Fig. 34.1
Growth in the elderly population in the USA (Source: Social Security Administration, Office of the Chief Actuary. Note: Projections based on intermediate assumptions of the 2003 Annual Report of the Board of Trustees of the Federal Old–Age and Survivors Insurance and the Federal Disability Insurance Trust Funds)
The USA has seen a rapid growth in its elderly population during the twentieth century. There has been an 11-fold increase in the number of Americans age ≥65 years, with 35 million in 2000 vs. 3.1 million in 1900. For the same years, the ratio of elderly to the total population jumped from 1/25 to 1/8. The trend is guaranteed to continue in the coming century as the “baby-boom” generation grows older. Between 1990 and 2020, those aged 65–74 is projected to grow 74 %.
The elderly population explosion is a result of an impressive increase in life expectancy. When the nation was founded, the average American could expect to live to the age of 35. Life expectancy at birth had increased to 47.3 by 1900, and the average American born in 2000 can expect to live to the age of 77.
The “oldest old” (those age ≥85) are the most rapidly growing elderly age group (Fig. 34.2). Between 1960 and 1994, they increased 274 % (three million, 10 % of elderly, 1 % of population) compared to 100 % increase in the elderly and a 45 % increase in the entire population. It is expected the oldest old will number 19 million in 2050, comprising 24 % of the elderly and 5 % of all Americans.
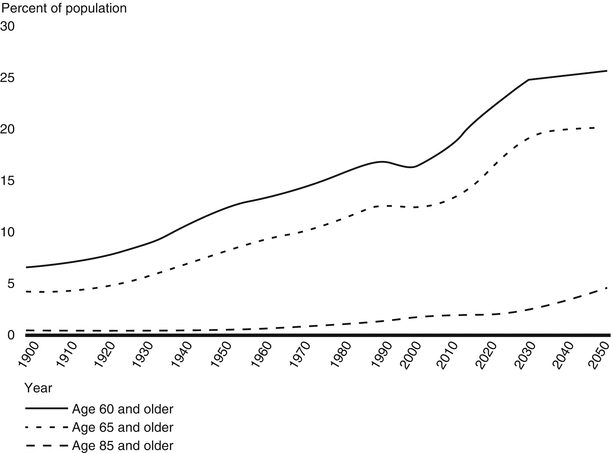

Fig. 34.2
Growth in elderly vs. super-elderly population in the USA (Source: GAO analysis of US Census Bureau data by the Administration on Aging)
Critical Care Resource Use in the Elderly
Elderly patients (age >65 years) currently comprise 42–52 % of ICU admissions and account for almost 60 % of all ICU days in the USA [3]. In addition, 40 % of Medicare patients who die are admitted to the ICU during their terminal illness, with decedents accounting for 25 % of all Medicare expenditures. Thus, a significant amount of critical care resources are used at the end of life caring for elderly patients.
Current estimates predict that by 2050, the percentage of the population older than 80 years will double, which will lead to an increasing demand for health-care resources, including intensive care [4]. In a large multicenter cohort study of 57 ICUs across New Zealand and Australia, elderly (age ≥80 years) patient ICU admissions increased roughly 6 % per year between 2000 and 2005 and represented approximately 14 % of total admissions in 2005 [5].
Although increasing numbers of very elderly patients are requiring ICU care, few large sample studies have investigated ICU admission of very elderly patients. An observational cohort study from 15 hospitals in France examined interhospital variability of ICU admission rates from the emergency department and its association with elderly patients’ (age >80) outcomes over a 1-year period. Rates of patients deemed eligible for ICU admission ranged from 5.6 to 38.8 % across the participating centers, and this variability persisted after adjustment for patients’ characteristics. Despite this variability, no association between level of ICU eligibility and either in-hospital death or 6-month death or functional deterioration was identified. In France, the likelihood that an elderly person will be admitted to an ICU varies widely from one hospital to another, and influence of ICU admission on elderly patients’ outcome remains unclear [6].
Critical Care Outcomes in the Elderly
ICU mortality for those older than 65 years (36.8 %) is significantly higher when compared to that for those less than 45 years old (14.8 %). In addition, elderly patients discharged from the ICU to subacute facilities have a higher mortality rate than similar patients discharged home.
In a study of 484 patients admitted to medical, surgical, and coronary ICUs in a large urban teaching hospital, it was determined that one-third (1/3) of adults older than 64 years admitted to the ICU die within 6 months of hospital discharge. Independent predictors of death at 6 months were number of days during the 30 days before hospitalization that the patient felt their “physical health was not good” on the health-related quality of life survey [odds ratio = 1.08; confidence interval 1.04–1.12], a higher Acute Physiology and Chronic Health Evaluation II score [OR 1.09; 95 % CI 1.06–1.12], and chronic pulmonary disease as a comorbidity [OR 2.22; 95 % CI 1.04–4.78]. Among survivors at 6 months, health-related quality of life had significantly worsened over time in the oldest patients but improved in the youngest survivors [7].
A larger study has confirmed similar findings [8]. A matched, retrospective cohort study was conducted using a 5 % sample of Medicare beneficiaries older than 65 years. There were 35,308 ICU patients who survived to hospital discharge. The ICU survivors had a higher 3-year mortality (39.5 %; n = 13,950) than hospital controls (34.5 %; n = 12,173) (adjusted hazard ratio [AHR], 1.07 [95 % CI, 1.–1.10]; p < .001) and general controls (14.9 %; n = 5266) (AHR, 2.39 [95 % CI, 2.31–2.48]; p < .001).
Those receiving mechanical ventilation had substantially increased mortality (57.6 % [1234 ICU survivors] vs. 32.8 % [703 hospital controls]; AHR, 1.56 [95 % CI, 1.40–1.73]), with risk concentrated in the 6 months after the quarter of hospital discharge (6-month mortality, 30.1 % (n = 645) for those receiving mechanical ventilation vs. 9.6 % (n = 206) for hospital controls; AHR, 2.26 [95 % CI, 1.90–2.69]). Discharge to a skilled care facility for ICU survivors (33.0 %; n = 11,634) and hospital controls (26.4 %; n = 9328) also was associated with high 6-month mortality (24.1 % for ICU survivors and hospital controls discharged to a skilled care facility vs. 7.5 % for ICU survivors and hospital controls discharged home; AHR, 2.62 [95 % CI, 2.50–2.74]; p < .001 for ICU survivors and hospital controls combined).
This study confirmed that there is a large US population of elderly individuals who survive the ICU stay to hospital discharge but who have a high mortality over the subsequent years in excess of that seen in comparable controls. The risk is concentrated early after hospital discharge among those who require mechanical ventilation.
Frailty and ICU Outcomes in the Elderly
It is important to consider not only age but functional status in elderly patients. The scoring systems currently used do not precisely assess comorbidity and prehospital functional status or disability. Frailty has recently been established as a concept to assess loss of physiological reserves and an inability to maintain homeostasis to combat disease or injury. Common signs include fatigue, weight loss, weakness, low activity level, slow motor performance, and cognitive loss. Frailty can be assessed by different scoring systems (frailty phenotype, clinical frailty score, Katz Index of Independence in activities of daily living). Recent studies have confirmed that frailty is a frequent occurrence in elderly ICU patients and is independently associated with increased ICU and 6-month mortality. Furthermore, frailty scales predict outcome more effectively than the commonly used ICU illness scores.
Planned Surgical Versus Medical and Unplanned Surgical ICU Admissions
Elderly patients requiring ICU admission after planned surgery have better long-term outcomes compared to elderly medical and unplanned surgical ICU admissions. This is likely related to the ability to optimize the elderly patient physiologically for surgical intervention.
Guidelines were recently published for optimal preoperative assessment of the geriatric surgical patient from the American College of Surgeons National Surgical Quality Improvement Program and the American Geriatrics Society. The guidelines recommend and specify 13 key issues of preoperative care for the elderly: cognitive impairment and dementia; decision-making capacity; postoperative delirium; alcohol and substance abuse; cardiac evaluation; pulmonary evaluation; functional status, mobility, and fall risk; frailty; nutritional status; medication management; patient counseling; preoperative testing; and patient-family and social support system [9].
Outcome Measures: Mortality Versus Long-Term Functional Outcomes
ICU survival may not be the most appropriate endpoint when evaluating the role of critical care, particularly in the elderly. The goal of critical care medicine is to restore patients to a level of function similar to that of their preadmission status. A practical goal, therefore, is to define the most accurate criteria for identification of elderly ICU patients most likely to benefit from ICU care regardless of age.
A study of long-term outcome in medical patients aged 80 or over following admission to an ICU documented a hospital mortality rate of 55 % with only 47 % of the ICU patients still alive at 2 years. Interestingly, factors independently associated with mortality were SAPS II score at ICU admission and the McCabe score. Conversely, functional status prior to admission (as assessed by Knaus or Karnofsky scores) was not associated with long-term mortality. In long-term survivors, SF-36 physical function scores were poor, but scores for pain, emotional well-being, and social function were not much affected. In addition, the group that was discharged had increased mortality compared to the general population of the same age not admitted to an ICU [10].
A prospective cohort study from a 10-bed, medical-surgical ICU in a 460-bed, tertiary, university hospital in France examined the outcome, functional autonomy, and quality of life of elderly patients (≥70 years, n = 75) hospitalized for more than 30 days in an ICU. The survival rate was 67 % in the ICU and 47% survived to discharge. Independence in activities of daily living was decreased significantly after the ICU stay, except for feeding. However, most patients remained independent (class A of the activities of daily living index) with the possibility of going home. Perceived quality of life scores remained good, even if the patients estimated a decrease in their quality of life for health and memory. Return to society appeared promising regarding patient self-respect and happiness with life. The estimated cost per survivor was of 55,272 EUR ($60,246 US). This study suggested that persistent high levels of ICU therapeutic intensity were associated with a reasonable hospital survival in elderly patients experiencing prolonged mechanical ventilatory support. These patients presented a moderate disability that influenced somewhat their perceived quality of life. These results are sufficient to justify prolonged ICU stays for elderly patients [11].
Elderly Critical Care Trauma Outcome and Resource Utilization
Elderly patients are at high risk for mortality after injury. According to 2010 National Vital Statistics Report preliminary data, accidental death was the ninth leading cause of death for those greater than 65 years old, with 15 % of these accidental deaths from motor vehicle collisions. Elderly trauma patients have increased mortality risk compared to younger trauma patients in all injury severity categories (Fig. 34.3).
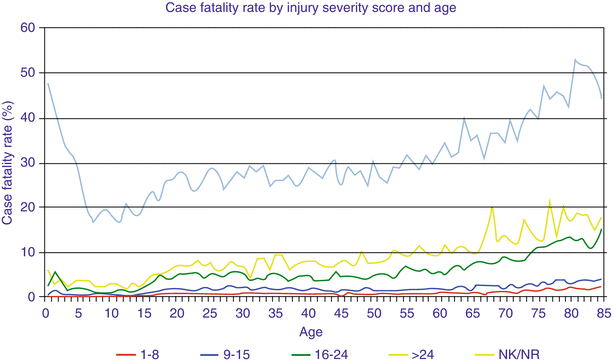

Fig. 34.3
Data from National Trauma Data Bank, Case Fatality Rate by Injury Severity Score and Age (American College of Surgeons NTDB)
A review of 26,237 blunt trauma patients admitted to all trauma centers (n = 26) in one state over 24 months confirmed that elderly (age ≥65 years, n = 7117) patients had significantly higher mortality rates than younger (age <65 years) trauma patients after stratification by Injury Severity Score (ISS), revised trauma score, and other preexisting comorbidities. Age greater than 65 years was associated with a two- to threefold increased mortality risk in mild (ISS <15, 3.2 % vs. 0.4 %; <0.001), moderate (ISS 15–29, 19.7 % vs. 5.4 %; <0.001), and severe traumatic injury (ISS ≥30, 47.8 % vs. 21.7 %; <0.001) compared with patients younger than 65 years. Logistic regression analysis confirmed that elderly patients had a nearly twofold increased mortality risk (OR 1.87; confidence interval, 1.60–2.18; <0.001). Elderly patients also had significantly longer hospital LOS after stratifying for severity of injury by ISS (1.9 fewer days in the age 18–45 group, 0.89 fewer days in the age 46–64 group compared with the age over 64 group). Mortality rates were higher for men than for women only in the ISS <15 (4.4 % vs. 2.6 %, <0.001) and ISS 15–29 (21.7 % vs. 17.6 %, = 0.031) groups. ICU LOS was significantly shorter in elderly patients with ISS ≥30. This study confirmed age as an independent predictor of mortality in trauma after stratification for injury severity in this largest study of elderly trauma patients to date. Interestingly, elderly patients with severe injury (ISS >30) had decreased ICU resource use secondary to associated increased mortality rates [12].
In a single-center Level I trauma center study, it was confirmed that age alone was associated with increased odds of being admitted to the hospital, independent of injury severity and other physiologic parameters. A total of 451 (8.68 %) elderly patients were 65 years or older; 62 % of the total population was admitted. Elderly patients had a significantly higher hospital admission rate (86.7 %; p < 0.001). Multivariate analysis showed that age over 64 years (OR 3.76), head injury (OR 5.3), ISS (OR 17.5), Glasgow Coma Scale score on arrival (OR 0.753), and initial systolic blood pressure (OR 0.987) were significant independent factors predictive of hospital admission (p < 0.001). Elderly patients were also admitted to the ICU at a higher rate (60.9 % vs. 38.5 %, p < 0.001) and were more likely to remain there for a longer period of time. Greater than 75 % of the elderly patients stayed for over 3 days. This has implications for trauma centers that see a significant proportion of geriatric trauma patients and for trauma systems that must prepare for the “aging of America” [13].
Trauma benchmarking efforts benefit from development of a geriatric-specific model for risk-adjusted analyses of trauma center outcomes. A total of 57,973 records of elderly patients (age older than 65 years) with data from the National Trauma Data Bank (NTDB) and the National Sample Project were used to construct a multivariable logistic regression model, which was compared with the American College of Surgeons Committee on Trauma’s Trauma Quality Improvement Project’s (TQIP) existing model. Additional analyses were performed to further objectively quantify the physiologic differences between geriatric patients and their younger counterparts. The geriatric-specific and TQIP mortality models shared several covariates: age, ISS, motor component of the Glasgow Coma Scale, and systolic blood pressure. This new model additionally used temperature and the presence of mechanical ventilation. This geriatric-specific regression model compared with the TQIP approximation (0.85 vs. 0.77; p = 0.048). Spline analyses demonstrated that elderly patients appear to be less likely to tolerate relative hypotension with higher observed mortality at initial systolic blood pressures of 90–130 mmHg. Although the TQIP model includes a single-age component, these data suggest that each variable needs to be adjusted for age to more accurately predict mortality in the elderly. Clearly, a separate geriatric model for predicting outcomes is not only warranted but necessary [14].
Super-Elderly Trauma Patients
The fastest-growing segment of the population is the “super-elderly,” i.e., those greater than 85 years old. It is projected that those 85 years and older will double from 2000 to 2030. By 2050 this age group will be five times larger than in 2000 and will make up a little over 4 % of the total population. Despite this growth there is little information of trauma outcomes in this group.
In a retrospective cohort study from a countywide trauma registry, overall mortality of very elderly trauma patients (n = 455, mean age 85.9 years, range 80–101) was 10 %, with head injury and injury severity as independent risk factors for increased mortality. They also confirmed that very elderly patients admitted to trauma centers (Levels I and II) had better outcomes than nontrauma centers, especially in the high injury severity (ISS 21–45) cohort (mortality 56 % vs. 8 % survival; p < 0.01) [15].
Another study compared the post-injury outcomes of super-elderly patients (n = 422, age ≥80 years) to elderly patients (n = 898, age 60–79 years) treated at a Level I trauma center after adjustment for gender, mechanism of injury, Glasgow Coma Scale, ISS, and admission vital signs. Super-elderly patients had significantly higher risk-adjusted in-hospital mortality compared with elderly patients [13.4 % vs. 7.7 %, adjusted OR 1.94 (95 % CI 1.14, 3.31), p = 0.015]. Of patients surviving hospitalization, super-elderly patients experienced shorter ICU and hospital length of stay but were more likely to require discharge to another level of care, defined as nursing facility, acute rehabilitation facility, or long-term acute care facility (AOR 3.78, CI 2.75–5.28, p < 0.0005). Importantly, super-elderly patients were more likely than elderly patients to die during hospitalization as a result of withdrawal of medical support (9.5 % vs. 5.5 %, p = 0.007) [16].
Performance Improvement in Elderly Trauma
Given the high mortality rate for elderly trauma patients, attention to modifiable risk factors in establishing a performance improvement program is imperative. Delays in recognizing the special needs of older trauma patients may result in suboptimal care.
