Location
Technical skills
Hospital systems issues
Teamwork/Communication
In-situ/on ward
+
++
++
Simulation center
++
−
++
In terms of who should be trained, there is growing evidence that the answer is the entire team, and not just the physicians. When reviewing programs that have demonstrated improvements in actual patient outcomes, Siassakos et al. noted that there were several common themes [52]. Key components of effective simulation training programs included the following:
1.
Teamwork training combined with clinical training in a multidisciplinary format: There has been a shift in focus of training from working with just physicians. It is now recognized that communication issues are a leading cause of poor outcomes and that the entire team needs to be engaged in the effort.
2.
Relevant, “in-house” training: Because of the difficulties getting complete teams together at simulation centers located outside of the hospital, many trained on their actual unit or at least in their hospital. This made multidisciplinary training possible and allowed for the identification of institution systems issues. Most importantly, these units worked to train almost 100% of their staff, and not just a select few.
3.
Local solutions: The successful programs took national guidelines and then evaluated their own systems. They then created solutions that followed best practices and yet still worked within the capabilities of their institution.
4.
Realistic training tools: With regard to simulators and training tools, the authors found that high fidelity and engagement of the learners was more important than having the most “high-tech” simulators available.
5.
Institution-level incentives: Besides strong support from leadership, hospitals with effective programs often were offered financial incentives including significant discounts on their malpractice premiums.
Gynecology Simulation
Background and History
Ancient Greece gave us the well-recognized apprenticeship model of training – see one, do one, teach one. This has been the mainstay of medical education, and especially surgical education, but has come under increased scrutiny in current times. This apprenticeship model is being recognized and identified as being outdated, inefficient, and potentially dangerous in the face of today’s complicated surgical environments. There is also an increased awareness and appropriate intolerance of high error rates in healthcare. These issues are driving a mandate that alternative and safer methods of training be developed and implemented. Simulation has clearly emerged as part of the solution to this problem [53].
The concept of simulation is not novel in surgery. As early as 800 BC, Sushruta (one of two potential “fathers of surgery”) recommended practicing on melons and wormed wood for training his students in surgery [54]. Many other sophisticated or high reliability organizations have used simulation technology for decades, and healthcare is only now trying to catch up. Aviation and nuclear energy for years have integrated simulation into both their education and quality improvement programs. The aviation industry has regularly scheduled assessments on flight simulators as an integral part of a pilot’s maintenance of licensure and accreditation. Many of these simulators started out very simply, and this holds true in gynecologic surgery as well.
Early pioneers of simulation in healthcare like David Gaba (Chap. 2) introduced the modern era of simulation in healthcare by promoting mannequin training in the late 1980s [55]. It has only been within the last 15 years that disciplines like surgery and gynecology have embraced the concept of surgical simulation. Other pioneers in simulation have called for our specialty to move away from the subjective approach of assessing a trainee’s skills and employ more objective metrics [56, 57]. It was also during this time that practice outside the operating room (OR) in either a simulated environment using box trainers or virtual reality was found to be more effective than traditional methods for developing operative skills [53, 58–60].
Simulation continued to develop and was growing as the landmark publication To Err Is Human became well known in 1999 [61]. The follow-up publication, Crossing the Quality Chasm, advocated the adoption of simulation training as a possible solution to the high error rates in healthcare [62]. After these publications, the promotions by leaders in the field, and the increasing evidence in the literature, simulation began to take hold as a serious contender as a method for learning surgical skills and especially in gynecology.
Gynecologic Simulators
A simulator can simply be an object, device, situation, or environment by which or in which a task or sequence of tasks can be realistically and effectively presented [63, 64]. Surgical simulators range from simple part-task trainers to sophisticated virtual reality simulators and from robotic simulators to standardized patients. In gynecology, many task trainers depict the pelvis and are used for specific procedures or skills like pelvic exams, intrauterine device (IUD) placement and removal, hysteroscopic resection, and urethral sling placement (Fig. 30.1).
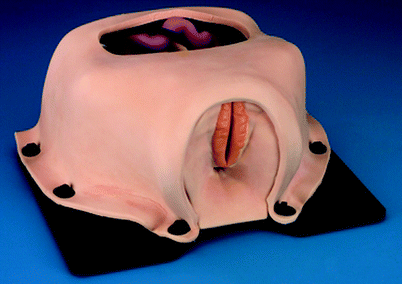

Fig. 30.1
Urethral sling procedure trainer. Limbs & Things, Savannah, GA (Photo courtesy of Limbs & Things ©2012 www.limbsandthings.com)
When it comes to actual surgical procedures like laparoscopy, robotic surgery, or open gynecologic cases, the field of simulation has changed dramatically. For laparoscopic simulators, there are three basic types: (1) box trainers, (2) virtual reality, (3) hybrid simulators.
Box Trainers
As the name implies, box trainers consist of a box that mimics the abdominal cavity with different levels of realism. They are usually connected to a video camera that can project what the learner is doing in the box onto a video monitor. There are different training models that can be used with real laparoscopic instruments through trocars that are set in the lid or top of the box. A striking advantage to this form of simulation is that most people can fabricate their own box trainer using readily available inexpensive items such as a box, a light bulb, an inexpensive webcam, and a PC monitor. In addition, these are very portable and accessible on the ward or at home. The major drawbacks for this type of simulator include the inability to record the simulations, the lack of built-in assessment and feedback tools, and the lack of anatomic and haptic fidelity.
Virtual Reality (VR)
Virtual reality (VR) surgical simulators contain an array of electronic devices that function together to allow one to experience auditory and visual input in order to simulate a real setting or event. Most of the time these devices employ software running on a computer connected to a physical interface, like a handpiece [63]. The VR simulator can have different training tasks which mimic actions performed during surgery, with varying degrees of realism. A distinct advantage is that the computer will register and collect all movements and actions that are made, thus providing an excellent method of objective assessment and feedback for the trainee.
Historically speaking, VR simulation can be classified into four different generations of simulators. The first generation VR simulator was simple and based on the manipulation of abstract objects in a three-dimensional non-anatomical virtual space. These particular simulators were designed for the development of particular physical skills like visual-spatial perception, hand-eye coordination, and manual dexterity (Fig. 30.2). The second generation VR simulators introduced anatomical objects like the ovary or fallopian tube. This inherently made the experience more realistic (Fig. 30.3). The third generation VR simulators had more sophisticated software programs combined with an anatomically correct mannequin for very realistic training (Fig. 30.4). The fourth generation VR simulators include didactic teaching programs with prerecorded video examples. This generation often offers a combination of basic skills training like dexterity, hand-eye coordination, and instrument handling. This functionality incorporates a cognitive component of surgical anatomy, sequencing of operative procedures, and surgical decision making [63, 64]. The advantage to VR simulators lies in their realism and the potential to provide objective feedback based on the mechanism of the simulator. The distinct disadvantage to the VR simulator is their cost. These high-fidelity simulators can easily cost over $100,000, thereby limiting the number of institutions that can afford them.

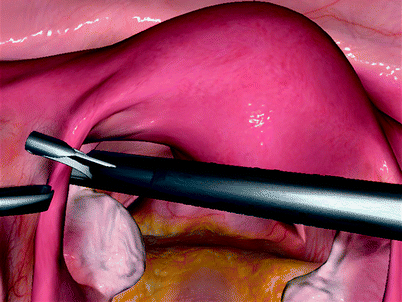
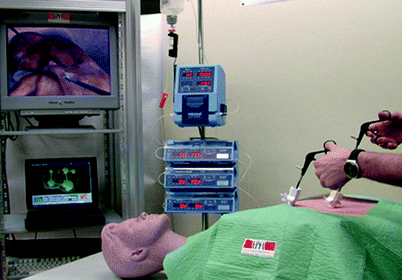

Fig. 30.2
Hand-eye coordination. LapMentor, Simbionix, Cleveland, OH (Used with permission from Simbionix, Cleveland, OH)

Fig. 30.3
Tubal sterilization, LapMentor, Simbionix, Cleveland, OH (Used with permission from Simbionix, Cleveland, OH)

Fig. 30.4
VR simulator with high-fidelity mannequin
Hybrid Simulators
Hybrid simulators, as the name implies, are essentially a combination of a box trainer and a VR simulator and may be thought of as a computer-enhanced video box trainer [63]. The combination of VR imaging with real instruments and physical materials allows trainees to have the sensation of manipulating real physical objects. Some of these systems may also include computer-generated assessment and feedback (Fig. 30.5).
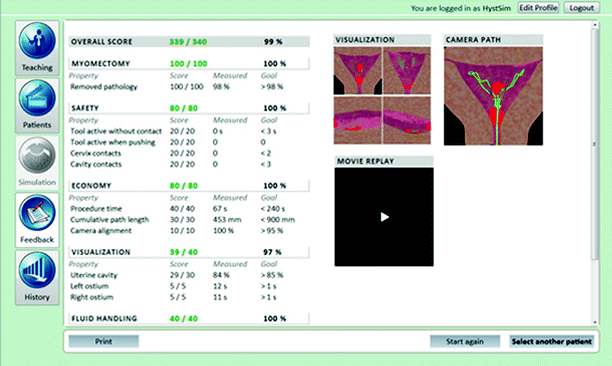

Fig. 30.5
VR simulator feedback, VirtaMed HystSim, Simbionix, Cleveland, OH (Used with permission from Simbionix, Cleveland, OH)
Robotic Surgery
Robotic laparoscopic surgery is the next frontier in gynecologic surgery and technology. While laparoscopic surgery has become fully integrated into the gynecology aspect of nearly all OB/GYN training programs, the future will have a heavy emphasis on robotic surgical training and techniques. Robotic technology in the OR offers minimally invasive surgery (MIS) options for many major surgical procedures. The robot is a combination of hardware and software programmed to communicate and interact with the environment. This technology markets itself as being different than the more traditional MIS method of laparoscopy (Fig. 30.6). In laparoscopy, the human eye perceives a two-dimensional view of the surgical site, while robotic equipment provides a three-dimensional view [65, 66]. Another difference is the ergonomics of conventional laparoscopy vs. the robot. In laparoscopy, the surgeon must stand while holding long instruments; with robotics the surgeons can sit while performing procedures [67]. Also, the robotic instruments provide significantly greater range of motion than traditional laparoscopic instruments, and the technology of the robot eliminates the “fulcrum effect” which in traditional laparoscopy forces surgeons to move their hands in the opposite direction of the instrument’s tip [66]. Finally, another advantage of the robot is that it reduces any tremors the surgeon may have and allows the surgeon to select the scale of the ratio of the size of hand movements to the movement of the instrument tips [66, 68, 69].
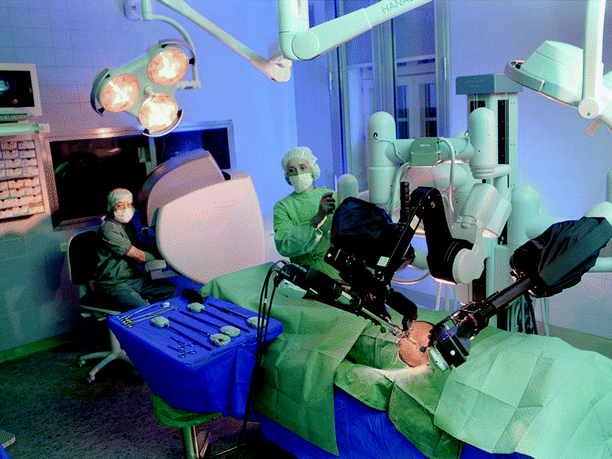

Fig. 30.6
Da Vinci robot. Intuitive Surgical, Sunnyvale, CA
While the da Vinci robotic surgery system offers several advantages in comparison to the traditional laparoscopic techniques, there are some disadvantages that limit its widespread use at all institutions. One of the main drawbacks of the robotic technology is the amount of time it is required for a surgeon to master its use. The next constraining factor is the cost of the device. The da Vinci robot costs well over $1 million, which makes it difficult for smaller hospitals to afford. Because of these factors, inexpensive simulation training methods are critical to decreasing learning time on the equipment.
Simulation for Gynecologic Procedures
While the traditional classroom setting cannot make up for actual hands-on operating time for a surgical trainee, the perceptual and psychomotor skills, which are of key importance for effective surgical technique, cannot be developed in lectures and seminars [70]. Simulation can provide additional learning opportunities in a way that can be self-directed and prepare the trainee for supervised training received in direct patient care [63]. Currently, there are simulators for gynecology that record the operator’s performance and provide instant automated individualized feedback to its user. This feedback allows the trainee to monitor and refine their technique. The aim for trainees is to arrive at actual surgical procedures with better hand-eye coordination, greater familiarity of equipment, better efficiency in movement, and better knowledge of the surgical sequence [63]. The Simbionix Hyst sim and pelvic exam simulators help trainees acquire skills efficiently (Figs. 30.7 and 30.8).
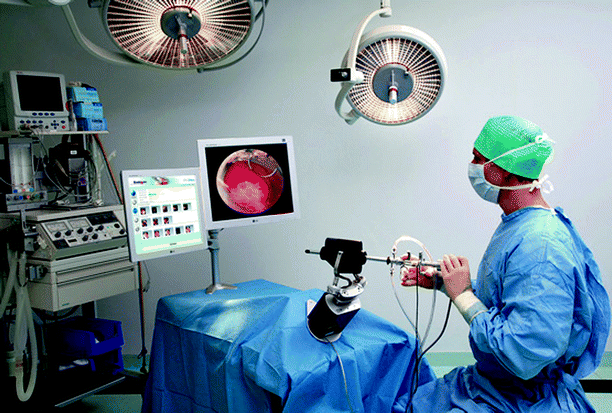
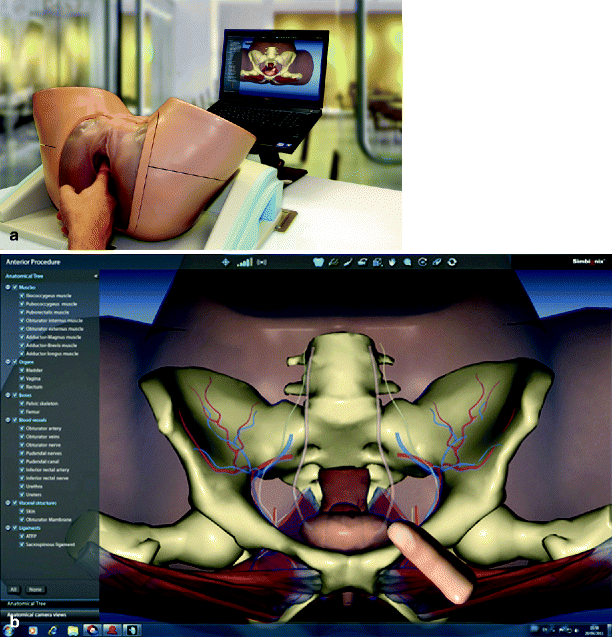

Fig. 30.7
Simbionix Hyst Sim (Used with permission from Simbionix, Cleveland, OH)

Fig. 30.8
(a) Simbionix pelvic trainer and (b) screen capture of trainee digit during pelvic palpation (Used with permission from Simbionix, Cleveland, OH)
Many institutions across the country are now developing and opening simulation centers to assist in the training of their students, residents, and physician staff. The centers may be discipline-specific or interdisciplinary. Many of these centers have sessions for training medical students, residents, nurses, and attending physicians individually and together in team training. Residency programs are also scheduling time with these centers to integrate simulation training into the curriculum. In institutions where there is no simulation center per se, departments can still use stand-alone task trainers and mannequins for training (Fig. 30.9a–c).
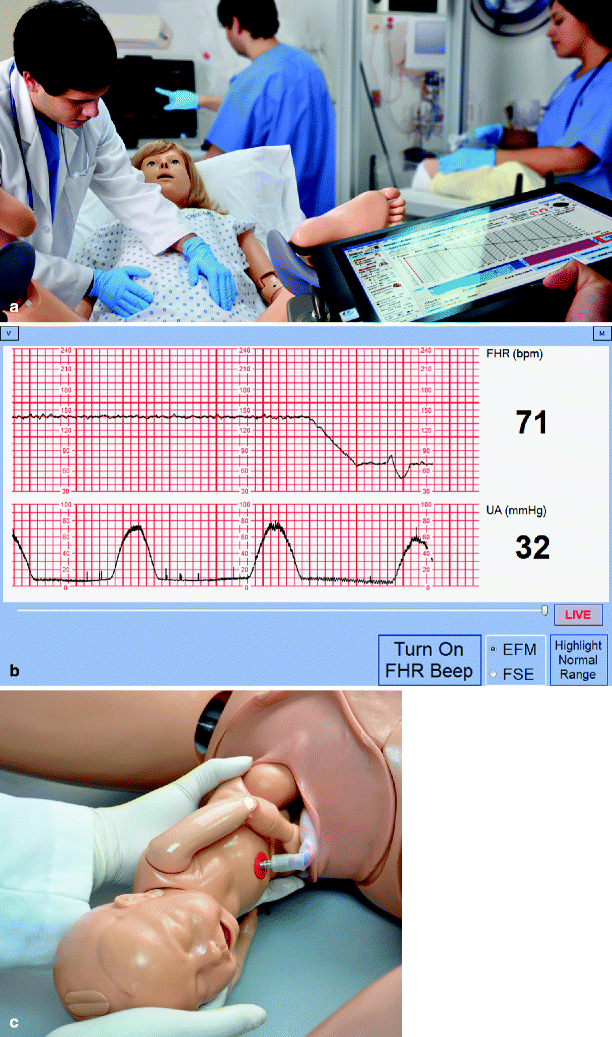

Fig. 30.9
(a) Multidisciplinary scenario of fetal distress (Photo courtesy of Gaumard), (b) simulated fetal heart tracing, and (c) delivery using Gaumard pregnancy simulator
Simulation is also an excellent method for developing interdisciplinary team training in the operating room as well. A critical feature of any teamwork training program is a multidisciplinary approach. Multidisciplinary simulation-based training can be adapted to analyze team performance during a simulated gynecologic emergency. Many institutions are having their ORs adopt well-known and developed team training exercises using simulation to practice rare but catastrophic emergencies that could happen during actual surgical procedures. In these team training exercises, many of the gynecologic simulators such as a VR or box trainers are replaced with high-fidelity mannequins to simulate actual patients. At times a task trainer can be combined with a standardized patient actor to get a more realistic simulation. One report by Powers et al. examined OR teams during simulated surgeries and tasks that included trocar access and management of intra-abdominal hemorrhage utilizing a physical laparoscopic model and measured individual and overall team performance [71].
Evidence for and Current Usage in Training
When looking at simulators for adjuvant teaching modalities, it is critical that the simulator is able to differentiate between learners with different skill levels to determine whether there is any progress in learning or skill acquisition [53]. This is referred to as construct validity and is one of several levels of validation. Consistently showing the same measurement from the same skill levels is important and is termed reliability. The ultimate criteria for a simulator’s value would be its predictive validity and transference to the actual OR, and this is the goal of all training programs.
In gynecology most studies have examined validation and transference in the use of box trainers or VR simulators. A study by Aggarwal et al. looked at one of the early commercially available laparoscopic VR simulators (LapSim®, Surgical Science Sweden, Göteborg, Sweden) and found that intermediate and expert surgeons differed in their ability to complete a surgical module of salpingectomy for ectopic pregnancy [19]. This implied that the skills needed for VR are similar to those needed for real surgery, a good example of construct validity for this simulator [63, 72]. In the same study when novices and intermediate surgeons practiced on the VR simulator and improved their performance in the simulation laboratory, the result in the actual OR was a reduced median procedure time [72]. Another randomized controlled trial that compared VR simulation training was being added to clinical surgical training with traditional surgical training alone for salpingectomy and found a significantly shortened time in training to achieve competency in salpingectomy [73].
A recent Cochrane review of VR laparoscopic training in surgery has suggested that, in participants with limited laparoscopic experience, VR training results in a faster reduction in operating time, errors, and unnecessary movements than does standard laparoscopic training [74].
In the studies discussed, even though construct validity in realism and training was shown, it is still not clear whether the simulators used and/or the designed curriculum were appropriate predictors of clinical surgical ability. The predictive validity has yet to truly be shown in any well-designed study or trial. As educators and surgeons, it is essential to critically analyze the different components (i.e., blood loss, instrument path, or operating time) that make up some of the scores in these studies and see which are truly most important in real life [63].
Team Training in Gynecology
Simulation is clearly being used to teach technical skills, but by comparison, there has been relatively little work in the surgical simulation arena designed to teach or assess, interpersonal and communication skills and professionalism nontechnical skills [75]. Team training and simulation is not new in healthcare. There are many well-established programs across the United States; however, the overwhelming majority in our specialty focus on obstetrics not gynecology. In recent years, the Agency for Healthcare Research and Quality (AHRQ) has sponsored investigations in hopes of enhancing patient safety through team training simulations.
There are currently a few programs that are developing team training exercises in surgery. These include Kaiser Permanente’s Highly Reliable Surgical Team (HRST) and the American College of Surgeons (ACS)/Association of Program Directors in Surgery (APDS) Surgical Skills Curriculum. The HRST and APDS Surgical Skills Curriculum are designed for different surgical specialties and are not specific for gynecology, though there is work to adapt them to the specialty. The ACS/APDS Surgical Skills Curriculum also includes team training that specifically aims to address nontechnical skills [76].
The (HRST) examines the relationship between their patient safety and highly reliable teams, and it is being shared with other institutions. For implementation, Kaiser collaborates with a hospital and begins with the identification and the training of project managers and a steering committee. After this, a safety survey is administered to all the staff, human factors training is provided, and metrics established. With the results of these parts, it is all integrated into the OR and includes items such as whiteboards, “glitch books,” briefings, a surgical pause, routine debriefings, and regularly scheduled simulation training events. The required elements and the team training focus on teamwork and communication in the OR between all disciplines.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








