CHAPTER 95
Vaginitis
Presentation
A woman complains of a vaginal discharge, possibly with itching and/or irritation of the labia and vagina. Odor, external dysuria, vague low abdominal discomfort, or dyspareunia may be present. (Suprapubic discomfort, internal dysuria, and urinary urgency and frequency suggest cystitis.)
Abdominal examination is benign, but examination of the introitus may reveal erythema of the vulva and edema of the labia, often with pustulopapular peripheral lesions (especially with Candida organisms). Speculum examination may disclose a diffusely red, inflamed vaginal mucosa with an adherent thick, white discharge resembling cottage cheese. These findings are also most likely the result of Candida organisms, especially when associated with vulvar pruritus.
A thin, homogeneous, gray-to-white milklike discharge smoothly coating the vaginal wall and having a fishy odor is characteristic of bacterial vaginosis.
Profuse yellow-green, sometimes frothy discharge with an unpleasant malodor and associated with vulvar irritation is characteristic of Trichomonas organisms.
Bimanual examination should show a nontender cervix and uterus, without adnexal tenderness or masses or pain on cervical motion (if present, see Chapter 93).
The appearance of the discharge is not pathognomonic and testing needs to confirm any suspicion.
What To Do:
 Take a brief sexual history. Ask if partners are experiencing related symptoms.
Take a brief sexual history. Ask if partners are experiencing related symptoms.
 Perform speculum and bimanual pelvic examination.
Perform speculum and bimanual pelvic examination.
 Collect urine for possible culture and pregnancy tests that may influence treatment.
Collect urine for possible culture and pregnancy tests that may influence treatment.
 Swab the cervix or urethra to culture for Neisseria gonorrhoeae and swab the endocervix to test for Chlamydia (see Chapter 83).
Swab the cervix or urethra to culture for Neisseria gonorrhoeae and swab the endocervix to test for Chlamydia (see Chapter 83).
 Touch pH indicator paper (Hydrion pH papers, ColorpHast pH Test Strips) to the vaginal mucus. A pH greater than 4.5 suggests bacterial vaginosis or Trichomonas organisms, but this is only useful if there is no blood or semen to buffer vaginal secretions. A normal pH (4 to 4.5) is found with Candida vulvovaginitis. Normal pH for a premenarchal or postmenopausal woman is 4.7, thus a less reliable test in these patients.
Touch pH indicator paper (Hydrion pH papers, ColorpHast pH Test Strips) to the vaginal mucus. A pH greater than 4.5 suggests bacterial vaginosis or Trichomonas organisms, but this is only useful if there is no blood or semen to buffer vaginal secretions. A normal pH (4 to 4.5) is found with Candida vulvovaginitis. Normal pH for a premenarchal or postmenopausal woman is 4.7, thus a less reliable test in these patients.
 For wet-mount examination, dab a drop of vaginal secretions on a slide, add a drop of 0.9% NaCl and a cover slip, and examine under 400× magnification for swimming protozoa (Trichomonas vaginalis), epithelial cells covered by adherent bacilli (“clue cells” of bacterial vaginosis), or pseudohyphae and spores (“spaghetti and meatballs” appearance of Candida albicans) (Figures 95-1 and 95-2).
For wet-mount examination, dab a drop of vaginal secretions on a slide, add a drop of 0.9% NaCl and a cover slip, and examine under 400× magnification for swimming protozoa (Trichomonas vaginalis), epithelial cells covered by adherent bacilli (“clue cells” of bacterial vaginosis), or pseudohyphae and spores (“spaghetti and meatballs” appearance of Candida albicans) (Figures 95-1 and 95-2).
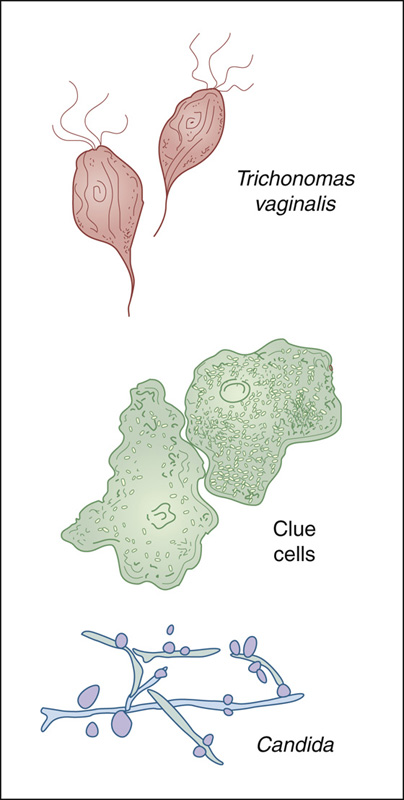
Figure 95-1 Test vaginal mucus on a slide with saline.
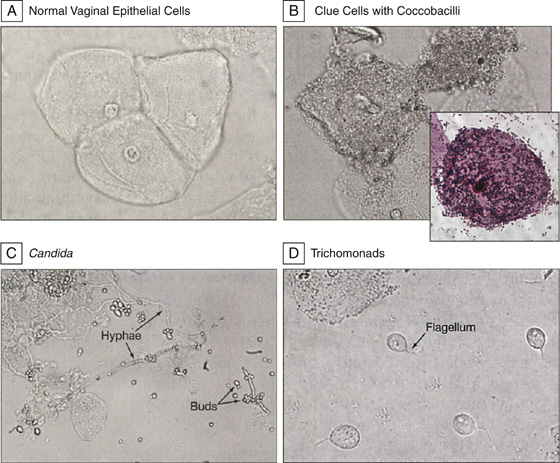
Figure 95-2 Microscopic examination of vaginal samples. (Adapted from Anderson MR, Klink K, Cohrssen A: Evaluation of vaginal complaints. JAMA 291:1368-1379, 2004.)
 If epithelial cells obscure the view of yeast, add a drop of 10% potassium hydroxide (KOH), smell whether this liberates the odor of stale fish (characteristic of Gardnerella organisms [bacterial vaginosis], Trichomonas organisms, and semen), and look again under the microscope for hyphae, pseudohyphae, or budding yeast.
If epithelial cells obscure the view of yeast, add a drop of 10% potassium hydroxide (KOH), smell whether this liberates the odor of stale fish (characteristic of Gardnerella organisms [bacterial vaginosis], Trichomonas organisms, and semen), and look again under the microscope for hyphae, pseudohyphae, or budding yeast.
 Gram stain a second specimen. This is an even more sensitive method for detecting Candida organisms and clue cells (see Figure 95-2, B), as well as a means to assess the general vaginal flora, which is normally mixed with occasional predominance of gram-positive rods.
Gram stain a second specimen. This is an even more sensitive method for detecting Candida organisms and clue cells (see Figure 95-2, B), as well as a means to assess the general vaginal flora, which is normally mixed with occasional predominance of gram-positive rods.
 When available, culture for T. vaginalis using Diamond’s medium, or other rapid tests available will confirm most cases of Trichomonas infection.
When available, culture for T. vaginalis using Diamond’s medium, or other rapid tests available will confirm most cases of Trichomonas infection.
 If Trichomonas vaginalis is the cause, prescribe metronidazole (Flagyl), 2 g, as one oral dose. A more expensive alternative that appears to be more effective and has fewer side effects is tinidazole (Tindamax), also taken as a single 2-g oral dose. Tinidazole is considered a second-generation nitroimidazole. The patient must abstain from alcohol for 24 hours postmetronidazole and 3 days after the last dose of tinidazole because of the disulfiram-like activity of these drugs. Men infected with T. vaginalis may be asymptomatic or have symptoms of urethral irritation and/or discharge, or they may develop prostatitis (see Chapters 82 and 83). Sex partners must receive the same treatment as the patient. Advise the patient and her partner to refrain from intercourse or to use a condom until therapy has been completed and patient and partners are asymptomatic, at least 7 days. Follow-up is unnecessary for men and women who become asymptomatic after treatment or who are initially asymptomatic.
