(1)
Chennai Breast Centre, Chennai, India
Image-guided core biopsy is an important part of any breast lesion that warrants further evaluation. Image-guided biopsies can be performed under ultrasound, mammographic, or MRI guidance.
Lesions that are seen on ultrasound are best sampled by ultrasound guidance. Stereotactic biopsy is limited to lesions that are not palpable and not seen on ultrasound.
Sampling Methods
Fine needle aspiration cytology, core needle biopsy, or vacuum-assisted biopsy can be used to obtain samples.
The reasons why fine needle aspiration cytology is preferred over core needle biopsy in many places are because of the perceived less cost of the procedure and the relative ease with which the procedure is done. It also does not require histological processing and therefore results are available much more quickly. FNAC continues to be the commonest method of choice for evaluating breast lesions in countries where there are limited resources. However, the inadequate smear rate and inconclusive report rates are high with an increased number of repeat biopsy procedures or surgical excision biopsy. When repeat biopsies are done, it not only increases the patient’s anxiety levels, it increases the cost of the procedure and there is a time delay in arriving at a diagnosis. Resorting to a surgical excision biopsy also increases the cost and needs of hospitalization/general anesthetic to do the procedure and may require definitive surgery again if it is malignant.
When a malignancy is diagnosed based on a FNAC, it is difficult to categorize further into whether it is ductal carcinoma in situ or an invasive malignancy. Sometimes it is difficult to differentiate a lobular from ducal carcinoma. It is also not easy to do receptor [ER/PR and Her 2 neu] studies with FNAC smears. In the neoadjuvant setting, the tumor might completely disappear after chemotherapy and it will not be possible to do other predictive or prognostic studies. Papillary lesions are more confidently diagnosed on core needle biopsy with immunohistochemistry if required, than by FNAC. However, FNAC is still very useful in diagnosis of chest wall recurrences and axillary node assessment prior to selection of patients for sentinel lymph node biopsy.
Core biopsy is technically slightly more challenging, costs slightly more, and takes a little longer to get the results. However, the advantages of core biopsy are as follows:
Histological sections are more readily interpreted by pathologists leading to a more definite diagnosis.
A good representative core biopsy is usually adequate to give a definitive diagnosis. Repeat biopsies and further excision biopsies for diagnosis can be avoided.
A large majority of benign lesions can be followed up without the need for surgical excision with a benign pathology report on core biopsy.
If the lesion is malignant, it is possible to differentiate invasive from in situ malignancy and lobular from ductal carcinoma on a core biopsy.
It is possible to do Estrogen and Progesterone receptor studies and Her 2 neu studies on core biopsy samples for proper preoperative treatment planning.
In a neoadjuvant setting, core biopsy tissue might be the only tissue available for prognostic marker and predictive marker studies, as the tumor might respond completely with chemotherapy.
Tumor banking, particularly in the neoadjuvant setting, is usual for molecular studies.
The availability of automated guns has made the procedure extremely easy with image guidance. There is no role for routine testing of coagulation parameters before a core biopsy unless the patient is on warfarin. Patients on aspirin or clopidrogel may bruise a bit more than usual and they are usually withheld for 5 days prior to the procedure. There is no role for routine antibiotics post procedure. The possible risks after core biopsy include.
Hematoma
Ultrasound guidance with color Doppler can usually identify vasculature, and this can be avoided. But, if bleeding occurs, it usually stops with pressure post procedure for 5 min. Ice compresses can be used later by the patient for comfort. The presence of a large hematoma can alter the tactile discrimination for the operating surgeon at the time of surgery to ascertain the gross surgical margins in breast conservation surgery.
Pneumothorax
This can be avoided by the needle staying parallel to the chest wall. It must be remembered that the automated gun has a needle trajectory (throw) of about 2 cm. With some automated guns, this throw can be reduced to 1.5 cm. It is important to keep the entire length of the needle in the breast in vision without angulation toward the chest wall and staying parallel to the chest wall to avoid pneumothorax. When the lesion is close to the chest wall, a generous quantity of local anesthetic can be injected (5–10 ml) behind the lesion between the muscle and the lesion. This lifts the lesion away from the muscle and avoids pain and pneumothorax.
Infection
Infection following a core biopsy is rare, and there is no role for routine antibiotics.
Needle track seedling of tumor: Needle track seedling is a potential risk, but studies have not shown any increase in the incidence of local recurrence because of needle track seedling. However, the site of the skin nick and the needle track can be kept well within the surgical incision, so it can be included in the excision. Targeting accurately and minimizing the number of passes will also reduce the risk of needle track seedling.
False Negative Result
It is possible to miss the lesion due to technical difficulties. Deep seated lesions, poor needle or lesion visualization, or a dense or fibrotic breast tissue may make the procedure difficult and therefore have a discordant result. When there is histological and radiologic discordance, i.e., when mammogram or ultrasound is suspicious of malignancy but core biopsy histopathology is benign or inconclusive, surgical excision must always be done. Accurate targeting of the lesion will minimize the chances of false negatives. Correlating radiological findings with pathology with appropriate recommendation for further biopsy/surgical excision or follow-up should be done.
Core Needle Biopsy
Different automated disposable guns and reusable guns with disposable needles are available. The automated devices are spring-loaded with two sets of springs to move the two sections of biopsy needles. They all have cocking mechanisms, safety device, and a trigger. The inner canula has the tissue trough and the beveled tip for penetration. The length of the aperture determines the after throw of the needle when fired (i.e., the distance travelled by the needle when fired). When the gun is fired, the inner needle advances forward followed almost by the outer canula that cuts the tissue and secures it in the trough. The needle is then withdrawn from the breast, specimen removed, and the gun cocked again for another pass. Coaxial needles are sometimes used to create a tunnel through the breast through which the biopsy needle is placed for taking samples. This avoids multiple tracks through the breast.
Ultrasound-Guided Core Needle Biopsy: A Step-by-Step Approach
1.
Lesion should be clearly visualized on ultrasound. Doppler is useful to look for blood vessels closer to the lesion, particularly for biopsies in the axillary area (Fig. 23.1).
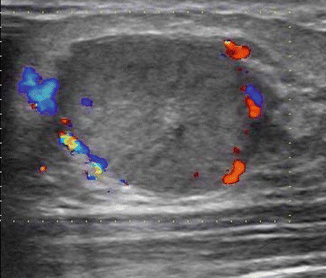

Fig. 23.1
Doppler is useful to avoid blood vessels closer to the lesion
2.
Biopsy tray should be readily available (Fig. 23.2).
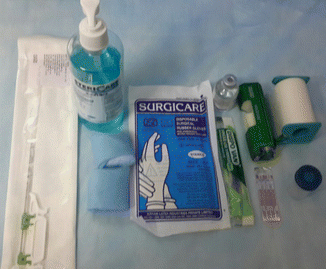

Fig. 23.2
Tray
Local anesthetic
11 blade
Gloves
Biopsy gun/ needle
Disinfectant
Sterile gauze
Formalin container to receive samples
3.
Consent.
An informed consent should be obtained.
4.
Patient positioning
It is important to get the patient positioned well before the procedure. The purpose of positioning is to ensure that the needle remains parallel to the chest wall during insertion and firing. The breast should be as flat as possible with the patients hand over the head. For lesions in the outer quadrant, an oblique 30–40° tilt would be useful. If the breast is ptotic and the skin very wrinkled, the assistant can stretch and hold the breast so that the biopsy site is flat and skin stretched. If an assistant is not available, a plaster can be used to fix the breast so that the area to be biopsied if flat.
5.
Position the machine in such a way that the operator can see the screen in front, without having to turn the head to see the monitor of the machine.
6.
Use the nondominant hand to hold the probe and the dominant hand to hold the biopsy device (Fig. 23.3).
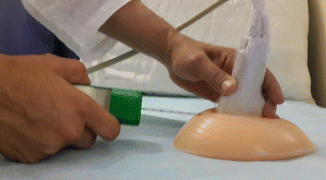

Fig. 23.3
Nondominant hand should hold the probe, and the dominant hand should use the biopsy gun
7.
The probe should be coated with jelly to make contact and covered with cling film, with another coat of jelly over it. This protects the probe from contact with blood (Fig. 23.4).


Fig. 23.4
Protect the probe with cling film
8.
Probe screen orientation. The probe is usually marked with a line or a dot to orient the left or right of the screen image. It is easier to get used to the needle entry through one side of the screen, i.e., either from the right or the left of the screen (Fig. 23.5).
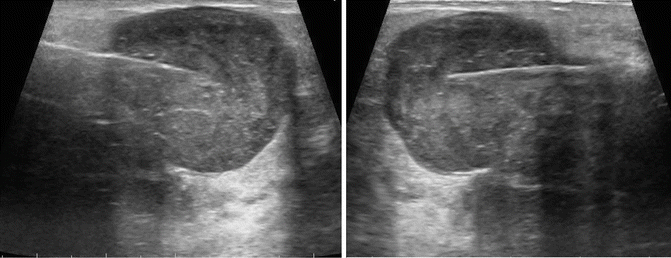

Fig. 23.5
It is easier to get used to the needle coming from one side of the screen
9.
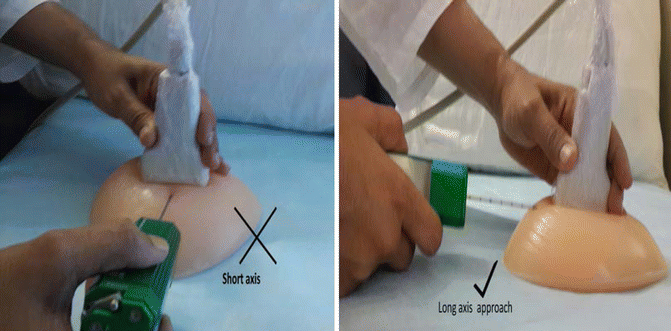
Approach : It is preferable to use the long axis approach as the needle will be parallel to the chest wall with this approach. The entire length of the needle should be visualized (Fig. 23.6).