CHAPTER 24
Subconjunctival Hemorrhage
Presentation
This condition may occur spontaneously or may follow a minor trauma, coughing episode, vomiting, straining at stool, or heavy exercise. There is no pain or visual loss, but the patient may be frightened by the appearance of her eye and have some sensation of superficial fullness or discomfort. Often a friend or family member is frightened by the appearance and insists that the patient see a physician. This hemorrhage usually appears as a bright red area covering part of the sclera but contained by the conjunctiva (Figure 24-1). It may cover the whole visible globe, sparing only the cornea.
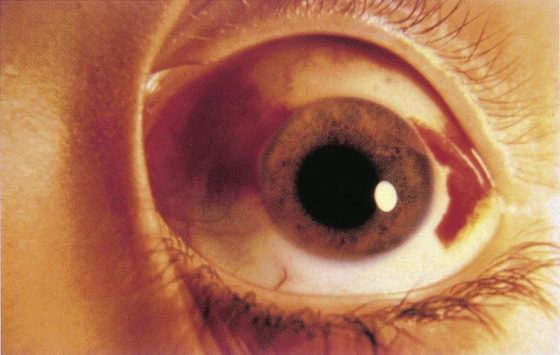
Figure 24-1 A bright red area covering part of the sclera. (From Marx J, Hockberger R, Walls R: Rosen’s Emergency Medicine, ed 6. St Louis, 2006, Mosby.)
What To Do:
 Look for associated trauma or other signs of a potential bleeding disorder, including overmedication with anticoagulants. A history of significant trauma or evidence of recurrent hemorrhage or bleeding from other sites (e.g., hematuria, melena, ecchymosis, epistaxis) warrants a careful evaluation for ocular trauma or a bleeding diathesis.
Look for associated trauma or other signs of a potential bleeding disorder, including overmedication with anticoagulants. A history of significant trauma or evidence of recurrent hemorrhage or bleeding from other sites (e.g., hematuria, melena, ecchymosis, epistaxis) warrants a careful evaluation for ocular trauma or a bleeding diathesis.
 Perform a complete eye examination that includes (1) best-corrected visual acuity assessment, (2) conjunctival sac inspection, (3) bright-light examination of the anterior chamber, (4) extraocular movement testing, (5) fluorescein staining, and (6) funduscopic examination.
Perform a complete eye examination that includes (1) best-corrected visual acuity assessment, (2) conjunctival sac inspection, (3) bright-light examination of the anterior chamber, (4) extraocular movement testing, (5) fluorescein staining, and (6) funduscopic examination.
 Reassure the patient that there is no serious eye damage; explain that the blood may continue to spread, but the redness should resolve in 2 to 3 weeks.
Reassure the patient that there is no serious eye damage; explain that the blood may continue to spread, but the redness should resolve in 2 to 3 weeks.
What Not To Do:
 Do not do an extensive hematologic workup for isolated subconjunctival hemorrhage in healthy patients who are not taking anticoagulants.
Do not do an extensive hematologic workup for isolated subconjunctival hemorrhage in healthy patients who are not taking anticoagulants.
 Do not neglect to warn the patient that the redness may spread during the next 2 days. If the patient is not warned, she may return, alarmed by the “growing hemorrhage.”
Do not neglect to warn the patient that the redness may spread during the next 2 days. If the patient is not warned, she may return, alarmed by the “growing hemorrhage.”
 Do not ignore any significant finding discovered during the history or complete eye examination. Penetrating injuries, lacerations, and ruptured globes also present with subconjunctival hemorrhage, obscuring the damage beneath.
Do not ignore any significant finding discovered during the history or complete eye examination. Penetrating injuries, lacerations, and ruptured globes also present with subconjunctival hemorrhage, obscuring the damage beneath.
Although this condition looks serious, it is usually caused by a harmless leak in a superficial conjunctival blood vessel resulting from trivial trauma or a sudden Valsalva maneuver or coughing. Patients only need to be reassured that although it appears to be serious, this is actually a minor problem that will resolve spontaneously over time without any eye damage. Recurrent hemorrhage or evidence of other bleeding sites should prompt evaluation for a vasculitis or clotting disorder, with blood tests that should include an erythrocyte sedimentation rate, a complete blood count, platelet count, prothrombin time, partial thromboplastin time, and international normalized ratio (INR).
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