If Trichomonas vaginalis is the cause, prescribe metronidazole (Flagyl), 2 g, as one oral dose. A more expensive alternative that appears to be more effective and has fewer side effects is tinidazole (Tindamax), also taken as a single 2-g oral dose. Tinidazole is considered a second-generation nitroimidazole. The patient must abstain from alcohol for 24 hours postmetronidazole and 3 days after the last dose of tinidazole because of the disulfiram-like activity of these drugs. Men infected with T. vaginalis may be asymptomatic or have symptoms of urethral irritation and/or discharge, or they may develop prostatitis (see Chapters 82 and 83). Sex partners must receive the same treatment as the patient. Advise the patient and her partner to refrain from intercourse or to use a condom until therapy has been completed and patient and partners are asymptomatic, at least 7 days. Follow-up is unnecessary for men and women who become asymptomatic after treatment or who are initially asymptomatic.
 Pregnant women who are symptomatic with trichomoniasis may be treated with a single 2-g dose of metronidazole, although 500 mg bid for 5 to 7 days is much better tolerated in patients already prone to nausea. Multiple studies and meta-analyses have not demonstrated a consistent association between metronidazole use during pregnancy and teratogenic or mutagenic effects in infants. The Centers for Disease Control and Prevention (CDC) no longer discourages the use of metronidazole in the first trimester. However, one study did note preterm labor increased when treating with metronidazole orally, thus treatment of asymptomatic pregnant patients can be delayed until after delivery. If symptomatic, consider clotrimazole 1% intravaginally for 7 days. This will relieve symptoms but is unlikely to eradicate the organisms; thus delayed treatment postdelivery will be needed.
Pregnant women who are symptomatic with trichomoniasis may be treated with a single 2-g dose of metronidazole, although 500 mg bid for 5 to 7 days is much better tolerated in patients already prone to nausea. Multiple studies and meta-analyses have not demonstrated a consistent association between metronidazole use during pregnancy and teratogenic or mutagenic effects in infants. The Centers for Disease Control and Prevention (CDC) no longer discourages the use of metronidazole in the first trimester. However, one study did note preterm labor increased when treating with metronidazole orally, thus treatment of asymptomatic pregnant patients can be delayed until after delivery. If symptomatic, consider clotrimazole 1% intravaginally for 7 days. This will relieve symptoms but is unlikely to eradicate the organisms; thus delayed treatment postdelivery will be needed.
 When the diagnosis of vulvovaginal candidiasis (VVC) is suggested clinically by a white cottage cheese–like discharge, pruritus and erythema in the vulvovaginal area, and vaginal pH less than or equal to 4.5, and when yeasts or pseudohyphae are demonstrated on either a wet preparation or a Gram stain, recommend fluconizole 150 mg PO as a single dose. It is secreted in vaginal secretions for 72 hours postingestion and is at least as effective as intravaginal treatment. In addition, it is preferred by many patients. Alternatively, if the oral route is not preferred or medication interaction precludes its use, miconazole (Monistat), 200-mg vaginal suppositories should be recommended. These are to be inserted qhs × 3 days, or alternatively, tioconazole (Monistat-1 or Vagistat-1), 6.5% cream, 5 g intravaginally can be used in a single application. (Use of cream also soothes irritated mucosa.) These treatments are available without prescription.
When the diagnosis of vulvovaginal candidiasis (VVC) is suggested clinically by a white cottage cheese–like discharge, pruritus and erythema in the vulvovaginal area, and vaginal pH less than or equal to 4.5, and when yeasts or pseudohyphae are demonstrated on either a wet preparation or a Gram stain, recommend fluconizole 150 mg PO as a single dose. It is secreted in vaginal secretions for 72 hours postingestion and is at least as effective as intravaginal treatment. In addition, it is preferred by many patients. Alternatively, if the oral route is not preferred or medication interaction precludes its use, miconazole (Monistat), 200-mg vaginal suppositories should be recommended. These are to be inserted qhs × 3 days, or alternatively, tioconazole (Monistat-1 or Vagistat-1), 6.5% cream, 5 g intravaginally can be used in a single application. (Use of cream also soothes irritated mucosa.) These treatments are available without prescription.
 With severe VVC (i.e., extensive vulvar erythema, edema, excoriation, and fissure formation), have the patient use clotrimazole (Mycelex) 1% cream, 5 g intravaginally for 7 to 14 days, or prescribe 150 mg of fluconazole in two sequential doses (second dose 72 hours after the initial dose). In patients with severe discomfort secondary to vulvitis, low-potency steroid creams used for the first 48 hours, in combination with a topical antifungal cream may be of benefit. Women with medical conditions such as uncontrolled diabetes or those receiving corticosteroid treatment also require more prolonged (i.e., 7 to 14 days), conventional antimycotic treatment. During pregnancy, only topical azole therapies, applied for 7 days, are recommended. Sex partners need not be treated unless they have balanitis. The patient only needs to return for follow-up visits if her symptoms persist or recur within 2 months of her initial treatment.
With severe VVC (i.e., extensive vulvar erythema, edema, excoriation, and fissure formation), have the patient use clotrimazole (Mycelex) 1% cream, 5 g intravaginally for 7 to 14 days, or prescribe 150 mg of fluconazole in two sequential doses (second dose 72 hours after the initial dose). In patients with severe discomfort secondary to vulvitis, low-potency steroid creams used for the first 48 hours, in combination with a topical antifungal cream may be of benefit. Women with medical conditions such as uncontrolled diabetes or those receiving corticosteroid treatment also require more prolonged (i.e., 7 to 14 days), conventional antimycotic treatment. During pregnancy, only topical azole therapies, applied for 7 days, are recommended. Sex partners need not be treated unless they have balanitis. The patient only needs to return for follow-up visits if her symptoms persist or recur within 2 months of her initial treatment.
 For recurrent infections, Fluconazole may be repeated and thus taken days 1, 4, and 7. Gastrointestinal side effects are fairly common, and serious side effects can occur. For recurrent Candida, the American Infectious Disease Society recommends 10 to 14 days of a topical or oral azole, such as miconizole or clotrimazole, followed by 6 months of either a clotrimazole 200-mg vaginal suppository twice weekly or weekly doses of oral fluconazole 150 mg.
For recurrent infections, Fluconazole may be repeated and thus taken days 1, 4, and 7. Gastrointestinal side effects are fairly common, and serious side effects can occur. For recurrent Candida, the American Infectious Disease Society recommends 10 to 14 days of a topical or oral azole, such as miconizole or clotrimazole, followed by 6 months of either a clotrimazole 200-mg vaginal suppository twice weekly or weekly doses of oral fluconazole 150 mg.
 If the diagnosis is bacterial vaginosis, prescribe metronidazole (Flagyl), 500 mg orally bid for 7 days; or tinidazole (Tindamax) can be used orally at 1 g daily for 5 days or 2 g daily for 2 days (taken with food). Alternatively, metronidazole, 0.75% vaginal gel (MetroGel-Vaginal), one applicator intravaginally qhs for 5 days; or clindamycin, 2% vaginal cream (Cleocin), one 5-g applicator intravaginally qhs for 7 days. Alternative therapy includes metronidazole as a single 2-g oral dose (noted to have lower efficacy than the above mentioned regimen); clindamycin, 300 mg orally bid for 7 days; or clindamycin ovules, 100 mg intravaginally qhs for 3 days. A topical single dose bioadhesive form of clindamycin is available (Clindesse); the patient uses one applicator. It is not clear as yet, but this may be less effective than other agents. Clindamycin-resistant organisms can develop in the vaginal mucosa postintravaginal treatment.
If the diagnosis is bacterial vaginosis, prescribe metronidazole (Flagyl), 500 mg orally bid for 7 days; or tinidazole (Tindamax) can be used orally at 1 g daily for 5 days or 2 g daily for 2 days (taken with food). Alternatively, metronidazole, 0.75% vaginal gel (MetroGel-Vaginal), one applicator intravaginally qhs for 5 days; or clindamycin, 2% vaginal cream (Cleocin), one 5-g applicator intravaginally qhs for 7 days. Alternative therapy includes metronidazole as a single 2-g oral dose (noted to have lower efficacy than the above mentioned regimen); clindamycin, 300 mg orally bid for 7 days; or clindamycin ovules, 100 mg intravaginally qhs for 3 days. A topical single dose bioadhesive form of clindamycin is available (Clindesse); the patient uses one applicator. It is not clear as yet, but this may be less effective than other agents. Clindamycin-resistant organisms can develop in the vaginal mucosa postintravaginal treatment.
 Intravaginal treatment is more expensive but carries fewer gastrointestinal side effects than the oral form, and some patients prefer using intravaginal products for treating this vaginosis. Vaginal therapy is considered more inconvenient by other patients and is associated with a high risk for vaginal candidiasis (10% to 30%). Metronidazole and timidazole cannot be used for 3 days after drinking alcohol. Sex partners need not be treated unless they have balanitis.
Intravaginal treatment is more expensive but carries fewer gastrointestinal side effects than the oral form, and some patients prefer using intravaginal products for treating this vaginosis. Vaginal therapy is considered more inconvenient by other patients and is associated with a high risk for vaginal candidiasis (10% to 30%). Metronidazole and timidazole cannot be used for 3 days after drinking alcohol. Sex partners need not be treated unless they have balanitis.
 During pregnancy, prescribe metronidazole, 500 mg orally bid or 250 mg orally tid for 7 days, or clindamycin, 300 mg orally bid for 7 days. Some prefer to use oral rather than topical therapy in pregnancy because it may also treat subclinical coinfections. Vaginal treatment is less preferred in pregnancy because of concerns about possible preterm labor.
During pregnancy, prescribe metronidazole, 500 mg orally bid or 250 mg orally tid for 7 days, or clindamycin, 300 mg orally bid for 7 days. Some prefer to use oral rather than topical therapy in pregnancy because it may also treat subclinical coinfections. Vaginal treatment is less preferred in pregnancy because of concerns about possible preterm labor.
 Follow-up visits are unnecessary unless symptoms recur.
Follow-up visits are unnecessary unless symptoms recur.
 To prevent rebound C. albicans after antibiotics reduce the normal vaginal flora, or for treatment of mild vaginitis, consider having patients douche with 1% acetic acid (half-strength white vinegar) to maintain a normal low pH vaginal ecology.
To prevent rebound C. albicans after antibiotics reduce the normal vaginal flora, or for treatment of mild vaginitis, consider having patients douche with 1% acetic acid (half-strength white vinegar) to maintain a normal low pH vaginal ecology.
 Remember that a patient may harbor more than one infection.
Remember that a patient may harbor more than one infection.
 Instruct the patient in the prevention of vaginitis. She should avoid routine douching, perfumed soaps and feminine hygiene sprays, and tight, poorly ventilated clothing.
Instruct the patient in the prevention of vaginitis. She should avoid routine douching, perfumed soaps and feminine hygiene sprays, and tight, poorly ventilated clothing.
 The differential
The differential
 Ninety percent of all cases of vaginitis are caused by bacterial vaginosis, vulvovaginal candidiasis, or trichomonal vaginitis. However, there are noninfectious causes as well— physiologic leukorrhea, a generally nonmalodorous, mucous-like, white or yellowish discharge without other symptoms, is usually estrogen induced. Atrophic vaginitis, caused by estrogen deficiency leads to inflammation of the vagina, and topical estrogen is the treatment of choice. Desquamative inflammatory vaginitis is rare, with signs and symptoms of pain, profuse discharge, and epithelial cell exfoliation. Clindamycin, for its antibacterial as well as its anti-inflammatory effect, works well for these patients. Seminal plasma allergy is in the differential; although rare, it presents with postcoital itching, burning, edema, and erythema and can have systemic symptoms as well.
Ninety percent of all cases of vaginitis are caused by bacterial vaginosis, vulvovaginal candidiasis, or trichomonal vaginitis. However, there are noninfectious causes as well— physiologic leukorrhea, a generally nonmalodorous, mucous-like, white or yellowish discharge without other symptoms, is usually estrogen induced. Atrophic vaginitis, caused by estrogen deficiency leads to inflammation of the vagina, and topical estrogen is the treatment of choice. Desquamative inflammatory vaginitis is rare, with signs and symptoms of pain, profuse discharge, and epithelial cell exfoliation. Clindamycin, for its antibacterial as well as its anti-inflammatory effect, works well for these patients. Seminal plasma allergy is in the differential; although rare, it presents with postcoital itching, burning, edema, and erythema and can have systemic symptoms as well.
What Not To Do:
 Do not blindly prescribe creams or other therapies for nonspecific symptoms of vaginitis. Perform the appropriate physical examination and laboratory tests before initiating one of the treatment regimens recommended.
Do not blindly prescribe creams or other therapies for nonspecific symptoms of vaginitis. Perform the appropriate physical examination and laboratory tests before initiating one of the treatment regimens recommended.
 Do not miss underlying pelvic inflammatory disease, pregnancy, or diabetes, all of which can potentiate vaginitis.
Do not miss underlying pelvic inflammatory disease, pregnancy, or diabetes, all of which can potentiate vaginitis.
 Do not attempt to treat trichomoniasis with metronidazole gel. It is unlikely to achieve therapeutic levels in the urethra and perivaginal glands where infection is also located, and is considerably less efficacious than oral preparations.
Do not attempt to treat trichomoniasis with metronidazole gel. It is unlikely to achieve therapeutic levels in the urethra and perivaginal glands where infection is also located, and is considerably less efficacious than oral preparations.
 Do not recommend the use of commercially obtainable unstandardized Lactobacillus for treatment of bacterial vaginosis. Recurrence rates are high, and vaginal Lactobacillus replacement remains a clinical research endeavor.
Do not recommend the use of commercially obtainable unstandardized Lactobacillus for treatment of bacterial vaginosis. Recurrence rates are high, and vaginal Lactobacillus replacement remains a clinical research endeavor.
 Do not miss candidiasis because the vaginal secretions appear essentially normal in consistency, color, volume, and odor. Nonpregnant patients may not develop thrush patches, curds, or caseous discharge.
Do not miss candidiasis because the vaginal secretions appear essentially normal in consistency, color, volume, and odor. Nonpregnant patients may not develop thrush patches, curds, or caseous discharge.
 Do not treat patients based on self-diagnosis. In one study, only 33.7% of women who self diagnosed vulvovaginal candidiasis were ultimately confirmed to have the disorder.
Do not treat patients based on self-diagnosis. In one study, only 33.7% of women who self diagnosed vulvovaginal candidiasis were ultimately confirmed to have the disorder.
 Do not treat sex partners of patients with bacterial vaginosis or C. albicans unless they show signs of infection or have had recurrent infections.
Do not treat sex partners of patients with bacterial vaginosis or C. albicans unless they show signs of infection or have had recurrent infections.
Discussion
Trichomoniasis and bacterial vaginosis are often grouped together, despite major differences in etiology, pathophysiology, and transmission implications. The reason that these two entities are frequently considered together is that they present with elevated vaginal pH, major shifts in vaginal flora, and abnormal vaginal discharge that is characteristically malodorous. Also, they frequently coexist.
Trichomonas vaginalis is a parasite that is transmitted primarily through sexual activity. In addition to the vaginal discomfort, trichomoniasis facilitates the transmission of human immunodeficiency virus (HIV). During pregnancy, infection has been associated with delivery of low-birth-weight infants and preterm deliveries. Diagnosis is typically made by identification of motile trichomonads on a saline wet preparation. It is important to note that wet-mount examination can be negative in up to 50% of culture-confirmed cases. Therefore, in suspect cases in which the wet-mount examination is negative, it is important to culture the vaginal discharge on Diamond Hollander medium or to use a DNA probe test (e.g., Affirm VPIII [Becton Dickinson and Company, Sparks, Md.]).
It is thought that bacterial vaginosis (BV) results from a disturbance in the normal vaginal flora, whereby the normal levels of Lactobacillus are reduced and replaced by less dominant organisms, such as Gardnerella vaginalis, Mycoplasma, Mobiluncus, Bacteroides spp., and Peptostreptococcus. Lactobacillus is necessary to maintain normal vaginal pH (<4.5) and to prevent proliferation of other organisms. Risk factors associated with BV include the number of sex partners in the previous 12 months, douching, smoking, and low socioeconomic conditions.
Patients with BV usually complain of thin, off-white, fishy-smelling discharge. However, because studies have demonstrated poor a correlation between vaginal symptoms and the final cause of vaginitis, clinicians should not treat vaginal complaints empirically based on patient history alone. BV is often diagnosed on the basis of a typical history in conjunction with clue cells on a wet preparation or an elevated vaginal pH. Although this approach to diagnosis is not unreasonable, accuracy can be improved by using complete Amsel criteria. This includes (1) milky homogeneous adherent discharge, (2) vaginal pH greater than 4.5, (3) clue cells in the vaginal fluid on light microscopy, and (4) positive whiff test. If three out of the four criteria are present, there is a 90% likelihood of BV. Cultures are not helpful in diagnosing BV. The Affirm VPIII DNA probe is a highly sensitive and specific test but is expensive, and there is a moderate delay for results. Gram staining is highly reliable and inexpensive, but it is not always available in a doctor’s office.
Bacterial vaginosis has been so called because of the absence of inflammatory signs traditionally associated with C. vaginitis. As such, in the absence of pain, soreness, burning, and dyspareunia, BV has been considered a noninflammatory condition—hence, the term vaginosis, and not vaginitis. The lack of major inflammatory signs has correlated with the lack of polymorphonuclear leukocyte accumulation in vaginal secretions in BV.
In pregnant women, BV has been associated with an approximately twofold risk for developing preterm delivery, premature rupture of membranes, low birth weight, and postpartum endometritis. Women who have BV are more likely to have upper genital tract infections than those who do not. Similarly, women who have pelvic inflammatory disease (PID) are more likely to have BV.
C. albicans is usually implicated as the cause of yeast infection. Vulvovaginal candidiasis (VVC) may be caused by less common nonalbicans species, such as C. glabrata and C. tropicalis, which tend to be more resistant to standard treatment.
Established risk factors for VVC include uncontrolled diabetes, steroid-induced immunosuppression, recent antibiotic use, and infection with HIV. C. albicans is more common in the summer under tight or nonporous clothing (jeans, synthetic underwear, and wet bathing suits). Vulvar pruritus is the most common symptom of VVC. Vaginal discharge is often minimal and sometimes absent. Although described as cottage cheese–like in character, the discharge may vary from watery to homogeneously thick.
Symptoms and signs are extremely nonspecific and can be simulated by a variety of noninfectious causes (e.g., contact and irritant dermatitis). In fact, only 20% of women presenting with pruritus have VVC. A recent assessment of the criteria for wet preparation–based diagnosis suggests that this approach is neither highly sensitive nor specific when using culture as the gold standard for diagnosis. Although costly, vaginal culture can be helpful in cases of recurrent symptoms or in women with typical symptoms and a negative KOH preparation. A reasonable approach is to reserve culture for cases of treatment failure and to routinely use a wet mount and KOH preparation or a Gram stain of a vaginal discharge in conjunction with physical examination findings. DNA-based diagnostic tools with fairly good degrees of sensitivity and specificity are also available.
Symptoms alone do not allow clinicians to distinguish confidently between the causes of vaginitis. However, if there is no itching, candidiasis is less likely, and lack of perceived odor makes bacterial vaginosis unlikely. Similarly, physical examination signs are limited in their diagnostic power. The presence of inflammatory signs is associated with candidiasis. Presence of a “high cheese” odor on examination is predictive of bacterial vaginosis, whereas lack of odor is associated with candidiasis. Laboratory tests, particularly microscopy of vaginal discharge, are the most useful way of diagnosing the three conditions described in this chapter.
Stay updated, free articles. Join our Telegram channel

Full access? Get Clinical Tree


