Introduction
Hidradenitis suppurativa (HS) is a chronic, relapsing inflammatory disease that involves the intertriginous regions such as the axillae, groin, inframammary, and anogenital regions [1]. HS is typified by chronicity, and patient and provider frustration. HS is believed to arise due to a defect in the terminal follicular epithelium. The initial process is abnormal cornification of the follicular infundibulum with follicular occlusion by keratin with subsequent active folliculitis. Secondary destruction of skin adnexae and the subcutis then develops. Abscesses form which may resolve spontaneously or progress into chronic cutaneous or subcutaneous tunneling (sinus tract formation) [2].
The French physician Alfred Velpeau first described HS in 1839 and reported it as an inflammatory process with superficial abscess formation affecting the axillary, mammary, and perianal regions [3]. The French surgeon Aristide Verneuil was the first to theorize a connection between HS and apocrine glands, naming the condition hidrosadenite phlegmoneuse [4, 5]. The term hidradeni-tis suppurativa is derived from “hidros” (sweat), “adeno” (gland), “itis” (inflammation), and “suppurativa” (pus forming).
Hidradenitis suppurativa has subsequently become classified as a member of the follicular occlusion tetrad, along with acne conglobata and dissecting cellulitis of the scalp and pilonidal sinus [6, 7, 8]. In 1975, the follicular occlusion tetrad was formed by the addition of pilonidal sinus [8]. Plewig and Steger introduced the term acne inversa in 1989 based on overwhelming data supporting the follicular origin of the disorder [9].
Of historical note: Karl Marx was known to have suffered from an incapacitating skin disease. Recent review of his correspondence detailed lesions called “furuncles,” “boils,” and “carbuncles” that were persistent, recurrent, destructive, and site-specific consistent with HS [10]. It is hypothesized that the mental effects of this disabling disease may well have influenced Marx’s work.
Hidradenitis suppurativa is probably more common than is typically realized. The disease is frequently ignored or missed, leadingto both patient’s and health care provider’s frustration [11]. The disease prevalence has been estimated at 1:100, 1:300, or 1:600, and as high as 4.1% based on objective findings in a young adult population [12–14].
There is no consensus regarding a relationship between HS and ethnicity. Some authors have suggested an increased frequency in African Americans [15–18], but others report no racial predilection [19]. The disorder is more common in women, with the female/male ratio ranging from 2:1 to 5:1 in most published series. The mean age of onset for men is 31.7 years and for women it is 26.4 years. Genitofemoral lesions are more commonly found in women, whereas the prevalence of axillary lesions does not differ significantly with gender [12].
Obesity tends to be more prevalent in patients with HS [20], although this has not been demonstrated in all studies [21].Itseems mostlikely that obesityisasecondary factor, aggravatingthe disease through mechanical trauma at skin folds rather than being a primary cause [22].
There is a high incidence of active smoking among HS patients compared with controls [23, 24]. No definitive causal mechanism has been determined; however, altered chemotaxis of polymorphic neutrophils might play a part [11].
Evidence from some families indicates transmission of HS occurs with single gene dominant inheritance [13, 25– 27]. A recent genome-wide scan in a four-generation Chinese family mapped the chromosome location locus at chromosome 1p21.1–1q25.3 [28]. The female predominance found in most studies does argue against a purely autosomal dominant inheritance, leading one to consider the possibility of hormonal influences on gene expression or the possibility of an X-linked chromosomal disease [11].
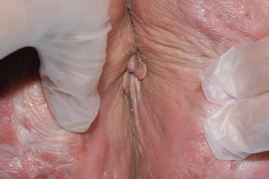
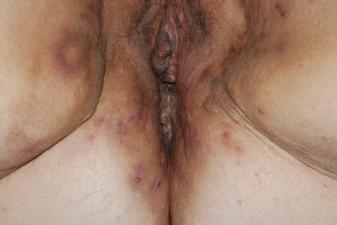
Figure 10.2 Hidradenitis suppurativa on the perianal tissue.
Hidradenitis suppurativa has been considered an androgen-dependent disorder [29]. Fifty percent of women report a flare-up before or during menses. Symptomatic improvement during pregnancy with postpar-tum flares is also often described. Numerous theories relating androgens to the pathogenesis of HS have been put forward, but none have achieved acceptance. Barth and Kealy studied apocrine glands, but they concluded that defects in these glands are not the primary cause of HS [30].
The diagnosis of HS is primarily based on the clinical presentation. There are currently no recommended diagnostic tests. A biopsy is not required, unless used to exclude another diagnosis. A thorough history and physical exam is sufficient and should elicit the three main features of HS [31]:
1 Typical lesions (painful deep subcutaneous nodules, fibrotic sinus tracts).
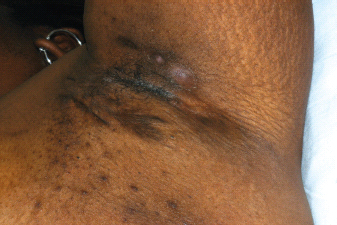
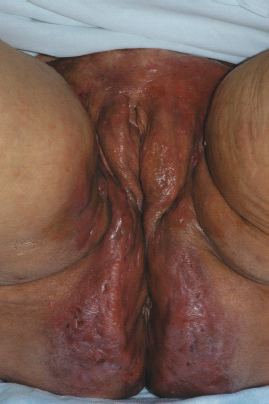
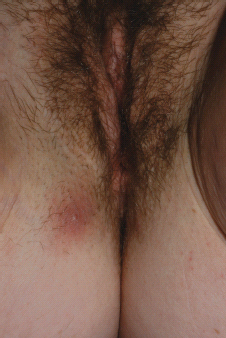
2 Typical locations (axilla, perianal, and genital regions); Figures 10.1–10.3.
3 Relapses and chronicity.
Two methods (Hurley and Sartorius) currently exist to evaluate disease severity and guide treatment. Hurley clinical staging [32] classifies patients in overall groups with early-stage disease benefiting from medical therapy and higher-stage disease requiring surgical intervention (Figures 10.4–10.6).
Stage I: One or more abscesses with no sinus tract or cicatrization.
StageII: One or more wildly separated recurrent abscesses with a tract and scarring.
Stage III: Multiple interconnected tracts and abscesses throughout the entire affected area.
Sartorius [33] developed a scoring system for monitoring of disease severity in individual patients. A total score as well as scores of selected regions chosen for surgical or other intervention can be calculated and followed over time.
1 Anatomical region involved (three points per region involved).
2 Number and scores of lesions (points per lesion of all regions involved: nodules 2; fistulas 4; scars 1; others 1).
3 The longest distance between two relevant lesions (<5 cm, 2 points; <10 cm, 4 points; >10 cm, 8 points).
4 Are all lesions clearly separated by normal skin? (Yes, 0 points; No, 6 points).
The differential diagnosis includes other follicular infections such as carbuncles/furuncles or pilonidal cysts. Infected Bartholin’s or epidermoid cysts and other chronic scarring conditions, such as tuberculosis and granuloma inguinale, may also be considered in HS. Crohn’s disease may present with ulcerations, fistulae, and lesions in the perianal region, and must be excluded in patients with digestive symptoms. HS rarely involves the anal canal and does not track above the dentate line. An association between Crohn’s disease and HS has been reported [34–37]. Squamous cell carcinomas may arise infrequently in HS, further emphasizing the need for close surveillance and biopsies of any suspicious lesions [38, 39]. Any excised tissue should be sent for pathology.
Unfortunately, HS is not a disease well known to health care providers, and patients may be referred to many specialists beforeadiagnosisis made andtheproper treatment initiated. One series of 164 patients reported a mean delay in diagnosis of 7 years [40]. This can only compound the frustration and distress experienced by patients suffering from HS, and contributes to the negative impact on their quality of life.
Figure 10.5 Stage II hidradenitis suppurativa with separated recurrent abscess with a tract and scarring.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree