1. Objectives: Create learning/assessment objectives
2. Learners: Incorporate background/needs of learners
3. Patient: Create a patient vignette to meet objectives which also must elicit the performance you want to observe
4. Flow: Develop flow of simulation scenario including initial parameters, planned events/transitions, and response to anticipated interventions
5. Environment: Design room, props, and script and determine simulator requirements
6. Assessment: Develop assessment tools and methods
7. Debriefing: Determine debriefing issues and mislearning opportunities
8. Debugging: Test the scenario, equipment, learner responses, timing, assessment tools, and methods through extensive pilot testing
Starting in 2010 there was an initiative by the Council of Residency Directors in emergency medicine and the Simulation Academy of the Society of Academic Emergency Medicine to update and revise an existing bank of cases used for oral examination practice. This initiative focused on building a shared bank of cases following a standard template which could be used by residency programs for simulation-based education, mock oral cases, or as an assessment resource. Each case was submitted by experienced simulation faculty and went through a rigorous peer-review process. The cases are accessible to all residency program members from emergency medicine. There are secure cases designed to be used for resident assessment as well as open-access cases which can be used to teaching or practice. This open-access portion of the website is available at www.cordem.org.
Equipment and Space
There has been strong growth in the use of simulation technology in emergency medicine since 2000, with the majority of accredited residency programs in the United States currently using some form of mannequin-based simulation [27]. Along with this trend has come a proliferation of simulation centers with technological resources and space dedicated to high-end clinical and procedural simulation, videoconferencing, and standardized patient encounters. Of the three professional organizations that have created accreditation standards for simulation programs (the American Society of Anesthesiologists, the American College of Surgeons, and the Society for Simulation in Healthcare), only the American College of Surgeons lists specific space and technological requirements for simulation centers. The SAEM Simulation Academy does not emphasize hardware or space requirements for simulation programs, recognizing that these are highly dependent on the educational goals and the resources available to individual programs [61]. Additionally, as high-fidelity simulators become increasingly portable and require less supporting equipment, it becomes less clear that a “fixed” simulation center is advantageous in every setting [28]. Successful in situ simulation can be conducted even within the confines of an ambulance, and its use in the clinical environment may indeed represent the natural evolution of the technology [62]. The following example provides a description of a dedicated space used for emergency medicine simulation but is not intended to be prescriptive.
For high-fidelity patient care scenarios, the space used for simulation should match the clinical environment in terms of equipment, patient monitoring, and available personnel as closely as possible (Fig. 20.1). For emergency medicine-specific simulation, this includes a basic cardiac monitor capable of displaying simulated vital signs and which can be manipulated remotely, IV supplies (IV catheters and start-kits, tubing, fluids, and an IV pole), equipment for managing airway emergencies (wall-mounted suction, bag–valve–mask, intubation tray), and a defibrillator and code cart. The added value of having functional equipment (e.g., suction, supplemental oxygen, defibrillator capable of delivering shocks) is debatable and should not be viewed as requisite for successful simulation. Additional equipment such as ventilators lends heightened realism to scenarios but at considerable cost and need for additional storage space. In situ simulation can mitigate many of these challenges, as scenarios can be conducted in the clinical environment with actual equipment.
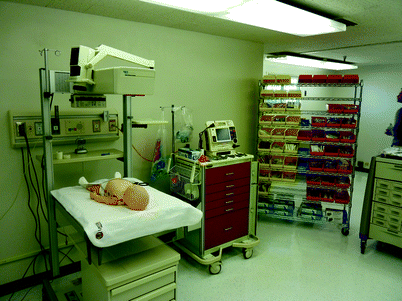

Fig. 20.1
Pediatric simulation lab
In addition to the simulation space, consideration should be given to a control area from which to conduct the scenario. Ideally, this should include a “line of sight” (such as a one-way mirror) to the simulation area in order to facilitate quick adjustments during scenarios in progress, as well as adequate sound proofing to prevent interference from those conducting the scenario (Fig. 20.2). This may require some creativity in the case of in situ simulation, where the ability to create adequate distance for those conducting the simulation can be difficult. In these instances, a well-placed curtain or an adjacent doorway may be the best option. An area for observation and debriefing, ideally in a location adjacent or close to the simulation area, should also be available (Fig. 20.3). Depending on the audiovisual capabilities of the facility, this space can be used for video monitoring of ongoing simulation as well as post hoc review for debriefing. Finally, it should be emphasized that dedicated space for equipment storage, as well as for fabrication and repair of materials used in simulation, is essential to any simulation program and may be underestimated or overlooked in initial design.



Fig. 20.2
Control room showing view of simulation area

Fig. 20.3
Debriefing room
Debriefing
Debriefing is a critical component of simulation education and is discussed extensively in Chaps. 6 and 7. For debriefing to be successful, it needs to be timely, focused, task based, and linked to established goals and objectives. The first part of developing a simulation program is identifying the learning objectives, which will be closely linked to the debriefing content. It is important that the faculty debrief to the task/learning objective rather than focusing on the learner being debriefed. In emergency medicine, video-assisted debriefing immediately after the scenario is used frequently. Most often team performances are debriefed with the entire team, and this is especially important in simulations that include a variety of healthcare professionals.
The specific debriefing model varies widely across different programs and with different learners. One common technique is the “Plus/Delta” model (what went well, the Plus vs. what can be improved, the Delta), which is useful for relatively straightforward discussions [63]. The WISER Simulation program uses a model referred to as “GAS” which stands for Gather–Analyze–Summarize. This three-step technique focuses on active listening followed by facilitating learner reflection and analysis of their actions and finally a summary of lessons learned [64]. A third technique is the “Debriefing with Good Judgment” model, which uses an advocacy–inquiry model to assist in the discovery of the participants’ “frame” or understanding of the situation that underlies the visible action [65]. This technique is useful to understand more complex individual and team behaviors. Emergency medicine educators have strongly embraced debriefing because of its important role in deliberate practice and the development of mastery skills.
Funding
Simulation programs require substantial initial investments of capital and robust sources of operational funding for both personnel and equipment [66]. To successfully cultivate an array of funding sources, the leadership team should make use of all available resources within an institution. A combination of internal and external funding sources is necessary in many cases. Fortunately, simulation training appeals to a broad audience and tends to easily address the needs and goals of administrators, department chairs, program directors, hospital and university governing boards, governmental granting agencies, private foundations, and individual philanthropists. The concepts of patient safety, healthcare quality, and efficient training and evaluation of providers resonate widely. When it is recognized that funding a simulation center is a “win–win” situation for the institution, the providers’, and most importantly the patients’, funding tends to follow.
Those in a position to initiate a simulation program will need to advocate for the utility of simulation training and the ability of well-designed programs to serve the needs of the individuals, programs, and the institution. As the center matures, the need to maintain funding will require proof of effectiveness. Robust data collection and tracking will demonstrate that a simulation center can help the institution efficiently meet its requirements from the Joint Commission, American Nurses Credentialing Center (ANCC), and the Accreditation Council for Graduate Medical Education (ACGME) [43, 45, 67–69].
Beyond even these requirements, consistent training and evaluation of providers to maintain skills and improve quality helps to justify financial outlay from administration. Reducing medical errors and improving quality through simulation may lead to a reduction in healthcare delivery costs and even a reduction in medical liability premiums [70]. Additional drivers such as maintenance of board certification make simulation a necessary element in ongoing training and provider evaluation [71]. Simulation funding should be viewed as an investment in quality, efficiency, and safety.
Budget Allocations
An investment in a simulation program pays dividends regardless of the clinical environment. Whether serving a small contract group, a large multihospital group, or an academic program with a residency, budgetary allocations will provide the most consistent source of funding. Centers have been started and even operated for several years with funding from a single large grant, but sustainability relies on consistent funding both for personnel and equipment. It becomes the job of the simulation leadership team to reveal the benefits of simulation and leverage the many drivers to generate budget allocations. As a simulation center develops a consistent source of funding, directors and staff can focus more of their energies on simulation program development and dissemination. Because simulation is increasingly being shown to improve real patient outcomes and even decrease healthcare costs, it has demonstrable value to all those who control operational and capital budgets. Those who control operational budgets often are the same individuals who will benefit from the data generated in a simulation center, helping them to fulfill training, reporting, and accreditation requirements.
Philanthropy
Foundations and individual donors are a critical source of funding for both capital and operational budgets. Capital purchases tend to be more appealing to donors, but the goals of various foundations differ. It takes a firm understanding of the development process to work with potential donors to achieve mutually beneficial goals. This almost always requires that the simulation team work with a skilled and experienced development staff. These individuals can help identify potential donors, prepare presentations, generate publications, and facilitate the donation process. This involves balancing the needs of a simulation center with those of an entire institution, but often the appeal of simulation attracts considerable interest. Smaller groups or those without development personnel may identify donors on their own. A grateful patient or family, a local foundation with a shared mission, or even personal connections can provide fruitful opportunities. It is important to recognize these very important contributions with naming rights, donor recognition displays, publications, and sponsorship materials.
Corporate donors can potentially provide funding through a variety of mechanisms. A company may be interested in providing discounted clinical equipment since it is to their advantage to have their product used by a large audience. They may be willing to rent space to train their sales representatives and healthcare providers, or provide sponsorship for CME programs. Lastly, they may be willing to provide donations outright for naming rights to a simulation space.
Those with a direct stake in simulation training, including current faculty, physicians, and nurses, are often willing to make contributions through a giving campaign. Many programs have alumni funds that are used for education. Alumni easily recognize the importance of quality training opportunities for current trainees. A simulation center provides such tangible benefits. When a donor sees a simulator, a task trainer, or a named simulation room, they know that their money is having a direct impact on training and patient care.
Granting Agencies
Federal agencies largely under Health and Human Services including NIH, HRSA, and AHRQ make specific calls for funding proposals. Writing a federal grant application requires a significant level of experience and sophistication, a task made much easier if a support staff is available. Novice grant writers should seek to develop a track record of peer-reviewed publication and smaller grants before pursuing federal funding. State funding from EMS agencies can be a fruitful place to start, as can specialty-specific granting bodies including the Society for Academic Emergency Medicine and the Emergency Medicine Foundation. Grants targeted not only at simulation but any program that involves patient safety, reduction of medical errors, and healthcare quality improvement may be suitable for simulation-based applications.
Fee Generation
Attempts are being made at some centers to operate on a fee-for-service business model. The success of such a model depends on potential client mix and the ability of these client groups to establish and operate their own programs rather than turning to a third party. Medium to large groups, hospitals, universities, and academic departments have the resources to seek funding in a number of areas, making an investment in creating a simulation program worthwhile. Individual practitioners and small groups may not be able create and operate their own simulation programs, thus are likely to be potential clients of a fee-for-service center. Future market conditions and an increasing desire for courses that incorporate simulation may lead some fee-for-service simulation centers to a greater likelihood of sustainability.
Few centers are currently able to cover all operating expenses with fees alone. For most centers, fee generation from CME and maintenance of certification courses will be most effective if viewed as a way to defray the cost of capital improvements and operations rather than a method to cover all operating costs or generate profits.
Faculty Development in Simulation
Emergency medicine faculty are similar to all simulation educators in that they should be familiar with the advantages and disadvantages of simulation as an educational tool. Simulation will not be effective unless it is used as a well-planned and thoughtful part of the entire curriculum [72]. Faculty time constraints and lack of training were the top two barriers to simulation use in a recent study of emergency medicine simulation users [27, 73]. Faculty members who are interested in providing educational sessions for physicians in residency training must therefore be supported with adequate release time and training. General educational competencies such as objective writing, feedback, and assessment are required skills in simulation [74–76]. All faculty should also be experts in the clinical content area. Finally, the faculty member must develop expertise in simulation-specific skills such as scenario design, debriefing, and some technical knowledge about simulator operation, capabilities, limitations, and programming. These skills can be gained through institutional level training programs or by attending specialty-specific meetings where simulation is a focus. Some examples of these include the AEM Consensus Conference, the Council of Emergency Medicine Program Directors Annual Meeting, or the ACEP Teaching Fellowships and Simulation Courses. Many emergency physicians have also received training at simulation-specific national courses such as the Institute for Medical Simulation at the Center for Medical Simulation or at the International Meeting for Simulation in Healthcare. Simulation skills should be seen as a core competency for emergency medicine faculty along with the more traditional teaching techniques.
Fellowships
With the almost universal use of simulation in emergency medicine training programs [27], there is growing need for educators trained in how to use the teaching method effectively. This has led to rapid growth in non-ACGME approved fellowships in simulation at a variety of simulation centers, many with active ED participation or leadership. As there is no recognizing body or regulation of such fellowships, so their content and focus varies widely. Many include master’s degree coursework in adult education or certificates. These fellowships are often conducted at interdisciplinary centers and with interdisciplinary leadership that reflect the composition of their simulation centers which often merge educators from different specialties. Funding can be provided by part-time clinical work, department funds, grants, or institutional budgets [28].
The Society for Academic Emergency Medicine lists six simulation fellowships (http://www.saem.org/fellowship-directory): Alpert Medical School of Brown University, Massachusetts General, St. Luke’s-Roosevelt Hospital Center, Stanford University School of Medicine, Summa Akron City Hospital, and University of California, Davis. Each of these fellowships has their own unique strengths and design that are described below. Additional fellowships are being added every year, so this list is meant to provide a sample and is not a comprehensive catalog.
The MGH Fellowship in Medical Simulation in Boston is a tailored program over 1–2 years and includes an established curriculum in the Harvard Macy Institute and the Institute for Medical Simulation. Fellows here run the “On-Demand Medical Education Service” which has been previously published [1, 9]. Certificates in teaching and learning and other advanced certificates are available. Fellows work approximately half time clinically as an EM attending at MGH or an affiliate. The St. Luke’s-Roosevelt program is one of the newest fellowships listed at SAEM and is located in New York City. Taking two people per year as about 20 h clinical, it is a 1-year fellowship and is a joint effort with other departments including critical care.
The Stanford University fellowship in California is one of the oldest and most established fellowships. It is a 1-year fellowship with work at four separate simulation centers. Fellows attend in the hospital emergency department. The Summa Akron City fellowship is a 1–2-year program in Akron, Ohio, and accepts up to two fellows per year. Fellows work in several simulation laboratories and attend in the emergency department at one of three local EDs. The University of California, Davis, simulation fellowship is a 1- or 2-year program, and fellows participate both at the center and in local disaster preparedness training. Fellows work part-time as attending physicians in the emergency department at the UC Davis Medical Center. The STRATUS Center for Medical Simulation Brigham and Women’s Hospital has a 2-year fellowship that includes matriculation into Harvard Graduate School of Education for a master’s degree in education.
Simulation-Based Education
Team Training
High-quality healthcare in essentially all clinical specialties requires a high level of team performance. Nowhere is this more apparent than in emergency medicine where rapid, accurate decision-making and communication must all operate efficiently and effectively to provide optimal care. Errors in communication and inefficiencies in team dynamics can lead to delays, incorrect treatment, and adverse outcomes [77]. By creating a structure to deliberately practice critical team skills in a systematic fashion, dissecting and debriefing all elements of a complex team dynamic, simulation training provides an opportunity that cannot be accomplished easily in a real-world setting.
The principles of team dynamics have evolved largely from other fields, most notably the flight industry. Crew resource management (CRM) principles are widely used in simulator-based exercises for pilots and flight crews [78]. CRM formed the basis for the development of the TeamSTEPPS® program by the Agency for Healthcare Research and Quality, a program that has come into wide usage for healthcare team training [79]. The elements of effective team training include team structure, leadership, situation monitoring, mutual support, and communication. Each of these elements is further subdivided to include key components that can be easily incorporated into simulation scenarios.
It is important to recognize that team training should itself form the simulation case objectives, leading to a delineation of the critical actions and development of evaluation tools. Often, learners will naturally focus on the medical management elements of a case, but when team training is the goal, it becomes the role of the scenario author and director to clearly define the goals, design the scenario to incorporate the critical elements, and focus on these elements in the debriefing.
Robust observation and evaluation tools such as the TeamSTEPPS® performance observation tool, the Behaviorally Anchored Rating Scale (BARS), and Behavioral Assessment Tool (BAT) can be useful adjuncts to scenario design, learner evaluation, and debriefing [79, 80]. Using such tools importantly focuses the objectives on the critical elements of team function.
Assembling the team to perform simulation training can present some challenges. Creating “buy in” and convincing administrators to allocate funds for training requires identifying discipline-specific drivers. Administrators easily recognize the value of simulation training once they become familiar with the ways in which it can help them train and evaluate staff, collect data for reporting requirements (e.g., Joint Commission, ACGME, ANCC), address patient safety goals, and contribute to the reduction of medical errors. Evidence is building in the literature to support these assertions [81]. Additionally, offering CME and CE credit often helps to serve the needs of both the simulation program and individual providers. Building team dynamics and esprit de corps in the real clinical setting has intrinsic value. “If we practice how we play, we play how we practice” resonates with both providers and departmental leaders.
Emergency medicine is uniquely positioned to take advantage of multidisciplinary and multispecialty team training opportunities, interacting with virtually every clinical specialty and often intersecting at the point where well-developed team skills can affect patient outcome. A trauma resuscitation bay, for example, is a nexus of interdisciplinary care requiring physicians, nurses, paramedics, and ancillary staff to function together efficiently and expertly. In the real clinical environment, team members change regularly. A single team with consistent individual members familiar with each other may be elusive. Incorporating standardized team training on a regular basis with all members of a department leads to more clearly defined expectations and greater consistency in care.
In an OR setting, team training has been shown to decrease patient mortality [82]. In the emergency department, team training can be applied to an array of multidisciplinary clinical scenarios. The high-intensity, low-frequency events such as mass casualty situations, pediatric arrest, emergent obstetrical delivery, and neonatal resuscitation all provide an opportunity to bring providers from several specialties and healthcare disciplines together for team training. Beyond the low-frequency events, using simulation to drill the more routine intradepartmental scenarios can improve team dynamics. ST-elevation myocardial infarction, stroke, respiratory distress, status asthmaticus, status epilepticus, and toxicologic emergencies are just some of the contexts within which such team training can take place.
Simulation can be used to develop and troubleshoot new protocols and systems that require a highly efficient team function. “Code STEMI,” “Code Stroke,” and sepsis response protocols, for instance, incorporate an array of moving parts, personnel, and equipment that must function seamlessly. A change in one or two variables may impact the delivery of essential interventions – door-to-balloon time, door-to-drug, or time-to-antibiotics. Rather than altering variables in the real clinical setting, changing them in a simulated setting can allow examination of their impact and help troubleshoot systems and provide an efficient, safe avenue to explore quality improvement. Team training is an essential part of quality healthcare delivery and patient safety, and simulation programs can clearly impact the many facets of healthcare team dynamics to optimize patient outcomes.
Procedural Training
The use of simulation to train practitioners to perform both routine and rare or high-risk procedures has gained traction among virtually every procedure-based specialty. This approach to training is founded not only on pragmatic considerations of patient safety but also on the concept of skill acquisition through deliberate practice [83–85]. Advanced surgical simulators have been developed for training in endoscopy and laparoscopy and have demonstrated a high degree of transfer of training to the clinical setting [86]. Likewise, obstetric simulators have been linked to improved technical proficiency, self-reported confidence and teamwork, and decreased incidence of complications such as shoulder dystocia [87].
Task trainers have become commercially available for a wide array of emergency department procedures. Products that offer a high degree of physical fidelity appear to be of greatest utility for procedures (e.g., intubation) that require complex motor movements and precise navigation of anatomic structures. Medical students trained on simulators can achieve proficiency with uncomplicated intubation in as little as 75–90 min [88], and clinicians trained on simulators perform equally well on fresh cadavers and live patients [89]. Procedures such as cricothyrotomy and chest tube placement are frequently taught with either commercially available products such as TraumaMan (Simulab Corp., Seattle, WA) or improvised synthetic or tissue-based task trainers. While these techniques are employed widely, the evidence for their efficacy in knowledge transfer to the clinical setting is limited. Additionally, there is sparse and conflicting data as to the comparative effectiveness of commercial task trainers versus tissue-based simulation for invasive procedure training [89, 90].
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree








