Fig. 20.1
Thermoregulatory responses (Reprinted with permission, Cleveland Clinic Center for Medical Art & Photography © 2015–2017. All Rights Reserved)
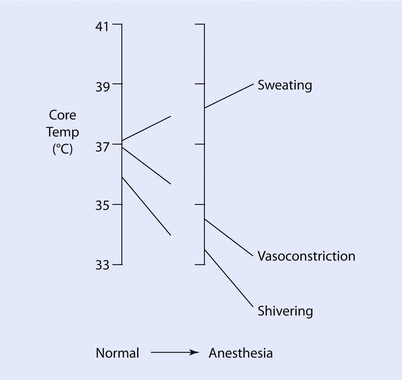
Fig. 20.2
Thermoregulatory thresholds
The ability to react accordingly is based on complex temperature sensing and thermoregulatory properties. Afferent sensing, central regulation, and autonomic and behavioral defenses are the main cornerstones of body temperature control.
Body temperature is sensed in the periphery and throughout the body by a wide range of nerves and receptors. The most important body temperature receptor is the transient receptor potential (TRP) protein. The TRP receptors were recently identified and consist of several subspecies. Among them, the TRPV receptors 1–4 are activated by heat, while other subspecies, such as the TRPM8 and TRPA 1, are activated by cold. Thereby activated signals are primarily transmitted by tracks of the anterior spinal cord to the brain, especially to the hypothalamus. Although, this is the most important pathway, there are many more redundant and independent pathways contributing to the thermoregulatory control.
Central autonomic thermoregulatory control depends on thermal inputs from the skin surface, peripheral tissues, the spinal cord, the hypothalamus, and most importantly the core temperature.
Efferent thermoregulation can be divided into behavioral and autonomic responses, whereas the behavior responses are by far the most powerful. Behavior responses included a wide range; for example, clothing, positioning, and even structural changes of buildings including isolation, heating, and air conditioning.
The primary autonomic thermoregulatory protection against hyperthermia includes pre-capillary vasodilatation and sweating, whereas the primary thermoregulatory protection against hypothermia includes arterio-venous shunt vasoconstriction, shivering, and non-shivering thermogenesis. Non-shivering thermogenesis is the activation of brown fat by thermogenin, but is mostly effective in infants, whereas it is not important in adults.
20.1.1 Thermoregulatory Response to Prevent Hypothermia
Prevention of hypothermia and initiation of the thermoregulatory responses are complex and consist mostly of vasoconstriction and shivering. The threshold for initiating vasoconstriction is only marginally below the sweating threshold (indicating that the ITR is usually only 0.2–0.4 ° C), whereas the threshold for initiating shivering is usually about 1 ° C below the vasoconstriction threshold.
Thermoregulatory vasoconstriction is mostly restricted to arterio-venous shunts, which are common in the acral regions including fingers and toes. These shunts are quite effective, as the range of the blood flow through these vessels can be increased by a factor of 10,000 (if maximally vasodilated) or can be reduced until nearly 0 (if maximally vasoconstricted) and subsequently directly influence the thermoregulatory vasoactive response of the entire extremities.
Shivering can increase the metabolic rate by a factor of 3 to 4 for about 3–4 h, but is finally limited by muscles tire. Although shivering is theoretically a sufficient thermoregulatory response, the effect is limited by the obligatory vasodilatation, which in turn is necessary to adequately perfuse and oxygenate the hyperactive muscles.
20.1.2 Thermoregulatory Response to Prevent Hyperthermia
Biochemical processes in humans are sensitive to hyperthermia and therefore prevention of hyperthermia by sweating and pre-capillary vasodilatation is important. Usually this is a synchronous process, as both responses are having the same triggering core temperature.
Sweating of up to 1 l is equal to dissipate more than ten times of their basal metabolic rate and is therefore usually quite effective.
20.2 The Model of Set Points
As the sweating and vasoconstriction threshold usually only differs marginally, some authors modeled the thermoregulatory system as a set point system. This model indicates, that the thermoregulatory system is ON or OFF. Despite the fact that the set point model is widely used, it does not consider the sequential activation of responses and it does not account for the effects of drugs such as anesthetics, ethanol, amphetamine, and buspirone on thermoregulatory control.
20.2.1 Heat-Loss During Anesthesia
Human tissue can be divided into a peripheral and a core thermal compartment, both attributing about 50% of the body mass. The peripheral thermal compartment represents mostly the extremities, whereas the core thermal compartment consists of the trunk and the head. The core thermal compartment is defined as the tissue that has a high and nearly constant temperature and is dominant in influencing the thermoregulatory responses. The temperature of the core thermal compartment is therefore tightly controlled. On the other hand, the temperature of the peripheral thermal compartment is significantly less narrowly defined. Or in other words, even a small change of the temperature of the core thermal compartment initiates a thermoregulatory response, whereas the temperature of the peripheral thermal compartment needs to change much more to initiate a thermoregulatory response. The peripheral thermal compartment contributes 20% to central thermoregulatory control. It is usually 2–4 ° C cooler than the central thermal compartment and is therefore acting as a thermal buffer, absorbing or dissipating heat as necessary to maintain core body normothermia.
As soon as a patient is transferred to the operating room (OR), several significant changes occur. The operating room is usually cooler and operative exposure causes hypothermia in the surgical patients. But, by far the most important thermoregulatory impairment is caused by anesthetics, which lead to a downward shift of the thermoregulatory thresholds. As a consequence, intraoperative hypothermia develops in 3 distinct phases (◘ Fig. 20.3).
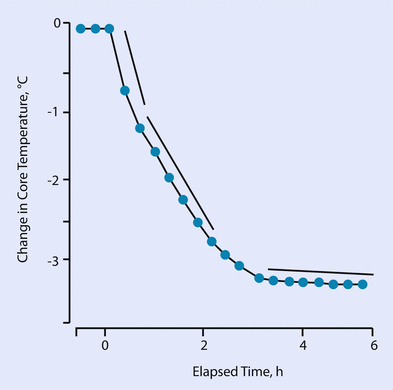

Fig. 20.3
Three phases of hypothermia during anesthesia
All anesthetics impair the thermoregulatory response and shift the vasoconstriction and the shivering threshold downwards (◘ Fig. 20.4). This shift is an obligatory function of the anesthetic drug, but is also affected by the actual concentration. A higher dosage of anesthetics therefore leads to a stronger influence (shift) of the thresholds. On average, during general anesthesia the vasoconstriction threshold is usually at around 34.5 ° C with commonly used drugs and doses.
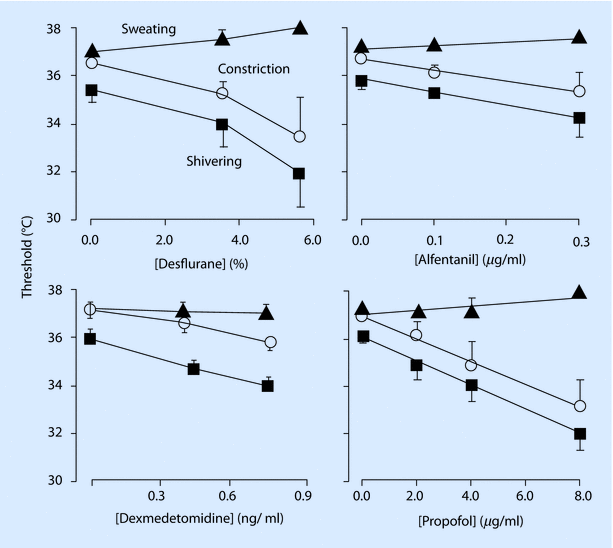

Fig. 20.4
Anesthesia impairs thermoregulation
Phase 1 (Redistribution Hypothermia)
During the first hour after induction of anesthesia, the core temperature rapidly drops. This drop is caused by balancing the temperature between the “cold” peripheral thermal compartment and the “warm” core thermal compartment. This period is therefore a shift of heat from the core to the peripheral thermal compartment, and is accelerated by the anesthesia-caused vasodilatation. Therefore this period is called “re-distribution.” This designation also makes clear that the actual amount of heat is not decreased (or at least minimally) during this period; the overall amount of heat is just distributed. Drop of temperature caused by re-distribution also occurs in actively warmed patients, as the amount of heat distribution exceeds the amount of external heat transfer. Only the so-called pre-warming (warming the peripheral thermal component before transferring the patient into the OR) might, to some limited extent, avoid re-distribution hypothermia.
Phase 2 (Slow Linear Decrease)
The period of re-distribution is typically followed by a period of slower, but linear reduction of core temperature. This period is characterized by an actual loss of heat to the environment by radiation and convection, while conduction and evaporation usually only marginally contributes.
The amount of decrease in core temperature during this period is a consequence of the gap between heat loss and metabolic heat production. Or in other words, the amount of heat loss exceeds the amount of heat production.
Phase 3 (Core Temperature Plateau)
As soon as the patient reaches a certain level of temperature, the core temperature does not further drop. This core-temperature plateau is a result of 1 out of 2 mechanisms or even a combination of both. The amount of metabolic heat production reaches the level of heat loss and therefore is balanced.
Depending on patient demographic factors, drugs used, and drug dosages, core temperature reaches the vasoconstriction threshold at which metabolically produced heat is constrained to the core thermal compartment and therefore core temperature ceases to drop. Nevertheless, body heat continues to decrease during this phase.
Once the thermoregulatory response is initiated, the arteriovenous shunts are vasoconstricted. Heat loss from the peripheral thermal compartment continues, but is limited by the decreased peripheral blood flow.
As vasoconstriction is usually effective, body core temperature rarely decreases enough to reach the shivering threshold, and most of the patients receive muscle relaxation agents. Shivering is extremely rare during general anesthesia. However, shivering is an important contributor to morbidity and mortality in the postoperative setting.
20.3 Effect of Drugs/Anesthesia on Temperature Regulation
Generally, all anesthetics including isoflurane, sevoflurane, inhaled anesthetic nitrous oxide, propofol, and opioids significantly influence the thermoregulatory regulation, by shifting the vasoconstriction and shivering thresholds downward. The extent of the shift is linear concentration-dependent for intravenous drugs, while it is disproportionate at higher concentrations for volatile anesthetics. On the other hand, sedatives such as midazolam do not influence the thermoregulatory responses, even if combined with clinical doses of opiods.
In the clinical setting and administration of usually used concentrations of drugs used for general anesthesia, the vasoconstriction threshold is shifted downwards to about 34.5 ° C. Once this threshold is reached, the thermoregulatory response is initiated and usually temperature does not further drop and does usually not reach the shivering threshold. The actual biochemical pathway of how anesthetics impair the vasoconstriction and shivering threshold remains currently unknown and is the target of ongoing biochemical studies.
General anesthesia is also responsible for a 30% reduction of the metabolic heat production.
Interestingly, the sweating threshold is marginally impaired. Therefore, the thermoregulatory response to hyperthermia during anesthesia is more or less equal to the response in awake patients.
20.3.1 Hypothermia During Regional Anesthesia
Consequences of Perioperative Hypothermia
Even mild perioperative hypothermia can cause a wide range of complications, including increased coagulopathy, increased risk of wound infections, prolonged drug metabolism and delayed recovery, and patient’s thermal discomfort.
The most important and best documented complication of perioperative hypothermia is coagulopathy, leading to substantially increased perioperative blood loss and need for transfusion. The impairment is based on reduced function of enzymes of the coagulation cascade, as well as decreased release of thromboxane A3, subsequently leading to reversible impairment of platelet aggregation. As a general rule, a drop of the core temperature by 1 ° C significantly increases the perioperative blood loss by about 20% and similarly the need for red blood cell transfusion.
Perioperative hypothermia increases the risk of wound infections, most likely by peripheral vasoconstriction, which is a direct consequence of hypothermia. Vasoconstriction leads to reduced perfusion of the wounded tissues and therefore reduces tissue oxygen partial pressure, which is the basis for oxidative killing of bacteria by neutrophils. In addition, perioperative hypothermia reduces systemic immune activation and motility of key cells, such as macrophages, and finally reduces tissue healing. Several years ago, the establishment of the Surgical Care Improvement Project (SCIP) required that patients either have a core temperature greater than 36 ° C at the end of surgery or that they were actively warmed in the intraoperative period. A recent study showed that patients in whom the SCIP guidelines were followed had higher core temperatures at the end of surgery as compared to those in whom the SCIP guidelines were not followed. Furthermore, the incidence of postoperative wound infections was lower in the SCIP patients.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






