Chapter 90 Therapeutic plasma exchange and intravenous immunoglobulin immunomodulatory therapy
Bloodletting to remove ‘evil humours’ has a long history of over 2000 years. Although not based on logic in the past, the removal of ‘noxious’ agents from the blood remains the rationale, but now there is scientific understanding of the pathophysiology of the diseases treated by plasma exchange.1 Exchange transfusions revolutionised the management of haemolytic disease in the newborn, and paved the way for therapeutic plasmapheresis and plasma exchange – the removal of plasma, with replacement by albumin-electrolyte solutions or fresh frozen plasma.
RATIONALE FOR PLASMA EXCHANGE
Theoretically, plasma exchange should be effective to treat any disorder in which there is a pathogenic circulating factor responsible for the disease. However, this premise is probably too simplistic, and other mechanisms may contribute to its beneficial effects (Table 90.1). It is a non-specific procedure, which brings about numerous, potentially undesirable, alterations in the plasma’s milieu interieur.
Table 90.1 Rationale for plasma exchange
| Removal of circulating toxic factor antibodies |
| Monoclonal antibodies |
| Autoantibodies |
| Alloantibodies, immune complexes, chemicals, drugs |
| Depletion of the mediators of inflammation |
| Replacement of deficient plasma factor(s) |
| Potentiation of drug action |
| Enhanced reticuloendothelial function |
| Altered immunoregulation |
| Potentiating effects of plasma exchange on other modes of therapy |
PATHOPHYSIOLOGY OF AUTOIMMUNE DISEASE
In general, autoimmune disease can be an acute, self-limiting (‘one hit’) disorder, intermittent or a chronic perpetuating disorder. Acute autoimmune disease may have an identifiable trigger, such as an infection, followed by a 10-day to 3-week gap until the pathogenic humoral or cellular factors appear in the circulating blood. At this point, end-organ damage commences, and clinical features of the disease appear.
The course of the disease will be determined by several factors:
The extent of damage is a product of the:
Cells are broadly divided into three kinetic characteristics:
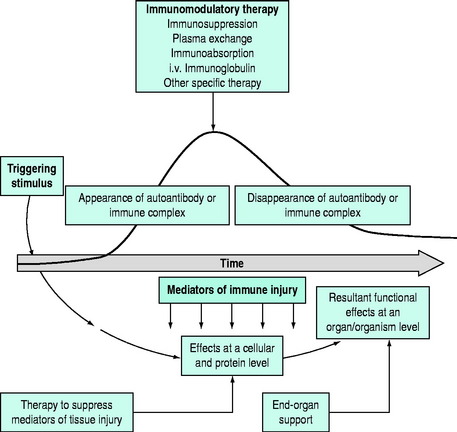
As most disorders are multifactorial, it is unlikely that a single form of therapy will be successful. A multipronged approach to therapy needs to be planned following an analysis of the basic underlying pathophysiology. The stage of the disease is also important (Figure 90.1). Clearly, plasma exchange will have a different response when autoantibody production is rising rapidly, compared with a stage when autoantibody has ceased production. Also, immunoregulation is a complex process, and therapies may interfere at different points in the immune mechanisms.
In some circumstances, specific and directed therapy may attack the most relevant link in the pathophysiological chain, but overall multiple approaches to therapy may be required. In general, plasma exchange is a temporising procedure and concomitant immunosuppressive therapy is required to maintain control. Plasma exchange for autoimmune disease should generally be regarded as a first step in immunomodulatory therapy, and restricted to acute or fulminant situations in which autoantibodies or immune complexes are responsible for life-threatening or end-organ damaging complications. There are some situations in which the humoral factor may be only transient (‘one antigen hit’ disorders), and no follow-up immunosuppression is required (e.g. acute postinfectious polyneuritis). Increasing monoclonal antibody therapy with rituximab (an anti-CD20 antibody) is finding a role in the longer term management of autoimmune diseases.2,3
The availability and recognition of the immunomodulatory effects of intravenous immunoglobulin has resulted in an exponential increase in its use in immune and inflammatory disorders, with its availability being one of the main drivers of the supply of human-derived plasma products. In most of the immune and inflammatory disorders in which plasma exchange has been used, intravenous immunoglobulin has been used. The mechanisms of action of intravenous immunoglobulin remain controversial. Intravenous immunoglobulin, fractionated from normal human plasma, was introduced as a replacement therapy for humoral immunodeficiency disorders, but is now widely used for a range of autoimmune and inflammatory diseases. Progress is being made in understanding the complex mechanisms by which IVIG has immunomodulatory actions. The mechanisms of action of IVIG involve modulation of expression and function of immunoglobulin Fc receptors, interference with activation of the complement system and the cytokine and immunoglobulin idiotype networks, and regulation of cell growth. There is also evidence for effects on activation, differentiation and effector functions of dendritic cells and T and B lymphocytes.4