CHAPTER 184
Warts
(Common Wart, Plantar Wart)
Presentation
Patients generally seek medical care when a wart has become painful, partially avulsed, or cosmetically unacceptable and annoying.
Common warts usually appear as one or more dome-shaped hyperkeratotic verrucous papules on the hands but may occur anywhere on the body. Plantar warts occur on the soles of the feet, interrupting the normal skin lines and frequently occurring at points of maximum pressure, such as over the heads of the metatarsal bones or on the heel. Plantar warts do not have a verrucous or cauliflower appearance but are surrounded by a thick painful callus that impairs walking. Both types of wart contain black dots within their substance, which represent thrombosed capillaries (Figures 184-1 and 184-2).
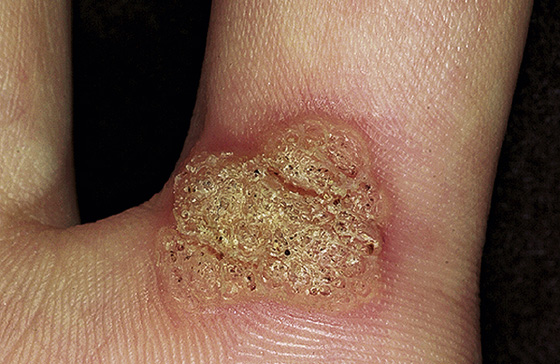
Figure 184-1 A common wart with black dots on the surface. (From Habif T: Clinical dermatology, ed 4. St Louis, 2004, Mosby.)
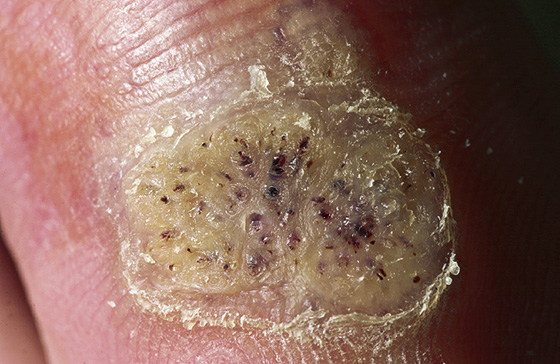
Figure 184-2 Thrombosed black vessels are trapped in the cylindrical projections. (From Habif T: Clinical dermatology, ed 4. St Louis, 2004, Mosby.)
These lesions may appear at any age but commonly occur in children and young adults. Their course is highly variable; most resolve spontaneously in weeks or months, and others may last years or a lifetime.
What To Do:
 Confirm the diagnosis by obtaining a typical history, along with noting classic physical findings, which include the obscuring of normal skin lines. Shaving off the overlying hyperkeratotic surface with a No. 15 or No. 10 surgical blade may also reveal the typical black dots of thrombosed vessels, along with a uniform mosaic surface pattern. (The pattern can be seen with a hand lens.)
Confirm the diagnosis by obtaining a typical history, along with noting classic physical findings, which include the obscuring of normal skin lines. Shaving off the overlying hyperkeratotic surface with a No. 15 or No. 10 surgical blade may also reveal the typical black dots of thrombosed vessels, along with a uniform mosaic surface pattern. (The pattern can be seen with a hand lens.)
 Inform patients that warts often require several treatments before a cure is realized and that, in general, the more rapid the wart removal technique, the more likely the process will cause pain.
Inform patients that warts often require several treatments before a cure is realized and that, in general, the more rapid the wart removal technique, the more likely the process will cause pain.
 If a slower, less painful treatment is selected, suggestive therapy generally works through the age of 10 years. A banana peel, a potato eye, or a penny applied to the skin and covered with tape for a 1- to 2-week period has been effective in young children. Another technique is to draw the body part on a piece of paper and then draw a picture of the wart on the diagram. Finally, crumble the pictures and throw them away.
If a slower, less painful treatment is selected, suggestive therapy generally works through the age of 10 years. A banana peel, a potato eye, or a penny applied to the skin and covered with tape for a 1- to 2-week period has been effective in young children. Another technique is to draw the body part on a piece of paper and then draw a picture of the wart on the diagram. Finally, crumble the pictures and throw them away.
 Other nonpainful techniques can be used on patients of any age. Duct tape occlusion therapy may be more effective than cryotherapy for common warts. The patient completely covers the wart and the area around the wart with common duct tape. This is left on for 6 days; the wart is then soaked in warm water until its surface is softened; then the surface is scraped off using an emery board or pumice stone. After 12 hours, the patient puts on a new piece of tape for another 6 days and then repeats the process for 2 months or until the wart is gone. This technique is effective approximately 85% of the time. When the skin lines are reestablished, the warts are gone.
Other nonpainful techniques can be used on patients of any age. Duct tape occlusion therapy may be more effective than cryotherapy for common warts. The patient completely covers the wart and the area around the wart with common duct tape. This is left on for 6 days; the wart is then soaked in warm water until its surface is softened; then the surface is scraped off using an emery board or pumice stone. After 12 hours, the patient puts on a new piece of tape for another 6 days and then repeats the process for 2 months or until the wart is gone. This technique is effective approximately 85% of the time. When the skin lines are reestablished, the warts are gone.
 More traditional keratolytic therapy (40% salicylic acid plasters—Mediplast and others) can also be used on both common and plantar warts. Shave excessive tissue from the surface of the wart using a No. 15 or No. 10 scalpel blade. Have the patient cut a piece of the salicylic acid plaster to a size and shape that will fit over the entire wart. (This is particularly useful for treating large plantar warts.) The sticky surface is applied to the wart and then secured with tape. The plaster is removed after 48 hours, and the white keratin is scraped off as described, using an emery board or a pumice stone. Another plaster is immediately applied, and the process is repeated every 2 days for many weeks or until the wart is completely gone.
More traditional keratolytic therapy (40% salicylic acid plasters—Mediplast and others) can also be used on both common and plantar warts. Shave excessive tissue from the surface of the wart using a No. 15 or No. 10 scalpel blade. Have the patient cut a piece of the salicylic acid plaster to a size and shape that will fit over the entire wart. (This is particularly useful for treating large plantar warts.) The sticky surface is applied to the wart and then secured with tape. The plaster is removed after 48 hours, and the white keratin is scraped off as described, using an emery board or a pumice stone. Another plaster is immediately applied, and the process is repeated every 2 days for many weeks or until the wart is completely gone.
 Salicylic acid liquid (DuoPlant gel, Occlusal-HP liquid and many others that are now available over the counter) is also effective but is more likely to cause inflammation and soreness.
Salicylic acid liquid (DuoPlant gel, Occlusal-HP liquid and many others that are now available over the counter) is also effective but is more likely to cause inflammation and soreness.
 One single-blinded clinical trial performed on 60 patients with common hand warts compared cryotherapy with the application of an 80% phenol solution (which is a caustic agent). Thirty patients were treated with cryotherapy and 30 patients were treated with 80% phenol, on a once-weekly basis until complete clearance of the lesions or a maximum duration of 6 weeks occurred. Complete clearance of warts after 6 weeks was observed in 70% of patients who were treated with cryotherapy, and 82.6% of patients in the 80% phenol group; there was no statistically significant difference between the two methods (P = .014). This study showed that 80% phenol and cryotherapy were both effective and simple treatments for common warts of the hands, and patients do not experience any pain during the phenol treatment.
One single-blinded clinical trial performed on 60 patients with common hand warts compared cryotherapy with the application of an 80% phenol solution (which is a caustic agent). Thirty patients were treated with cryotherapy and 30 patients were treated with 80% phenol, on a once-weekly basis until complete clearance of the lesions or a maximum duration of 6 weeks occurred. Complete clearance of warts after 6 weeks was observed in 70% of patients who were treated with cryotherapy, and 82.6% of patients in the 80% phenol group; there was no statistically significant difference between the two methods (P = .014). This study showed that 80% phenol and cryotherapy were both effective and simple treatments for common warts of the hands, and patients do not experience any pain during the phenol treatment.
 For resistant lesions, the immunomodulating drug imiquimod 5% cream (Aldara) can be used in combination with a keratolytic agent. It is essential to débride the thick scale before applying imiquimod. The patient applies the cream daily before bedtime and covers the area with tape (for ≥12 hours). This may be used 3 days per week for 10 to 16 weeks. This treatment is quite expensive, costing from $200 to $250.
For resistant lesions, the immunomodulating drug imiquimod 5% cream (Aldara) can be used in combination with a keratolytic agent. It is essential to débride the thick scale before applying imiquimod. The patient applies the cream daily before bedtime and covers the area with tape (for ≥12 hours). This may be used 3 days per week for 10 to 16 weeks. This treatment is quite expensive, costing from $200 to $250.
 The most rapid but most painful treatment for common warts is cryotherapy. The hyperkeratotic surface is reduced using a scalpel blade; then liquid nitrogen is applied to the wart using a cotton-tipped applicator until a 1- to 2-mm zone of frozen tissue is created and maintained around the lesion for about 5 seconds. The area is then allowed to thaw. A second or third freeze during the same treatment session may increase the cure rate. Severe pain may develop and last for minutes to hours; appropriate analgesia should be provided. Inform the patient that a small blister that is sometimes hemorrhagic will develop under the wart. If the wart does not completely resolve, freezing may be repeated in 2 to 4 weeks. One small randomized controlled trial provided evidence to support the use of cryotherapy over salicylic acid treatment for common warts only. For plantar warts, they found no clinically relevant difference between cryotherapy, salicylic acid treatment, or a wait-and-see approach after 13 weeks. It should also be noted that one study demonstrated that OTC refrigerants did not achieve results equivalent to liquid nitrogen when used for treating warts.
The most rapid but most painful treatment for common warts is cryotherapy. The hyperkeratotic surface is reduced using a scalpel blade; then liquid nitrogen is applied to the wart using a cotton-tipped applicator until a 1- to 2-mm zone of frozen tissue is created and maintained around the lesion for about 5 seconds. The area is then allowed to thaw. A second or third freeze during the same treatment session may increase the cure rate. Severe pain may develop and last for minutes to hours; appropriate analgesia should be provided. Inform the patient that a small blister that is sometimes hemorrhagic will develop under the wart. If the wart does not completely resolve, freezing may be repeated in 2 to 4 weeks. One small randomized controlled trial provided evidence to support the use of cryotherapy over salicylic acid treatment for common warts only. For plantar warts, they found no clinically relevant difference between cryotherapy, salicylic acid treatment, or a wait-and-see approach after 13 weeks. It should also be noted that one study demonstrated that OTC refrigerants did not achieve results equivalent to liquid nitrogen when used for treating warts.
 Recalcitrant warts or periungual warts that may be difficult or painful to remove should be referred to a dermatologist. Carbon dioxide (CO2) laser vaporization and pulsed-dye laser treatments may be used under certain circumstances, and they have a 51.1% to 90% success rate.
Recalcitrant warts or periungual warts that may be difficult or painful to remove should be referred to a dermatologist. Carbon dioxide (CO2) laser vaporization and pulsed-dye laser treatments may be used under certain circumstances, and they have a 51.1% to 90% success rate.
What Not To Do:
 Do not mistake corns (clavi) that form over the metatarsal heads for plantar warts. After paring warts with a No. 15 blade, they will reveal centrally located black vessels (dots) that will sometimes bleed with additional paring. Corns, on the other hand, have a hard, painful, well-demarcated translucent central core (Figure 184-3). Lateral pressure on a wart causes pain, but pinching a plantar corn is painless.
Do not mistake corns (clavi) that form over the metatarsal heads for plantar warts. After paring warts with a No. 15 blade, they will reveal centrally located black vessels (dots) that will sometimes bleed with additional paring. Corns, on the other hand, have a hard, painful, well-demarcated translucent central core (Figure 184-3). Lateral pressure on a wart causes pain, but pinching a plantar corn is painless.
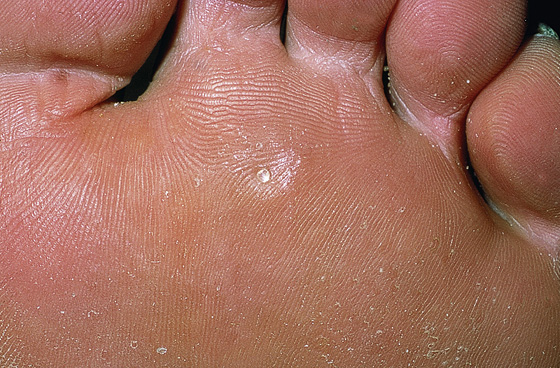
Figure 184-3 A pared corn shows a translucent core. (From White G, Cox N: Diseases of the skin, ed 2. St Louis, 2006, Mosby.)
Discussion
Warts are common and usually benign. They are caused by human papillomaviruses. The virus infects keratinocytes, which proliferate to form a mass that remains confined to the epidermis. There are no “roots” that penetrate the dermis. Warts are transmitted simply by touch. Plantar warts may be acquired from moist surfaces in communal swimming areas.
Diagnosis is usually made by history and simple examination of these familiar-appearing growths. Some warts respond quickly to routine therapy, whereas others are resistant. Subungual and periungual warts are more resistant to treatment than are warts located in other areas. There may be more to these warts than meets the eye, with a portion of the wart being hidden under the nail.
Because warts are confined to the epidermis, they can usually be removed with little, if any, scarring.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


