| Pneumocystis jirovecii pneumonia (PCP) |
| Esophageal candidiasis |
| Wasting syndrome |
| Kaposi sarcoma |
| Disseminated Mycobacterium avium infection |
| Tuberculosis |
| Cytomegalovirus (CMV) disease |
| HIV-associated dementia |
| Recurrent bacterial pneumonia |
| Toxoplasmosis |
| Immunoblastic lymphoma |
| Chronic cryptosporidiosis |
| Burkitt lymphoma |
| Disseminated histoplasmosis |
| Invasive cervical cancer |
| Chronic herpes simplex |
Presentation
- Primary HIV infection:
- Acute seroconversion occurs 2–6 weeks after initial exposure.
- Symptoms may include: fever, fatigue, lymphadenopathy, pharyngitis, diarrhea, weight loss, and rash.
- Acute seroconversion occurs 2–6 weeks after initial exposure.
- A number of complications can result from HIV and its progression to AIDS. The presentation of some of these complications is summarized in Table 58.2.
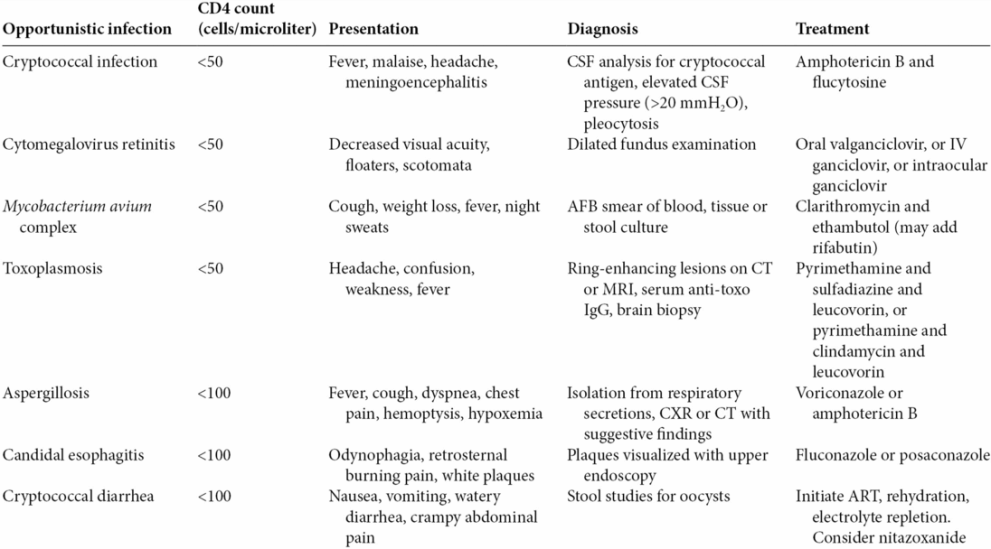

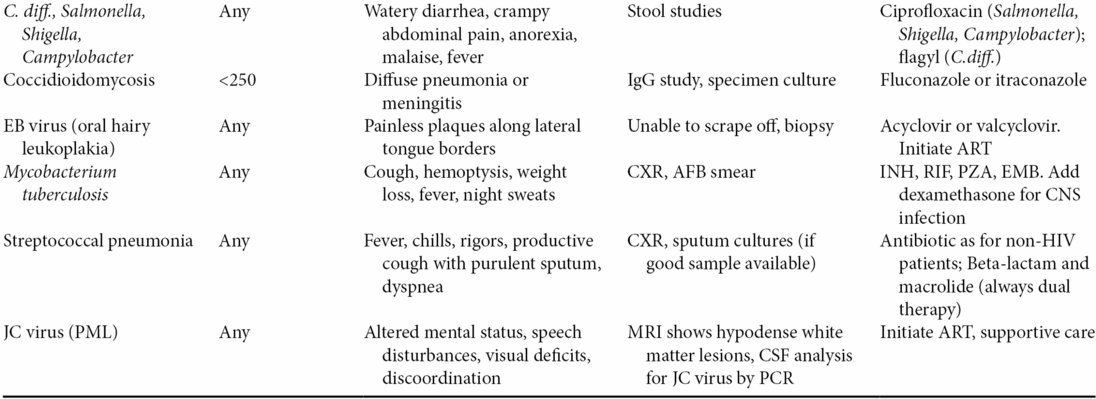
AFB, acid-fast bacillus; ART, antiretroviral therapy; BAL, bronchoalveolar lavage; C.diff., Clostridium difficile; CSF, cerebrospinal fluid; CT, computed tomography; CXR, chest radiography; EBV, Epstein–Barr virus; EMB, ethambutol; TMP, trimethoprim; IgG, immunoglobulin G; INH, isoniazid; JC, John Cunningham; KOH, potassium hydroxide; LDH, lactate dehydrogenase; MRI, magnetic resonance imaging; PaO2, partial pressure of oxygen in arterial blood; PCR, polymerase chain reaction; PML, progressive multifocal leukoencephalopathy; PZA, pyrazinamide; RIF, rifampin; SMX, sulfamethoxazole.
Diagnosis, evaluation, and critical management
- Enzyme-linked immunoassay (ELISA) or rapid HIV test followed by Western blot analysis for confirmation is the current gold standard for diagnosis of the condition.
- Opportunistic infections should be evaluated according to Table 58.2.
Sudden deterioration
- In the deteriorating patient with HIV/AIDS, the usual considerations of airway, breathing, and circulation (ABC) should be made.
- Patients with decreased level of consciousness and concern for airway compromise should be intubated.
- Additional intravenous access should be obtained with large-bore lines in anticipation of aggressive resuscitation with fluids.
- Broad-spectrum antibiotics should be initiated with additional coverage for suspected opportunistic infections (Table 58.2).
- Patients with decreased level of consciousness and concern for airway compromise should be intubated.
- Medication side effects and drug interactions can cause organ dysfunction, cardiac arrhythmias, or electrolyte abnormalities. Consider stopping the offending agent(s).
- Immune reconstitution inflammatory syndrome (IRIS) should remain a consideration.
- IRIS is a constellation of symptoms characterized by fever and worsening of the clinical manifestations of the underlying opportunistic infection.
- In this condition, the immune system begins to recover after the initiation of antiretroviral therapy (ART), and starts responding to the opportunistic infection with an excessive inflammatory response that worsens the initial symptoms.
- It is typically seen within the first 4–8 weeks after initiation of ART, and most commonly with mycobacterial infections.
- It is a clinically challenging diagnosis since its differentiation from progression of the initial opportunistic infection, the development of a new opportunistic infection, an unrelated organ dysfunction, or drug toxicity cannot be easily made.
- Patients should receive supportive care. Systemic corticosteroids may be indicated and initiated after consultation with an infectious disease specialist.
- IRIS is a constellation of symptoms characterized by fever and worsening of the clinical manifestations of the underlying opportunistic infection.
- Special considerations for the pregnant patient
- Pregnancy should not prevent diagnostic imaging that may assist in diagnosing opportunistic infections. Abdominal shielding should be considered to limit radiation exposure to the fetus.
- Immediate initiation of ART should be considered when opportunistic infections are diagnosed in pregnant patients. This can minimize transmission of disease to the fetus.
- Pregnancy should not prevent diagnostic imaging that may assist in diagnosing opportunistic infections. Abdominal shielding should be considered to limit radiation exposure to the fetus.
- System-specific complications and special considerations
- Central nervous system:
- Reported complications: encephalitis, seizure, lymphoma, meningitis.
- Altered mental status should be worked up with CT or MRI of the brain to evaluate for mass-occupying lesions, and lumbar puncture to evaluate for opportunistic infections.
- Broad-spectrum antibiotics, antivirals, and antifungals should be started if there is suspicion for meningitis in the setting of a low CD4 count.
- Reported complications: encephalitis, seizure, lymphoma, meningitis.
- Pulmonary:
- Reported complications: pneumonia, tuberculosis, PCP-related pneumothorax, and fungal infections.
- A chest radiograph (CXR) may be nonspecific. A chest CT should be considered in the setting of hypoxia or dyspnea with an equivocal CXR.
- Reported complications: pneumonia, tuberculosis, PCP-related pneumothorax, and fungal infections.
- Cardiovascular:
- Reported complications: pericardial effusion, dilated cardiomyopathy, myocarditis, coronary artery disease.
- An electrocardiogram should be performed urgently if the patient presents with chest pain.
- Consider bedside ultrasonography to evaluate for pericardial effusion and cardiac ejection fraction in the patient presenting with heart failure symptoms.
- Reported complications: pericardial effusion, dilated cardiomyopathy, myocarditis, coronary artery disease.
- Gastrointestinal:
- Reported complications: diarrhea, esophagitis, pancreatitis, and liver failure.
- Check for hepatitis B and C co-infections.
- Reported complications: diarrhea, esophagitis, pancreatitis, and liver failure.
- Renal:
- Reported complications: HIV nephropathy, and acute renal failure.
- HIV nephropathy is an indication for the initiation of ART.
- Stop all nephrotoxic medications and hydrate the patient.
- Some antiretroviral drugs are associated with nephrolithiasis and should be avoided.
- Reported complications: HIV nephropathy, and acute renal failure.
- Central nervous system:
Vasopressor of choice: Patients with AIDS who are presenting with hypotension and evidence of shock are likely to be in septic shock. Norepinephrine is currently the initial vasopressor of choice in this situation.
References
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




