CHAPTER 19
Hordeolum
(Stye)
Presentation
The patient complains of redness, nodular swelling, and pain in the eyelid, perhaps at the base of an eyelash (stye or external hordeolum) or deep within the lid (meibomitis, meibomianitis, or internal hordeolum, which is best appreciated with the lid everted) and perhaps with conjunctivitis and purulent drainage. In some cases, the complaint may be that of generalized edema and erythema of the lid (cellulitis). There may be a history of similar problems.
Examination most commonly reveals a localized tender area of swelling, often with a pointing eruption on either the internal or the external side of the eyelid (Figure 19-1).
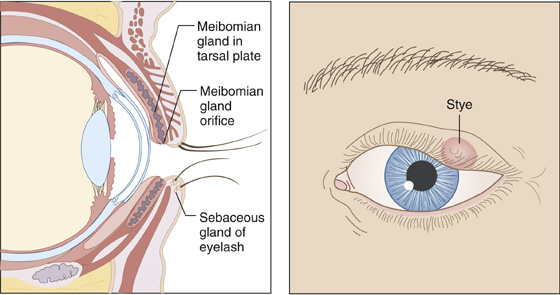
Figure 19-1 Stye of sebaceous gland (gland of Zeiss).
What To Do:
 Examine the eye, including assessment of best-corrected visual acuity and inversion of the lids (see Chapter 17 for technique). No corneal or intraocular disease should be found.
Examine the eye, including assessment of best-corrected visual acuity and inversion of the lids (see Chapter 17 for technique). No corneal or intraocular disease should be found.
 Show the patient how to instill antibiotic drops or ointment (e.g., polymyxin B/trimethoprim [Polytrim], 10 mL, 1 drop q2-6h, or polymyxin B/bacitracin, 3.5 g, 1- to 2-cm ribbon lower lid qid) into the lower conjunctival sac q2-6h.
Show the patient how to instill antibiotic drops or ointment (e.g., polymyxin B/trimethoprim [Polytrim], 10 mL, 1 drop q2-6h, or polymyxin B/bacitracin, 3.5 g, 1- to 2-cm ribbon lower lid qid) into the lower conjunctival sac q2-6h.
 Instruct her to apply warm tap water compresses for approximately 15 minutes qid.
Instruct her to apply warm tap water compresses for approximately 15 minutes qid.
 If there are signs of spreading infection (e.g., tender lid edema and erythema with or without preauricular lymphadenitis), provide appropriate systemic antibiotic coverage (e.g., cephalexin [Keflex], 500 mg q6h; dicloxacillin [Dynapen], 500 mg q6h; or erythromycin, 333 mg tid for 7 days). Consider coverage for methicillin-resistant Staphylococcus aureus (MRSA) if it is prevalent in your community (e.g., doxycycline, 100 mg bid for 7 days).
If there are signs of spreading infection (e.g., tender lid edema and erythema with or without preauricular lymphadenitis), provide appropriate systemic antibiotic coverage (e.g., cephalexin [Keflex], 500 mg q6h; dicloxacillin [Dynapen], 500 mg q6h; or erythromycin, 333 mg tid for 7 days). Consider coverage for methicillin-resistant Staphylococcus aureus (MRSA) if it is prevalent in your community (e.g., doxycycline, 100 mg bid for 7 days).
 Instruct the patient to consult an ophthalmologist or return to the ED or clinic if the problem is not clearly resolving in 2 days or if it gets any worse. Tell her not to squeeze the stye, because this may spread the infection into surrounding tissues. Also let her know that frequent recurrences are common.
Instruct the patient to consult an ophthalmologist or return to the ED or clinic if the problem is not clearly resolving in 2 days or if it gets any worse. Tell her not to squeeze the stye, because this may spread the infection into surrounding tissues. Also let her know that frequent recurrences are common.
 If the abscess does not spontaneously drain or resolve in 2 days and if it is pointing, it may be incised with the tip of a No. 11 scalpel blade or 18-gauge needle. Drainage should be accomplished by making a small puncture at the point of maximum tissue thinning, where underlying pus is visible. Again, instruct the patient to continue using warm compresses and then to consult an ophthalmologist or return to the ED or clinic if the problem is not clearly resolving in 2 days or if it gets any worse.
If the abscess does not spontaneously drain or resolve in 2 days and if it is pointing, it may be incised with the tip of a No. 11 scalpel blade or 18-gauge needle. Drainage should be accomplished by making a small puncture at the point of maximum tissue thinning, where underlying pus is visible. Again, instruct the patient to continue using warm compresses and then to consult an ophthalmologist or return to the ED or clinic if the problem is not clearly resolving in 2 days or if it gets any worse.
What Not To Do:
 Do not overlook orbital or periorbital cellulitis, which is a severe infection and requires aggressive systemic antibiotic treatment.
Do not overlook orbital or periorbital cellulitis, which is a severe infection and requires aggressive systemic antibiotic treatment.
 Do not culture drainage from a stye unless MRSA is suspected. Eye cultures are usually of little clinical value, and they are costly.
Do not culture drainage from a stye unless MRSA is suspected. Eye cultures are usually of little clinical value, and they are costly.
 Do not make deep incisions along the lid or eyelash margins. This can lead to lid deformity or abnormal eyelash growth.
Do not make deep incisions along the lid or eyelash margins. This can lead to lid deformity or abnormal eyelash growth.
Discussion
The terminology describing the two types of hordeolum has become confusing. Meibomian glands run vertically within the tarsal plate, open at tiny puncta along the lid margin, and secrete oil to coat the tear film. The glands of Zeiss and Moll are the sebaceous glands opening into the follicles of the eyelashes. Either type of gland can become occluded and superinfected (S. aureus is the causative pathogen in 90% to 95% of cases), producing meibomianitis (internal hordeolum) or a stye (external hordeolum). The immediate care for both acute infections is the same.
A chronic granuloma of the meibomian gland is called a chalazion; it is painless, will not drain, and requires excision.
Most hordeola eventually point and drain by themselves. Therefore warm soaks (qid for 15 minutes) are the mainstays of treatment. When lesions are pointing, surgical drainage speeds the healing process.
If the patient appears to have diffuse cellulitis of the lid, fever, and/or painful or restricted extraocular movements, posterior extension (creating an orbital cellulitis) should be suspected. Such cases must be managed aggressively with IV antibiotics and immediate subspecialty consultation.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree



