CHAPTER 54
Oral Herpes Simplex
(Cold Sore, Fever Blister)
Presentation
Patients have swelling, burning, or soreness at the vermilion border of the lips followed by the appearance of clusters of small painful vesicles on an erythematous base (Figure 54-1). The vesicles then rupture to produce red, irregular ulcerations with swollen borders and crusting, which eventually heal without leaving a scar. These lesions can also occur on the hard palate or gingiva. Episodes may recur after exposure to sunlight or emotional or physical stress. The initial episode is usually the worst, with generalized malaise, low-grade fever, tender cervical adenopathy, and occasional exudative pharyngitis lasting 2 to 3 weeks. Recurrences are milder and shorter, with a prodrome of itching or burning at the lesion site. The painful ulcers that eventually form last 7 to 10 days.
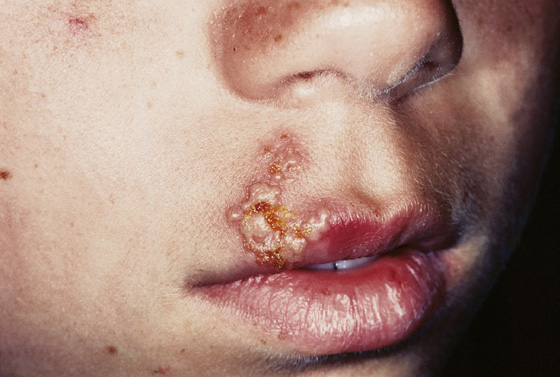
Figure 54-1 Herpes simplex labialis. (From Bolognia J, Jorizzo J, Rapini R: Dermatology. St Louis, 2003, Mosby.)
What To Do:
 When there is any doubt about the diagnosis, scrape the base of a vesicle (warn the patient that this hurts), smear it on a slide, stain it with Wright or Giemsa solution, and examine it for multinucleate giant cells (look for nuclear molding). This is called a Tzanck preparation and establishes the diagnosis of herpes. Alternatively, a swab can be sent for viral cultures, which may take days to grow. When performing a culture, the ulcer base should be swabbed vigorously, because herpes simplex virus (HSV) is an intracellular infection and adequate cell sampling is required.
When there is any doubt about the diagnosis, scrape the base of a vesicle (warn the patient that this hurts), smear it on a slide, stain it with Wright or Giemsa solution, and examine it for multinucleate giant cells (look for nuclear molding). This is called a Tzanck preparation and establishes the diagnosis of herpes. Alternatively, a swab can be sent for viral cultures, which may take days to grow. When performing a culture, the ulcer base should be swabbed vigorously, because herpes simplex virus (HSV) is an intracellular infection and adequate cell sampling is required.
 For minor symptoms, docosanol (Abreva), a topical cream available without a prescription, started within 12 hours of prodromal symptoms, decreases time to healing by about half a day.
For minor symptoms, docosanol (Abreva), a topical cream available without a prescription, started within 12 hours of prodromal symptoms, decreases time to healing by about half a day.
 For moderate-to-severe symptoms, prescribe penciclovir 1% cream (Denavir), 1.5 g. Have the patient apply it every 2 waking hours for 4 days. This treatment has been shown to hasten the resolution of lesions and pain in immunocompetent adults who have recurrent herpes simplex labialis, regardless of whether it is applied early or late in the course of the eruption. Started within 1 hour of papule appearance and applied every 2 hours while awake, it will decrease healing time by about 1 day.
For moderate-to-severe symptoms, prescribe penciclovir 1% cream (Denavir), 1.5 g. Have the patient apply it every 2 waking hours for 4 days. This treatment has been shown to hasten the resolution of lesions and pain in immunocompetent adults who have recurrent herpes simplex labialis, regardless of whether it is applied early or late in the course of the eruption. Started within 1 hour of papule appearance and applied every 2 hours while awake, it will decrease healing time by about 1 day.
 An alternative treatment is oral acyclovir (Zovirax), 400 mg 5 times per day for 7 days. This therapy reduces viral shedding, appearance of new lesions, and severity of pain and has been shown to decrease time to healing by 1 day. A much more convenient regimen with the same efficacy is a 1-day course of valacyclovir (Valtrex), to begin with the first symptoms of herpes labialis, 2 g q12h (2 doses). A much more costly regimen of famciclovir (Famvir), 500 mg bid for 7 days, can shorten the duration of symptoms by 2 days.
An alternative treatment is oral acyclovir (Zovirax), 400 mg 5 times per day for 7 days. This therapy reduces viral shedding, appearance of new lesions, and severity of pain and has been shown to decrease time to healing by 1 day. A much more convenient regimen with the same efficacy is a 1-day course of valacyclovir (Valtrex), to begin with the first symptoms of herpes labialis, 2 g q12h (2 doses). A much more costly regimen of famciclovir (Famvir), 500 mg bid for 7 days, can shorten the duration of symptoms by 2 days.
 Treat recurrences early, if possible during the prodrome or at the first sign of the first skin lesion.
Treat recurrences early, if possible during the prodrome or at the first sign of the first skin lesion.
 For comforting topical treatment, an equal mixture of kaolin-pectin (Kaopectate) and diphenhydramine (Benadryl) elixir can coat and dry the area and reduce pain. By adding an equal part of lidocaine (Xylocaine) 2% viscous solution, a mouthwash is created that can be swished in the mouth and then expectorated (do every 3 to 4 hours). Topical lip salves (Orabase, Zilactin, or Aphthasol) and application of cold compresses will also relieve the pain.
For comforting topical treatment, an equal mixture of kaolin-pectin (Kaopectate) and diphenhydramine (Benadryl) elixir can coat and dry the area and reduce pain. By adding an equal part of lidocaine (Xylocaine) 2% viscous solution, a mouthwash is created that can be swished in the mouth and then expectorated (do every 3 to 4 hours). Topical lip salves (Orabase, Zilactin, or Aphthasol) and application of cold compresses will also relieve the pain.
 Prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) or even narcotics and mild sedation for the most severe pain.
Prescribe nonsteroidal anti-inflammatory drugs (NSAIDs) or even narcotics and mild sedation for the most severe pain.
 Instruct the patient to keep lesions clean and to avoid touching them, which will prevent spreading the virus to the eyes, unaffected skin, and other people. Instruct the patient about the benefits of thorough hand washing. The patient should avoid kissing and other close contact while lesions are apparent.
Instruct the patient to keep lesions clean and to avoid touching them, which will prevent spreading the virus to the eyes, unaffected skin, and other people. Instruct the patient about the benefits of thorough hand washing. The patient should avoid kissing and other close contact while lesions are apparent.
 Inform the patient that oral herpes need not be related to genital herpes, that the vesicles and pain should resolve over about 2 weeks (barring superinfection), that they are infectious during this period (and perhaps at other times as well), and that the herpes simplex virus, residing in sensory ganglia, can be expected to cause recurrences from time to time (especially during periods of illness or stress). If the patient has more than six outbreaks a year, his primary care physician should consider prescribing acyclovir prophylactically.
Inform the patient that oral herpes need not be related to genital herpes, that the vesicles and pain should resolve over about 2 weeks (barring superinfection), that they are infectious during this period (and perhaps at other times as well), and that the herpes simplex virus, residing in sensory ganglia, can be expected to cause recurrences from time to time (especially during periods of illness or stress). If the patient has more than six outbreaks a year, his primary care physician should consider prescribing acyclovir prophylactically.
What Not To Do:
 Do not prescribe topical acyclovir or corticosteroids. They are ineffective. Do not use topical anesthetics on keratinized skin. They are effective only on oral mucosa and lip vermilion.
Do not prescribe topical acyclovir or corticosteroids. They are ineffective. Do not use topical anesthetics on keratinized skin. They are effective only on oral mucosa and lip vermilion.
Discussion
In most cases, herpes labialis is caused by herpes simplex virus type 1 (HSV-1). Primary herpes usually appears as gingivostomatitis (Figure 54-2), pharyngitis, or a combination of the two, whereas recurrent infections usually occur as intraoral or labial ulcers.
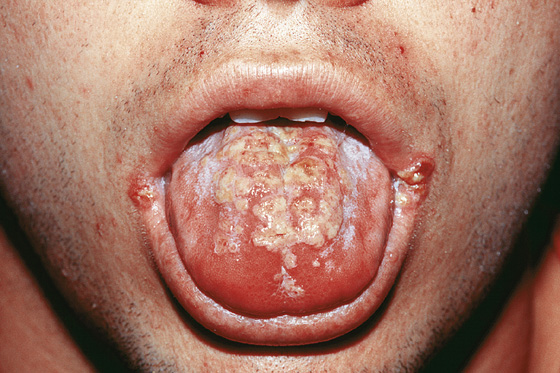
Figure 54-2 Acute herpes simplex gingivostomatitis in a young adult. (From White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
Primary infection is acquired mainly by direct person-to-person contact, such as kissing, wrestling, sexual intercourse, and inadvertent touching of lesions. Healthcare workers are at particular risk for finger or hand infections (whitlows). Primary infection tends to be a disease of childhood or young adulthood; is more severe than recurring episodes; is preceded by a temperature of up to 105° F, sore throat, and headache; and is followed by red, swollen gums that bleed easily.
This gingivostomatitis may need to be differentiated from herpangina, acute necrotizing ulcerative gingivitis, Stevens-Johnson syndrome, Behçet syndrome, and hand-foot-and-mouth disease. Herpangina is caused by Coxsackievirus group A and involves the posterior pharynx. The 1- to 4-mm intraoral vesicles do not extend beyond the soft palate and tonsillar pillars. Acute necrotizing ulcerative gingivitis, also known as Vincent angina or trench mouth, is bacterial in origin, causes characteristic blunting of the interdental gingival papillae, and responds rapidly to treatment with penicillin. Stevens-Johnson syndrome is a severe form of erythema multiforme. In this syndrome, there are characteristic lip lesions, the gingiva is only rarely affected, and there may be bull’s-eye skin lesions on the hands and feet. Behçet syndrome is thought to be an autoimmune response and is associated with genital ulcers and inflammatory ocular lesions. Hand-foot-and-mouth disease is also caused by Coxsackievirus group A and is associated with concurrent lesions of the palms and soles. Fifteen percent of these cases present with oral ulceration only, making differentiation from herpes difficult, but tender cervical adenopathy is uncommon in hand-foot-and-mouth disease. Recurrent aphthous stomatitis (RAS) (see Chapter 41) is usually located on the loose mucosal surfaces of lips or buccal mucosa of the cheeks.
Recurrent HSV infection most commonly occurs on the cutaneous lip and vermilion (herpes simplex labialis). Primary infection, unlike recurrent HSV, affects both the keratinized surfaces of the oral mucosa (such as the hard palate and gingiva, where the mucosa is tightly adherent to underlying bone) and the nonkeratinized mucosal surfaces.
Secondary recurrences of cold sores are due to reactivation of latent infection in the trigeminal ganglion. Possible causes of HSV-1 reactivation include stress, fever, menstruation, gastrointestinal disturbance, infection, fatigue, and exposure to cold or sunlight.
Home remedies for cold sores include application of ether, lecithin, lysine, and vitamin E. Because herpes is a self-limiting affliction, all of these therapies work, but in controlled studies, none has outperformed placebos (which also do very well).
Among immunocompetent patients, HSV infections are usually self limiting, and reactivation is rapidly controlled by the host’s immune system. In the immunocompromised person, however, the reactivated virus might continue to replicate, forming large, slowly expanding, long-lasting ulcerative lesions. More important, potentially fatal herpetic encephalitis or disseminated HSV infection is possible.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


