Fig. 4.1
Synchrony between patient’s inspiratory effort (bottom curve) and pressure support (upper curve). Paw airway pressure, Pdi transdiaphragmatic pressure, TiV ventilator’s inspiratory time, TiP patient’s inspiratory time, T sync time of synchrony, Insp or Exp Tr inspiratory or expiratory trigger
Neurally adjusted ventilatory assist (NAVA) is a new spontaneous ventilatory mode, first described in 1999 by Sinderby et al. [4], based on electric triggering and proportional ventilation. NAVA uses an esophageal catheter to collect the diaphragmatic electrical activity (EAdi) and to synchronize (in terms of timing and amount of pressure) the assistance to the patient’s inspiratory effort. There has been increasing use of NAVA, and a limited number of physiological studies have pointed out the clinical potential benefit of this new ventilatory mode. First, electric triggering, replacing pneumatic triggering, allows better synchrony between the patient and the ventilator. For example, in a subject with dynamic hyperinflation, synchronization of the pressure support with EAdi could increase patient–ventilator interaction (Fig. 4.2). In the same way, auto-triggering, which frequently occurs with leaks, could be resolved with electrical triggering.
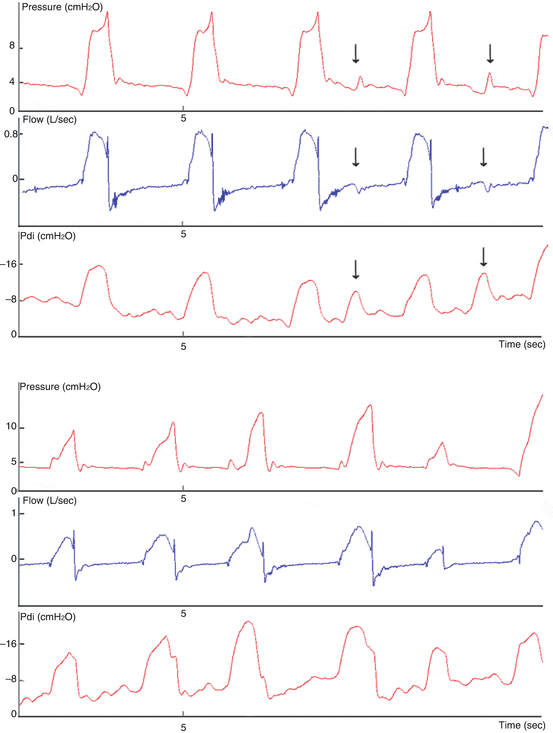

Fig. 4.2
Asynchronies with ineffective efforts. Pressure/time, flow/time and trans-diaphragmatic/time curves in noninvasive pressure support ventilation (upper figure) and noninvasive neurally adjusted ventilatory assist (bottom). Black arrows represent ineffective efforts
Studies have been published on the invasive application of NAVA mode and have shown better synchronization between the patient and the ventilator [5, 6]. Therefore, NAVA could be an interesting alternative to pressure support ventilation (PSV) in NIV.
4.2 Noninvasive NAVA Studies (Table 4.1)
Table 4.1
Characteristics of studies comparing NAVA to PSV in NIV
Year, author | No. of patients | Patients | PSV settings | Leaks | NAVA benefits |
|---|---|---|---|---|---|
2008, Camarota | 10 | ARF post extubation | Helmet®, NIV algorithm, all patients: PS 12 cmH2O, PEEP 10 cmH2O, expiratory trig 50 % | NAVA 43 % PSV 5 % | Decrease Inspiratory and expiratory trig delay, AI Increase time of synchrony |
2012, Piquilloud | 13 | 5 ARF 8 prophylactic post extubation 6 COPD | Oro-nasal mask, No NIV algorithm Optimized settings for each patients | NAVA 15 % PSV 14 % | Decrease inspiratory trig delay, AI, ineffective effort, delayed cycling, premature cycling |
2012, Schmidt | 17 | Prophylactic post extubation 4 COPD | Oro-nasal mask, with and without NIV algorithm, All patients PEEP 4cmH2O, expiratory trig 30 % | With NIV algorithm : NAVA 26 % PSV 13 % | Decrease inspiratory trig delay, AI, delayed cycling, premature cycling |
2013, Bertrand | 13 | ARF (5 post extubation, 7 pneumonia) No COPD | Oro-nasal mask, NIV algorithm, PEEP 5-10 cmH2O, expiratory trig 30 % | NAVA 13 % PSV 14 % | Decrease inspiratory trig delay, Ti excess, ineffective effort, delayed cycling, AI |
In 2008, Moerer et al. [7] studied seven healthy adult volunteers receiving NIV via the Helmet® device. They showed that, compared with pneumatically triggered NIV, neurally triggered NIV offers better patient-ventilator synchrony, better breathing comfort, and less trigger effort during increasing levels of PSV and respiratory rate.
Another clinical study by Cammarota et al. [8] used the Helmet® interface to compare NAVA versus PSV in 10 patients in acute respiratory failure (ARF). They also showed a better synchrony in NAVA mode compared with PSV. However, the severe asynchrony rate was relatively high in PSV mode (70–80 %), which was probably due to the interface [9].
In 2012, Piquilloud et al. [10] assessed 13 patients receiving NAVA and PSV with an oro-nasal face mask. Without using a NIV algorithm, but with an optimized setting in PSV, they reported a greater patient-ventilator interaction in NAVA compared with PSV, mainly due to the reduction of ineffective effort. More recently, Bertrand et al. [11] showed similar results on 13 patients with ARF (without chronic obstructive pulmonary disease (COPD)).
Schmidt et al. [12] particularly focused on the NIV algorithm. This dedicated software has been developed by manufacturers to take leaks into account and to automatically adjust the flow and the inspiratory trigger. They compared, in 17 patients receiving prophylactic post-extubation NIV, NAVA versus PSV with and without NIV algorithm. They found that NAVA with this software offers the best synchrony between the patient and the ventilator. Interestingly, NAVA without NIV-mode was more effective in reducing the asynchrony index (AI) than PSV with NIV algorithm.
4.3 Discussion
All of these physiologic studies are concordant and seem to indicate that NAVA increases patient-ventilator synchrony compared with PSV in NIV.
The use of neural triggering is particularly interesting in NIV. Leaks frequently occur, even with the NIV algorithm, and can alter a pneumatic inspiratory trigger. Leaks can generate auto-triggering, which is a main source of discomfort. Based on neural triggering, NAVA does not prevent leaks but allows the reduction of the inspiratory trigger delay and auto-triggering frequency [13]. Under NAVA, the trigger can also be pneumatic as the algorithm is first arrived, first served between pneumatic and neural triggering. However inspiratory trigger delays are important in patients with dynamic hyperinflation, and, in these patients, neural trigger starts before pneumatic trigger.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