We have reported our performance improvement efforts in elderly trauma care. In 2004 (baseline data), the in-hospital mortality rate for the most severely injured trauma patients (ISS >24) at our trauma center was 30 %, consistent with the reported mortality rate from the NTDB for patients with this severity of injury. Over 5 years, our mortality rate decreased significantly for severely injured patients with an ISS > 24–18 %, representing a 12 % absolute reduction in mortality (p = 0.011). During the same 5-year time period, the proportion of elderly patients cared for at our trauma center increased from 23.5 % in 2004 to 30.6 % in 2008 (p = 0.0002), while there was a significant reduction in mortality over this time period. Class I trauma activations increased significantly from 5.5 % in 2004 to 15.5 % in 2008. A greater percentage of patients were admitted to the ICU (25.8 % vs. 30.4 %) with no difference in the mechanism of injury throughout the 5 years. Trauma Quality Improvement Program (TQIP) data for our institution confirmed improved trauma outcomes with observed-to-expected ratio and 95 % confidence intervals of 0.64 (0.42–0.86) for all patients, 0.54 (0.15–0.91) for blunt single-system patients, and 0.78 (0.51–1.06) for multisystem patients [17].
One method to improve trauma geriatric outcome is to establish geriatric-specific triage criteria to identify trauma center care in injured older adults. It has been established that standard adult EMS triage guidelines provide poor sensitivity in older adults and that geriatric trauma triage guidelines significantly improve sensitivity. A recent study has confirmed that trauma center care improves outcomes even in older, minimally injured patients and proposed that an age threshold (age ≥ 70 years) should be considered as a criterion for trauma center triage.
Another method to improve trauma geriatric outcome is to establish geriatric trauma patient care protocols. These protocols are created from evidence-based guidelines that serve to reduce variation in care. Patient care protocols have been found to positively impact patient care with reduced duration of mechanical ventilation, shorter LOS in the ICU and shorter overall hospitalization time, reduced mortality, and reduced health-care costs.
A single-institution study documented that use of new protocols helped guide practical changes in geriatric trauma care that resulted in a 32 % decrease in LOS for elderly trauma patients. The four protocols implemented were a VAP bundle, massive transfusion protocol, reversal of coagulopathy protocol, and rib fracture protocol [18].
Some trauma centers have created a dedicated geriatric trauma service. This concept was studied in a Level II trauma center which documented a significant decrease in the ED LOS and ICU LOS, decreased time from ED to OR, decreased hospital stay, and decreased mortality (3.8 % vs. 5.7 %). There was also a significant decrease in pneumonia, respiratory failure, and UTI rates [19]. Other institutions have been able to show similar results once standard protocols are initiated in the care of geriatric patients [20].
A number of trauma centers have developed an inpatient geriatric trauma consultation service (GTCS), a proactive geriatric consultation model aimed at preventing and managing age-specific complications, and discharge planning for elderly patients admitted to the trauma service. A report by Fallon and colleagues in 2006 documented that geriatricians identified 14 % of patients who presented with alcohol issues, 36 % of patients exhibited signs of delirium, and 46 % of patients presented with a new medical condition(s). Geriatricians assisted with advanced care planning in 15 % of cases and disposition decisions to promote function in 49 %, made medication changes in 65 %, decreased inappropriate medications in 20 %, and assisted with pain management in 42 %. Trauma surgeons followed 91 % of one or more recommendations. They concluded that outcomes of older patients can be improved through geriatricians’ expertise by addressing new and existing medical issues and reducing hospital-acquired complications such as functional decline, falls, delirium, and death [21].
A recent single-center before (n = 238)/after (n = 248) case series documented that the rate of adherence to recommendations made by the GTCS team was 93.2 %. There were fewer consultation requests made to Internal Medicine and Psychiatry in the post-GTCS group. Interestingly, there were no differences in any of the prespecified complications except delirium (50.5 % pre-GTCS vs. 40.9 % post-GTCS, p = 0.05). Among patients admitted from home, fewer were discharged to long-term care facilities among the post-GTCS group (6.5 % pre-GTCS vs. 1.7 % post-GTCS). This study documented that a proactive geriatric consultation model for elderly trauma patients may decrease delirium and discharges to long-term care facilities. Future studies should include a multicenter randomized trial of this model of care [22].
Most recently, the American College of Surgeon published the ACS TQIP Geriatric Trauma Management Guidelines. This document summarizes efforts to improve elderly trauma outcome, including initial evaluation (Table 34.1), standardizing when to obtain a geriatric consultation (Table 34.2), focus on medication management (Table 34.3), and pain control and delirium avoidance (Table 34.4). It serves as an important repository of performance improvement information relevant to the care of the elderly injured patient [23].
Table 34.1
Consideration in initial trauma evaluation of elderly patients
The primary survey for the elderly is the same as for any injured patient, but the secondary survey should emphasize the following:
Stay updated, free articles. Join our Telegram channel
Full access? Get Clinical Tree
 Get Clinical Tree app for offline access
Get Clinical Tree app for offline access

|


