0.3 mg/dL within 48 hours, or
- Prerenal: inadequate perfusion of the kidney (most common) (see Table 46.1)
- Renal: diseases intrinsic to the kidney (see Table 46.2)
- Postrenal: obstruction distal to the kidney (see Table 46.3).
Table 46.1. Etiologies of prerenal AKI: the most common cause of renal failure
| Dehydration |
| Hemorrhage |
| Gastrointestinal losses |
| Diuretics |
| Hyperglycemia |
| Burns |
| Heart failure |
| Cirrhosis |
| Drugs (angiotensin-converting enzyme inhibitors, NSAIDs) |
Table 46.2. Etiologies of renal AKI: most commonly caused by acute tubular necrosis, or acute interstitial nephritis
| Acute interstitial nephritis: beta-lactams, sulfa-based drugs, NSAIDs |
| Renal ischemia |
| Antimicrobials: aminoglycosides, amphotericin B |
| Intravascular hemolysis: hemolytic uremic syndrome and thrombotic thrombocytopenic purpura |
| Rhabdomyolysis |
| Other toxic agents: cisplatin, cyclosporine A, contrast dye |
Table 46.3. Etiologies of postrenal AKI: the least common cause of AKI, due to obstruction distal to the renal parenchyma
| Papillary necrosis |
| Retroperitoneal mass |
| Prostatic hypertrophy |
| Urethral stricture |
Presentation
Classic presentation
- Since the etiology of AKI varies greatly, findings on initial examination may be vague.
- Common signs and symptoms include:
- Decreased urine output
- Signs and symptoms of reduced kidney function: lethargy, fatigability, anorexia, nausea, and vomiting
- Dark or turbid urine
- Pulmonary and peripheral edema.
- Decreased urine output
Critical presentation
- Altered mental status and seizure.
- Hyperkalemia with associated arrhythmias.
- Pulmonary edema causing respiratory failure.
Diagnosis and evaluation
- History and physical examination
- A careful patient history will frequently reveal etiology of renal failure (e.g., medications or recent administration of contrast dye).
- Diagnostic tests
- Urine studies: urinalysis, microscopy, creatinine, osmolality, and electrolytes (Table 46.4).
- Bladder catheter: enables hourly monitoring of urine output, and treats postrenal obstruction.
- Renal ultrasound: demonstrates signs of urinary obstruction including hydronephrosis and evaluates kidney size to determine acuity of injury.
- Calculate the following:
- Fractional excretion of sodium (FENA):
- FENA = (U Na/P Na)/(U Cr/P Cr).
- <1% indicates prerenal causes of AKI.
- >2% indicates intrinsic causes including acute tubular necrosis (ATN).
- FENA = (U Na/P Na)/(U Cr/P Cr).
- A sodium level <20 mEq/L suggests a prerenal condition in a patient with oliguria.
- Creatinine clearance (CrCl) may be calculated to assess general kidney function:
- CrCl = (140 – age [years]) × weight (kg)/72 × Cr (mg/dL) × 0.85 (in women)
- Fractional excretion of sodium (FENA):
- Urine studies: urinalysis, microscopy, creatinine, osmolality, and electrolytes (Table 46.4).
- KDIGO AKI Severity Score is used to define the degree of kidney injury.
- Stage 1: 1.5–1.9 times baseline, or
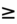 0.3 mg/dL increase in the serum creatinine, or urine output <0.5 mL/kg/hour for 6–12 hours.
0.3 mg/dL increase in the serum creatinine, or urine output <0.5 mL/kg/hour for 6–12 hours.
- Stage 2: 2.0–2.9 times baseline increase in the serum creatinine, or urine output <0.5 mL/kg/hour for 6–12 hours.
- Stage 3: >3 times baseline increase in the serum creatinine, or increase in serum creatinine to
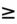 4.0 mg/dL, or urine output of <0.3 mL/kg/hour for >24 hours, or anuria for
4.0 mg/dL, or urine output of <0.3 mL/kg/hour for >24 hours, or anuria for 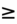 12 hours, or the initiation of renal replacement therapy, or, in patients <18 years old, decrease in estimated GFR to <35 mL/minute per 1.73 m2.
12 hours, or the initiation of renal replacement therapy, or, in patients <18 years old, decrease in estimated GFR to <35 mL/minute per 1.73 m2.
- Stage 1: 1.5–1.9 times baseline, or
- The clinical utility of AKI scoring systems is uncertain, but they help predict mortality. As the stage of AKI worsens, the risk of death and need for renal replacement therapy increases.
Table 46.4. Urine microscopy/urinary sediment findings: probable etiology
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree




