CHAPTER 32 Paravertebral block
Clinical anatomy
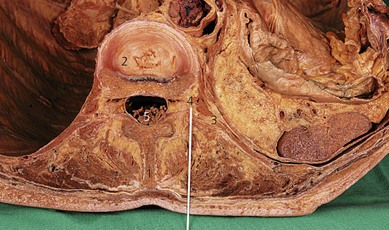
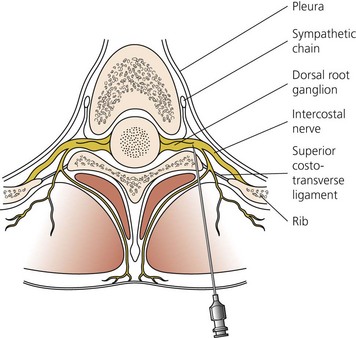
The paravertebral space is a wedge-shaped area on both sides of the vertebral column (Fig. 32.1). The boundaries of the space are: posteriorly, the superior costotransverse ligament; laterally, the posterior intercostal membrane; and anteriorly, the parietal pleura. At the base of the triangle (medially) is the posterolateral aspect of the vertebra, disc, and intervertebral foramen (Fig. 32.2). Contents of the paravertebral space include fatty tissue, intercostal vessels, spinal (intercostal) nerve, dorsal ramus, rami communicantes, and sympathetic chain (anteriorly). The paravertebral space is continuous medially with the epidural space and laterally with the intercostal space. The inferior limit of this space occurs at the origins of the psoas major muscle. The superior limit extends into the cervical region.
Surface anatomy
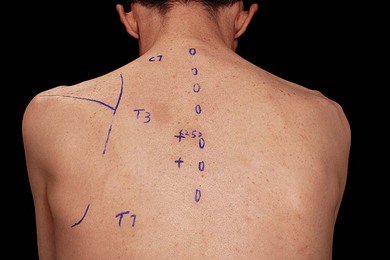
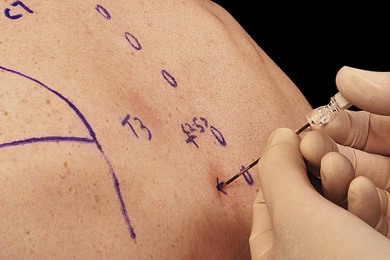
The main landmarks for the paravertebral block are the spinous and transverse processes. Identification of the appropriate vertebral level for blockade is facilitated by knowledge of dermatomes and anatomic landmarks that suggest vertebral level (Fig. 32.3). The spinous process of C7 (vertebrae prominens) is prominent and does not move with neck flexion. The spine and inferior angle of the scapula lie at the T3 and T7 vertebral levels, respectively.
Sonoanatomy
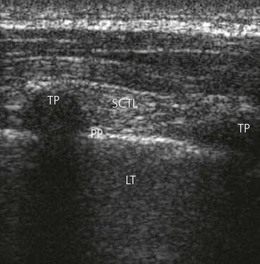
A linear array transducer is placed initially at a point 2.5 cm lateral to the tip of the spinous process in a vertical orientation, obtaining a sagittal paramedian view of the transverse processes (TP), superior costotransverse ligament (SCTL) and underlying pleura (Fig. 32.4). The transverse processes are seen as interrupted hyperechoic lines with loss of image beneath. The parietal pleura is identified as a bright structure running deep to the adjacent TPs and can be seen to slide with patient respirations. The superior costotransverse ligament, though less distinct, is seen as a collection of homogeneous linear echogenic bands alternating with echo-poor areas running from one TP to the next (Fig. 32.4).
Technique
Landmark-based approach
The needle insertion point is infiltrated with local anesthetic using a 25-G needle. An 18-G Tuohy needle is inserted perpendicular to the skin until contact is made with the transverse process (Fig. 32.5). This usually occurs 2–4 cm from the skin. The location of the transverse process is critical in the performance of this block. If this contact is not made, it is likely that the needle lies between the transverse processes. The needle should be withdrawn and redirected in a caudal or cephalic direction (Fig. 32.6). Once the transverse process is identified, the needle is withdrawn and redirected in a cephalic/caudad direction to ‘walk’ over/under the transverse process.
< div class='tao-gold-member'>
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree