathing circuit and gas flows to any value of inspired oxygen from 21% to 100%. The minute ventilation of 5 litres/minute replenishes the gas in the alveolus. Oxygen is being removed from the alveolus by the pulmonary blood flow and carbon dioxide delivered to it. Normal values of oxygen consumption are 250ml/min with 200ml/min of carbon dioxide being excreted during expiration. The volume of the lung at the end of a expiration (functional residual capacity, FRC) is approximately 2–2.5 litres and this provides a store of oxygen. With sudden occlusion of the airway, when breathing air, this reserve will last no more than 1–2 minutes before the patient becomes critically hypoxaemic. After breathing 100% oxygen the reserve extends the safety time to about 8–10 minutes. Gas flow in a tube may be either laminar or turbulent and the size of the tube is an important determinant of flow. Laminar flow is more energy efficient and the factors which affect it are the pressure difference between the two ends, the length of the tube, the viscosity of the gas and the radius of the tube. The Poiseuille equation states that for laminar flow in a tube: It can be seen that flow is proportional to the fourth power of the radius, which indicates the very great contribution that calibre and patency makes to gas flow in the airway. As the airway narrows, gas flow becomes turbulent and noisy. The first comprehensive practice guidelines for management of the airway were published in 1993 by the American Society of Anesthesiologists. It proposed a sequential five-step plan of evaluation of the airway, preparation for difficulty, airway management plan at the start and end of anaesthesia and follow-up of the patient. Evaluation of the airway is the first of these vital steps and must be part of the preoperative assessment in all patients. The purpose of airway evaluation is to: • decide which device will be most suitable for airway management • judge whether there are likely to be problems with airway management • explain the airway management plan in the explanation/consent process • warn the patient of common or serious complications Around the time of induction of general anaesthesia a facemask is used to preoxygenate the patient. Preoxygenation means applying a close fitting facemask to the patient whilst they are still awake and supplying 100% oxygen in the breathing circuit for a few minutes. The air in the lungs is replaced by oxygen and this provides a safety reservoir. Immediately after induction of anaesthesia the patient is ventilated initially by facemask. The factors which determine the manner in which the airway is subsequently managed are: • risk of aspiration of gastric contents • length of procedure • requirement for intermittent positive pressure ventilation (IPPV) • body mass index • risk to the airway from proposed surgery • ease of intubation during surgery should this be needed • position of the patient. Continued use of the facemask is possible for short elective procedures when there is no risk of gastric aspiration and no requirement for IPPV. One hand of the anaesthetist constantly holds the facemask in place and this makes it difficult to complete the anaesthetic record chart or respond to perioperative events. The airway is most commonly (in the UK) managed by laryngeal mask, in approximately 70% of operations. This is because the risk of aspiration in elective surgery is low, surgery usually lasts less than 2 hours, the body mass index (BMI) is < 35, the airway will not be compromised by surgery, the anaesthetist at the head of the patient may easily intubate during surgery if the need arises and the patient is supine. Tracheal intubation is generally required for: • patients at risk of aspiration of gastric contents – preoperative food < 6hr or fluid < 2hr before surgery – delayed gastric emptying (including pregnancy > 16 weeks) – gastro-oesophageal reflux – acute abdomen • surgery > 2–3 hours • obesity • head down or prone position • prolonged IPPV • head and neck surgery • disease process affecting the airway. Difficult facemask ventilation can be defined as the inability to maintain the oxygen saturations above 90% with 100% oxygen or reverse signs of inadequate ventilation. It is rare in patients presenting for ‘general’ surgery. In a recent study of 22,260 patients, using a four-point scale of difficult facemask ventilation (Table 7.1), the following factors were associated with difficult facemask ventilation: • body mass index (BMI) > or = 30kg m-2 • presence of a beard • Mallampati class 3 or 4 • age > or = 57 years • jaw protrusion – severely limited history of snoring. Table 7.1 Grades of difficult facemask ventilation (from Han et al.1)
Chapter 7 Assessment of the airway
Adrian Pearce
SUMMARY
INTRODUCTION
Basic Science
Anatomy
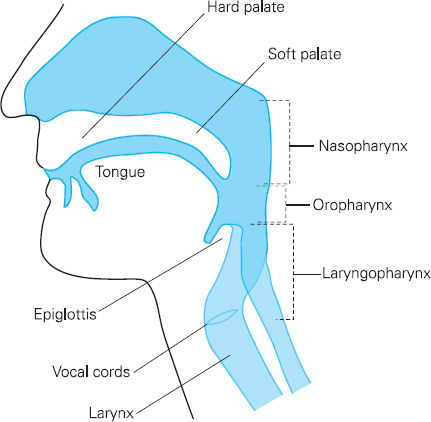

Physiology
Physics
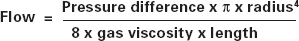
Clinical practice
Which airway device will be suitable?
Preoperative assessment and Individual devices
Difficult facemask
| Grade | Description | Percentage of patients |
| 1 | Ventilated by mask | 77 |
| 2 | Ventilated by mask with oral airway/adjuvant with or without muscle relaxant | 21 |
| 3 | Difficult ventilation (inadequate, unstable, or requiring two providers) with or without muscle relaxant | 1.4 |
| 4 | Unable to mask ventilate with or without muscle relaxant | 0.16 |
There are a number of severe or obvious clinical features which would suggest that the airway should be secured before induction of general anaesthesia:
• stridor (noisy breathing)
• difficulty with breathing
• severe limitation of head and neck movements
• large oropharyngeal masses or laryngo-pharyngeal disease
• grossly irregular contour of the face/jaw precluding application of the facemask.
Difficult laryngeal mask
The laryngeal mask is not designed for use in patients with a significant likelihood of gastric aspiration or those with laryngeal pathology. The seal it provides allows ventilation to a pressure of (only) 20cm H2O which will be inadequate for patients with poor lung function or obesity. It may be difficult to insert (by the standard Brain insertion technique) in those with mouth opening < 2cm, those with large oropharyngeal masses or those with a high arched palate.
Difficult tracheal intubation
Most of the extensive literature on preoperative airway assessment is on prediction of difficult intubation. Intubation is most commonly performed by direct laryngoscopy, in which a laryngoscope is placed in the mouth and direct line-of-sight to the larynx obtained. Abnormalities of the jaw or teeth, tongue, palate, pharynx, epiglottis or larynx may cause difficulty with intubation.
Common research definitions of difficult intubation are:
• More than three attempts at laryngoscopy are required.
• It takes longer than 10 minutes to complete intubation.
• There is a poor view of the larynx – the epiglottis only or no view at all.
• Intubation can be achieved only by specialised equipment, such as a flexible fibrescope.
Prediction of difficult airway management
If difficulty with airway management is predicted preoperatively the anaesthetic team has time to consider various options and discuss these with the patient. The options are to prepare special equipment or organise more senior help, undertake intubation in the conscious sedated patient before induction of general anaesthesia, undertake the proposed surgery under local or regional anaesthesia or re-consider the need for surgery.
Prediction of the difficult airway is by:
• history
• clinical examination
• specific bedside ‘predictive’ tests
• special investigations.
History
The following information should be obtained from the patient and recorded:
• Previous difficult airway management during anaesthesia
• Current disease process if it affects the head, neck or mediastinum
• Any past disease, surgery or radiotherapy to the head, neck or mediastinum
• Medical diseases with some association with difficult airway management
• Difficult or noisy breathing (including snoring)
• Delayed gastric emptying or oesophageal reflux.
It is particularly important to pick up a previous problem with airway management since this is one of the most predictive factors. This may alter the scheduling of the patient and the anaesthetic department should be informed so that a consultant anaesthetist can be involved. Current diseases, such as a dental abscess, enlarged thyroid, tonsillar abscess, epiglottitis or oedema of the tongue or floor of the mouth, are relevant. Any past or current disease process which narrows or distorts the airway, limits head extension, limits mouth opening or causes difficulty with breathing is highly significant. A number of medical diseases such as rheumatoid arthritis, acromegaly and obstructive sleep apnoea have some association with difficult airway management. Rheumatoid arthritis causes limited mobility of neck movements, impaired mouth opening and jaw protrusion and may narrow the laryngeal inlet.
Table 7.2 Features of a history of previous difficult airway management
| Patient knows of previous problems |
| Patient has written record of previous problems |
| Anaesthetic notes describe difficulty |
| After previous anaesthetics: |
• Front teeth displaced/chipped • Severe bruising of lips/pharynx • Unexpected admission to ICU with tear in the pharynx or larynx |
| MedicAlert bracelet indicating ‘Difficult Airway’ or ‘Difficult Intubation’ |
Clinical examination
The patient is examined for the anatomical and pathological features listed in Table 7.3. Some of these features will be obvious on external examination (swellings, scars, receding jaw, large tongue) and others will require testing (mouth opening and movement of the head/neck). The practitioner gains an impression of whether the patient ‘looks’ as though airway management will be difficult. Clinical examination will also detect any noisy or laboured breathing and these are particularly important since they usually indicate narrowing or obstruction of the airway.
Table 7.3 Predictive factors on general examination
| Features that suggest presence of a difficult airway |
| Anatomical features: |
| Obesity |
| Thick short neck |
| Arthritis of neck and spine – restricting flexibility or causing deformity |
| Receding or small mandible |
| Beard (this may be hiding a small lower jaw) |
| Limited mouth opening |
| Prominent ‘overbite’ or ‘buck teeth’ (maxillary incisors anterior to mandibular incisors) |
| Dental caps, crowns and bridges on upper front teeth |
| Lack of any teeth (full dentures should accompany patient to theatre) |
| Large and rigid hairstyles, hair extensions and wigs (especially at back of head; ponytails should not be worn) |
| Pathological features: |
| Scars and radiation changes over neck and face |
| Swellings on the face, neck and inside mouth |
| Presence of bleeding or secretions from the mouth or nose |
| Noisy breathing – hoarse voice, stridor, blocked nasal passages |
Specific ‘bedside’ predictive tests
A number of tests have been suggested to improve the prediction of difficult airway management. The common ones used at the bedside during preoperative evaluation are described in Table 7.4. Where distances are measured, one common unit is the finger breadth (fb) equivalent to 1.5–2cm. The test most commonly used in preoperative assessment schemes is the Mallampati classification. Mallampati suggested that the oropharyngeal space was one determinant of difficult intubation and the test is done in the seated patient, asking them to open their mouth widely, protrude the tongue and the examiner scores the visibility of the posterior pharyngeal wall structures and fauces. Mallampati only described three classes (see Figure 7.3) in which Class 1 (the best) described a view of the whole uvula, fauces and posterior pharyngeal wall, Class 2 incomplete view of the fauces and uvula but some view of the posterior pharyngeal wall and Class 3 (the worst) the tongue against the palate with no view of the posterior pharyngeal wall. Later authors added Class 4, where the tongue lies against the hard palate, and Class 3 which indicates the tongue against the soft palate. There is great inter-observer variation in performing the test and whilst it is often performed it is not very predictive. It does, at least, force the practitioner to examine mouth opening.
Table 7.4 Commonly performed bedside predictive tests
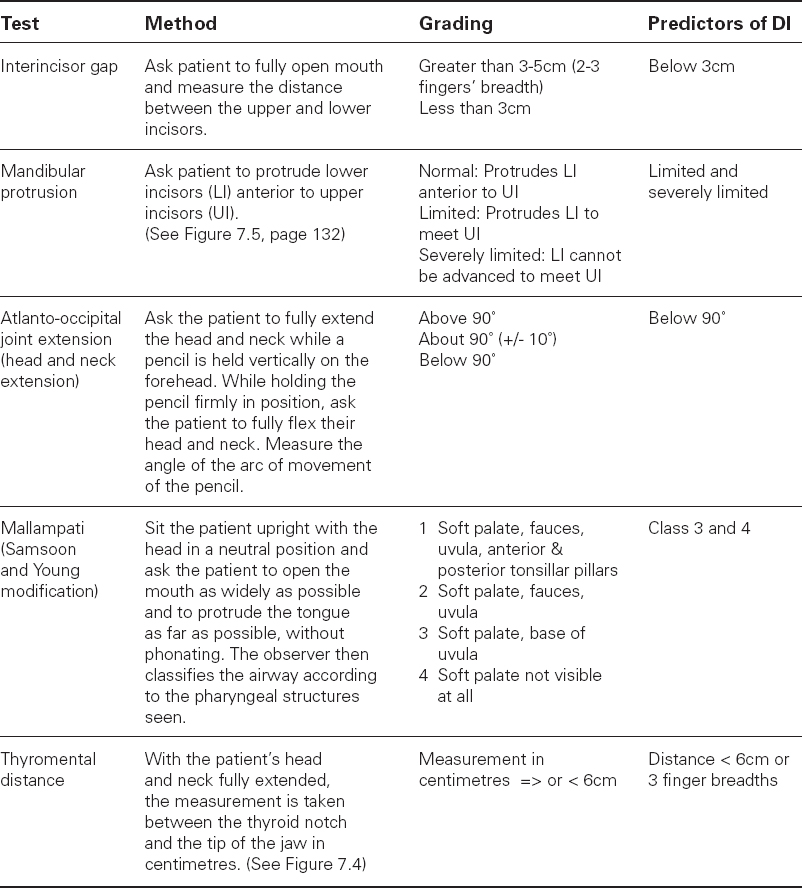
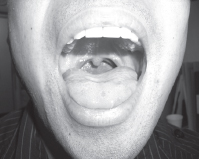
Figure 7.3a Mallampati 1
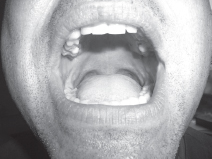
Figure 7.3b Mallampati 2
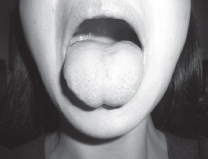
Figure 7.3c Mallampati 3
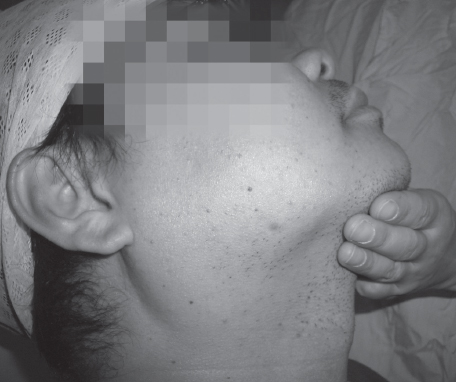
Figure 7.4 Thyromental distance or Patil test. The distance between the chin and thyroid notch measured in finger breadths with the neck fully extended. Less than 3fb or 6cm is the discriminant value.
Special investigations
The following investigations are used when the disease process impinges on the airway, to provide more information. The results are particularly helpful to the anaesthetist in planning airway management.
• Chest or thoracic inlet X-ray.
• CT or MR scan from base of skull to carina.
• Flow-volume loops (respiratory function test).
• Flexible naso-endoscopy to view the supraglottis and larynx.
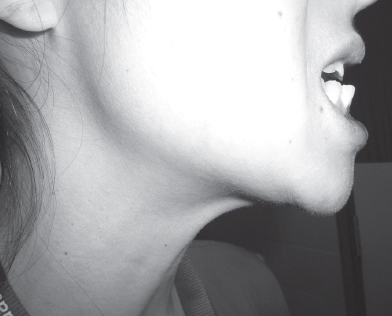
Figure 7.5 Mandibular protrusion, or the ability to protrude the lower teeth beyond the top teeth. Here there is good or normal protrusion.
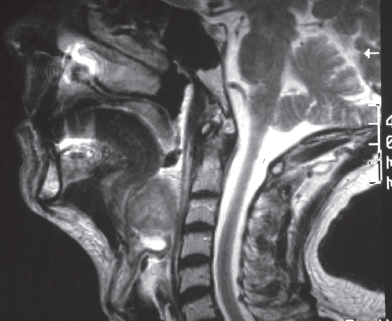
Figure 7.6 An MRI scan showing a large tumour at the base of the tongue. This would make normal intubation very difficult and the patient was managed by a nasal fibreoptic intubation under sedation.
How predictive are bedside tests?
The broad answer is not very predictive. The predictive ability of a test can be understood only by mentioning a few terms. The term ‘difficult patient’ is used to indicate a patient with a difficult airway and to help description the Mallampati test will be used. Mallampati Class 3 or 4 would be test results indicating difficult intubation and Mallampati Class 1 or 2 would indicate a ‘normal’ (easy intubation) patient.
Sensitivity
Sensitivity is the ability of a test to exclude false positives or, put another way, label a difficult patient as difficult. It is the proportion of ‘difficult’ patients who are correctly identified. A test is 100% sensitive if it identifies all the ‘difficult’ patients.
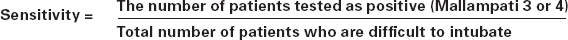
Specificity
Specificity is the ability of a test to exclude false negatives or, put another way, to label a normal patient as normal. It is the proportion of ‘easy’ patients who are correctly identified. A test is 100% specific if all normal patients are identified as normal/easy.
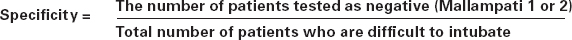
Positive predictive value (PPV)
The PPV is the percentage of all patients found to be difficult out of all those predicted to be difficult by the test.
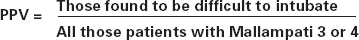
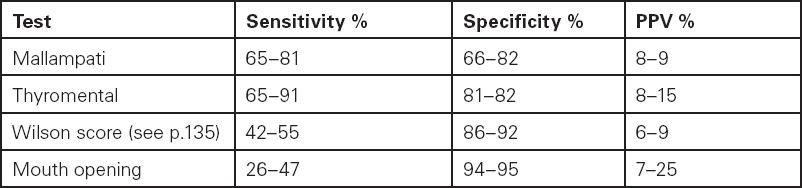
The prevalence of difficult intubation in ‘general surgical’ patients is no more than 1–4% and the predictive tests do not have a high enough specificity to label all normal patients as normal. The sensitivity, specificity and PPV of various tests are given in Table 7.5. A PPV of 8% means that only 8% of the patients with Mallampati Class 3/4 will be found to be difficult to intubate and such a test is of little clinical use.
Table 7.5 Sensitivity, specificity and positive predictive value
It must be recognised that prediction of difficult intubation is not particularly accurate and patients predicted to be easy may prove difficult and those predicted to be difficult may prove to be easy intubations. Good practice requires the anaesthetist to have an airway strategy which deals with unanticipated difficult intubation and/or ventilation.
What to do if difficulty is predicted
It is easy to predict difficult intubation when there are gross abnormalities such as limited mouth opening, limited neck extension, previous difficult intubation, anatomical narrowing or distortion of the airway, small mouth, receding jaw, large tongue or previous head and neck resective surgery. Figure 7.7 shows a patient presenting for surgery with a receding jaw, limited mouth opening (Figure 7.8) and poor jaw protrusion who had a previous record of difficult intubation.
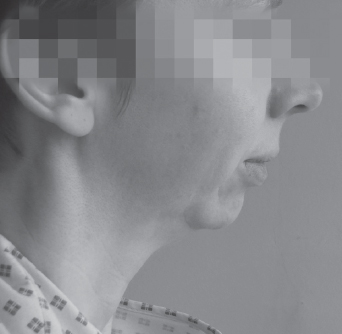
Figure 7.7 Patient with a receding jaw

Figure 7.8 Limited mouth opening (about 1fb)
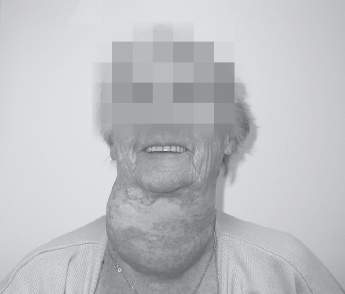
Figure 7.9 A grossly enlarged thyroid mass
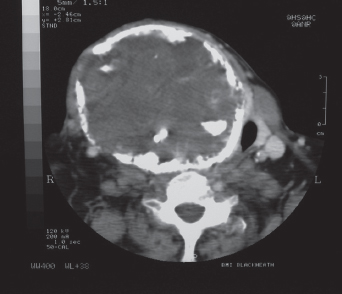
Figure 7.10 Gross deviation of the trachea from the midline
The preoperative assessment nurse contacted directly the anaesthetist scheduled for the list and the airway was managed successfully by awake fibreoptic intubation. Figure 7.9 shows a patient with a very large thyroid mass which, from the CT scan (Figure 7.10), has caused substantial deviation and narrowing of the airway. These are examples of severe problems for which the anaesthetist should be pre-warned so that they can prepare special equipment or get more senior help. Generally it is wise to contact the anaesthetic department directly and speak to the relevant anaesthetist.
Table 7.6 Wilson risk-sum score
Weight
| <90kg | 0 |
| 90-110kg | 1 |
| >110kg | 2 |
Head and neck movement
| > 90 degrees | 0 |
| ˜ 90 degrees | 1 |
| < 90 degrees | 2 |
Jaw movement, jaw protrusion
| Incisor gap > 5cm, Normal | 0 |
| Incisor gap < 5cm, Limited | 1 |
| Incisor gap < 5cm, Minimal | 2 |
Receding mandible
| Normal | 0 |
| Moderate | 1 |
| Severe | 2 |
Buck teeth
| Normals | 0 |
| Moderate | 1 |
| Severe | 2 |
However, most patients seen preoperatively look quite normal and do not have airway narrowing. It is in these ‘apparently normal’ patients that the specific predictive tests are used and the results are poor. Abnormalities in several tests are more predictive than individual tests and some scoring systems incorporate up to 10 factors. One of the most well-known (but rarely used) scoring systems in the UK is the Wilson risk-sum score (Table 7.6) when a score > 2 is the discriminant value. Others used are by Arné2 (Table 7.7) with a best-predictive score of 11 and El-Ganzouri.3 It is worth noting that the combination of limited mouth opening and severely limited protrusion of the lower jaw usually scores highly. In patients with some findings which might indicate difficulty with airway management it is reasonable to record the findings on the preoperative assessment chart. The anaesthetist can make his or her own judgement when the patient is admitted. An illustrative flow-chart is given in Figure 7.11 (see page 138).
Table 7.7 Arné risk index
| Factor | Scoring | Points |
| History of difficult intubation | Yes | 10 |
| Pathologies associated with DI | Yes | 5 |
| Clinical symptoms | Yes | 3 |
| Thyromental distance | < 6.5cm | 4 |
| Head/neck movement | 80–100 | 2 |
| < 80 | 5 | |
| Mallampati | Class 2 | 2 |
| Class 3 | 6 | |
| Class 4 | 8 | |
| Mouth opening, jaw protrusion | 3.5–5.0cm, Limited | 3 |
| < 3.5cm, Minimal | 13 |
Patient explanation and consent
At preoperative assessment it is usual to provide an explanation, tailored to an individual, of the plans for airway management. Preoxygenation is undertaken in most patients and is performed by ‘clear plastic facemask, which allows you to breathe oxygen so that your lungs are filled with oxygen before starting the anaesthetic’. Intubation is commonly described as ‘placing a breathing tube in your windpipe so that your breathing is protected whilst you are asleep’. There is no UK requirement currently for written consent for anaesthesia but the national consent form does specify that the patient will have the opportunity to talk to the anaesthetist. The Association of Anaesthetists of Great Britain and Ireland (www.aagbi.org) recommends that it is not appropriate to gain consent for each specific aspect of management, such as tracheal intubation.
Patients should be warned of common or serious complications:
Teeth
The patient should be asked to detail any false, loose, capped or crowned teeth and these should be recorded on a chart. Of particular importance are the upper and lower incisors, which will bear the brunt of the biting force on an oral airway or laryngeal mask, or may be damaged during intubation. The damage may be chipping or gross displacement. It is good practice to warn the patient that loose or capped teeth are at risk and that the anaesthetist will take steps to minimise the chance of this happening. Intraoperative strategies involve placing a posterior bite-block, using nasal rather than oral tubes or airways, avoiding intubation if possible and intubation by flexible fibrescope rather than direct laryngoscopy. The most common problem reported by anaesthetists to Medical Defence organisations is dental damage.
Sore throat
Both the laryngeal mask and tracheal intubation are associated with a sore throat which usually responds to simple analgesia such as paracetamol and improves within 24 hours. The complication is common enough to be mentioned in preoperative assessment. The incidence of sore throat is about 5.8 to 34% with the laryngeal mask and 14.4 to 50% with tracheal intubation.
Voice change
Tracheal intubation may cause some degree of short-term voice change, such as huskiness. This is assumed to be due to vocal cord dysfunction secondary to the presence of a tracheal tube. Most anaesthetists would avoid intubation in a professional singer although long-term complications from perioperative intubation are exceedingly rare. Any alteration in timbre or strength of voice should have recovered in 48 hours. Prolonged alteration needs to be investigated.
CONCLUSION
Complications of difficult airway management are serious and include brain damage and death due to hypoxia. Preoperative airway assessment is the first essential step in airway management. It starts the process of planning, allows discussion with the patient of options and common complications and allows a judgement to be made as to whether there will be any problems with airway management. These judgements are easy to make if there are obvious or severe problems in the history or clinical examination. Even in patients who do not look difficult to intubate and have no history of previous problems, the practitioner must always check for adequate mouth opening and neck mobility. The seriousness of difficult airway management has led to the description of many ‘predictive’ tests but the rarity of the condition renders these tests poorly predictive.
Figure 7.11 Guide for airway assessment
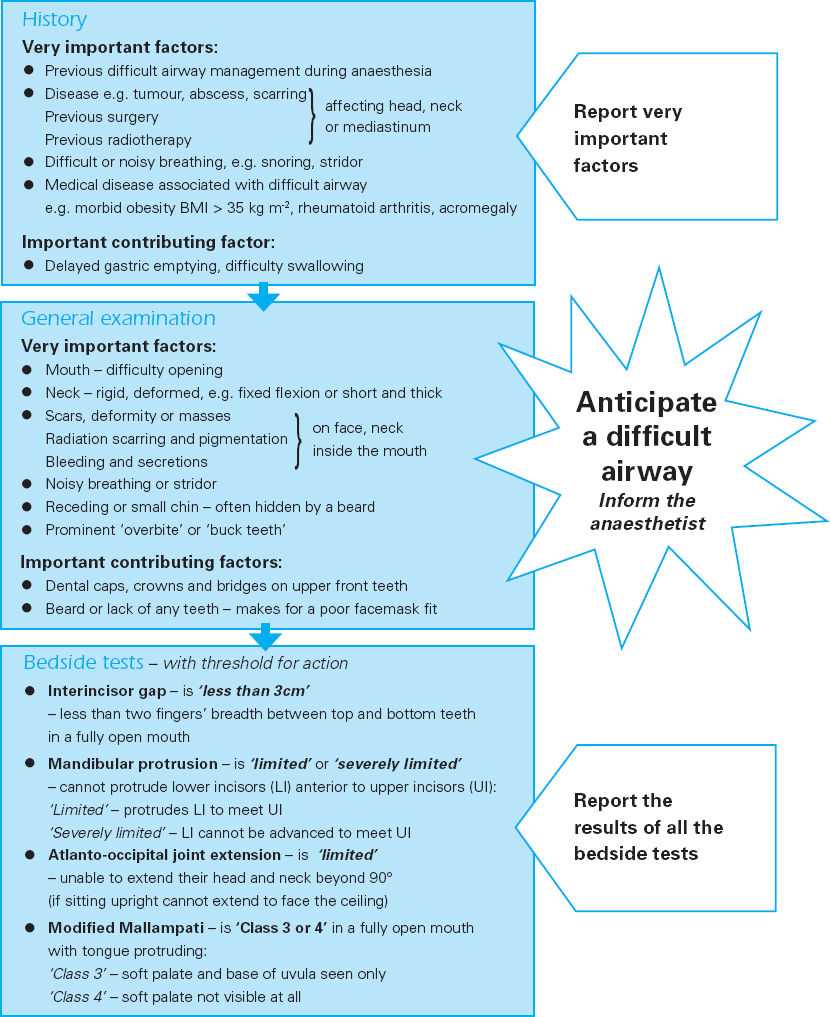
The tests, though, are commonly found in preoperative assessment schemes. Ultimately, the anaesthetist must make a judgement as to whether the factors picked up in preoperative assessment should change their normal airway management plans. This judgement remains one made commonly through experience rather than scientific tests.
REFERENCES
1. R. Han, K.K. Tremper, S. Kheterpal et al. (2004). Grading scale for mask ventilation. Anaesthesiology 101: 267.
2. J. Arné, P. Descoins, J. Fusciardi et al. (1998). Preoperative assessment for difficult intubation in general and ENT surgery: Predictive value of a clinical multivariate risk index. British Journal of Anaesthesia 80: 140–6.
3. A.R. El-Ganzouri, R.J. McCarthy, K.J. Tuman et al. (1996). Preoperative airway assessment: Predictive value of a multivariate risk index. Anesthesia and Analgesia 82: 1197–204.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






