Antiseizure Medications Used for Neuropathic Pain
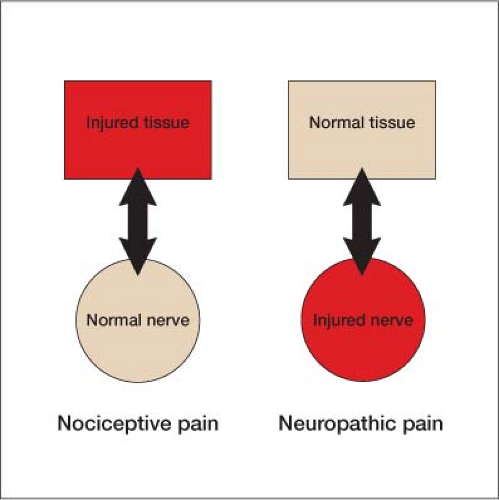
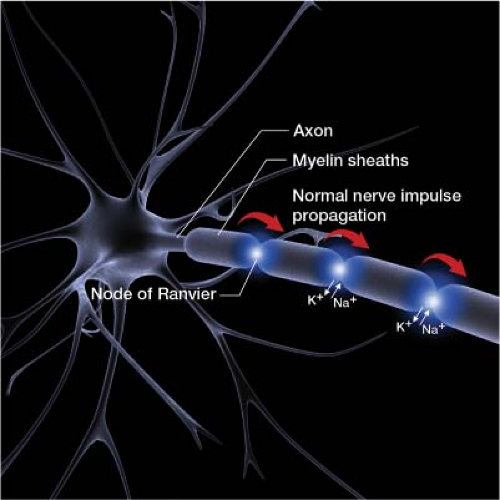
Neuropathic pain is a painful sensation from damaged nerves rather than damaged tissue (Fig. 14-1). A stimulus with sufficient strength triggers the start of a neurotransmission. On a grand scale the impulses travel along the neural pathways from a small peripheral nerve, to a larger more centralized nerve, to the spinal cord, and then up to the brain for interpretation. At a local level a stimulus above the minimal threshold triggers the dendrites of a nerve to internalize the signal, propagate that action potential, in a well-controlled manner, along its axon as sodium rushes in and potassium rushes out at the nodes of Ranvier. Finally the nerve via a calcium controlled–channel system releases neurotransmitters across the synaptic cleft at the axon terminal to pass the impulse on to the next nerve (Fig. 14-2). With damaged nerves, ectopic neuronal pacemakers can form at various sites along the length of the nerve. In addition, there is an increased response
to stimuli that would not normally be painful (Fig. 14-3). This aberrant firing pattern of damaged nerves is transmitted to the brain and interpreted as neuropathic pain.
to stimuli that would not normally be painful (Fig. 14-3). This aberrant firing pattern of damaged nerves is transmitted to the brain and interpreted as neuropathic pain.
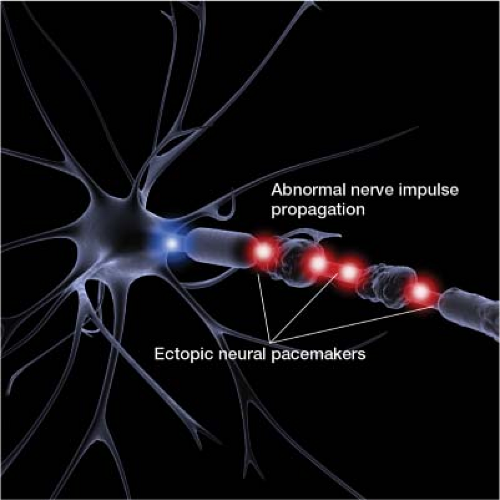 Figure 14-3 Ectopic neuronal pacemakers forming at various sites along the length of an injured nerve. |
For years, physicians have been trying to control aberrant nerve firing that originates in the central nervous system (CNS) with antiepileptic (antiseizure) drugs. In seizure patients, the build-up of electrical charge from pathologic nerve firing provokes seizures. Most antiepileptic drugs work by desensitizing and decreasing the kindling of electrical charge produced by aberrant nerve firing. Although most of the antiepileptic medications function poorly in the peripheral nervous system, a few are effective. They help control pathologic nerve firing peripherally.
In clinical practice, three antiseizure medications are primarily used for neuropathic pain: Gabapentin (Neurontin), pregabalin (Lyrica), and carbamazepine (Tegretol). Ironically, gabapentin does not affect the neurotransmitter γ-aminobutyric acid (GABA). The drug received its name before its method of action was fully understood; developed to mimic GABA, gabapentin never did. Instead, it works by blocking the α2/δ-calcium channel. When calcium enters a neuron through a voltage-gated calcium channel, the release of neurotransmitters into the synaptic cleft results, triggering an action potential. Experts think that blocking the calcium-dependent release of the neurotransmitters glutamate and substance P, reducing pathologic action potentials.
Lyrica is the newer form of gabapentin and also blocks the α2/δ-calcium channel (Fig. 14-4). Lyrica has a higher affinity to hyperexcited neurons, selectively targeting aberrant nerve firing. Some experts believe it works faster. It is unclear if Lyrica has a clinical advantage over gabapentin, because the two drugs have not been vigorously compared in clinical trials. Gabapentin is also available as a time-release formula called Gralise.
Carbamazepine stabilizes neurons by blocking sodium channels, which decreases the likelihood of an
action potential (Fig. 14-5). An increased density of abnormal sodium channels occurs in damaged nerves. The sodium channels in damaged nerves differ pharmacologically and demonstrate different depolarization characteristics compared with ones in healthy nerves.1 Tegretol is generally reserved for neuropathies of the facial region such as trigeminal neuralgia.
action potential (Fig. 14-5). An increased density of abnormal sodium channels occurs in damaged nerves. The sodium channels in damaged nerves differ pharmacologically and demonstrate different depolarization characteristics compared with ones in healthy nerves.1 Tegretol is generally reserved for neuropathies of the facial region such as trigeminal neuralgia.
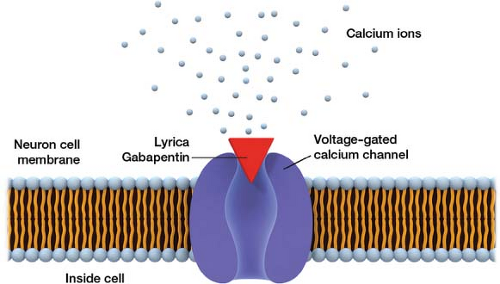 Figure 14-4 Gabapentin’s and Lyrica’s method of action as calcium channel blockers.
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|