| Judicious use of rapid sequence intubation (RSI) versus awake technique |
| Back-up planning |
| Prioritization of oxygenation |
| Early recognition of failure |
| Early use of surgical technique if necessary |
| Avoidance of ED intubation if necessary |
Recognizing failure (Figure 3.1)
- When first-line techniques fail to result in intubation, early identification of failure is paramount.
- If unsuccessful, laryngoscopy should be abandoned and oxygen restored with mask ventilation.
- Extraglottic airways (EGA) can be placed quickly and may provide better ventilation than bag-mask ventilation.
- If an intubation attempt fails and reoxygenation fails, a cricothyroidotomy must be performed immediately.
- Failure to recognize a “can’t intubate, can’t oxygenate” scenario will result in the patient’s death.
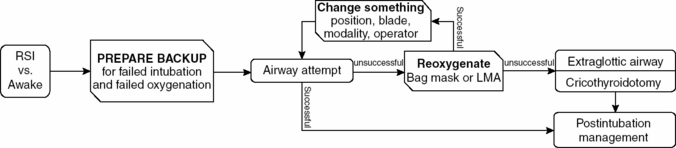
Figure 3.1. (© Reuben Strayer & emupdates.com, used with permission. Adapted from: Reuben Strayer. Emergency Department Intubation Checklist v13. 2012. http://emupdates.com/2012/07/08/emergency-department-intubation-checklist-v13/; accessed July 23, 2012).
Decision to intubate (Table 3.2)
- Many factors at play must be balanced, including:
- Early management of a sick patient
- Potential danger of paralyzing a patient
- Limited clinical evaluation of an intubated patient
- Early management of a sick patient
Table 3.2. Indications for intubation
| Indication | Rationale | Comments |
| Ventilation | The patient is not safely breathing on their own | Circumstances make it difficult to match the patient’s inherent drive (e.g., salicylate toxicity) |
| Oxygenation | Intubation allows high FiO2 and positive end-expiratory pressure | Noninvasive ventilation may suffice for many patients |
| Protection | Alterations in mental status may blunt protective airway reflexes, and conditions such as vomiting may result in aspiration | Obstructive processes (e.g., expanding hematoma) may threaten tracheal patency |
| Expected course | A presently stable patient may be expected to deteriorate | Early intubation is often safer prior to deterioration |
| Metabolic demand | Decrease work of breathing in critically ill patients (e.g., severe sepsis) | Oxygen consumption from respiration alone can rise from baseline of 5% to 50% |
Noninvasive ventilation
- In patients protecting their airway, noninvasive ventilation (NIV) may be appropriate.
- Many patients will improve dramatically with NIV and avoid intubation.
- NIV provides:
- Up to 100% FiO2
- Pressure-support, decreasing the work of breathing
- PEEP, overcoming shunt physiology (e.g., severe pneumonia, acute pulmonary edema).
- Up to 100% FiO2
- Although alteration in mental status is a traditional relative contraindication to NIV, critically ill emergency department (ED) patients can be closely monitored by experienced airway operators.
- NIV can be used to achieve two simultaneous goals:
- It can potentially improve the patient sufficiently to obviate the need for intubation.
- Barring sufficient improvement, NIV will optimize preoxygenation if intubation is necessary.
- It can potentially improve the patient sufficiently to obviate the need for intubation.
Oxygenation
- Oxygenation is the primary concern in airway management.
- As hemoglobin and oxygen bind cooperatively, desaturation is slow above SpO2 90%.
- Below 90%, hemoglobin molecules quickly lose bound oxygen, and critical hypoxia can occur in seconds.
- Due to the technical aspects of pulse oximetry, there is a lag of up to 2 minutes in the measured SpO2. Therefore, a reading in the 80–90% range may indicate that the actual SpO2 is much lower.
- Laryngoscopy should be abandoned when SpO2 reads 90% in order for the patient to be reoxygenated.
Laryngoscopy and intubation
- The following steps are necessary to place an endotracheal tube (or an EGA):
- Positioning
- Oxygenation
- Equipment and discussion of back-up plan
- Medication administration
- Laryngoscopy and intubation (or EGA placement)
- Postintubation management.
- Positioning
Positioning
- Proper positioning is essential for laryngoscopy.
- The same positioning principles will aid in preoxygenation and mask ventilation.
- Proper positioning lifts the anterior pharyngeal structures off the posterior pharynx and optimizes glottis view.
- A combination of head, neck, and body positioning can be used to optimize both of these goals.
- Jaw thrust: lifting the jaw anteriorly by the angles of the mandible to open the pharynx.
- Ear-to-sternal-notch: the patient’s head should be elevated in order for the external auditory meatus to be at the same level as the manubrium, in a plane parallel to the ceiling (Figure 3.2a).
- Jaw thrust: lifting the jaw anteriorly by the angles of the mandible to open the pharynx.
- Some patients (including: obese, with pleural effusions, at risk for vomiting) may benefit from elevating the head of the bed to 30 degrees while maintaining the same positioning principles (Figure 3.2b).
- Positioning for a video laryngoscope (VL):
- VL with conventional blades: positioning is unchanged.
- VL with an angulated blade: completely neutral head and neck position, with the head flat on the bed and the face plane parallel to the ceiling.
- VL with conventional blades: positioning is unchanged.
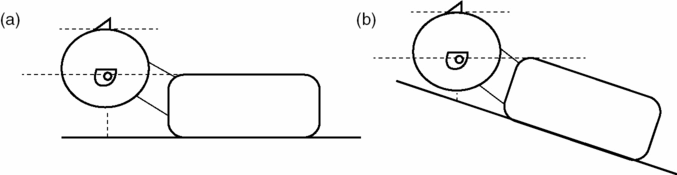
Figure 3.2. Patient positioning.
Preoxygenation
- The goal of preoxygenation is not merely to achieve an SpO2 of 100%, but also to de-nitrogenate the lungs, completely filling the lungs with oxygen to act as an oxygen reservoir during laryngoscopy.
- Preoxygenate with a non-rebreather mask (NRB) set to 15 liters per minute or higher, for at least 3 minutes.
- If hypoxia persists despite high-flow oxygen, the patient is likely shunting and may require PEEP delivered via NIV.
- Obtunded hypoxic patients, if still ventilating on their own, may be safer to ventilate with NIV under close supervision than with bag-mask ventilation.
- In the apneic patient, bag-mask ventilation (BMV) should be performed.
- Two-operator technique will provide a better mask seal as one operator can use both hands to secure the mask to the patient’s face.
- Nasal trumpets and oral airways, if tolerated, can be invaluable in maintaining pharyngeal patency.
- Use slow, smooth, controlled breaths of only half the volume of a standard bag.
- Patients obtunded due to severe metabolic acidosis will require a much faster respiratory rate, and must be ventilated during the apneic period to avoid cardiac arrest.
- Most bags accept a PEEP valve if necessary.
- Ventilators can be attached to masks, allowing for control of tidal volumes, respiratory rate, and PEEP if needed.
- Two-operator technique will provide a better mask seal as one operator can use both hands to secure the mask to the patient’s face.
- Fully obtunded and apneic patients oxygenate better with the rapid placement of an EGA.
Apneic oxygenation and oxygenation during laryngoscopy
- NRB should be left in place during the apneic period.
- As the oxygen in the lungs is filtered into the body, an O2-gradient is established allowing passive flow of oxygen from the high-FiO2 of the NRB to the lungs.
- A nasal cannula set to 15 lpm will similarly provide high-flow oxygen during laryngoscopy.
- If there are insufficient oxygen wall adaptors to provide three sources of oxygen (bag-mask, NRB, and nasal cannula), place a portable oxygen tank under the bed to provide a third source.
Extraglottic airways
- Numerous EGA options exist, primarily laryngeal tubes (mainly used in the pre-hospital setting) and laryngeal masks.
- EGA are typically used as rescue devices when it is difficult to provide BMV.
- Laryngeal masks do not fully “secure” the airway as vomit may dislodge them.
- Many second-generation laryngeal masks permit intubation through the mask.
Laryngoscopy
- Principles of laryngoscopy are identical for direct and video laryngoscopy, with the exception of different positioning.
- Suction should be available under the patient’s right shoulder. Two or more Yankauer suction tips may be necessary if blood, vomit, or copious secretions are expected.
- Various devices exist for video laryngoscopy.
- Many devices use traditional curved blades and may be used either directly or with the video monitor.
- Devices with angulated or indirect blades are operated similarly but do not allow for direct visualization.
- Angulated blades will often insert too far; if the glottis cannot be seen, withdraw slowly.
- Lifting the handle straight toward the ceiling may also improve the view.
- Video devices improve views but may be defeated by blood, mucus, or vomit.
- Tube delivery may be more difficult as the angle of attack to the trachea is steeper.
- Many devices use traditional curved blades and may be used either directly or with the video monitor.
- Stylets vastly improve tube control and delivery and should be shaped straight to the cuff, then angled to 35 degrees.
- Deliver the tube from the side (3-o’clock): rotation about the long axis will give subtle control in the vertical axis, and the tube will not obscure the glottic view.
- A partial glottic view is sufficient if the tube can be directed above the posterior cartilages (Figure 3.3).
- Tube delivery with angulated VL is often facilitated with malleable stylets shaped similarly to the blade, or with proprietary stylets.
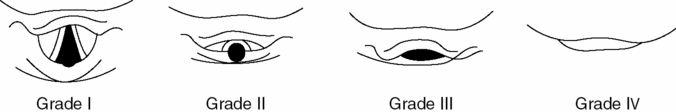
Figure 3.3. View of the vocal cords. Grade I: the entire glottis opening is visualized. Grade II: only the posterior aspect of the glottis opening is visualized. Grade III: only the tip of the epiglottis is visualized. Grade IV: only the soft palate is visualized.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree






